Does Timing of Delirium Onset Affect Outcomes in The Critically Ill?
Jennifer P. Booth, PharmD; Daniel S. Eiferman, MD, MBA; Judith A. Tate, PhD, RN; and Claire V. Murphy1*, PharmD
1Department of Pharmacy, The Ohio State University Wexner Medical Center. 410 West 10th Avenue, Columbus, OH 43210, USA.
2Department of Surgery, Division of Trauma, Critical Care, and Burn, The Ohio State University Wexner Medical Center. 410 West 10th Avenue, Columbus, OH 43210, USA.
3College of Nursing, The Ohio State University, 368 Newton Hall, 1585 Neil Avenue, Columbus, OH, 43210, USA.
Submission: March 25 2021; Published: January 27, 2022
*Corresponding author: Claire V. Murphy, PharmD, BCPS, FCCM, Lead Specialty Practice Pharmacist – Critical Care, The Ohio State University Wexner Medical Center, Department of Pharmacy, 410 West 10th Avenue Room
368 Doan Hall, Columbus, OH 43210, Tel: (614) 293-8470; Fax: (614) 293-3165
How to cite this article: Jennifer P Booth, Daniel S Eiferman, Judith Tate, Claire V. Murphy. Does Timing of Delirium Onset Affect Outcomes in The Critically Ill?. A Research Article and Review of The Literature. J Anest & Inten care med. 2022; 11(5): 555821. DOI 10.19080/JAICM.2022.11.555821
Abstract
Introduction: Intensive care unit (ICU) delirium increases morbidity and mortality, but little is known regarding the role timing of development plays.
Objective: To evaluate the effect of timing of ICU delirium onset and identify risk factors for late-onset delirium.
Methods: Clinical outcomes of adult patients with early- and late-onset delirium were compared. A multivariable logistic regression analysis was performed to identify factors associated with late-onset.
Results: A total of 150 patients were included (108 early-onset; 42 late-onset). No difference was observed in ICU length of stay among survivors. In-hospital mortality was significantly higher for late-onset (40.5 vs. 24.1%, p= 0.046). Surgical ICU admission increased risk of late-onset (AOR 3.71, p=<0.001), while hypertension (AOR 0.40, p=0.021) and prehospital antidepressant use (AOR 0.28, p=0.002) reduced risk.
Conclusion: While less common, late-onset delirium was associated with higher mortality risk. Future research should focus on preventative strategies in patients at risk for late-onset delirium.
Keywords:Delirium, Intensive care units, Critical care, Critical care outcomes, Risk factors, Neurocognitive disorders
Abbreviations:ICU: Intensive Care Unit; LOS: Length of Stay; CAM-ICU: Confusion Assessment Method for the ICU; REDCap: Research Electronic Data Capture; IQR: Interquartile Range
Introduction
Delirium is a common consequence of critical illness, with prevalence of 31.8-87% for patients admitted to the intensive care unit (ICU) and approximately 80% for mechanically ventilated ICU patients [1-3]. Delirium is associated with longer hospital and ICU lengths of stay (LOS), increased mortality, higher healthcare costs, increased mechanical ventilation requirements, and cognitive impairment after discharge [1-3]. Known risk factors for ICU delirium include age, illness severity, alcohol abuse, hypertension, dementia, and respiratory disease [2-4]. Processes of care during ICU admission that may increase risk of delirium include mechanical ventilation and inpatient administration of benzodiazepines, sedatives, and analgesics [1,2,4].
While there has been a significant focus on the identification of risk factors for delirium, few studies have described the timing of delirium onset. Regal and colleagues reported that 95.8% of delirium studies documented diagnoses without timing of onset [5]. Of available studies that report timing of onset, one study reported a mean time to onset of ICU delirium as 1.5-1.7 days which was corroborated by Lin and colleagues who found that nearly half of delirium onset occurred on the second day after admission to the ICU [6,7]. Overall, the number of studies analyzing the time to onset of delirium is sparse and with significant limitations.
Therefore, this study aims to evaluate the effect of timing of ICU delirium onset on patient outcomes and identify any associated risk factors relative to timing. Understanding the effect of timing of onset may guide management of ICU delirium and assist clinicians with appropriate risk stratification including the development of targeted delirium prevention protocols.
Materials and Methods
Study Design and Patient Population
A single-center, retrospective analysis of adult patients with ICU delirium was conducted at a tertiary care, academic medical center. Adult patients between the ages of 18 to 89 years who were admitted to the medical or surgical ICU for at least 48 hours and subsequently developed ICU delirium between January 1, 2016 and December 31, 2016 were eligible for inclusion. Diagnosis of delirium was defined by the documentation of a positive Confusion Assessment Method for the ICU (CAM-ICU) at any time point during ICU admission. Onset of delirium was defined as the time from ICU admission to the first documented positive CAMICU. Early-onset delirium was defined as an onset of delirium less than or equal to 24 hours of ICU admission, whereas late-onset delirium was defined as an onset of delirium greater than 24 hours from ICU admission. Patients were excluded if delirium developed before ICU admission, CAM-ICU status was documented as “unable to assess” throughout the first 24 hours of ICU admission, or if they were pregnant, incarcerated, or admitted to the neurocritical care unit. If a patient met criteria for evaluation on more than one hospital admission, only the first admission was included for evaluation; whereas if a patient had multiple ICU admissions during the index hospitalization, they were excluded from evaluation.
Patients who developed early-onset ICU delirium were compared to those who developed late-onset ICU delirium with a primary outcome of ICU LOS among survivors. Secondary outcomes included hospital LOS among survivors, all-cause hospital mortality, and discharge disposition.
Data collection
Patients were randomly selected using a random number generator from an electronic report of ICU admissions during the study period and were then screened for inclusion and exclusion criteria. Patients were screened until 150 met inclusion criteria for evaluation. For patients meeting criteria, de-identified data was then entered and managed using the secure, web-based application, REDCap (Research Electronic Data Capture) [8].
Data collection included date and time of delirium diagnosis, date and time of hospital and ICU admission and discharge, demographic information, social history including concurrent substance (alcohol, tobacco, and illicit drug) use, reason for ICU admission, ICU type, past medical history, and home medications prior to admission. Past medical history was based on documentation within the provider notes and included: anemia, chronic kidney disease, chronic respiratory disease (chronic obstructive pulmonary disease, asthma), cognitive impairment (Alzheimer’s disease, dementia, Parkinson’s disease, mental retardation and developmental disability), diabetes mellitus, heart disease (coronary artery disease, congestive heart failure), hypertension, liver disease, mental disorder (attention-deficit/ hyperactivity disorder, anxiety, bipolar, depression, schizophrenia, obsessive-compulsive disorder, posttraumatic stress disorder), obesity (body mass index > 30 kg/m2), vision/hearing impairment, and vitamin/mineral deficiency. Home medications were collected based on the reconciled prior to admission medication list within the electronic medical record. Home medications collected included those that are known to have action on the central nervous system such as anticholinergics, anticonvulsants, antidepressants, antipsychotics, baclofen, barbiturates, benzodiazepines, clonidine, gabapentin, mirtazapine, opioids, pregabalin, steroids, trazodone, and z-hypnotics.
Statistical analysis
Categorical variables are presented as frequency (percentages) and were compared using the Pearson chi-square. Continuous variables were summarized by mean + standard deviation for normally distributed data or median [interquartile range (IQR) 25-75%] for non-normally distributed data and were compared using the student’s t-test or Wilcoxon rank-sum test respectively. All tests were two-tailed, and a p value < 0.05 was determined to represent statistical significance. After univariable analysis, a backwards, stepwise, multivariate logistic regression was performed to determine independent risk factors for lateonset ICU delirium. Variables significant at the 0.20 level in the univariable analysis were included in the multivariable logistic regression model. All statistical analyses were performed using SPSS version 24.0 for Windows (SPSS, Inc., Chicago, IL).
This study was granted exempt status by the institutional review board of The Ohio State University (Study #2018E0478).
Results
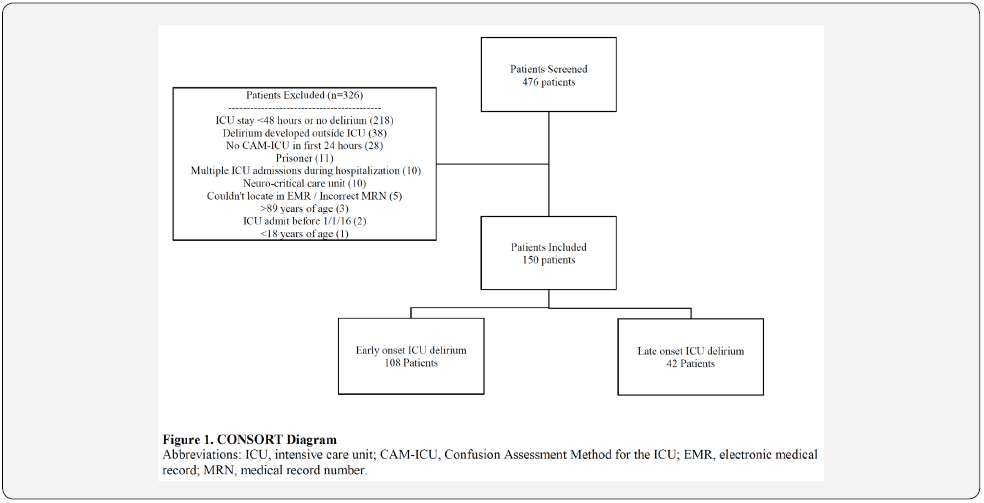
A total of 2,550 patients were eligible for screening, from which 476 randomly selected patients were screened to obtain 150 eligible patients for evaluation (Figure 1). Early-onset ICU delirium was observed in 108 patients (72%), and late-onset ICU delirium in 42 patients (28%). The primary reasons for exclusion were an ICU LOS of less than 48 hours and lack of delirium development (n=326).
Baseline characteristics including age, race, reason for ICU admission, and current substance abuse were similar between both groups (Table 1); however, the early-onset group had a lower proportion of males and were more likely to be admitted to the medical ICU. Significant differences were observed between groups with regards to comorbidities and prescribed medications prior to hospitalization. All of the following were observed at a significantly higher frequency in the early-onset group compared to the late-onset group: past medical history of hypertension and prior to admission antidepressant, benzodiazepine, gabapentin or pregabalin.
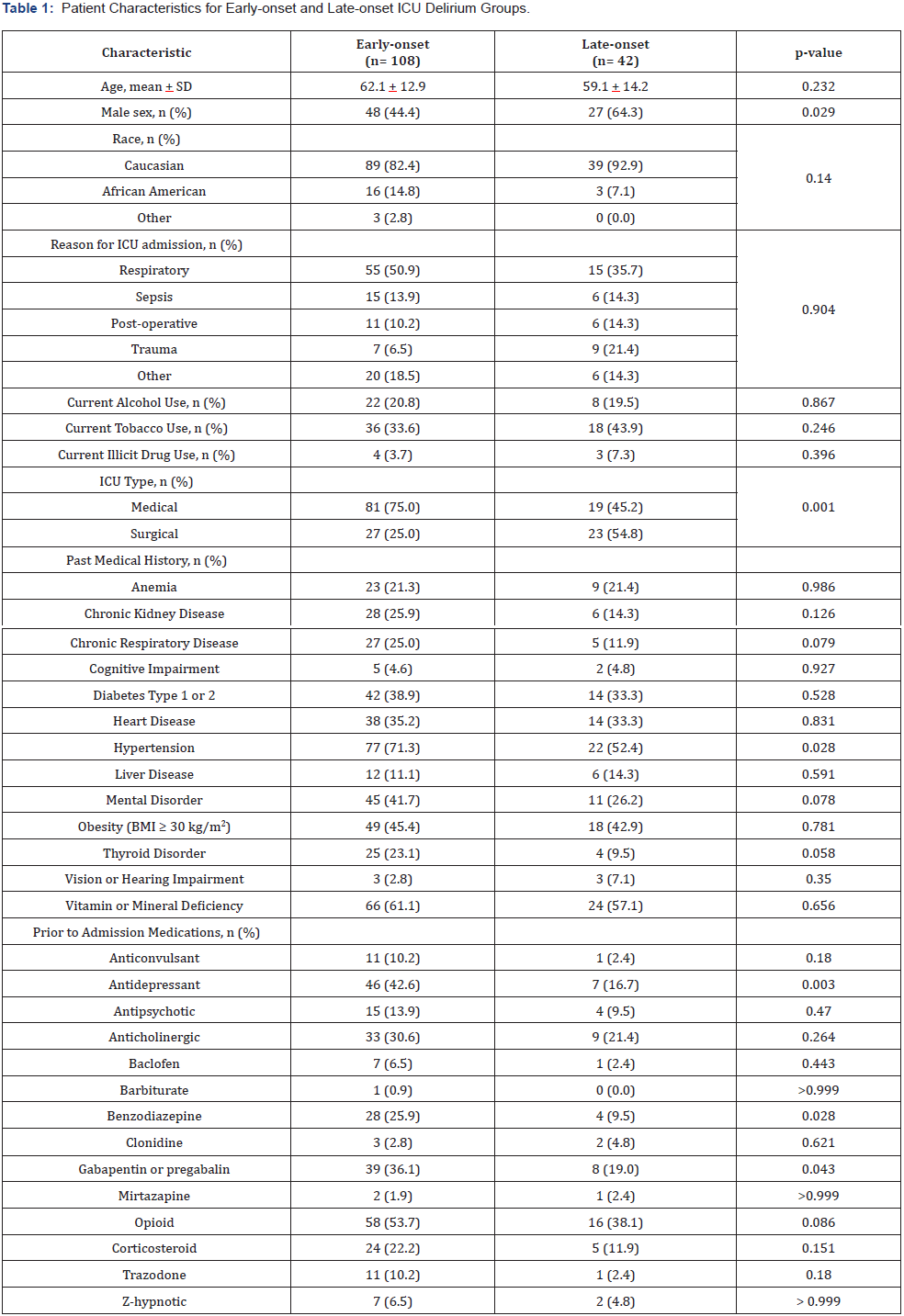
Abbreviation: BMI, body mass index.
The median time to delirium onset from hospital admission was 43.5 hours (13.3-107.6) for the early-onset group and 88.9 hours (47.3-173.3) for the late-onset group; whereas the median time to delirium onset from ICU admission was 1.8 hours (0.2- 10.6) for the early-onset group and 49.5 hours (35.5-86.1) for the late-onset group (Table 2). There was no significant difference in the primary outcome, ICU LOS among survivors, or secondary outcomes: hospital LOS among survivors and discharge disposition. However, in-hospital mortality was significantly higher for the late-onset delirium group (Table 2).
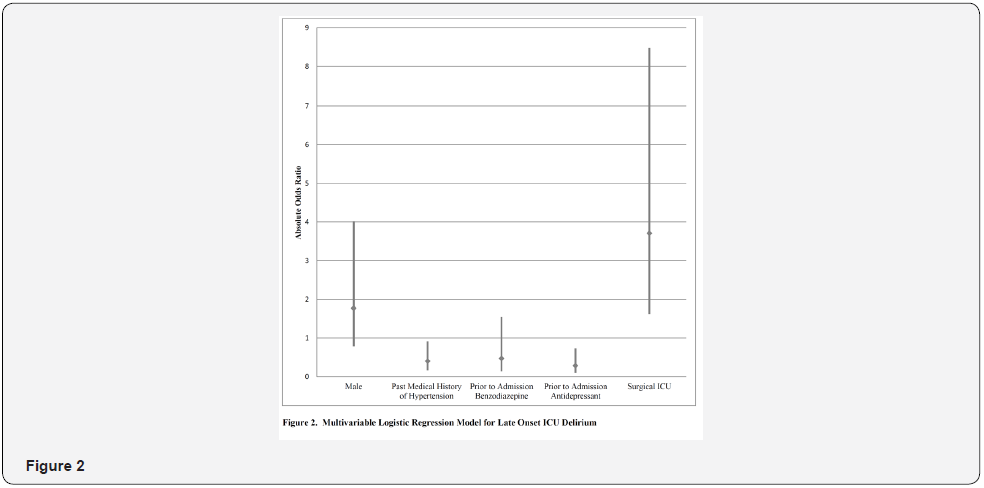
After adjusting for male sex and prior to admission benzodiazepine use, the following factors were significantly associated with late-onset delirium (Figure 2): surgical ICU admission (AOR 3.71, 95% CI 1.62-8.48, p<0.001), past medical history of hypertension (AOR 0.40, 95% CI 0.17-0.91, p=0.021) and prior to admission antidepressant use (AOR 0.28, 95% CI 0.10-0.73, p=0.002).
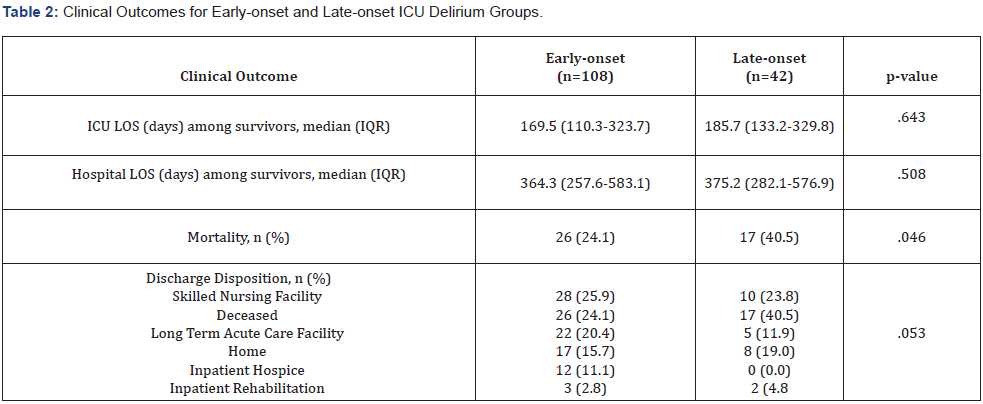
Abbreviations: ICU, intensive care unit; LOS, length of stay; IQR, interq
Discussion
Early-onset delirium was more prevalent in this cohort of patients that developed delirium during their ICU admission, with 72% developing delirium within the first 24 hours of ICU admission. In-hospital mortality was significantly lower among this population compared to those with late-onset delirium, suggesting that the timing of ICU delirium may affect clinical outcomes. Admission to the medical ICU, past medical history of hypertension, and prior to admission antidepressant use were independent predictors of the development of earlyonset delirium; whereas admission to the surgical ICU was an independent predictor of late-onset delirium.
To the best of our knowledge, this is the first study to compare early and late-onset ICU delirium across a heterogenous population of medical and surgical ICUs patients in order to identify risk factors and effects on clinical outcomes. Our results are similar to Kim and colleagues who found that surgical patients who developed post-operative delayed delirium (>5 days following surgery) were associated with significantly longer duration of delirium and hospital LOS as compared to medical ward and postoperative delirium patients (within 5 days) [9].
Previous studies have dichotomized delirium at ICU admission at 24 hours and at 5 days to investigate the timing of delirium and its effect on outcomes [7,9-12]. Although there is no widely accepted definition distinguishing early and late-onset delirium, our interquartile ranges for early-onset (0.2-10.6 hours) and lateonset (35.5-86.1 hours) suggest the existence of a natural gap at a point in time between 12 and 36 hours. McCusker and colleagues defined prevalent and incident delirium at admission in their prospective cohort study [10]; however, this definition would not have been appropriate for our retrospective study as it would not have captured those who developed delirium shortly after ICU admission and/or those that were not assessed with CAM-ICU immediately upon admission. Shu-Min Lin and colleagues only reported results for an early-onset delirium group, defined as development within five days of ICU admission [7]; whereas this definition would not have been appropriate for the current study as only four patients in our study developed delirium later than five days into their ICU stay. In other words, five days is likely to capture most cases of delirium and is not a useful cutoff for early versus late-onset. Overall, our results are similar to the available studies that report timing of delirium onset, in which the majority of delirious patients in our study presented within the first 48 hours of ICU admission.
Our results suggest that medical ICU patients with more comorbidity may be predisposed to early-onset delirium, whereas surgical ICU patients tend to develop delirium later in their ICU stay. We believe there are several plausible explanations for these findings. First, late-onset delirium in surgical ICU patients may be multi-factorial and secondary to post-operative complications, also explaining the significantly higher in-hospital mortality in these patients. In other words, development of late-onset delirium may serve as a marker of deterioration in the surgical ICU. This is corroborated by a retrospective observational study of postoperative surgical ICU patients by Lee and colleagues that reported greater ICU LOS, hospital LOS, and mortality with late brief (for <1 day after post-operative day 0) and persistent delirium (for ≥1 days), compared to early brief (for <1 day on post-operative day 0) or no delirium [13]. Next, the inflammatory or septic state of many medical ICU patients and/or higher comorbidity at admission may contribute to the pathophysiology of early-onset of delirium development in these patients [9,14]. Finally, early-onset delirium was also significantly more common in patients with antidepressants, benzodiazepines, and gabapentin or pregabalin as prior to admission medications suggesting that the affects from these neuropsychiatric medications may play a role in the development of early-onset delirium [15].
Currently, there is no recommended pharmacological agent for the treatment of delirium [16]. Instead, non-pharmacologic prevention and management strategies remain the focus of ICU delirium management protocols within ICU liberation bundles. We believe that recognition of the differences between early and late-onset delirium may assist clinicians with improved risk stratification and the development of targeted delirium prevention protocols for high-risk patients. By targeting prevention efforts based on risk, patients most vulnerable to the development of delirium may benefit even when resources are limited. Recommended prevention strategies include multi-component non-pharmacologic strategies to optimize mobility, sleep, hearing, and vision [16]. Our results suggest that early-onset delirium may be refractory to prevention due the limited amount of time for ICU protocols and interventions to impact delirium development. Therefore, the focus of delirium management strategies should be on resolution of early-onset delirium and prevention of late-onset delirium.
Limitations of this study include the retrospective study design including the reliance of data collection from the electronic medical record, limited sample size, and lack of a widely accepted definition to distinguish between early and late-onset delirium [17]. Patients admitted to the neuro-critical care unit were excluded due to the challenges associated with assessing delirium in this population; however, patients with traumatic brain injury were not explicitly excluded. Additionally, the configuration of our critical care service separates medical ICU and surgical ICU patients; however, we recognize many ICUs combine both patient populations. The heterogeneity of these two patient populations limits the generalizability of our study and the conclusions that can be drawn from this cohort; however, we believe this also to be a strength as it allowed us to explore potential differences between two distinct patient populations with inherently different timelines throughout their ICU LOS.
Conclusion
Early-onset delirium was common among ICU patients with delirium. Patients in the medical ICU, with hypertension, or on antidepressants prior to admission were more likely to develop early-onset delirium. In-hospital mortality was lower in earlyonset delirium, suggesting that timing may affect clinical outcomes. Additional research is needed to analyze medical and surgical ICU patients separately to further explore the differences between early and late-onset delirium. Better understanding of the role of delirium timing may help guide ICU delirium prevention and management and improve clinical outcomes.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
References
- Cavallazzi R, Saad M, Marik PE (2012) Delirium in the ICU: an overview. Ann Intensive Care 2(1): 49.
- Jones SF, Pisani MA (2012) ICU delirium: an update. Curr Opin Crit Care 18(2): 146-151.
- Ouimet S, Kavanagh BP, Gottfried SB, Skrobik Y (2007) Incidence, risk factors and consequences of ICU delirium. Intensive Care Med 33(1): 66-73.
- Van Rompaey B, Schuurmans MJ, Shortridge-Baggett LM, Truijen S, Bossaert L (2008) Risk factors for intensive care delirium: a systematic review. Intensive Crit Care Nurs 24(2): 98-107.
- Regal PJ (2017) Delirium, in 405 articles of medical (non-surgical or ICU) inpatients: unproven speed of onset and recovery. Clin Interv Aging 12: 377-380.
- Wang W, Li HL, Wang DX, Zhu X, Li S-L, et al. (2012) Haloperidol prophylaxis decreases delirium incidence in elderly patients after noncardiac surgery: a randomized controlled trial*. Crit Care Med 40(3): 731-739.
- Lin SM, Huang CD, Liu CY, Lin H-C, Wang C-H, et al. (2008) Risk factors for the development of early-onset delirium and the subsequent clinical outcome in mechanically ventilated patients. J Crit Care 23(3): 372-379.
- Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, et al. (2009) Research electronic data capture (REDCap) – A metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 42(2): 377-381.
- Kim S, Kim JJ, Oh J, Park J, Park JY (2018) Delirium characteristics and outcomes in medical and surgical inpatients: A subgroup analysis. J Crit Care 43: 156-162.
- McCusker J, Cole MG, Dendukuri N, Belzile E (2003) Does delirium increase hospital stay? J Am Geriatr Soc 51(11): 1539-1546.
- Moschetta AL, Silveira CV, Dalacorte RR, Schneider RH, da Silva Filho IG (2009) Time of delirium onset and prognosis amongst Southern Brazilian hospitalized elderly patients. Dement Neuropsychol 3(4): 303-307.
- Kotfis K, Bott-Olejnik M, Szylińska A, Listewnik M, Rotter I (2019) Characteristics, risk factors and outcome of early-onset delirium in elderly patients with first ever acute ischemic stroke - a prospective observational cohort study. Clin Interv Aging 14: 1771-1782.
- Lee H, Ju JW, Oh SY, Kim J, Jung CW, et al. (2018) Impact of timing and duration of postoperative delirium: a retrospective observational study. Surgery S0039-6060(18): 30035-30037.
- Piva S, McCreadie VA, Latronico N (2015) Neuroinflammation in sepsis: sepsis associated delirium. Cardiovasc Hematol Disord Drug Targets 15(1): 10-18.
- La MK, Thompson Bastin ML, Gisewhite JT, Johnson CA, Flannery AH (2018) Impact of restarting home neuropsychiatric medications on sedation outcomes in medical intensive care unit patients. J Crit Care 43: 102-107.
- Devlin JW, SkrobikY, Gélinas C, Needham DM, Slooter AJC, et al. (2018) Clinical Practice Guidelines for the Prevention and Management of Pain, Agitation/Sedation, Delirium, Immobility, and Sleep Disruption in Adult Patients in the ICU. Crit Care Med 46(9): e825-e873.
- Katznelson R, Djaiani G, Tait G, Wasowicz M, Sutherland AM, et al. (2010) Hospital administrative database underestimates delirium rate after cardiac surgery. Can J Anaesth 57(10): 898-902.






























