Challenges In Securing Central Venous Access in a Case of Ankylosing Spondylitis with Kyphotic Deformity
Raunak Parida1, Rakesh Kumar1 and Swetha Rudravaram2*
1Department of Anaesthesia, All India Institute of Medical Sciences, India
2Department of Anesthesia, Fellow Pediatric Anesthesia, Chacha Nehru Bal Chikitsalya, India
Submission: December 24, 2021; Published: May 17, 2022
*Corresponding author: Swetha Rudravaram, DNB Anesthesia, Fellow Pediatric Anesthesia, Chacha Nehru Bal Chikitsalya, New Delhi, India
How to cite this article: Raunak P, Rakesh K, Swetha R. Challenges In Securing Central Venous Access in a Case of Ankylosing Spondylitis with 002 Kyphotic Deformity. J Anest & Inten care med. 2022; 12(1): 555830. DOI 10.19080/JAICM.2022.12.555830
Abstract
Ankylosing spondylitis is an inflammatory disorder that primarily affects the axial skeleton although extra-articular structures and peripheral joints can also be involved. Over time the disease causes fusion and rigidity of the spine and can result in hyperkyphotic hump. While securing an internal jugular venous access, patients are usually positioned in a Trendelenburg position to distend the vein, increase the cross-sectional area and improve the chance of successful cannulation. We report the case of a 40-year-old male with ankylosing spondylitis with a kyphotic deformity presenting for deformity correction. Due to the severity of kyphosis, had a very limited neck extension the patient was not able to lie supine and thus trendelenburg position was not feasible. In this case report we focus on the challenges involved in securing a central venous access in a suboptimal position and briefly discuss the anaesthetic management.
Keywords:Ankylosing spondylitis; central venous access; difficult positioning
Case Details
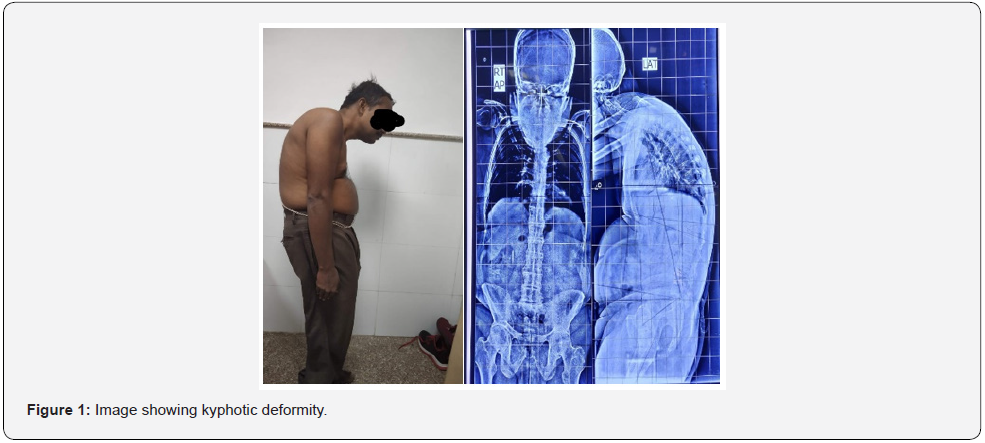
A 40-year-old male, weighing 62 kgs presented with deformity of the back since 12 years and was diagnosed with ankylosing spondylitis. It was associated with morning stiffness and dull aching pain that was partially relieved with non-steroidal anti-inflammatory drugs. There was no history of trauma / tuberculosis / fever / weight loss or previous surgeries. The patient had no other comorbidities and had an effort tolerance of more than 4 metabolic equivalents (METS). No other associated features of ankylosing spondylitis were present. On examination, vitals were normal. A kyphotic deformity involving the thoracolumbar vertebrae was noticed (Figure 1). Bilateral lower limb power, deep tendon reflexes and sensory examination were within normal limits. On airway examination, the patient had less than 10 degrees neck extension with adequate mouth opening, intact teeth and a mallampati grade 3. Hemogram, electrocardiogram and 2D echocardiography were within normal limits and pulmonary function tests (PFT) showed a moderate restrictive pattern.
Anaesthetic management
The patient was brought to the operating room (OR) after an appropriate period of fasting. Standard monitoring was instituted,and the patient was placed in a semi sitting position as positioning the patient in supine was not possible due to the existing kyphosis. This was done with the help of pillows and sheets stacked in the form of a ramp under the head, neck, and upper back. After preoxygenation, the patient was induced with fentanyl 50 ug intravenously and sevoflurane. Check ventilation was done and then succinylcholine 75 mg IV was given. Patient was intubated with an 8.0 mm cuffed reinforced endotracheal tube in a semi-sitting position with fiberoptic bronchoscope guidance.
A triple lumen catheter was placed in the right internal jugular vein using USG guidance in the semi-sitting position. As the IJV tends to collapse in the sitting position, an inspiratory pause and a positive end expiratory pressure (PEEP) of 10 cm of H2O was used to help in the placement. A 20G arterial cannula was placed in the right radial artery. The patient was carefully positioned in prone with adequate padding of the pressure areas and the abdomen was kept free. Anaesthesia was maintained with total intravenous anaesthesia (TIVA) using propofol and fentanyl infusion as Motor evoked potentials (MEP) monitoring was required during the surgery. Intra operative vitals were stable, and the patient had a small pleural tear on the right side during the surgery which was repaired. During the eight-hour surgery, the blood loss was 3.5 litres which was replaced with 5 units of packed red blood cells, 4 units of fresh frozen plasma, 3 units of platelets along with 3lts of crystalloids and 1.5 litres of hydroxyethyl starch. The urine output was 850ml. In view of the difficult airway and massive blood loss, the patient was not extubated and was shifted to intensive care unit. The patient was extubated on post operative day 2 and discharged from the hospital after 7 days.
Discussion
Ankylosing spondylitis is an inflammatory disorder that primarily affects the axial skeleton although extra-articular structures and peripheral joints can also be involved [1]. Overtime the disease causes fusion and rigidity of the spine and can result in hyperkyphotic hump. Anesthetic challenges range from a potential difficult airway (due to the involvement of the cervical and thoracic spine) to perioperative complications due to the involvement of cardiovascular and respiratory system [2]. While securing a internal jugular venous access, patients are usually positioned in a Trendelenburg position to distend the vein, increase the cross sectional area and improve the chance of successful cannulation [3]. Other methods to increase the chances of successful cannulation include application of peep [4], application of liver/abdominal pressure, simulated Valsalva manoeuvre [5] and passive leg raising [6] PEEP increases the intrathoracic pressure impeding venous return and compressing the superior vena cava distending the internal jugular vein. Addition of PEEP also decreases the carotid artery overlap with the IJV [7]. Application of high positive airway pressure may have adverse consequences such as hypotension and an ideal pressure of 20 cm of H2O has been suggested to achieve increased vein diameter with a low complication rate [8].
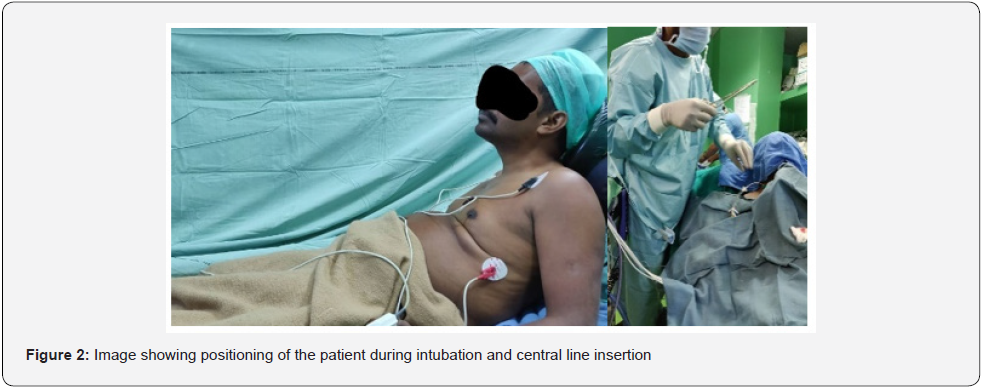
In our patient, due to the severity of the deformity, Trendelenburg position was not feasible. The application of PEEP and inspiratory pause predictably distended the right IJV, and cannulation was possible in a semi sitting position using ultrasound guidance without any complications (Figure 2).
Conclusion
Securing central venous access in patients with ankylosing spondylitis can be challenging especially when positioning in supine or trendelenburg is impossible due to the deformity. The application of PEEP and inspiratory pause can make this process a lot easier by distending the internal jugular vein and decreasing overlap with the carotid artery.
References
- John Varga (2018) Systemic sclerosis and related disorders. In: Jameson, Fauci (eds.) Harrison's principles of internal medicine. 20th edition. McGraw Hill education; Chapter 353: 2564-2567.
- Woodward LJ, Kam PC (2009) Anaesthetic implications of ankylosing spondylitis. Anaesthesia 64(5): 540-548.
- Garcia-Leal M, Guzman-Lopez S, Verdines-Perez AM, et al. (2021) Trendelenburg position for internal jugular vein catheterization: A systematic review and meta-analysis. Vol 233(5): 246.
- Lee SC, Han SS, Shin SY, Lim YJ, Kim JT, et al. (2012) Relationship between positive end‐expiratory pressure and internal jugular vein cross‐sectional area. Acta anaesthesiologica scandinavica. vol 56(7): 840-845.
- Armstrong PJ, Sutherland R, Scott DH (1994) The effect of position and different manoeuvres on internal jugular vein diameter size. Acta anaesthesiologica scandinavica 38(3): 229-231.
- Xie S, Yu Q, Li T, Xu M, et al. (2019). Comparison of the effect of different degrees of passive leg raising on the internal jugular vein cross-sectional area in patients before thoracic surgery. BMC anesthesiology 19(1): 78.
- Machanalli G, Bhalla AP, Baidya DK, et al. (2018). Sono-anatomical analysis of right internal jugular vein and carotid artery at different levels of positive end-expiratory pressure in anaesthetised paralysed patients. Indian journal of anaesthesia. Vol 62(4): 303-309.
- Zhou Q, Xiao W, An E, et al. (2012). Effects of four different positive airway pressures on right internal jugular vein catheterisation. Eur J Anaesthesiol. Vol 29(5): 223-228.






























