Mortality Risk Factors of Emergency Surgery in Adults: A Longitudinal Study/b>
Bengono Bengono RS1,2*, Jemea B1,3, Amengle AL1,4, Mbengono Metogo JA1,5, NdikontarR1,4, Nkongo R.A1, Esiene A1,6, Owono E.P1,6 and Ze Minkande J1,4
1Department of Surgery and Specialties, Faculty of Medicine and Biomedical Sciences, The University of Yaoundé, Cameroon
2Department of Anaesthesia and intensive care, Sangmélima Reference Hospital, Cameroon
3Department of Anaesthesia and intensive care, Yaoundé Teaching Hospital, Cameroon
4Department of Anaesthesia and intensive care, Yaoundé Gynaeco-Obstetric and Pediatric Hospital, Cameroon
5Department of Anaesthesia and intensive care, Douala General Hospital, Cameroon
6Department of Anaesthesia and intensive care, Yaoundé Central Hospital, Cameroon
Submission: November 30 2021; Published: January 03, 2022
*Corresponding author: Bengono Bengono Roddy Stephan, Department of Surgery and Specialties, Faculty of Medicine and Biomedical Sciences, The University of Yaoundé, Cameroon
How to cite this article: Bengono B R, Jemea B, Amengle A, Mbengono M J, Ndikontar R, et al. Mortality Risk Factors of Emergency Surgery in 002 Adults: A Longitudinal Study. J Anest & Inten care med. 2022; 11(4): 555819. DOI 10.19080/JAICM.2022.11.555819
Abstract
Background: Emergency surgery is a challenge for the care. The purpose of the study was to study the risk factors for mortality in emergency surgery in adults.
Patients and Methods: It was a longitudinal and prospective study conducted from December 1st, 2017, to April 30th, 2018, in adults operated for a surgical emergency at the Central Hospital of Yaoundé. The variables studied were the operative indication, the operative risk, the anesthesia’s technique, the complications, the risk factors for mortality. These data were analyzed with the Epi info software version 3.5.4 and the logistic regression was done using the Statistical Package for Social Sciences (SPSS) software version 20.0.
Results: We involved 283 patients. Sex-ratio was 0.2. The median age was 30.6 years and extremes of 18 and 83 years. Obstetric and gynecologic surgeries (76.4%) and digestive surgeries (14.8%) were the most frequent. ASA 2 class was the most represented (47.7%). Surgical risk was minor in 78.8% of cases. Intraoperative complications occurred during the maintenance period (77.9%). They were mainly cardiovascular (79.6%). Postoperative complications were predominantly infectious (33.8%). Fourteen deaths were recorded, with a mortality rate of 4.9% and the factors associated with these deaths were age > 65 years (42.9%), ASA class> 2 and the occurrence of complications.
Conclusion: One in 20 patients died during the perioperative period. The risk factors were related to the presence of comorbidities and the anesthesia’s technique. An optimization of the care would improve the management of the surgical emergencies in the adult.
Keywords:Risk Factors; Mortality; Emergency Surgery
Introduction
The management of surgical emergencies in developing countries is often confronted with socio-economic problems, the clinical condition of the patient, the distance from healthcare facilities, self-medication, the lack of health education, late arrival in hospital structures, lack of medical transport, insufficient technical platform and adequate human resources. It is therefore a real challenge [1]. In sub-Saharan Africa, traumatic emergencies are the most frequent, with a predominance of Road traffic accidents [2]. The mortality rate after emergency surgery in adults remains high [3]. Over 3 million postoperative deaths occur worldwide per year. There are multiple methods for predicting which patients are at high risk of death or complications from surgery [4]. In Cameroon, Ngowé et al. [5] in 2007, found a mortality of 8.1% with a predominance of trauma [5]. Perioperative mortality depends on the urgency of the surgery, the type of surgery, the patient’s preoperative condition, the time to treatment and the occurrence of complications [6-8]. Scott John et al in the United States reported that a patient undergoing emergency surgery was eight times more likely to die postoperatively than a patient undergoing elective surgery [9]. With a major postoperative morbidity rate of around 15%, a short-term mortality rate between 1 and 3%, and a reproducible association between shortterm morbidity and long-term survival, the impact of surgical complications on individual patients, healthcare resources, and society at large is clearly evident [4]. The aim of our study was to analyze the risk factors for mortality in emergency surgery.
Patients and Methods
This was a longitudinal and prospective study carried out from December 1, 2017, to April 30, 2018, in adults operated for a surgical emergency at the Yaoundé Central Hospital. After approval from the national ethics committee, was included in our study, any patient over the age of 18, admitted for emergency surgery in an operating room at the Yaoundé Central Hospital, and who have given their consent. The sampling was consecutive. Recruitment was carried out during the anesthetic consultation. The data recorded were the age, the sex, the past history, the operative risk (surgical and anesthetic), the operative indication, the anesthesia technique, the ASA, Altemeier and Boersma classifications. During the intraoperative period, in the operating room, the monitoring parameters (BP, HR, RR, SpO2), the duration of anesthesia, the duration of the surgery, the operative procedure and the intraoperative complications were noted.
The postoperative phase was evaluated in the hospital wards and in the intensive care unit. The data collected were the parameters vital signs (BP, HR, RR, SpO2, state of consciousness, temperature), postoperative complications. Postoperative followup continued until the 30th postoperative day. The variables studied were the operative indication, the operative risk, the anesthesia’s technique, the operative complications, the mortality and risk factors for mortality. Early postoperative complications occurred within 6 hours of the operation. Late postoperative complications occurred beyond the first six hours. The data collected was entered, coded and analyzed using Epi info 3.5.4 version 2012. The continuous variables were expressed as mean with the standard deviation. Categorical variables were expressed by frequencies and proportions. The search for associated factors was performed by multivariate logistic regression analysis using Statistical Package for Social Sciences version 20.0 software (IBM Corp. Released 2013. IBM SPSS Statistics for Windows, Version 23.0 Armonk, NY: IBM Corp). This logistic regression model was able to determine factors associated with death and a p value <0.05 was considered statistically significant. The study was conducted in accordance with the basic principles of the Helsinki Declaration on research involving individuals.
Results
The sample size was 283 patients. The median age was 30.6 years with extremes of 18 and 83 years. The most represented age group was 18 to 29 (n = 160, 56.5%). The sex-ratio was 0.2. ASA 1 and 2 classes represented 90.5% of the workforce (n = 256). The average time to take charge was 265.5 minutes, or approximately 4h 43 minutes, with extremes of 8 minutes to 5 days. General anesthesia was the predominant technique (n = 144, 50.9%). Intraoperative complications were found in 61 patients (21.6%). Intraoperative complications mainly occurred during the maintenance period (n=141, 77.9%). They were cardiovascular (n= 144, 79.6%). Postoperative complications were predominantly infectious (n=27, 33.8%). The mortality rate was 4.9% (n = 14). Infection was the most common cause (n = 6, 42.9%). The factors associated with these deaths were age > 65 years (42.9%), ASA class > 2 and occurrence of complications (Table 1-5).

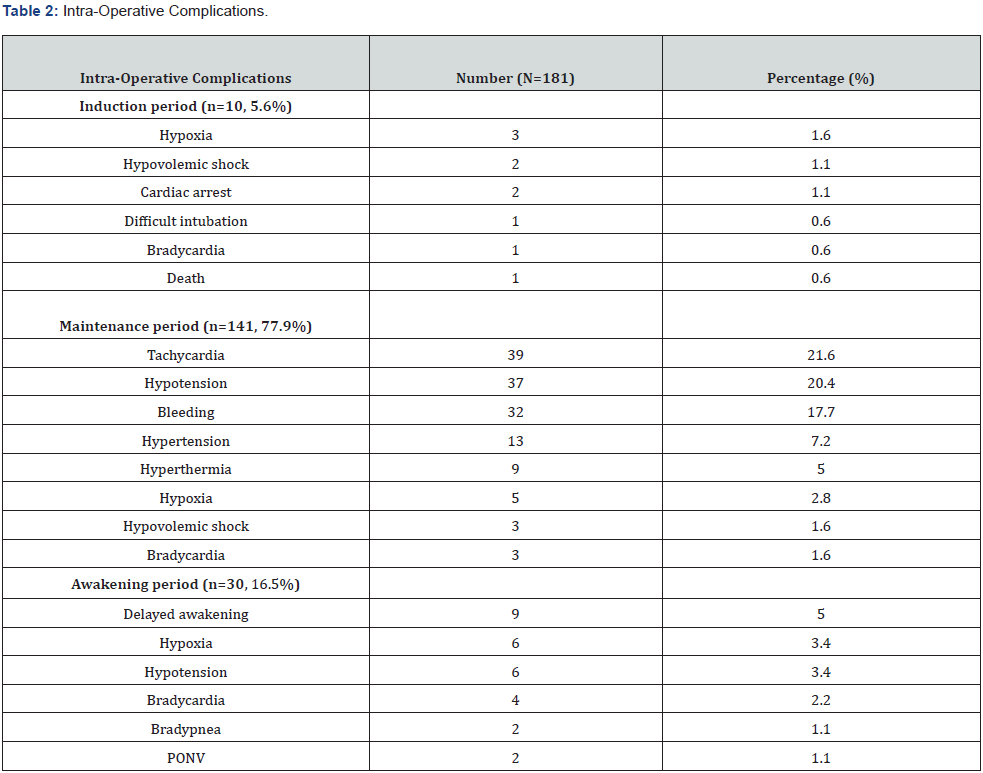
Note: PONV: Postoperative Nausea and Vomiting.
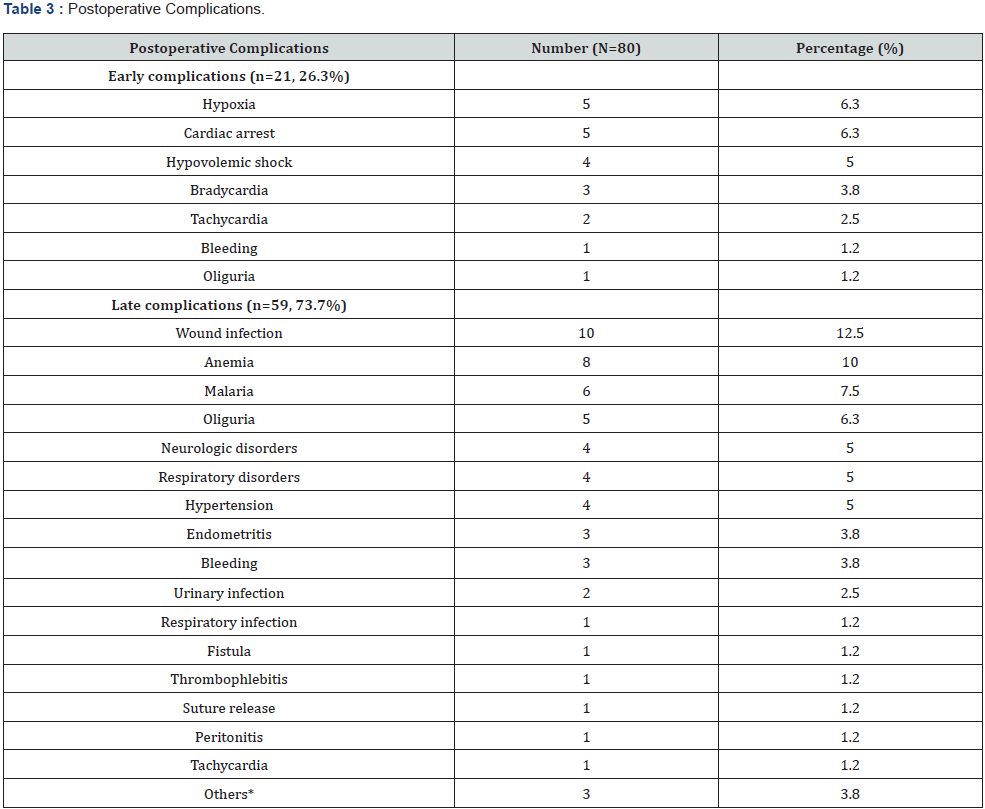
Others*: Enteritis, Chorioamniotitis, Phlebitis.
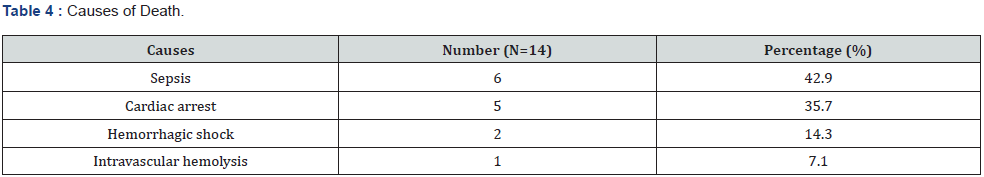
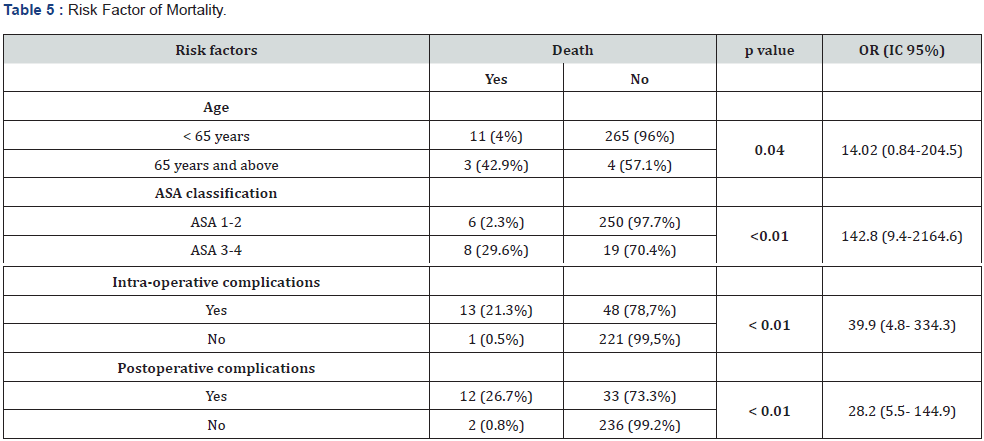
Discussion
The study involved 283 patients predominantly female. The median age was 30.6 years. ASA classes 1 and 2 accounted for 90.5% of the cases. The surgical risk was minor (78.8%). Intraoperative complications occurred during the maintenance period (77.9%). They were mainly cardiovascular (79.6%). Postoperative complications were predominantly infectious (33.8%). The death rate was 4.9%, or 14 deaths. Factors associated with mortality were age>65 years, ASA class >2 and occurrence of complications. The preoperative data revealed a young population, the majority ASA 1 and 2 classes and a minor surgical risk. This was linked to the mapping of the Cameroonian population. This was a young population with few comorbidities. This was confirmed by others Cameroonian series. Ngowé et al found a mean age of 32.5 years [4]. Owono et al. found a minor (46.6%) and intermediate (53.4%) surgical risk in his sample [10]. General anesthesia was the predominant technique (50.9%). This is the technique most practiced in our context, specifically during emergency surgery. General anesthesia remains the safest emergency anesthetic technique even though it is responsible for many respiratory disorders [11]. Emergency general surgery is characterized by a comorbid, physiologically acute patient population with disparately high rates of perioperative morbidity and mortality [12]. The average time to take charge was 4 hours with extremes of 8 minutes to 5 days. It depended on the surgical indication and the socio-economic conditions of the patient. Ngowé et al. in Cameroon, found similar results [4]. The rate of occurrence of perioperative complications was high. The intraoperative complications were mainly cardiovascular. Late postoperative complications were infectious. This was linked to the socio-economic conditions and the non-optimal conditions of care. The surgical management of emergencies in emerging countries is very often confronted with socio-economic problems, the clinical condition of the patient, the remoteness of care structures, self-medication, lack of education. health, late arrival in hospital structures, lack of medical transport, insufficient technical platform and insufficient medical and paramedical staff [1]. The death rate was 4.9%. The main causes were infectious. This mortality depended on the operative indications, the preoperative preparation and the delay in treatment. These results were similar to those of several African series. The mortality rate after emergency surgery in adults remains high. A study carried out in Madagascar in 2016 revealed a mortality rate of 4.4% [3]. In Senegal in 2006, Gaye et al found a mortality of 4.3% [2]. Scott John et al reported that a patient who received emergency surgery was eight times more likely to die postoperatively than a patient who received elective surgery [9]. The main causes of death are linked to multiple traumas, time to treatment and the presence of septic shock [5,13,14]. Over 3 million postoperative deaths occur worldwide per year. Some of these may be avoidable through risk-assessment–based modification of treatment pathways, such as postoperative critical care admission [4]. Mortality rate for patients undergoing non cardiac surgery in Europe-based on the European Surgical Outcomes Study-is 4% with crude mortality rates varying widely between countries (ranging from 1.2% to 21.5%). By comparison, emergency surgery has poorer outcomes and a higher mortality rate with recent studies reporting the 30- day mortality to be between 14 and 15% [15]. Factors associated with mortality were age>65 years, ASA class>2 and occurrence of complications.
These results were linked to the anesthetic risk (ASA classification), the support delay and the low socio-economic status. These results are similar to those obtained in several studies [1,5,16]. Perioperative mortality depends on the emergency of the surgery, the type of surgery, the patient’s preoperative condition, the time to treatment and the occurrence of intra and postoperative complications [6-8]. Analysis of the patients who died within three days of surgery showed an older age, a higher P-POSSUM, lactate, and ASA grade, and they were more physiologically compromised, with a lower systolic blood pressure, raised creatinine, and raised heart rate [17]. Increasing evidence suggests that postoperative mortality in both high and low/middle-income settings is due less to what happens in the operating theatre and more to our ‘failure to rescue’ patients who develop postoperative complications [18]. Preoperative risk prediction is important for guiding clinical decision-making and resource allocation. Clinicians frequently rely solely on their own clinical judgement for risk prediction rather than objective measures. The combination of subjective assessment with a parsimonious risk model improved perioperative risk estimation [4]. Emergency surgery outcomes in the UK were worse than those seen in the USA, suggesting an 8-fold increase in mortality in patients who had a predicted mortality rate of 0-5%. The report suggested that the differences could be overcome by better identification of high-risk patients; improved triage and preassessment; better intraoperative care; and improved postoperative care, including increased use of critical care [4]. Risk stratification tools facilitate a meaningful comparison of surgical outcomes between surgeons, hospitals and healthcare systems. In the perioperative setting, risk stratification tool can help to objectify the clinical triage process and to quantify probability of serious morbidity and mortality. Such tools can thus support surgical decision making and can aid in the informed consent process.
The provision of safe surgery is an international healthcare priority. Guidelines recommend that preoperative risk estimation should guide treatment decisions and facilitate shared decisionmaking [4]. The study presented certain limits, like the short duration of the data collection period. It had as a corollary a small sample size. This was different from the characteristics of the other studies. It was also a monocentric study. All this did not allow us to generalize our results at the national level.
Conclusion
One in 20 patients died during the perioperative period. The risk factors were related to the operative risk and the anesthesia’s technique. An optimization of the care would improve the management of the surgical emergencies in the adult. There is a need to accurately stratify patient risk so as to make the most of limited resources and improve perioperative outcomes
Conflicts of Interest
The authors declare no conflicts of interest.
Author Contribution
All authors contributed to the development and conduction of this article. All authors have read and approved the final version of the manuscript.
Acknowledgments
To all patients who have given their consent.
References
- Sall B K, Kane O, Diouf E, Beye M D (2002) Emergencies in a tropical University Teaching Hospital. PAnesthesiologist point of view. Med trop 62: 247–250.
- Gaye I, Leye P A, Traoré M M, Ndiaye P I, Boubacar Ba E H, et al. (2016) Perioperative management of emergency abdominal surgery in adult patients at the Aristide Le Dantec University Hospital. Pan Afr Med J 24: 190.
- Velomora A, Rabenjarison F, Razafindraibe FAP, Rabemazava AZL, Rakotoarison CN, et al. (2016) Mortality in the emergency departement of the Tanambao I d'Antsiranana University Teaching Hospital Madagascar. Revue Tropical Journal of surgery AMC 10: 16-17.
- Danny J N W, Harris S, Sahni A, Bedford J R, Cortes L, et al. (2020) Developing and validating subjective and objective riskassessment measures for predicting mortality after major surgery: An international prospective cohort study. PLoS Med 17(10).
- Ngowe MN, Mboudou E, Nonga B, Mouafo TF, Ze MJ, et al. (2009) Hospital mortality of surgical emergencies in adult at Yaoundé. RACS 3(5): 5-8.
- Narayan M, Tesoriero R, Brandon R B, Klyushnenkova E N, Chen H, et al. (2015) Acute care surgery: defining mortality in emergency general surgery in the state of Maryland. J Am Coll Surg 220(4): 762–770.
- Rupert M P, Moreno R P, Peter Bauer, Pelosi P, Metnitz P, et al. (2012) Mortality after surgery in Europe: a 7-day cohort study. Lancet 380(9847): 1059–1065.
- Symons NRA, Moorthy K, Almoudaris AM, Bottle A, Aylin P, et al. (2013) Mortality in high-risk emergency general surgical admissions. Br J Surg 100(10): 1318–1325.
- Scott JW, Olufajo OA, Gabriel AB, Rose JA, Zogg CK, et al. (2016) Use of National Burden to Define Operative Emergency General Surgery. JAMA Surg 151(6): 1–7.
- Etoundi PO, Bengono RB, A E, JA M Mbengono, ML N Mengo, et al. (2017) Anesthesia consultation for elective surgery: epidemiology and evaluation of the operative risk at the Yaoundé Central Hospital. Health Sci Dis 18 (1): 51-55.
- B Riou, O Langeron (2016) Anesthetic risk. Encycl Méd Chir Sci Médicales Elsevier SAS Paris (edn) Anesthésie-Réanimation 2: 1-4.
- Havens JM, Columbus AB, Seshadri AJ, Brown CVR, Tominaga GT, et al. (2018) Risk stratification tools in emergency general surgery. Trauma Surg Acute Care Open 3(1).
- Mensah E, Tchaou B, Hodonou MA, Fatigba H, Tamou BE KR, et al. (2015) Issue of the management of surgical emergencies. RAMUR 20(1): 46.
- Binam F, Malongte P, Beyiha G, Minkande ZE J, Takongmo S, et al. (2002) Emergency Medicine Capacity: Emergencies future in Africa. Med Trop 62: 275–277.
- Tribuddharat S, Sathitkarnmanee T, Sappayanon P (2019) Emergency Surgery Mortality (ESM) Score to Predict Mortality and Improve Patient Care in Emergency Surgery. Anesthesiology Research and Practice p7.
- Harissou A, Ibrahim AMM, Oumarou H, Mansour A, Amadou M, et al. (2015) Diagnostic delay and involvement prognostic in African environment. Case of surgical digestive emergencies in Zinder National Hospital, Niger. Eur. Sci. Journal, ESJ 11.
- Aggarwal G, Broughton KJ, Williams LJ, Peden CJ, Quiney N. (2020) Early Postoperative Death in Patients Undergoing Emergency High-Risk Surgery: Towards a Better Understanding of Patients for Whom Surgery May Not Be Beneficial. J Clin Med 9(5): 1288.
- Biccard BM, Madiba TE, Kluyts HL, Munlemvo DM, Madzimbamuto FD, et al. (2018) Perioperative patient outcomes in the African Surgical Outcomes Study: a 7-day prospective observational cohort study. Lancet 391(10130): 1589–1598.






























