Effectiveness of an Invasive Mechanical Ventilation Weaning Protocol
Miriam Sánchez-Maciá1,2*, Maria José Castaño-Picó1,2, Jaime Miralles-Sancho1, Ana Pérez-Carbonell1 and Loreto Maciá-Soler1,2
11Hospital General Universitario de Elche. Calle Almazara, 11, 03203, Elche, Alicante. España, Spain
22Universidad de Alicante, Carretera de San Vicente del Raspeig, s/n, 03690, San Vicente del Raspeig, Alicante. España, Spain
Submission: January 13, 2021; Published: February 22, 2022
*Corresponding author: Miriam Sánchez-Maciá. Carretera de San Vicente del Raspeig, s/n, 03690, San Vicente del Raspeig, Alicante, Spain. Phone: 965903400
How to cite this article: Sá nchez-Macia M, Castañ o Picó MJ, Miralles-Sancho J, Pé rez-Carbonell A, Maciá -Soler L. Effectiveness of an Invasive Mechanical Ventilation Weaning Protocol. J J Anest & Inten care med. 2022; 11(5): 555823. DOI 10.19080/JAICM.2022.11.555823
Abstract
Objective: to know the effectiveness of the process of disconnection of invasive mechanical ventilation through the implementation of a standardized protocol led by the nursing team of a surgical Intensive Care Unit and implemented in a multidisciplinary way to reduce the ventilatory time of patients facing to the traditional clinical method of weaning.
Method: case-control study. 91 patients who required invasive mechanical ventilation for 24 hours or more were included and a group with the application of the standardized protocol was compared with the group that followed the usual clinical method.
Results: with the application of the standardized protocol, it was possible to reduce the time of invasive mechanical ventilation (85.29 ± 46.72 vs 116.92 ± 94.39); the time spent at weaning (2.40 ± 1.43 vs 41.250± 51.60) and the reintubation figures (2% vs 17%).
Conclusion: the use of disconnection protocols carried out in a multidisciplinary way is a useful tool to reduce invasive mechanical ventilation times and achieve improvements in the patient’s health.
Keywords:Artificial respiration; Critical Care; Evidence-based clinical practice; Weaning; Protocol; Nursing.
Introduction
Invasive mechanical ventilation (IMV) is considered an essential procedure that should be present in the Intensive Care Units (ICU) [1-3], constituting one of the main interventions that are performed in the management of critically ill patients [4-5]. Approximately, 35% of admissions in these units require IMV [6], and its incidence is expected to increase in the coming decades [5]. The indications for the use of IMV are multiple, such as its use in postsurgical patient, acute respiratory failure, neurological deterioration or shock, among others [7], also considering that its application is determined by the failure of other previous treatments [1]. Thanks to mechanical ventilation, life can be saved many times, but its prolonged use can have a negative impact on the patient’s health [8-13] associated with a higher rate of complications such as increased mortality [1,6,8,9,14-16], pneumonia associated with mechanical ventilation (VAP) [6,12,14,17], morbidity [9,14,15], increased hospital stay [5,8,11,15] and increased costs [2,7,9] among others. IMV produces associated complications, which is why it is necessary to reduce its use time as much as possible [9,12,18-20], being clear to the clinical team that the sooner it is removed or replaced by other techniques, the better the patient’s prognosis will be [21].
It has been studied that the weaning process occupies about 40% of the total time that the patient spends connected to the ventilator [7,14,17,21-23], and the evidence of this data indicates the significant difficulty of its withdrawal. In addition, according to recently published studies [1,8,18], the assessment to know if the patient is ready to be extubated may not be adequate, since 50% of those accidentally extubated do not require new reintubation, which suggests the other 50% may be on the respirator longer than necessary. To adjust the intubation time, it seems that applying standardized protocols can reduce the times without harming health, and also allow early identification of the patient who is actually in ventilatory weaning conditions.
According to the literature consulted, the use of IMV disconnection protocols seems beneficial, finding data that indicate a decrease in the total time of mechanical ventilation, the duration of weaning and the length of stay in the ICU without having an impact on the mortality and morbidity of the patient [24], as well as a significant reduction in costs [25-27]. The use of protocols brings efficacy to daily clinical practice and avoids individual judgment based on own experience, which in turn allows to reduce the variability in the disconnection process [4,8,28] with patients with similar characteristics.
The role of the nurse in this context has been considered relevant [4,5,8,15,25,29-32] and beneficial. However, it is difficult to find a definite guideline for the extubation process [24] and it continues to be an issue in which there is a lack of consensus [4] since the optimal timing and technique continue to be the subject of debate by professionals, reason why research in this field is justified.
The objective of the study we present is to know if the use of a standardized weaning protocol, carried out in a multidisciplinary way from the beginning of the process, reduces the connection time to the mechanical ventilator in critical patients compared to another group of patients who are disconnects without the application of a standardized protocol with exclusively clinical criteria. Secondary objectives are to compare the reintubation rates, the duration of the weaning process and the days of stay in the ICU between the two groups of patients.
Material and Method
A case-control study was conducted in the Critical Surgical Care Unit of the Elche General Hospital and the Alicante General Hospital, consisting of 9 beds and 12 beds respectively for critical surgical patients. The protocol was validated at the Elche Hospital [4] so that the same protocol was used as a validated tool for this study.
The work was approved by the ethics committees of both hospitals, and informed consent was obtained from the relatives of the patients who were part of the control group according to the indications of the ethics committee. In the group of cases, this consent was not required since the protocol was already consolidated in the center, and it was the only way to proceed with the patient.
Before starting the study, three one-hour meetings were held at the Alicante Hospital whose patients were to be part of the control group, where all the personnel who participated were explained what the study consisted of and what the objectives set. A specific logbook for data collection was prepared for this centre and aspects about its proper completion as the only information gathering tool were discussed. Only one hour-long meeting was held at the General Hospital of Elche since the pilot study had already been carried out previously and the data collection logbook had been worked on, so the staff was already trained with the study.
The inclusion criteria were all patients over eighteen years of age who underwent surgery admitted to both units, who required IMV for a time greater than or equal to twenty-four hours and who were subsequently extubated and whose family members had also signed the informed consent prepared for this purpose. Patients who died during the IMV period and patients with tracheostomy ventilation were excluded.
A total of ninety-one patients who met the inclusion and exclusion criteria were part of the study. In the control group, the patient was extubated according to the usual clinical practice where there was no previously standardized protocol and the procedure was carried out according to the individual criteria of the responsible physician. In the group of patients at the Elche General Hospital, the patient was extubated following the protocol created for this purpose and designed specifically for this study (Figure 1). The data of both centers were obtained during the period of time between January 1, 2016 and December 1, 2019.
The variables studied were the same as those used in the pilot study conducted at the Elche General Hospital. As sociodemographic variables: age and sex; as outcome variable the time of invasive mechanical ventilation; as explanatory variables: presence of comorbidities measured as Charlson comorbidity index value [33], length of stay in the unit, time spent in weaning, reintubations, time until the weaning process begins from the patient’s admission, anesthetic risk classification (ASA) (American Society of Anesthesiologists) and Acute Psysiology and Chronic Haealth Evaluation (APACHE) II. In addition, the indicator SAPPS (Simplified Acute Physiology Score) III was added as a variable in both groups.
The statistical package Statical Package for the Social Science (SPSS) 26.0 was used to analyze the data. For the analysis and comparison of continuous quantitative variables such as total IMV time, stay in days or weaning time, Student´s T test, and they were expressed as mean ± standard deviation (SD). For the analysis of qualitative variables such as sex or reintubations, contingency tables were made and the Fisher test or the Chi-square test were used, finally expressed as a percentage. In addition, correlation tests were performed between the IMV time variable and the rest of the study variables using the Pearson test to correlate numerical variables when at least one of them followed a normal distribution, or the Spearman’s test if none had a normal distribution. A value of p<0.05 was considered statistically significant.
Results
The study included a total of ninety-one patients, fifty belonging to the group in which the protocol was applied (Elche Hospital) and forty-one belonging to the group without standardized protocol (Alicante Hospital). In the group of cases, 2 patients were excluded because tracheostomy was finally performed. In the control group, 14 patients were excluded because they did not meet the IMV time criteria established prior to the study inclusion. The variables studied and their comparison are shown in Table 1,where the characteristics of the patients and the description of the variables of both groups are observed.

Both groups were comparable in terms of age (p=0,351), sex (p=0,399), ASA classification (p=0,874) and severity according to SAPSS III (p=0,400) without finding statistically significant differences, observing an average age above 60 years (66,92 ± 17,143 vs 63,54 ± 17,122), with a predominance of male sex (54% vs 63,4%) and with an ASA classifier that reaches a value of 3 on a scale of 5 points in both samples (2,83±0,975 vs 2,80±0,901).
The type of surgery performed on the patient was different in both groups (p=0,001), with general surgery interventions being predominant compared to the rest of specialties (62% vs 43,9%), followed by neurosurgery interventions (16% vs 26,8%). In the CCI, significant differences were also found (p=0,001), obtaining higher values in the control group (2,84 ± 2,721 vs 4,72 ± 2,613).
As to the variables most closely related to IMV, significant differences were found in weaning in hours (p<0,01), the total time the patient spends connected to IMV (p=0,048) and reintubations (p=0,021). During weaning, measured in hours, a significant decrease in the time used with the application of the protocol was observed (2,40 ± 1,43 vs 41,250 ± 51,60) compared to the usual clinical practice; something that affected the variable total IMV time (p=0,048), achieving a reduction of approximately 31 hours (85,29 ± 46,72 vs 116,92 ± 94,39). The time it takes to start weaning from the patient’s admission was not affected by the use of the protocol, without differences between the two samples (p=0,981), something similar happened in terms of the patient’s hospital stay in the ICU (p=0,855).

*CCI= Charlson comorbidity index; ☨ASA= American Society of Anesthesiologists; ‡ SAPS III= Simplified Acute Physiology Score III; § IMV= invasive mechanical ventilation
The ventilatory mode with which the patient was connected to the IMV varied between both groups according to the application of the multidisciplinary protocol or the extubstantiation according to the individual criteria of the physician, finding important differences in this aspect (Table 2). In the protocol group, the ventilatory modality to which the patient was connected once IMV started was Assisted/Controlled (A/C) in 100% of the cases, while in the control group this mode was used in the 56,1% of patients. When it was determined that the patient was ready to begin weaning, it was changed to spontaneous mode (ESP) in 100% of the patients in the case group, while in the control group there was more variability in this respect, with Synchronised Intermitent Mandatory Ventilation (SIMV) being more predominant (43,9%). When using oxygen in T, differences were also observed (100% vs 9,8%), occurring in the same way when carrying out reductions in support pressure where, in the case of controls, most were performed according to medical criteria while in the group of cases the pattern established in the protocol was followed (100% vs 39%). It should be noted that in the control group most of the patients (36,58%) were extubated using only decreases in support pressure, while in the case group, 100% of the patients initially used decreases in support pressure followed by the use of oxygen in T.
The variables that were most related to the IMV time in the group with the protocol were age in years (p=0,032), the time it takes to start weaning from the patient’s admission to the unit (p≤0,01) and reintubations (p≤0,01) as shown in Table 3. In the control group, stay in days (p≤0,01) and the time it takes to start weaning from the patient’s admission to the unit (p≤0,01).
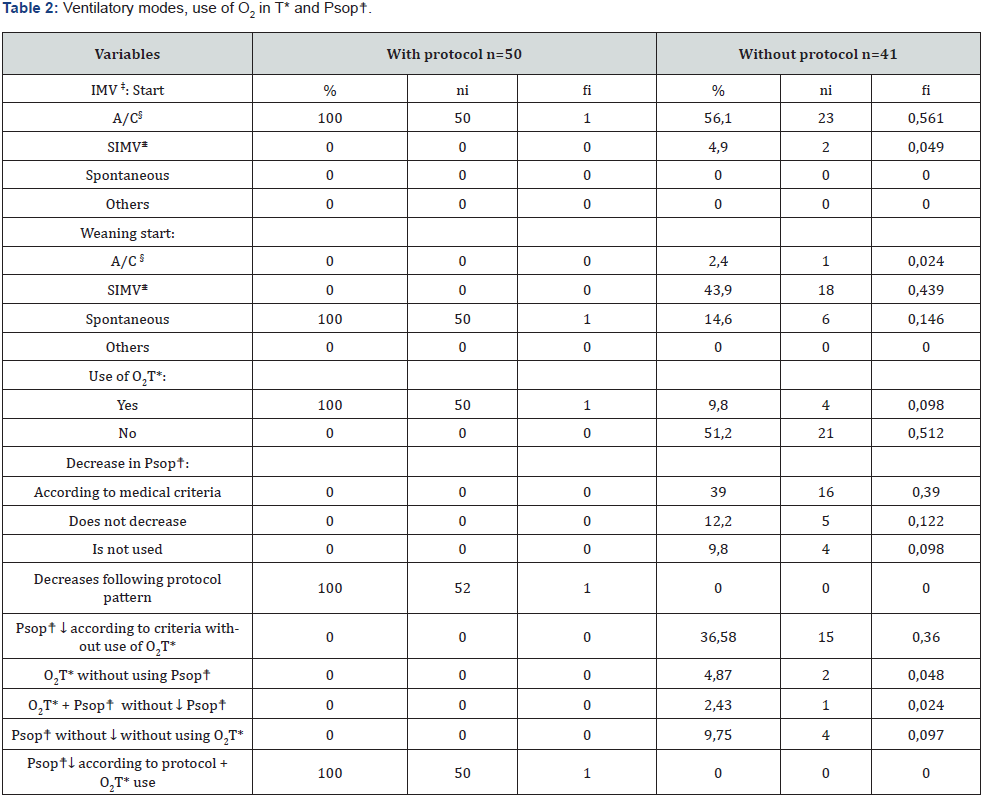
*O2T=oxygen with T-piece; ☨Psop= support pressure; ‡IMV= invasive mechanical ventilation; §A/C= Assisted/controlled; ⩨SIMV= synchronized intermittent mandatory ventilation.
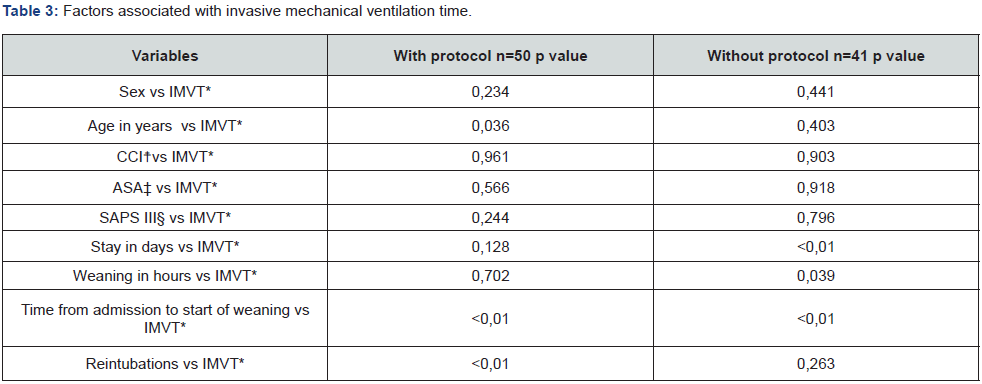
*IMVT= invasive mechanical ventilation time; ☨CCI= Charlson Comorbidity Index; ‡ASA= American Society of Anesthesiologists; §SAPS III= Simplified Acute Physiology Score III.
Discussion
The work carried out tries to evaluate whether the implementation of a protocol is really effective assumed by a medical-nurse team within the IMV disconnection process, and therefore, if its inclusion can achieve improvements in care, in contrast to the usual clinical practice where all the weight of the process falls on the responsible doctor and on his own individual clinical judgment. To achieve this goal, it is necessary to implement a standardized protocol based on scientific evidence where the individual judgment of each professional does not affect the care provided to the patient, and therefore, does not contribute to the appearance of certain clinical variability in patients with similar characteristics. In this case, the protocol that is applied is adapted to the conditions of the critical surgical patient and its approach from a multidisciplinary point of view where the joint work between the doctor and the nurse is clearly reflected in its algorithm.
The use of disconnection protocols has been beneficial in the literature to reduce hospital stay [1,8,11,15,24], reflecting figures of around 11% [15]. The review carried out by Hirzallab et al. [8] showed that, thanks to the use of protocols led by nurses, it was possible to reduce the length of stay compared to the usual care provided by the doctor; data that conflict with those obtained by other authors such as Sephayar et al. [29], who obtained a shorter mean hospitalization but without statistically significant differences when comparing both groups. In our case, it was also not possible to reduce the ICU stay, something that could be due to the influence of other factors independent of the respiratory failure itself and which have repercussions on the discharge of the patient, such as the need to request tests prior to discharge or the physician’s conservative attitude due to the associated comorbidities of the surgical patient. It should be noted that the increase in stay was not correlated with the increase in IMV time in the protocol group, but nevertheless it did correlate in the control group, thus indicating that the variable IMV time had more representativeness in the control group and that in the group with protocol the reasons for the lengthening of the stay could be other different.
The time it takes to start the weaning process from the time the patient is admitted until he is ready to be extubated did not vary either when comparing both groups. In the previous pilot study, there was an important difference between the prospective and retrospective cohorts; being this much longer the time it took in the prospective group. This difference was probably produced by the fact that when applying a protocol, a series of very rigid criteria were taken into account to assess whether the patient was a candidate, which were not taken into account in the group without protocol, thus reducing the times. In this case, the absence of statistical significance could be indicating that, although a standardized protocol is not applied in the control group, the same parameters described in the literature could be assessed. Furthermore, a correlation was also observed between IMV time and the time it takes to start the weaning process in both groups. In previous works, this variable has not been compared, so it has not been possible to make the comparison and discussion.
In studies previously carried out [6,20,25], positive results were obtained regarding the importance of the nurse when assessing the patient and their ability to successfully overcome the weaning process. Sephayar et al. [29] indicate that, thanks to the nurses’ assessment, the inconveniences of using IMV can be reduced, which leads to timely weaning; considering the nurse’s judgment as relevant when preparing for safe and effective weaning. In the Cochrane review [15], it was possible to reduce the duration of weaning by 70% thanks to the application of protocols, stating that they can also train the nurse to start the process early, identifying more quickly the patients who are ready to your start; similar data to those found in the review by Hirzallab et al. [8] where the time was reduced from 47 hours to 25 hours. The results obtained in the previous bibliography are in line with those found in our work, where the weaning time was significantly reduced in the case of the application of the protocol, reducing the times from 41 to 2 hours approximately. This difference is determined by the inclusion of the nurse in the process, where all the changes made at the ventilatory level take place step by step according to the indications without the need to wait for the assessment of the responsible physician; something that makes the disconnection much more agile and allows the patient not to stay connected to the ventilator longer than necessary. In the protocol group, there was no significant correlation between the time spent in weaning and the total duration of IMV, something that did not occur in the control group, probably because in the latter group the time spent in weaning is much longer, being a variable oof great importance and the most influential when measuring IMV times.
The total time that the patient spends connected to the IMV is lengthened in the case of the control group; something that has already been published in previous studies where, with the application of protocols, it was possible to reduce the ventilatory time by 26% [15] compared to the usual clinical practice. According to Ward et al. [28], ventilatory time can be reduced from 7 to 3 days with the application of disconnection protocols. Authors such as Hirzallab et al. [8] explain that the use of these tools can increase the autonomy of nurses and at the same time reduce mechanical ventilation times; similar statements were also made by other authors such as Atefeh et al. [31], who managed to reduce the time by approximately 13 hours with the use of nurseled protocols. In our case, we managed to reduce the total IMV time by more than 31 hours compared to the group without a protocol, times more than significant if we consider the high complications that the patient may suffer from lengthening ventilatory times. In addition, it must be considered that the shortening of the time did not have a negative impact on the need for reintubations, which are more numerous in the case of patients without protocol, difference that can be explained by the fact of following a very explicit a very explicit guideline in the extubation process without skipping any step that could lead to a poor assessment of the preparation of the patient to be definitely weaned. According to previously published studies, the use of weaning protocols has been observed to be effective for rapid extubation [1,19], finding a significant relationship between the nurse’s influence and the success in the removal of the tube [30], achieving reductions in reintubations [29]. In the Cochrane review [15], reintubations were reduced from 10% to 8% with the use of protocols; in our case, the reduction ranged from 17% to 2% with the use of a nurse-directed protocol.
The main differences in the disconnection process between the two compared samples are determined by the application of the designed protocol. In the previous bibliography, it is indicated that the SIMV mode is not recommended for prolonged weaning since it can cause fatigue and muscle overload with the consequent increase in days of mechanical ventilation [1-4], which is why it was ruled out in our protocol, observing here differences in the control group, where the SIMV mode is used only in 4,9% of the patients who start mechanical ventilation but nevertheless, it is subsequently used in 43,9% of the patients once they are consider candidates for weaning. Training of the respiratory muscles can be achieved by gradually decreasing the support pressure on the respirator, usually up to 8 cm H2O [1], or by using a T-piece to supply oxygen to the patient. Authors such as Hernández-López et al. [21] indicate that there is a problem when it comes to knowing whether the spontaneous breathing test should be performed with a T-tube or with decreases support pressure, the first one having lower sensitivity and better specificity when identifying a possible reintubation. In any case, the weaning period should not exceed 120 minutes [17,21,22,26,34-38], something that was reflected in the protocol group, not happening in the control group, where the weaning time is much higher. In most patients in the control group, the support pressure with decreases according to medical criteria was used at the time of weaning. while in the group of cases both techniques were used to ensure correct extubation. According to the work carried out by Chittawatanarat et al. [22], where they compared the use of the T-piece and the decreases in support pressure in the spontaneous breathing test in patients underwent surgery, the use of support pressure led to a greater number of disconnection attempts, but once achieved, reintubation was greater in weaned group with T-piece.
Although the results obtained in our work follow the same line as the previously consulted bibliography, there are some differences that make it not similar in its entirety. In most of the works consulted, the importance of the application of a weaning protocol to achieve improvements in the patient connected to the IMV is mentioned, but in very few of them speak about the importance of the nurse within this context and the need to approach the process from a multidisciplinary point of view; something that is considered of maximum relevance in our work. This is perhaps the main difference with previous studies; but it is also important to note that our sample consists exclusively of surgical patients, something that does not happen in the rest of publications where mixed units are mentioned in which there are patients who have undergone surgery and others who, on the contrary, have not specified it. The fact of working with surgical patients implies having to adapt the protocols to certain conditions, such as the fact of needing an upcoming surgery. In addition, the role of the nurse and the doctor in initiating the disconnection process is not described in such detail in any of the papers consulted, describing in such detail the steps to be taken to avoid having to go back once the patient is considered a candidate.
However, in our case, the sample size can be indicated as a limitation, probably due to the limited size of the units studied and the type of patients that are received in them, which means that they do not meet the mechanical ventilation criterion greater than or equal to 24 hours to be included in the study.
Conclusion
With the implementation of a disconnection protocol carried out in a multidisciplinary way, the time spent in weaning, the time of invasive mechanical ventilation and the reintubation figures can be reduced without observing negative consequences on the patient’s health.
The inclusion of the advanced practice nurse in such complex procedures should be considered an important aspect to achieve comprehensive and quality care that is adapted to the needs of the patient.
Acknowledgements
To the General University Hospital of Elche and to all the staff of the Surgical Critical Care Unit for their involvement in the project. To the General University Hospital of Alicante and to all the staff of the Resuscitation Unit, with special mention to Dra Dra Marı́a Galiana and the nurse Pilar Donate.
Conflict of Interests
There are no conflicts of interest or economic interests.
References
- Schönhofer B, Geiseler J, Dellweg D, Fuchs H, Moerer O, et al. (2020) Prolonged Weaning: S2k Guideline Published by the German Respiratory Society. Respiration 1-102 doi: 10.1159/000510085.
- Oliveira SMR, Novais RMF, Carvalho AAS (2019) Impact of a ventilatory weaning protocol in an intensive care unit for adults. Texto Contexto Enferm 28.
- Chung W-C, Sheu C-C, Hung J-Y, Hsu T-J, Yang S-H, et al. (2020) Novel mechanical ventilator weaning predictive model. Kaohsiung J Med Sci 36(10): 841-849.
- Sánchez-Maciá M, Miralles-Sancho J, Castaño-Picó MJ, Pérez-Carbonell A, Maciá-Soler J (2019) Reduction of ventilatory time using the multidisciplinary disconnection protocol. Pilot study. Rev. Latino-Am. Enfermagem 27: e3215.
- Guilhermino MC, Inder KJ, Sundin D (2018) Education on invasive mechanical ventilation involving intensive care nurses: a systematic review. Nurs Crit Care 23(5): 245-255.
- Sandoval Moreno LM, Casas Quiroga IC, Wilches Luna EC, García AF (2019) Efficacy of respiratory muscle training in weaning of mechanical ventilation in patients with mechanical ventilation for 48hours or more: A Randomized Controlled Clinical Trial. Med Intensiva (Engl Ed) 43(2): 79-89.
- Sosa-Medellín MA, Marín-Romero MC (2017) Extubación fallida en una unidad de cuidados intensivos de la Ciudad de México. Med Int Méx 33(4): 459-465.
- Hirzallah FM, Alkaissi A, do Céu Barbieri-Figueiredo M (2019) A systematic review of nurse-led weaning protocol for mechanically ventilated adult patients. Nurs Crit Care 24(2): 89-96.
- Baptistella AR, Sarmento FJ, da Silva KR, Baptistella SF, Taglietti M, et al. (2018) Predictive factors of weaning from mechanical ventilation and extubation outcome: A systematic review. J Crit Care 48: 56-62.
- Shrestha GS (2017) Point-of-care ultrasonography and liberation from mechanical ventilation. Crit Care 21(1): 54.
- Jung B, Vaschetto R, Jaber S (2020) Ten tips to optimize weaning and extubation success in the critically ill. Intensive Care Med 46(12): 2461-2463.
- Rizzo JA, Haq M, McMahon RA, Aden JK, Brillhart DB, et al. (2021) Extubation Failure in a Burn Intensive Care Unit: Examination of Contributing Factors. J Burn Care Res 42(2): 177-181.
- Kerlin MP, Small D, Fuchs BD, Mikkelsen ME, Wang W, et al. (2021) Implementing nudges to promote utilization of low tidal volume ventilation (INPUT): a stepped-wedge, hybrid type III trial of strategies to improve evidence-based mechanical ventilation management. Implement Sci 16(1): 78.
- Burns KEA, Raptis S, Nisenbaum R, Rizvi L, Jones A, et al. (2018) International Practice Variation in Weaning Critically Ill Adults from Invasive Mechanical Ventilation. Ann Am Thorac Soc 15(4): 494-502.Erratum in: Ann Am Thorac Soc (2018) 15(7): 894.
- Blackwood B, Burns KEA, Cardwell CR, O'Halloran P (2014) Protocolized versus non-protocolized weaning for reducing the duration of mechanical ventilation in critically ill adult patients. Cochrane Database Syst Rev (5): CD006904. DOI: 10.1002/14651858.CD006904.pub3.
- Dres M, Estellat C, Baudel JL, Beloncle F, Cousty J, et al. (2021) Comparison of a preventive or curative strategy of fluid removal on the weaning of mechanical ventilation: a study protocol for a multicentre randomised open-label parallel-group trial. BMJ Open 11(8): e048286.
- Zein H, Baratloo A, Negida A, Safari S (2016) Ventilator Weaning and Spontaneous Breathing Trials; an Educational Review. Emerg (Tehran 4(2): 65-71.
- Lewis KA, Chaudhuri D, Guyatt G, Burns KEA, Bosma K, et al. (2019) Comparison of ventilatory modes to facilitate liberation from mechanical ventilation: protocol for a systematic review and network meta-analysis. BMJ Open 9(9): e030407.
- Jansson MM, Syrjälä HP, Ala-Kokko TI (2019) Implementation of strategies to liberate patients from mechanical ventilation in a tertiary-level medical center. Am J Infect Control 47(9): 1065-1070.
- Santibañez-Velázquez M, Medina-García G, Ocharán-Hernández ME (2020) Association of independent risk factors with post-extubation failure in patients undergoing mechanical ventilation weaning. Gac Med Mex 156(6): 539-545.
- Hernández-López GD, Cerón-Juárez R, Escobar-Ortiz D, Graciano-Gaytán L, Gorordo-Delsol LA, et al. (2017) Retiro de la ventilación mecánica. Medicina crítica (Colegio Mexicano de Medicina Crítica) 31(4): 238-245.
- Chittawatanarat K, Orrapin S, Jitkaroon K, Mueakwan S, Sroison U (2018) An Open Label Randomized Controlled Trial to Compare Low Level Pressure Support and T-piece as Strategies for Discontinuation of Mechanical Ventilation in a General Surgical Intensive Care Unit. Med Arch 72(1): 51-55.
- Viruez-Soto José Antonio, Tinoco-Solórzano Amílcar, Cerezo Gonzales Julian (2020) Espacio muerto y destete de ventilación mecánica invasiva en residentes de la gran altitud. Horiz Med 20(4): e958.
- Nitta K, Okamoto K, Imamura H, Mochizuki K, Takayama H, et al. (2019) A comprehensive protocol for ventilator weaning and extubation: a prospective observational study. J Intensive Care 7: 50.
- Starnes E, Palokas M (2017) Nurse initiated protocols for spontaneous breathing trials in adult intensive care unit patients: a scoping review protocol. JBI Database System Rev Implement Rep 15(10): 2421-2426.
- Borges LGA, Savi A, Teixeira C, de Oliveira RP, De Camillis MLF, et al. (2017) Mechanical ventilation weaning protocol improves medical adherence and results. J Crit Care 41: 296-302.
- Merjildo DF, García WP, Rabanal CL, Piérola JZ (2019) Mortalidad y factores relacionados al fracaso del destete de la ventilación mecánica en una unidad de cuidados intensivos de Lima, Perú. Rev Med Hered 30(1): 5-11.
- Ward D, Fulbrook P (2016) Nursing Strategies for Effective Weaning of the Critically Ill Mechanically Ventilated Patient. Crit Care Nurs Clin North Am 28(4): 499-512.
- Sepahyar M, Molavynejad S, Adineh M, Savaie M, Maraghi E (2021) The Effect of Nursing Interventions Based on Burns Wean Assessment Program on Successful Weaning from Mechanical Ventilation: A Randomized Controlled Clinical Trial. Iran J Nurs Midwifery Res 26(1): 34-41.
- Sánchez-Isaza, JA, Sáez-Álvarez E, Samudio-Bejarano P (2021) Influencia de la enfermería en el éxito de la extubación en pacientes con ventilación mecánica. Therapeía. Estudios y propuestas en ciencias de la salud. Abril: 141-55.
- Ghanbari A, Mohammad EA, Paryad E, Atrkar RZ, Kazem MM, et al. (2020) Comparison between a nurse-led weaning protocol and a weaning protocol based on physician's clinical judgment in ICU patients. Heart Lung 49(3): 296-300.
- Fagoni N, Piva S, Peli E, Turla F, Pecci E, et al. (2018) Comparison between a nurse-led weaning protocol and weaning based on physician's clinical judgment in tracheostomized critically ill patients: a pilot randomized controlled clinical trial. Ann Intensive Care 8(1): 11.
- Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40(5): 373-383.
- Ambrosino N, Vitacca M (2018) The patient needing prolonged mechanical ventilation: a narrative review. Multidiscip Respir Med 13: 6.
- Mart MF, Brummel NE, Ely EW (2019) The ABCDEF Bundle for the Respiratory Therapist. Respir Care 64(12): 1561-1573.
- Chen L, Gilstrap D, Cox CE (2016) Mechanical Ventilator Discontinuation Process. Clin Chest Med 37(4): 693-699.
- Lin FC, Kuo YW, Jerng JS, Wu HD (2020) Association of weaning preparedness with extubation outcome of mechanically ventilated patients in medical intensive care units: a retrospective analysis. Peer J 8: e8973.
- Bernardes Neto SCG, Torres-Castro R, Lima Í, Resqueti VR, Fregonezi GAF (2021) Weaning from mechanical ventilation in people with neuromuscular disease: a systematic review. BMJ Open 11(9): e047449.






























