Petroleum Jelly as an Alternative Coupling Medium in Focus Assessed Transthoracic Echocardiography (FATE)
C Smit* and A Breedt*
Department of Anaesthesiology and Critical Care, Faculty of Medicine and Health Sciences, Stellenbosch University, South Africa
Submission: November 15, 2021; Published: March 04, 2022
*Corresponding author: C Smit, Department of Anaesthesiology and Critical Care, Faculty of Medicine and Health Sciences, Stellenbosch University, South Africa, ORCID: https://orcid.org/0000-0002-8168-6416
A Breedt, Department of Anaesthesiology and Critical Care, Faculty of Medicine and Health Sciences, Stellenbosch University, South Africa, ORCID ID: https://orcid.org/0000-0002-5242-3684
How to cite this article: C Smit, A Breedt. Petroleum Jelly as an Alternative Coupling Medium in Focus Assessed Transthoracic Echocardiography (FATE). J Anest & Inten care med. 2022; 11(5): 555825. DOI 10.19080/JAICM.2022.11.555825
Abstract
Background:The use of ultrasound gel as a coupling medium has been the standard of practice for all ultrasound studies performed at most hospitals worldwide. This study aimed to introduce petroleum jelly [petrolatum] as an alternative coupling agent, specifically with regard to focus assessed transthoracic echocardiography [FATE], by comparing its use to conventional ultrasound gel.
Methods:A crossover, double-blinded, non-inferiority study was conducted to ascertain whether petroleum jelly scores equal to ultrasound gel in terms of image quality [depth, penetration, detail, and overall quality] and user experience [pressure applied, amount of gel used, user friendliness, and patient tolerance] using a General Electric [GE] Vscan Extend handheld ultrasound [HHU] device. The automated ejection fraction calculation was also noted and statistically compared.
Results:No significant difference was found between image quality or user experience in FATE scans performed with the conventional ultrasound gel and petroleum jelly. The automated ejection fraction calculation results obtained from scans with petroleum jelly showed minimal inter-user variability. Blinded sonographic review also did not rate the images obtained with either coupling medium significantly different in any measure. Finally, petroleum jelly is more cost effective than conventional ultrasound gel.
Conclusion:Petroleum jelly produces images of comparable quality to that obtained using conventional gel. The use of petroleum jelly as an alternative coupling medium could increase the practice of ultrasound in settings with resource limitations.
Keywords:ultrasound, echocardiography, point-of-care, critical care
Introduction
Sonography has become a vital clinical tool in resource-limited settings due to reduced cost, increased patient comfort, ease of portability, real-time diagnosis capability, and lack of ionizing radiation [1]. The World Health Organization (WHO) has described ultrasound as an effective, safe, versatile and low-cost clinical modality [2]. One of the largest global healthcare organizations, Partners in Health, has studied the use of ultrasound in low-resource settings and found this modality to be a helpful skill that is teachable and “a critical component in global health delivery” [3]. Throughout the world, point-of-care ultrasound has proven to be an ideal imaging modality in rural and resource-limited countries. Clinical predictive capability is made easier for most clinicians, including for anaesthetists, through modalities such as transthoracic echocardiography (TTE). Focus assessed transthoracic echocardiography (FATE), which is a TTE protocol that focusses on obvious pathologies, provides important diagnostic information that changes perioperative patient management. The FATE protocol principally aims to exclude obvious cardiac and pleural pathologies [4]. Moreover, perioperative case series reports, and multiple clinical studies have shown that FATE can prevent adverse events and have a direct clinical impact on patient mortality [5-7], which is why several academic societies now advocate focused TTE as a mandatory skill for critical care physicians [8,9].
Image acquisition, however, needs to be precise, and the correct views must be obtained in a short amount of time, all of which is contingent upon user experience and, importantly, the coupling medium used. Indeed, using an appropriate coupling medium is crucial in ultrasonography to improve the conduction of the ultrasound waves between the probe and the patient’s tissue [4]. Limited access to ultrasound coupling gel in low-resource settings can significantly hamper the clinical application of FATE. This study aims to introduce petroleum jelly as a cost effective and readily available alternative coupling medium.
The primary objective of this study was to compare petroleum jelly to conventional ultrasound gel as an alternative coupling medium during FATE by having medical staff at the Faculty of Medicine and Health Sciences at Stellenbosch University rate the quality of the petroleum jelly-and conventional gel-based images, as well as their user experience whilst scanning an anatomical model. Secondarily, the automated ejection fraction calculation during each scan and the clinical acceptability of the images obtained using both mediums was assessed and compared by having an expert echocardiographer blindly review the images. Lastly, the cost effectiveness of using petroleum jelly instead of conventional gel was also calculated and compared.
Methods
Following review and approval from the Stellenbosch University Health Research Ethics Committee (ref #S21/03/039), a double-blinded, non-inferiority trial was performed using participants from the medical staff from the Department of Anaesthesiology and Critical Care, Faculty of Medicine and Health Sciences, Stellenbosch University. This specific sample population was chosen as medical personnel from this department uses FATE daily for critical patient care and perioperative patient evaluation and would benefit the most by the research being conducted. All participants performed FATE scanning on an anatomical model with a clinically normal cardiac anatomy using a handheld ultrasound device (GE Vscan Extend). This handheld ultrasound (HHU) device is a digital smart device that gives specific instructions on how to perform a FATE scan using an application called “Scan Coach”. These user instructions give specific information regarding the probe positioning for every view that needs to be obtained during the FATE scan. The participants were blinded, mediums unlabelled, and the sequence of mediums used randomised using a computer program. A scanprotocol was completed by participants for each coupling medium individually. The study participants acquired images that were then saved and uploaded onto the device. The participant was able to access reference ultrasound images of a normal anatomy and examples of common pathologies for each scanning plane whilst performing the FATE scan. Furthermore, the participant could also review 3D animations that showed the relationship between the probe positioning and resulting ultrasound images, with annotated schematics of the anatomical landmarks to acquire the desired view.
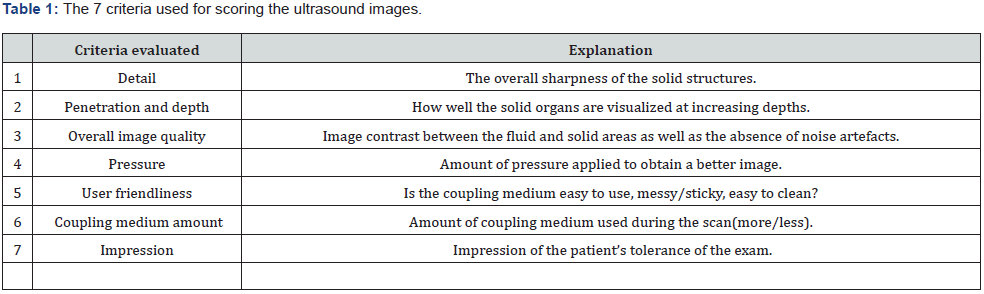
The LVivo EF application on the GE Vscan Extend HHU was also utilized during each scan to calculate the ejection fraction using a modified Simpson’s method. This application does automatic edge detection of the left myocardial wall with use of apical 4-chamber views to calculate the end-diastolic volume, end-systolic volume, and ultimately the ejection fraction. The participants were asked to score the ultrasound images obtained from the two separate scans on a 5-point Likert scale in terms of 7 criteria (Table 1) (See Addendum).
Sonographic review
The images obtained during every scan were also evaluated blindly by a cardiac physiologist using a Likert scale. An image pair was compared individually for each image parameter. Images were scored out of 10 in terms of image quality, depth, and penetration, and whether the image could be used clinically or not (see Addendum).
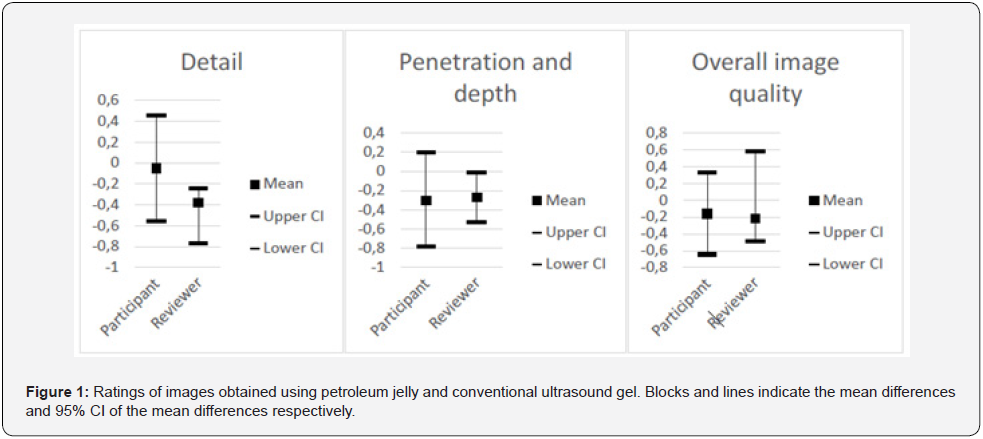
During digital evaluation, a grayscale tablet was used to evaluate the echo density in the muscle areas and echo-free areas in multiple regions of interest of each image (Figure 1). Muscular areas appear whiter on the scale and blood appears darker. A difference of 3 or more tones indicates an artifact and the quality of an image was judged by the number of artifacts present.
Addendum:
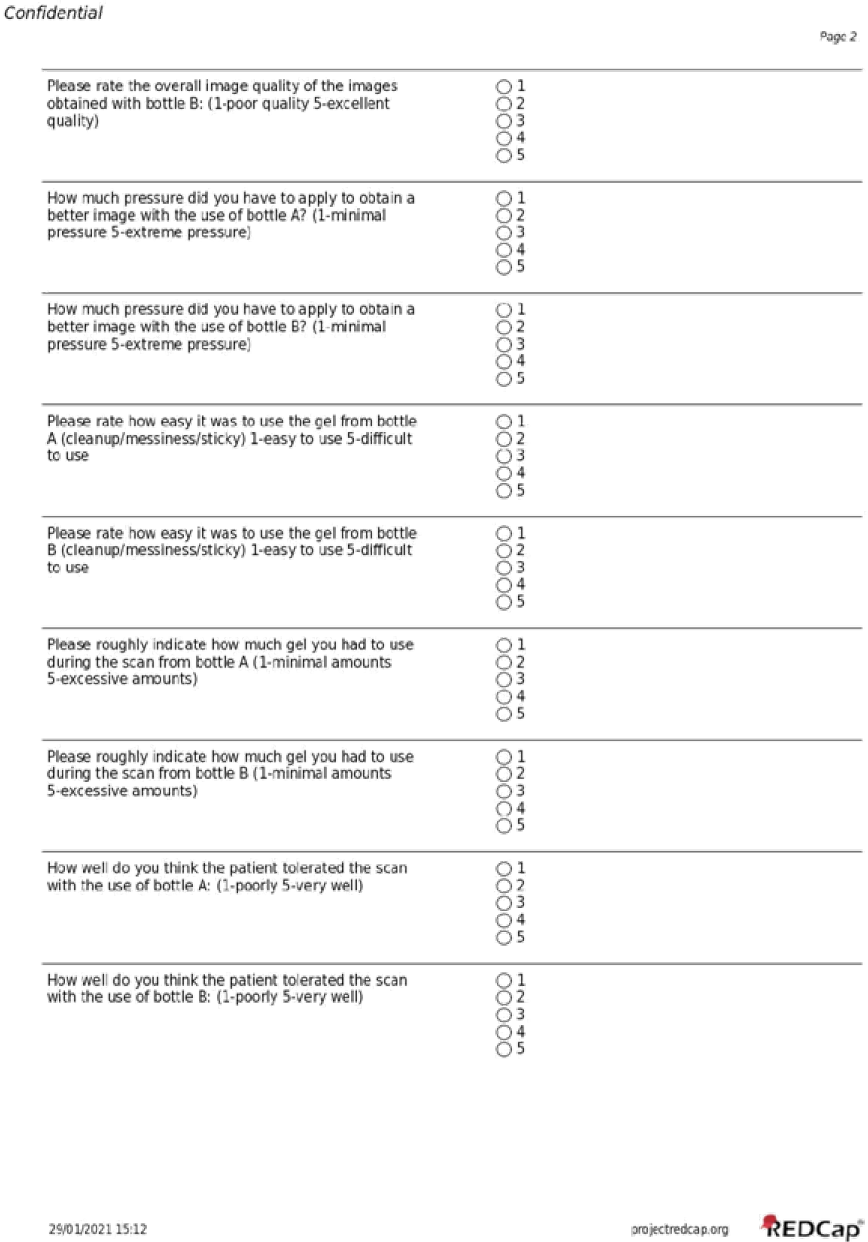



Statistics
Statistical analysis was done using Microsoft Excel® (Microsoft Corp, Redmond, WA, USA). and IBM SSPS Statistics Version 25 [10] and was based on a mixed linear model. Participants as well as the reviewer completed a digital online questionnaire. All data was collected and processed using RedCap (Research electronic data capture) software [11] hosted by Stellenbosch University.
A paired means power analysis of the 2x2 crossover design was done using Design and Analysis of crossover trials by Jones and Kenward [12,13] that estimated a power of 82% using a sample size of 34 from a population of 45 with an alpha of 0.05 and a beta of 0.17836. This would detect a mean paired difference of 1.0 with an estimated standard deviation of 4.5 and with a significance level (alpha) of 0.05 using a one-sided paired t-test. We set our non-inferiority margin as a difference of less than 1 unit (20%) on the respective Likert scales used. Discussions with clinicians and radiologists revealed that a difference of more than 1 unit on a 5-point Likert scale would be clinically significant. As the variance was unknown beforehand, we calculated a sample size that would be more than adequate to prove non-inferiority and were able to recruit 37 participants.
The automated ejection fraction obtained during each scan was recorded using an Excel spreadsheet, and a chi-squared McNemar’s test was done using the binomial distribution to determine whether the inter-user variance obtained met the set standard of 5% [14].
Results
Data was collected over a period of 8 weeks at the Department of Anesthesiology and Critical Care (DACC), Stellenbosch University. All participants met the inclusion criteria: medical staff members from the Anesthesiology department and surgical Intensive Care Unit who had never used petroleum jelly as a coupling medium during FATE ultrasound. The participant group consisted of 28 doctors from the DACC and 9 doctors from the Intensive Care Unit; this included 7 consultants, 21 registrars, and 9 medical officers, respectively. From this group, 7 had 3–5 years of experience with FATE ultrasound, 15 less than 3 years, and 15 little to none.
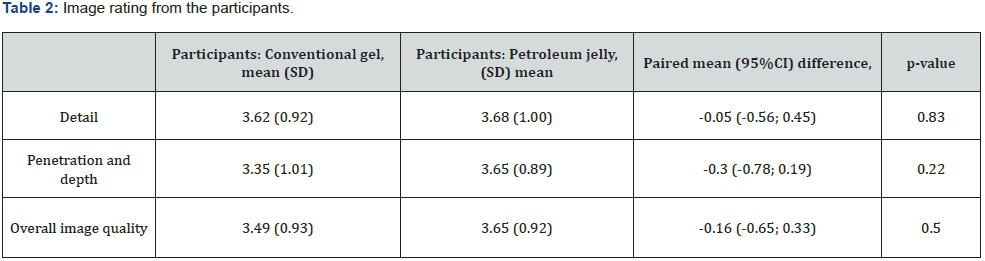
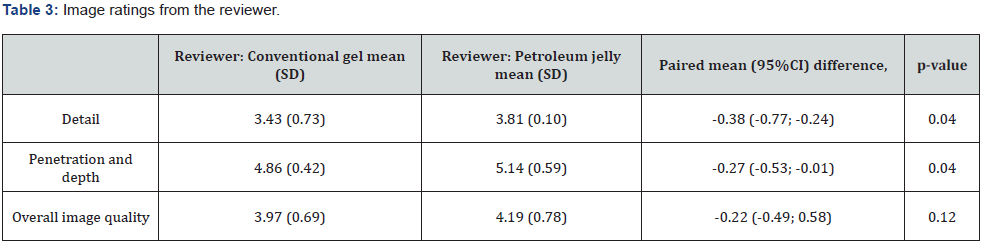
The rating of the overall image quality for images obtained using petroleum jelly as the coupling medium compared to the rating of the overall image quality for images obtained using traditional ultrasound gel amongst participants was non-inferior: paired mean diff.(participants) = -0.16 (95% CI: -0.65; 0.33) (Table2). In comparison, the radiological reviewer found that the images obtained from petroleum jelly were statistically superior in terms of detail (p=0.04) as well as depth and penetration (p=0.04), however not clinically superior as the paired difference did not exceed a value of one unit (Table 3).
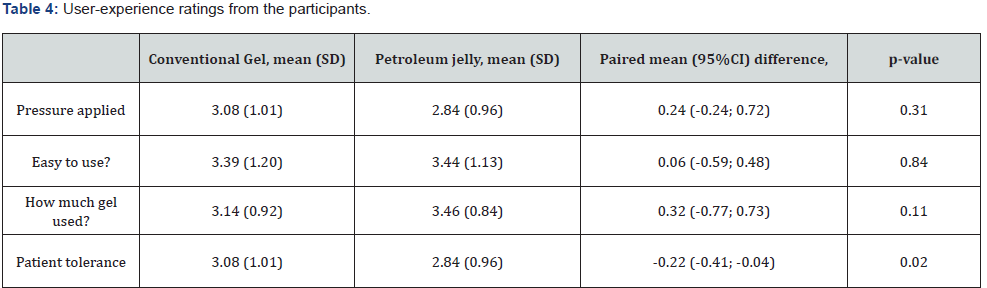
User experience (Table 4)
Participants found no perceptive difference in terms of user experience whilst comparing the two mediums from the questions asked. Both mediums were comparatively easy to use; paired mean difference = 0.06; 95% CI (-0.59; 0.48). Relatively similar amounts of both mediums were used for either scan; paired difference = 0.32; 95% CI (-0.77; 0.73). The average amount of pressure applied during each scan with either medium was also similar; paired mean difference =0.24 (-0.24; 0.72). There was, however, a statistically significant assessment that conventional ultrasound gel is better tolerated by the patient than petroleum jelly; paired mean difference=-0/22; 95%CI (-0.41; -0.04) (p=0.02).
Conventional ultrasound gel is purchased by Tygerberg Hospital from Health and Beyond suppliers at R11.31 per 250 mL bottle and white petrolatum at R7.50 per 250 mL jar [15]. Approximately 2–5 mL of conventional gel as well as petroleum jelly was used, respectively, on average among participants to perform a scan, which would mean that petroleum jelly use would save this institution R3.81 per bottle, 10 cents per mL, and 50 cents per scan.
Ejection fraction calculation
The inter-user variability for ejection fraction determination during scans done using ultrasound gel and petroleum jelly were both found to be 1%. Using petroleum jelly during automated ejection fraction determination is thus comparable to using ultrasound gel and meets the criteria for acceptability considering a set acceptable inter-user variability of 5% [14].
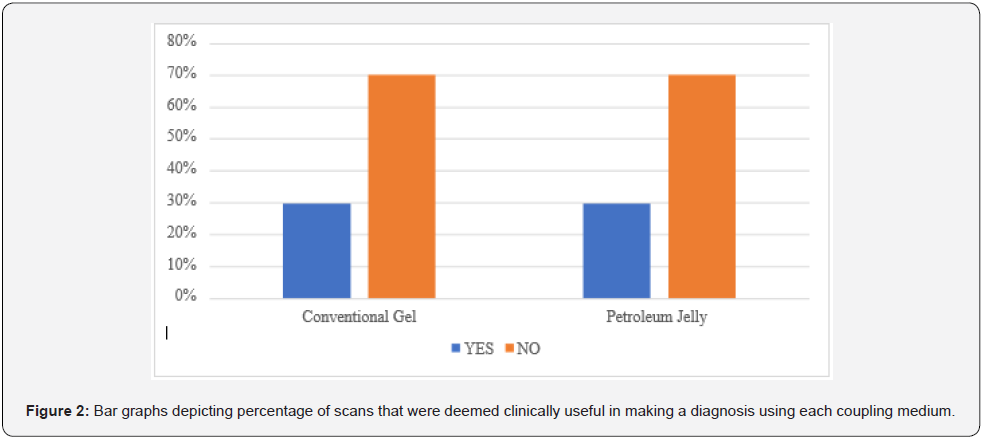
Clinical usability (Figure 2)
The sonographic reviewer was asked at the end of each evaluation to ascertain whether the images from the individual scans could be deemed “clinically usable” in their opinion.
A Chi Squared McNemar’s test of independence was performed and showed no significant association between the coupling medium used and the determination of clinical acceptability by the sonographic reviewer; (p=1) meaning that the exact same percentage of scans using petroleum jelly were deemed clinically usable to make a clinical diagnosis as were using conventional ultrasound gel (29.7%).
Discussion
Although ultrasound is an increasingly necessary and useful diagnostic tool, most resource-limited settings do not have the adequate funding for this technology nor the necessary coupling mediums to make use of this resource. In most urban and large hospital settings, commercial ultrasound gel is used for this purpose. Unfortunately, the availability of commercial ultrasound gel in low-resource settings is scarce and usually expensive. Commercial ultrasound gel is manufactured locally but needs to be imported in most other parts of Africa. For many rural and deprived communities, the cost and availability of ultrasound gel imposes a significant constraint on the quality and number of scans that are available to clinicians, even in settings where reliable ultrasound scanners are available [16]. Moreover, the gel that needs to be imported is sold at a higher price locally due to inclusion of importation duties and profits that local vendor make from procurement. Although these expenses might seem trivial in a developed country where resources are abundant, in an impoverished setting, this expense is far too big and one of the first of the clinical resources to be sacrificed.
These costs are invariably transferred to the patients that make use of health facilities and places extra financial constraints on health departments. Furthermore, for the sake of gel conservation, some establishments have gone as far as to ration the amount of coupling medium used for a scan to inadequately small amounts, which compromises the quality of the scans [16]. These developments are indeed very alarming, especially considering the high mortality and morbidity reported in deprived communities in trauma and obstetric cases, where ultrasound is a cornerstone of clinical management and patient treatment [16]. Thus, a need exists for alternative coupling mediums A multitude of alternatives to commercial gel have been suggested and tried, unfortunately with limitations and severe paucity in the literature—olive oil being expensive and unavailable in most settings, corn-starch having a manufacturing process that is complex and expensive, and the suggested WHO recipe of ethylenediaminetetraacetic, trolamine, propylene glycol, and carbomer being difficult to source and producing poor images [3].
A study by Engelbrecht and Palma in 2015 [17] showed that petroleum jelly could be used as a coupling agent for ocular ultrasound in an Emergency Department. However, Engelbrecht and Palma reported solely that the petroleum jelly did not damage the ultrasound probe, so there are no comparative data regarding the quality of the ultrasound images obtained with the respective coupling mediums.
This study clearly demonstrates that using petroleum jelly as a coupling medium produces sonographic images that are comparable and non-inferior to those produced by conventional ultrasound gel. Image quality was not negatively affected using petroleum jelly as a coupling medium, as proven by the blinded participants as well as a blinded reviewer. Participants also found petroleum jelly comparatively easy to use, with no difference in amount of pressure applied during the scan using equal amounts of both coupling mediums. Although patient tolerance showed a comparatively statistically significant difference, a clinically significant difference could not be proven. Inferential analysis of the automated ejection fraction calculation obtained during scans using either medium show that the calculation obtained from scans using petroleum jelly as a coupling medium showed an acceptable inter-user variability of less than 5% [15], a result identical to the variability amongst calculations using conventional ultrasound gel. Lastly, the blinded sonographic reviewer deemed the same ratio of scans clinically acceptable from the pooled scans using either of the mediums.
Strengths and Limitations
There is no evidence in the literature regarding the effect of petroleum jelly on ultrasound probes. This study was also conducted in a single center. Furthermore, performing and rating an ultrasound image depends on the subjective opinion of the sonographer, which can vary according to experience and personal bias towards the coupling medium used. Finally, ultrasound is a highly dynamic investigation, which can be very user dependent.
Conclusion
Petroleum jelly is an inexpensive, widely available, simpleto- use resource that produces images of similar quality to that of conventionally produced ultrasound gel. As we have formally demonstrated the non-inferiority of petroleum jelly in comparison to conventional ultrasound gel in FATE ultrasound, the ideal is to promote the use of this medium in settings that are resource-limited, attempting to increase the capacity for the use of ultrasound for diagnostic purposes, screening, and monitoring, as well learning.
Acknowledgements
The authors would like to thank Dr Jan Steyn, the head of Echocardiography at SUNHeart at Tygerberg Hospital, for the review of the echocardiographic information.
Conflict of Interest
The authors declare that there are no financial or personal relationships that may have inappropriately influenced the authors in writing this paper.
Ethical Approval
Approval to conduct the study was obtained from the Health Research Ethics Committee of Stellenbosch University (21784).
References
- Hill CR (1973) Medical ultrasonics: an historical review. Br J Radiol 46(550): 899–905.
- WHO (1998) Training in diagnostic ultrasound: essentials, principles and standards. Report of a WHO Study Group. World Health Organization technical report series P. 875.
- https://www.pih.org/practitioner-resource/manual-of-ultrasound-for-resource-limited-settings
- Holm JH, Frederiksen CA, Juhl-Olsen P, Sloth E (2012) Echo didactics: Perioperative use of focus assessed transthoracic echocardiography (FATE). Anesth Analg 115(5): 1029-1032.
- Jørgensen MRS, Juhl-Olsen P, Frederiksen CA, Sloth E (2016) Transthoracic echocardiography in the perioperative setting. Curr Opin Anaesthesiol 29(1): 46–54.
- Canty DJ, Royse CF (2009) Audit of anaesthetist-performed echocardiography on perioperative management decisions in non-cardiac surgery. Br J Anaesth 103(3): 353–358.
- Hori K, Matsuura T, Mori T, Nishikawa K (2015) Usefulness and growing need for intraoperative transthoracic echocardiography: a case series. BMC Anesthesiol 15: 90.
- Cowie B (2009) Focused Cardiovascular Ultrasound Performed by Anesthesiologists in the Perioperative Period: Feasible and Alters Patient Management. J Cardiothorac Vasc Anesth 23(4): 450–456.
- Fagley RE, Haney MF, Beraud AS, Comfere T, Kohl BA, et al. (2015) Critical care basic ultrasound learning goals for American anesthesiology critical care trainees: Recommendations from an expert group. Anesth Analg 120(5): 1041–1053.
- IBM Corp (2017) IBM SPSS Statistics for Windows, Version 25.0. IBM Corp, Armonk, NY, USA.
- Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, et al. (2009) Research electronic data capture (REDCap) -- A metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 42(2): 377–381.
- Machin D, Campbell M, Fayers P, Pinol A (1997) Sample Size Tables for Clinical Studies. (2nd edn) Blackwell Science, Malden, MA, USa.
- Zar Jerrold H (1984) Biostatistical Analysis (2nd edn). Prentice-Hall. Englewood Cliffs, New Jersey, USA.
- Pellikka PA, She L, Holly TA, Lin G, Varadarajan P, et al. (2018) Variability in Ejection Fraction Measured by Echocardiography, Gated Single-Photon Emission Computed Tomography, and Cardiac Magnetic Resonance in Patients with Coronary Artery Disease and Left Ventricular Dysfunction. JAMA Netw Open 1(4): e181456.
- https://www.afrimedics.co.za/product/ultrasound-gel/?Utm_source=Click&utm_medium=Channel&utm_campaign=pricecheck_ZA&SFDRRE%20F=SFDR_117882153
- Aziz A, Dar P, Hughes F, Solorzano C, Muller MM, et al. (2018) Cassava flour slurry as a low-cost alternative to commercially available gel for obstetrical ultrasound: a blinded non-inferiority trial comparison of image quality. BJOG 125(9): 1179–1184.
- Engelbert PR, Palma JK (2015) Petroleum jelly: A novel medium for ocular ultrasound. J Emerg Med 49(2): 172–174.






























