Abstract
Introduction: Population ageing, including in sub-Saharan Africa, has led to an increasing number of elderly patients requiring anesthetic management. These patients present age-related physiological changes and a high burden of comorbidities, exposing them to an increased risk of perioperative adverse events.
Objective: To evaluate retrospectively patient characteristics, anesthetic management, and perioperative incidents in elderly patients undergoing surgery at the Peace hospital of Ziguinchor.
Patients and Methods: A retrospective, descriptive, and analytical study was conducted over a 21-month period including patients aged 60 years and older who underwent surgery under general or regional anesthesia. Data collected from operating room registers and anesthesia records included demographic characteristics, comorbidities, preoperative investigations, anesthetic techniques, perioperative incidents, and their management. Statistical significance was set at p < 0.05.
Results: A total of 357 patients aged 60 years or older were included, representing 10.2% of anesthetic activity. The mean age was 70.4 years, with a maximum of 94 years. Male predominance was observed (sex ratio 2.4). Hypertension was the most frequent comorbidity (48%), followed by diabetes (11%). Preoperative anemia was present in 63.7% of patients. Surgical indications were mainly urological (36%) and general surgery (35%). General anesthesia accounted for 55% of anesthetic techniques. The most common peroperative incident was arterial hypotension (38%). Operative duration was strongly correlated with incident occurrence, with rates increasing from 20.8% for surgeries lasting less than 50 minutes to 76.4% for those exceeding 120 minutes (p < 0.001). Thirty-days postoperative mortality rate was 4.5% and was independently associated with higher ASA physical status (III-IV) and prolonged operative duration (≥120 minutes).
Conclusion: Anesthetic management of elderly patients is characterized by a high prevalence of comorbidities and a high incidence of perioperative arterial hypotension. Thirty-days postoperative mortality in elderly patients is mainly determined by baseline physical status and operative duration rather than chronological age alone. Preoperative optimization and close monitoring are essential to reduce perioperative risk.
Keywords:Elderly Patients; Anesthesia; Perioperative Incidents; Sub-Saharan Africa
Abbreviations:WHO: World Health Organization; ASA: American Society of Anesthesiologists; MET: Metabolic Equivalent; BIS: Bispectral Index
Introduction
The World Health Organization (WHO) defines elderly individuals as those aged 60 years and older. This population is steadily increasing worldwide. Since 2020, the number of people aged over 60 years has exceeded that of children under five years of age [1]. Population ageing also affects low-income countries. In sub-Saharan Africa, individuals aged over 60 years accounted for 4.7% of the population in 1995 [2]. According to projections, by 2050, two-thirds of people aged over 60 years will be living in low- and middle-income countries [1]. As a result, the medical management of elderly patients will increasingly concern all medical specialties. For anesthesiologists and intensivists, the perioperative management of elderly patients remains a major challenge, both in emergency and elective surgical settings. Age-related physiological changes make this population more susceptible to poor tolerance of both anesthesia and surgery. The objective of this study was to evaluate anesthetic management in elderly patients at Peace hospital of Ziguinchor (Senegal).
Patients and Methods
This was a retrospective, descriptive, and analytical study involving patients aged 60 years and older who underwent surgery at Peace hospital of Ziguinchor. The study period covered 21 months, from January 1, 2024 to September 30, 2025. Patients were identified using operating room registers and anesthesia records. Patients aged over 60 years with unusable anesthesia records, as well as those managed under local anesthesia alone, were not included. Anesthesia records provided information on preoperative clinical and paraclinical assessment, anesthetic management, perioperative incidents and their management, and postoperative patient disposition. Epidemiological data were collected. Preoperative data included diagnosis, type of surgery, medical history and comorbidities, ongoing treatments, and results of preoperative investigations. The American Society of Anesthesiologists (ASA) physical status classification and metabolic equivalent (MET) were also recorded.
Intraoperative data included the type of anesthesia, induction technique, anesthetic agents used, perioperative incidents, and their management. Postoperative data included information on postoperative analgesia, postoperative orientation of the patient, and surgical outcomes. Data entry was performed using Microsoft Excel 2016. Statistical analysis was conducted using Epi Info version 7.2.6 and SPSS. Categorical variables were compared using the chi-square test. Statistical significance was defined as a p-value < 0.05. Intraoperative hypotension was defined as any recorded systolic arterial pressure < 90mmHg or a decrease > 40% from baseline during anesthesia. Bradycardia was defined as any recorded heart rate< 50beats per minute during anesthesia. Quantitative variables were described using means and compared using Student’s t-test. Qualitative variables were expressed as frequencies and percentages and compared using chi-square test or Fisher’s exact test, as appropriate according to expected cell counts. A univariate analysis was performed to identify factors associated with the occurrence of peroperative incidents and factors associated with 30-days postoperative mortality. A multivariate logistic regression model was used to identify factors independently associated with postoperative mortality. Results are presented as adjusted odds ratios (aORs) with their 95% confidence intervals.
Results
During the study period, 357 patients aged 60 years and older underwent surgery, representing a frequency of 10.2%. The mean age was 70.4 years, with extremes ranging from 60 to 94 years. Patients aged between 60 and 75 years accounted for 74.2% of the study population. Male patients were predominant, with a sex ratio of 2.4. Hypertension was present in 48% of patients, while diabetes was reported in 11%. A history of stroke was noted in 10 patients (3.7%). Previous hernia repair was found in 13% of patients, and 5% had a history of prostate surgery. Amlodipinebased treatment was reported in 26% of patients, and 8% were receiving angiotensin-converting enzyme inhibitors. Antidiabetic treatments were recorded in 27 patients (7.5%). Urological surgery was the most frequent specialty, followed by general surgery and orthopedic surgery, accounting respectively for 36%, 35%, and 14% of cases.
Elective surgery represented 76% of procedures. In emergency settings, acute surgical abdomen was the most frequent indication (48%), followed by soft tissue infections (20%). In elective surgery, bladder and/or prostate tumors were the most common indications (29%), followed by uncomplicated hernia disease (25%). Testicular and spermatic cord disorders accounted for 10% of elective surgical diagnoses. At pre-anesthetic evaluation, the mean body weight was 63 kg, with extremes ranging from 31 to 101 kg. Mean systolic blood pressure was 141 mmHg, with values ranging from 80 to 220 mmHg. In 54.3% of patients, systolic blood pressure exceeded 140 mmHg. Pneumonia was reported in 5.9% of patients. Digestive disorders were present in 29%, lower urinary tract symptoms in 19%, and neurological disorders in 4.7% of patients. A preoperative blood test was performed in 94.1% of patients, showing a mean hemoglobin level of 11.9 g/ dL, with extremes ranging from 6.8 to 18.6 g/dL. Mild to severe anemia was observed in 63.7% of patients, and thrombocytopenia in 7.14%.
Anemia was defined according to WHO criteria. Renal function assessment was performed in 45% of patients and revealed impaired renal function in 15.9%. Urine culture was systematically performed for scheduled urological surgery and revealed urinary tract infection in 13.1% of cases, with Escherichia coli being the most frequently isolated pathogen (5%). Electrocardiography was performed in 82% of patients and showed rhythm and/or conduction abnormalities in 27.4%. Signs of cardiac overload and coronary hypoperfusion were observed in 17.9% and 9.2% of patients, respectively. Transthoracic echocardiography was performed in 12% of patients and revealed valvular heart disease in 4.5% and cardiomyopathy in 2.8%. The metabolic equivalent ranged between 4 and 7 in 47% of patients. At the end of preoperative assessment, ASA physical status II was assigned to 54% of patients, and ASA III to 21.8%.
General anesthesia was the most frequently used technique (55%), followed by neuraxial regional anesthesia (40%). Induction was conventional, using fentanyl, titrated propofol, and neuromuscular blocking agents. Atracurium and vecuronium were used in 23.5% and 22% of patients, respectively. Isoflurane and sevoflurane were used in 36.1% and 19.3% of cases, respectively. Antibiotics were administered either for prophylaxis or therapy, with amoxicillin-clavulanic acid being the most commonly used (49.8%), followed by ceftriaxone (26.6%). Arterial hypotension was the most common perioperative incident, occurring in 38% of patients. The incidence of perioperative incidents increased with age, from 38.87% in patients aged 60-74 years to 50% in the very elderly; however, this association was not statistically significant (p = 0.615). Incidents were more frequent in patients with a metabolic equivalent below 4 (53.6%), without statistical significance (p = 0.25), and during emergency surgery compared with elective surgery (49% vs. 42%; p = 0.27). A significant association was observed between operative duration and the occurrence of perioperative incidents (Table 1). Surgeries lasting less than 50 minutes were associated with a low incidence of incidents (20.8%), whereas surgeries exceeding 120 minutes were associated with a high incidence (76.4%) (p < 0.001).
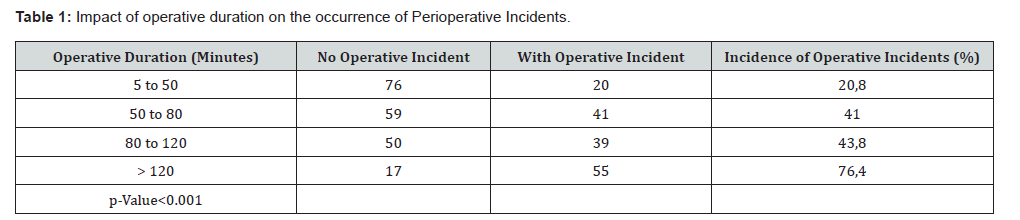
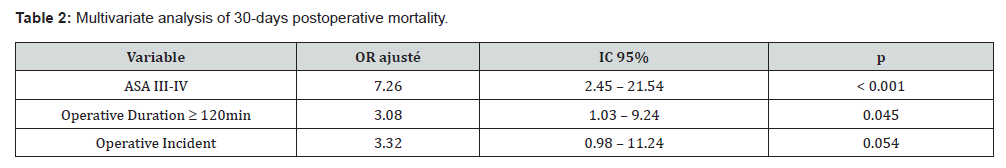
Blood transfusion was required in 11.7% of patients, and vasopressors were administered in 38.3%. The mean operative duration was 97.27 minutes, with extremes ranging from 20 to 720 minutes. Postoperative admission to the intensive care unit occurred in 10.3% of cases. Postoperative regional analgesia was provided in 14% of patients, while the others received intravenous analgesia with paracetamol and tramadol. Reoperation was required in 2.8% of patients (Table 2). No intraoperative deaths were recorded. Postoperative mortality was 4.48%. Deaths occurred mainly in patients operated on for neoplastic diseases (50%) and abdominal emergencies (25%). The median time to death was 4 days (Range: 1-25 days). In multivariate analysis, 30- days postoperative mortality was independently associated with ASA physical status class ≥ 3 (p<0.001) and operative duration ≥ 120 minutes (p=0.045). The occurrence of a perioperative incident was associated with a non-significant increase in mortality (OR 3.32; P=0.054). ASA class ≥ 3 was the factor most strongly associated with 30-days postoperative mortality.
Discussion
In our study, the frequency of anesthesia in elderly patients was 10.2%. This proportion is considerably lower than that reported in high-income countries [3]. This difference reflects demographic disparities between Western populations and those of sub-Saharan Africa. Indeed, the Senegalese population is particularly young, with a mean age of 23.6 years [4]. In contrast, in high-income countries, improvements in healthcare systems have contributed to increased life expectancy. Hypertension was the most common comorbidity in our study, affecting 48% of patients. Hypertension is highly prevalent in sub-Saharan Africa, with reported rates exceeding 60% among individuals over 65 years of age, and a high proportion of patients remain undiagnosed or untreated [5]. Due to genetic and socioeconomic factors, hypertension in individuals of African descent tends to occur earlier, be more severe, and progress more rapidly, leading to earlier complications [6]. This results in more severe target organ damage. Postoperative complications associated with hypertension include sudden death, ventricular failure, myocardial ischemia and infarction, renal injury, and stroke [7].
The anesthesiologist plays a crucial role in improving outcomes in hypertensive patients through adequate preoperative assessment and optimized intraoperative and postoperative management. Calcium channel blockers are generally well tolerated perioperatively and may be continued until premedication, allowing effective blood pressure control [8]. In contrast, angiotensin-converting enzyme inhibitors and angiotensin II receptor blockers should be discontinued prior to surgery, as they may potentiate the cardiovascular depressant effects of anesthetic agents [7]. Electrocardiographic abnormalities were observed in 54.5% of patients, mainly among those with hypertension. Most rhythm disturbances were benign, except for two cases of complete atrioventricular block, three cases of atrial flutter/fibrillation, and one case of long QT syndrome. In patients with long QT syndrome, perioperative management aims to minimize the risk of malignant ventricular arrhythmias due to repolarization abnormalities and increased morbidity.
Drugs such as ketamine, epinephrine, succinylcholine, and atropine should therefore be avoided in these patients [9]. The two patients with complete atrioventricular block were equipped with permanent pacemakers. In such cases, electromagnetic interference from electrocautery may cause pacemaker malfunction, which can be particularly dangerous in pacemakerdependent patients [10]. The preferential use of bipolar electrocautery or ultrasonic surgical devices is recommended to reduce this risk. Arterial hypotension was the most frequent perioperative incident, occurring in 38% of patients. This is the most commonly reported complication during anesthesia in elderly patients [11]. Hypotension is partly related to the combined effects of anesthesia and age-related cardiovascular fragility. Aging is associated with myocardial alterations, reduced arterial wall compliance, and impairment of autonomic nervous system function. Autonomic dysfunction increases the risk of anesthesia-induced vasoplegia due to inhibition of sympathetic counter-regulatory mechanisms [12]. Peroperative hypotension appears to be more closely related to the patient’s overall health status, reflected by a higher ASA physical status, rather than chronological age alone.
Elderly patients with poor baseline health or comorbidities such as hypertension and diabetes are at increased risk of intraoperative hypotension [11]. Our study also demonstrated that operative duration was significantly associated with the occurrence of perioperative incidents (p < 0.001). This association may be explained by the complexity of surgical procedures and prolonged exposure to anesthetic agents in physiologically vulnerable patients. Reducing the incidence and severity of peroperative hypotension requires optimal preoperative control of comorbidities, careful selection of anesthetic techniques and agents, effective control of surgical bleeding, and prompt correction of any hypotensive episodes. Whenever feasible, regional anesthesia should be preferred. In addition, depth-ofanesthesia monitoring using the bispectral index (BIS), combined with careful titration of anesthetic agents, may help reduce the hemodynamic impact of anesthesia in elderly patients [13]. Postoperative mortality at 30 days was 4,5%. Multivariate analysis identified ASA physical status and operative duration of at least 120 minutes as independent predictors of mortality.
The results reinforce the central role of preoperative physical status and surgical burden in determining short-term postoperative survival among elderly patients. This study has several limitations that should be acknowledged. First its retrospective design exposes the results to potential selection and information biases related to the completeness and accuracy of anesthesia records. Second, the monocentric nature of the study limits the generalizability of the findings to other healthcare facilities, particularly those with different resource availability. Furthermore, the study population was heterogeneous and surgical procedures had different levels of complexity which may influence the occurrence of perioperative events. Despite these limitations, this study provides valuable data on anesthetic management and perioperative complications among elderly patients in a resource-limited setting.
Conclusion
Anesthesia in elderly patients represents a growing challenge in low- and middle-income countries. In our setting, elderly patients accounted for a relatively low proportion of surgical activity; however, they presented with a high burden of comorbidities, particularly hypertension, and a significant rate of perioperative incidents. Arterial hypotension was the most frequent complication and was strongly associated with prolonged operative duration rather than chronological age alone. These findings highlight the importance of comprehensive preoperative assessment, optimal control of comorbidities, careful selection and titration of anesthetic agents, and vigilant intraoperative monitoring in elderly patients. Whenever feasible, regional anesthesia and strategies aimed at minimizing hemodynamic instability should be prioritized. Improving perioperative care for this vulnerable population may contribute to reducing morbidity and postoperative mortality in resource-limited settings.
References
- (2025) World Health Organisation. Ageing and health. Geneva: WHO.
- Schoumaker B (2000) Le vieillissement en Afrique Subsaharienne. In: Espace, population, société 3: 379-390.
- Canales C (2025) The older adult surgical patient: a review of optimization and gaps in clinical practice. Perioper Med 14(1): 104.
- (2024) National Agency for Statistics and Demography (ANSD). RGPH-5, 2023-Interim Global Report. Dakar: ANSD.
- Houehanou C (2018) Hypertension artérielle en Afrique Subsaharienne. JMV-Journal de Médecine Vasculair 43(2): 87.
- Cane Fabien (2017) Hypertension in people of African descent. Rev Med Suisse 13(574): 1576-1579.
- Barby T, Coriat P (2004) Hypertension and anesthesia. EMC-Anesthesia-Resuscitation 1(1): 25-25.
- Stone JG (1988) Myocardial ischemia in untreated hypertensive patients: effects of a single small oral dose of a beta-adrenergic blocking agent. Anesthesiology 68(4): 495-500.
- O’Hare M (2018) Perioperative management of patients with congenital or acquired disorders of the QT interval. British Journal of Anaesthesia 120(4): 629-644.
- Gayot J (2014) Cardiac arrest secondary to pacemaker dysfunction during general anesthesia in a young adult patient. French Annals of Anaesthesia and Resuscitation 33(4): 266-268.
- Ba EHB (2017) Intra-anesthetic arterial hypotension in elderly patients during emergency surgery: what are the risk factors? Pan Afr Med J 26: 242.
- Mérat S, Pasquier P, Péraldi C, Sauvageon X (2021) Field-related anesthetic procedures. Paris: Arnette 2: 278.
- Zhuen Chew Wei (2022) Bispectral Index (BIS) monitoring and postoperative delirium in eldery patients undergoing surgery: a systematic review and meta-analysis with trial sequential analysis. J cardiothorac vasc anesth 36(12): 4449-4459.






























