Dual Pectoral Nerve and Serratus Anterior Blocks for Postoperative Analgesia After Breast Surgery: Placebo-Controlled Comparative Study Versus Paravertebral Block
Amir Abouzkry Elsayed MD* and Sherif Kamal Arafa MD
Department of anesthesia and Surgical Intensive Care, Faculty of Medicine, Kafrelsheikh University, Egypt
Submission: September 11, 2020 Published: January 11, 2021
*Corresponding author: Amir Abouzkry Elsayed; Department of anesthesia and Surgical Intensive Care, Faculty of Medicine, Kafrelsheikh University, Egypt, Tel: 00201016326544
How to cite this article: Amir Abouzkry Elsayed M, Sherif Kamal Arafa M. Dual Pectoral Nerve and Serratus Anterior Blocks for Postoperative Analgesia After Breast Surgery: Placebo-Controlled Comparative Study Versus Paravertebral Block. J Anest & Inten care med. 2021; 11(1): 555805 10.19080/JAICM.2021.11.555805
Abstart
Background and Objectives: To evaluate outcome of pain management after modified radical mastectomy (MRM) using US-guided combined pectoral and serratus anterior (PEC1/SAB) block versus thoracic paravertebral block (PVB).
Methodology: Ninety women were categorized into control group received no block, PVB group received PVB and PEC1/SAB group received PEC1 and SAB immediately after surgical wound closure using levobupivacaine. Postoperative (PO) pain was monitored for 24-hr PO; using 11-points numeric rating scale (NRS) and at NRS score ≥4, IV morphine (0.05 mg/kg) was given. Primary outcome was reduction of 24-hr amount of morphine consumption by 20% with regional block in relation to no block. Results were analyzed using paired t-test, One-way ANOVA Test and Chi square test.
Results: PVB and PEC1/SAB blocks significantly reduced PO morphine consumption by 40.4% and 49.2%, respectively and PEC1/SAB block significantly reduced the amount used by 14.8% of the dose received with PVB block. Duration of PO analgesia was significantly longer, and number of morphine requests and collective 24-hr NRS scores were significantly lower in with blocks than no block with non-significant differences between both types of block. Morphine-induced side effects were more manifest in control patients.
Conclusion: PVB or PEC1/SAB blocks allowed reduction of PO morphine consumption by >40% than no block with significantly longer duration of PO analgesia and lower number of requests of additional analgesia in comparison to no block. PEC1/SAB block significantly reduced amount of morphine consumption than PVB.
Keywords:Modified radical mastectomy, thoracic paravertebral block, combined pectoral, and serratus anterior (PEC1/SAB) block, morphine consumption
Abbreviations:MRM: modified radical mastectomy, US-guided: Ultrasound-guided, PEC1/SAB: combined pectoral and serratus anterior block, PVB: paravertebral block, PO: Postoperative, NRS: numeric rating scale, IV: intravenous
Introduction
Breast cancer is the most common malignancy of women and is the chief cause of cancer-related death with an exponentially increasing incidence secondary to increases in life expectancy and cancer-inducing risk factors especially changes in reproductive activity [1]. Breast cancer surgery is the primary therapeutic intervention, but it is frequently associated with postoperative (PO) pain that causes prolonged hospital stay, increased expenses and consumption of health services resources and long-term affection of patients’ quality of life [2].
Persistent pain after breast surgeries is mostly secondary to poorly treated acute pain [3]. There is emerging evidence suggesting the adjuvant use of regional analgesia for perioperative pain management [4] for its better analgesic results [5], very few cardiovascular or pulmonary side-effects [6] and avoidance of systemic opioid analgesia which may have effects on oncological outcomes [4].
Thoracic paravertebral block (PVB) provided ipsilateral somatic and sympathetic nerves blockade through injection of local anesthetic (LA) adjacent to thoracic vertebra close to points of emergence of spinal nerves from the inter-vertebral foramina [7]. PVB was successfully employed in analgesic protocols for breast surgery [3] for its high analgesic potency and low sideeffects profile [8].
Pectoral nerve (PEC) blocks can provide analgesia for surgical procedures involving the breast and anterior chest wall [9]. The PEC1 block involves LA injection between pectoralis major and minor muscles at level of the 3rd rib to anaesthetize pectoral nerves and PEC2 block involves one injection of LA between pectoral muscles and another between pectoralis minor and serratus anterior (SA) muscles to anaesthetize the anterior cutaneous branches of the intercostal nerves and the intercostobrachial and long thoracic nerves [10].
Chest ultrasound (US) imaging at the 5th rib in mid-axillary line identified two potential spaces in relation to SA muscle and LA injection in superficial plane provides wider (T2-9) dermatome spread with blockade of long thoracic and thoracodorsal nerves [11] while deep plane injection allows intercostal branches block and provides adequate analgesia [12]. The SA block (SAB) provides complete hemithorcic paraesthesia and can be an alternative to PVB and central neuraxial blockade, which may be technically more challenging and have a higher potential adverseeffect profile [13]. This study targets to evaluate the outcome of pain management after modified radical mastectomy (MRM) using combined PEC1/SAB block versus thoracic PVB.
Methodology
This prospective comparative single center clinical trial was conducted at department of Anesthesia, ICU and pain management, Aswan University hospital since January 2017 till May 2019. The protocol of the study was approved by the Local Ethical Committee (EC Ref No.: aswu/109/6/16) and enrolled patients signed written fully informed consent concerning the study target and methodology. All women aged 20-70 years and assigned for MRM were eligible for evaluation. Collected baseline data included age, body weight and height for calculation of body mass index (BMI), clinical examination to determine ASA grade, baseline heart rate (HR) and arterial blood pressure. Patients with co-morbidities were adjusted and maintained on their preoperative therapies till day of surgery and postoperatively to maintain the control state. Exclusion criteria included ASA grades III and IV, BMI ≥35 kg/m2, chest or spine abnormalities, previous chest surgery, history of previous fracture rib, neurological diseases, peripheral neuropathy, coagulopathies, allergy to local anesthetics (LA), inability to interpret the used pain score and refusal to sign the written consent.
Groups
Patients free of exclusion criteria were included in the study and were randomly allocated into three equal groups using sealed envelopes containing cards carrying the label for each group that were prepared by an assistant not included in the study and envelopes were chosen by patient herself.
1. Control group (Group C) included patients received no LA block.
2. PVB group included patients received ultrasound guided PVB
3. PEC1/SAB group included patients received US-guided PEC1 and SAB
Levobupivacaine was used for the studied blocks depending on its high cardiovascular collapse/CNS ratio that indicates its greater safety margin than racemic bupivacaine [14]. Also, Levobupivacaine has dose-dependent vasoactive properties that may potentially prolong duration and slow systemic absorption, as opposed to bupivacaine which has vasodilatory properties and may lead to more rapid systemic absorption [15].
Dose of levobupivacaine was calculated according to Berde & Strichartz [16] as weight-based dose, not to exceed 2 mg/ kg to avoid local anesthetic toxicity. The preparation used was levobupivacaine 0.25% that provided 2.5mg/ml. The volume to be injected was 40 ml for patients in both PEC1/SAB and PVB groups. For patients of PEC1/SAB group the calculated dose was given as 10 ml for PEC1 block and the remaining part was used for SAB. For patients of PVB, multilevel PVB injections from T2 to T6 were used and the calculated dose (40ml) was divided equally between these levels.
LA blocks procedure
Nerve block was performed after skin closure and covering of wound area under US guidance using 6-13 MHz linear transducer (Sonosite, MicroMaxx machine, USA) as follows:
1. US-guided PVB: patient was placed in lateral position to expose the wound ipsilateral side, then the transducer was placed parallel to vertebral column to identify the spinous process of T4 and then moved laterally to identify its transverse process searching for the costotransverse ligament (CTL) to identify the PV space which site was confirmed by viewing the echogenic line of the pleura underneath of CTL. Then, a 22-gauge Quincke’s spinal needle was advanced in the plane and the calculated volume of 0.25% levobupivacaine was injected in the PV space equally at multiple levels from T2 to T6.
4. US-guided PEC1 and SAB: patient was in supine position with ipsilateral arm was abducted above the head, skin at the infra-clavicular region was sterilized, the transducer was placed infra-clavicular, moved laterally to locate the axillary artery and vein directly above the 1st rib so as to identify the pectoral muscles, a 22-gauge Quincke’s spinal needle was inserted at the 3rd rib level between pectoralis major and minor muscles to inject 10 ml 0.25% levobupivacaine in the fascial plane between the two muscles. Thereafter, the US probe was placed over the 5th rib in the mid axillary line and under US-guidance a 22-gauge Quincke’s spinal needle was directed towards the inter-fascial plane between the serratus anterior muscle and external intercostal muscle, needle site was assured by injection of 3-ml of normal saline to create of hydro dissection, and then the created fascial plane was perfused by the remaining part of the calculated volume of levobupivacaine 0.25%.
Anesthetic procedure
Patients attended the pre-anesthetic room fasting for a minimum of 6-hr and were premedicated by midazolam (2 mg IV), ondansetron (4 mg IV), and paracetamol (1gm IVI). Anesthesia was induced, in all groups, using fentanyl 2 ug/kg, propofol 1-2 mg/kg and rocuronium 0.6 mg/kg, and was maintained with sevoflurane 2%, fentanyl 1 ug/kg and rocuronium 0.1mg/kg as required. After endotracheal intubation, the lungs were ventilated with 50% O2 in air for a tidal volume of 6-8 ml/kg, end-tidal carbon dioxide (ETCO2) of 35-40 mmHg and inspiration: expiration (I:E) ratio of 1:2. Patients were continuously non-invasively monitored for mean arterial pressure (MAP), heart rate (HR), ECG, SpO2 and ETCO2. At the end of surgery and prior to extubation, patients received their assigned block for management of postoperative (PO) pain according to the label of the card. Thereafter, intravenous injection of neostigmine 0.05 mg/kg with atropine 0.02 mg/kg IV was done to reverse the residual neuromuscular blockade, patients were extubated and shifted to the post-anesthesia care unit (PACU).
Patients were monitored for pain sensation, for 24-hr PO; using 11-points numeric rating scale (NRS) from 0 to 10 where 0 indicates no pain and 10 indicates worst pain imaginable. NRS was used for being more practical than the graphic visual analogue scale, easier to perceive for most people, and does not need clear vision, pen, and paper [17]. All patients received ketorolac tromethamine (Ketolac; amp 30mg/ml; Amryia Pharmaceuticals, Alex, Egypt) as 1-ml diluted to 10-ml with normal saline (0.9%) and given slowly intravenous postoperatively every 8-hrs for a maximum of 3-doses/day. Additional analgesia was provided for patients who had NRS score ≥4; as morphine in a dose of 0.05 mg/ kg diluted in 10-ml of normal saline (0.9%) and was given slowly IV with monitoring of respiratory rate (RR) for a rate not less than 8/min and SpO2 not less than 94% on room air. Patients were also monitored for hemodynamics, conscious level and central nervous and cardiovascular signs of systemic local anesthetic toxicity in PACU and in the ward.
Study outcomes
1. Primary outcome was the reduction of 24-hr PO mean amount of morphine consumption by 20% difference between studied groups.
2. Secondary outcome
- PO pain severity as judged after extubation; at 30-min, 2, 4, 8, 12, 18 and 24-hr PO using NRS score
- Duration of PO analgesia, defined as duration of analgesia till having NRS score ≥4 and receiving morphine as additional analgesia.
- Development of block injection-related complication, LA side effects or additional analgesia induced side effects.
Sample size calculation
Previously, Sidiropoulou et al. [18]18 reported non-significant lower morphine consumption with continuous ropivacaine 0.5% infusion in comparison to ropivacaine 0.5% PVB in a study included 24 patients/group. Combined PEC1/SAB block with US guided infiltration was supposed to do preferably than continuous infusion and decrease the amount of morphine consumed during 24-hr PO down to a level to get a significant difference in comparison to PVB. A sample size of 29 patients per group would achieve a power of 83.4% with α value of 0.05 and β value of 0.2 and fulfill the study target to get significant difference in the mean morphine consumption between both study groups in comparison to control group and in between both of the study groups. To protect against drop out cases we added 3 cases, so the total number was 90 cases for 30 patients per group.
Statistical Analysis
Obtained data were presented as mean±SD, median, numbers and percentages. Results were analyzed using paired t-test, Oneway ANOVA Test and Chi square test. Statistical analysis was conducted using the IBM SPSS (Version 23, 2015) for Windows statistical package. P value <0.05 was considered statistically significant.
Results
During the study duration, 102 women were eligible for evaluation and 90 of women who had fulfilled the inclusion criteria were categorized into the three study groups (Figure 1).
Evaluation of demographic and clinical data showed nonsignificant differences between women of studied groups (Table 1).
Regarding primary outcome, patients who received PVB or PEC1/SAB blocks consumed significantly lower doses of PO morphine than control patients. Moreover, the extent of reduction of PO morphine consumption was 40.4% and 49.2% by PVB and PEC1/SAB, respectively, in relation to that consumed by control patients. Furthermore, the use of PEC1/SAB block significantly reduced morphine consumption than PVB by about 14.8% of the dose received by patients who received PVB block. Consequently, the duration of PO analgesia was significantly longer, and number of requests of additional analgesia and the collective 24-hr scores were significantly lower in patients received PVB and PEC1/SAB blocks in comparison to that recorded for control patients with non-significant differences between PVB and PEC1/SAB groups (Table 2).

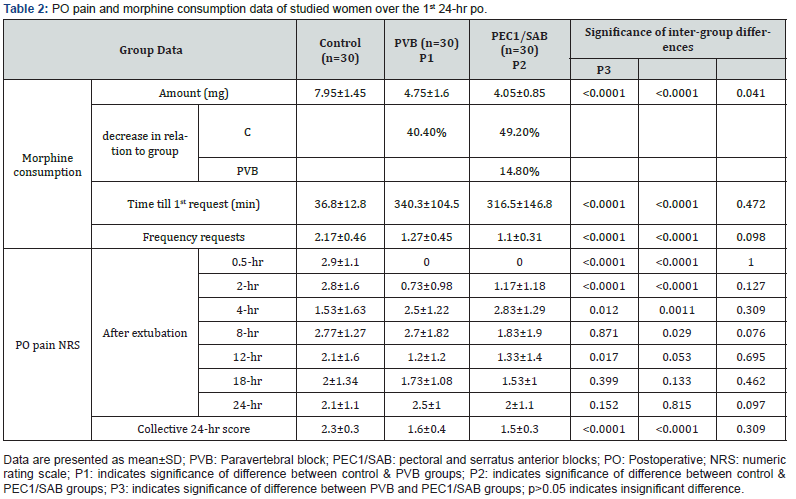

All surgeries were conducted uneventfully with a mean duration till completion of mastectomy of 75.5±9.9 min. The wound was closed, with drainage for 24-hrs to guard against seroma formation. Mean duration for mastectomy and amount of operative blood loss showed non-significant differences between the three groups. Mean duration till completion of block was nonsignificantly shorter with PVB, so total theater time for patients received nerve block was non-significantly shorter with PVB (Table 3). Mean HR and MAP measures recorded during surgery showed non-significant variance between patients of all studied groups.
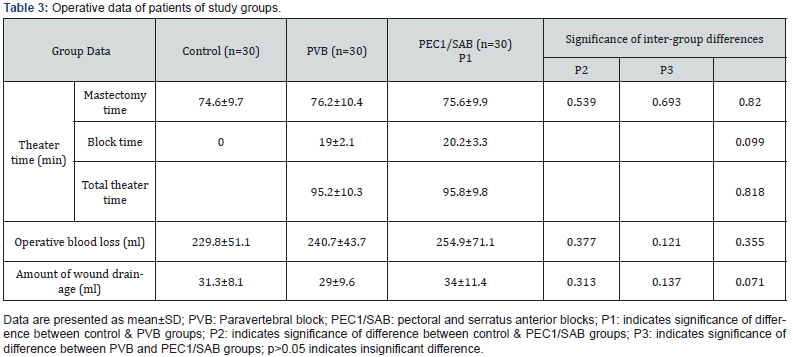
All patients had drain removal after 24-hrs PO to guard against development of ascending wound infection. There was non-significant difference between patients of studied groups regarding the amount of wound drainage. No patient developed surgical or block-related complications, such as limb edema, pneumothorax, vascular puncture, or local anesthetic toxicity. Morphine-induced side effects were more manifest in patients of group C, but fortunately no patient developed respiratory depression (Table 4).
Patients who had PONV required ondansetron injection, while other manifestations were mild and required no treatment.
Discussion
The use of either PVB or PEC1/SAB blocks for women underwent MRM allowed PO morphine consumption reduction by about 40-50% with significantly longer duration of PO analgesia and lower number of requests of additional analgesia in comparison to control patients received no block. However, PEC1/SAB block did more favorably than PVB as manifested by reduction of morphine consumption by 15% with significantly lower amount of morphine consumed during 24-hr PO. Unfortunately, no previous study was found to compare the three types of regional blocks; however, multiple studies compared outcomes of using either PECS or SAB versus controls receiving opioid-based analgesia during breast surgeries under general anesthesia (GA), where PEC block whether administered to provide perioperative [19-21], intraoperative [22] or PO analgesia [23,24] for women undergoing MRM, significantly reduced pain scores, intraoperative (IO) and PO opioid use and provided significantly longer duration of analgesia with associated reduction of the incidence of PONV in comparison to GA alone. Moreover, Fancellu et al. [22] documented that PECS plus sedation can allow perfect anesthesia for breast-conserving surgery, thus avoiding general anesthesia.

Regarding SAB, Rahimzadeh et al. [25], Yoon et al. [26] and Ahiskalioglu et al. [27] using US-guided SAB reported statistically lower pain scores, 24-h opioid consumption, and incidence of PONV in comparison to control women received GA without blocks. Moreover, Abdallah et al. [28] compared PEC or SAB blocks versus control group received opioid-based analgesia and found either type of block was associated with reduced IO and PO opioid consumption and PONV compared with control and reported non-significant difference between both types of block for these 2 outcomes.
Furthermore, Versyck et al. [29] reported that PEC block showed better analgesic efficacy than systemic analgesia alone and comparable analgesic efficacy to a thoracic PVB for breast cancer surgery, while Singh et al. [30] reported that use of PECS block with GA for breast surgery has significant IO opioid-sparing effect than PVB and Grape et al. [31] after searching the electronic databases for trials comparing PECS block with PVB as analgesic treatment after radical mastectomy had documented that PECS block provides marginal PO analgesic benefit than PVB till 2-hr PO and then the difference became non-significant. Also, Gupta et al. [32] documented that SAB is an alternative analgesic technique to thoracic PVB for MRM although PVB provides a longer duration of analgesia.
In a comparative study of combined SAB/PECS blocks for women undertaken mastectomy under GA versus GA alone, Matsumoto et al. [33] found combined blocks significantly reduced IO opioid consumption, morphine use and pain scores in PACU and till 24 h after surgery. In addition to these advantages, Wang et al. [34] found such combination contributed to better sleep quality and higher patient satisfaction of pain relief and Grasso et al. [35] found the combined blocks significantly reduced PONV and hospital stay. In an interesting comparative study, Song et al. [36] found the combination of PECS, SAB and parasternal intercostal blocks showed no differences in pain scores in comparison to PECS/SAB alone during rest but significantly reduced pain scores during activity.
The reported superior pain relief and reduction of morphine consumption with the use of combined PECS/SAB block in comparison to PVB during MRM, could be attributed to the complementary effect of both types of block to magnify the advantages and cover weak points of each if used separately. In support of this assumption, Kubodera et al. [37] compared PECS and SAB for analgesia after mastectomy and found the 24-h PO pain scores and morphine consumption within 24 hours was nonsignificantly lower in PECS than SAB block, while the proportion of patients without pain till 2-months PO was significantly less with SAB, but pain scores were significantly lower with PECS.
One of the strong points of our trial is the use of a consistent concentration and volume of local anaesthetic drug in PVB and PEC1/SAB groups (40 ml of 0.25% levobupivacaine). Our methodology therefore presented a reasonable comparative evaluation of both groups comparing to other researchers used different concentrations and volumes between groups in the same study. We performed multilevel PVB injection to provide more effective analgesia in PVB group. The reported superior pain relief and reduction of morphine consumption with the use of combined PECS/SAB block in comparison to PVB during MRM, could be attributed to the complementary effect of both types of block to magnify the advantages and cover weak points of each if used separately. Unfortunately, no previous study was found to compare the three types of regional blocks. Our analysis, however, had some limitations. We could not determine the onset time of block or the sensory block level as blocks were done under general anesthesia, at the end of surgical procedure. We did not put a catheter to facilitate prolonged postoperative pain relief in our small study. Wide scale studies are mandatory to establish the ideal injection modalities for SAB (superficial or deep to serratus anterior muscle) and the analgesic duration with and without adjuvants to improve the post-operative analgesic mechanisms for MRM.
Conclusion
Regional blocks for PO analgesia improved quality of pain control after MRM with reduced opioid consumption and sparing of opioid-related side effects. Multimodal nerve block using combined PEC1/SAB block provided superior analgesia with significant reduction of morphine consumption than PVB and is recommended for MRM as adjuvant to GA. However, wide scale studies are mandatory to establish these results and to define the impact of combined block on patients’ quality of life.
References
- Tabrizi F, Rajabzadeh H, Eghtedar S (2020) Effects of the Continuous Care Model on the Health-Promoting Lifestyle in Breast Cancer Survivors: A Randomized Clinical Trial. Holist NursPract34(4):221-233.
- Kouwenberg C, de Ligt K, Kranenburg L, Rakhorst H, de Leeuw D, et al.(2020) Long-Term Health-Related Quality of Life After Four Common Surgical Treatment Options for Breast Cancer and the Effect of Complications: A Retrospective Patient-Reported Survey Among 1871 Patients. Plast Reconstr Surg146(1):1-13.
- Saporito A, Aguirre J, Borgeat A, Perren A, Anselmi L, et al.(2019) Persistent postdischarge pain and chronic postoperative pain after breast cancer surgery under general anesthesia and single-shot paravertebral block: incidence, characteristics and impact on quality of life and healthcare costs. J Pain Res12: 1193-1199.
- Pawa A, Wight J, Onwochei DN, Vargulescu R, Reed I, et al. (2018) Combined thoracic paravertebral and pectoral nerve blocks for breast surgery under sedation: a prospective observational case series. Anaesthesia73(4): 438-443.
- Schuitemaker RJB, Sala-Blanch X, Rodriguez-Pérez CL, Mayoral R JT, López-Pantaleon LA, et al. (2018) The PECS II block as a major analgesic component for clavicle operations: A description of 7 case reports. Rev EspAnestesiolReanim65(1): 53-58.
- Moon EJ, Kim SB, Chung JY, Song JY, Yi JW(2017) Pectoral nerve block (Pecs block) with sedation for breast conserving surgery without general anesthesia. Ann Surg Treat Res93(3): 166-169.
- Karmakar MK, Samy W, Li JW, Lee A, Chan WC, et al. (2014) Thoracic paravertebral block and its effects on chronic pain and health-related quality of life after modified radical mastectomy. Reg Anesth Pain Med39(4): 289-298.
- Fang B, Wang Z, Huang X(2019) Ultrasound-guided preoperative single-dose erector spinae plane block provides comparable analgesia to thoracic paravertebral block following thoracotomy: a single center randomized controlled double-blind study. Ann Transl Med7(8): 174.
- Calì Cassi L, Biffoli F, Francesconi D, Petrella G, Buonomo O(2017) Anesthesia and analgesia in breast surgery: the benefits of peripheral nerve block. Eur Rev Med Pharmacol Sci21(6): 1341-1345.
- Campos M, Azevedo J, Mendes L, Rebelo H (2018) Pectoral nerve block as a single anesthetic technique for breast surgery and sentinel lymph node investigation. Rev EspAnestesiolReanim65(9): 534-536.
- Blanco R, Parras T, McDonnell JG, Prats-Galino A(2013) Serratus plane block: A novel ultrasound-guided thoracic wall nerve block. Anaesthesia68: 1107-1113.
- Diéguez García P, Fajardo Pérez M, López Álvarez S, Alfaro de la Torre P, PensadoCastiñeiras AP(2013)Ultrasound-assisted approach to blocking the intercostal nerves in the mid-axillary line for non-reconstructive breast and axilla surgery. Rev EspAnestesiolReanim60(7): 365-370.
- Broseta AM, Errando C, De Andrés J, Díaz-Cambronero O, Ortega-Monzó J(2015) Serratus plane block: the regional analgesia technique for thoracoscopy? Anaesthesia70(11): 1329-1330.
- di Gregorio G, Neal JM, Rosenquist RW, Weinberg GL(2010)Clinical presentation of local anesthetic systemic toxicity: a review of published cases, 1979 to 2009. Reg Anesth Pain Med35(2): 181-187.
- El-Boghdadly K, Pawa A, Chin KJ(2018)Local anesthetic systemic toxicity: current perspectives. Local Reg Anesth11: 35-44.
- Berde CB, Strichartz GR(2015)Local anesthetics. In: Miller RD (Ed.). Miller’s Anesthesia, eighth ed. Elsevier, Philadelphia, USA p. 1043.
- Williamson A, Hoggart B(2005)Pain: a review of three commonly used pain rating scales. J Clin Nurs14(7): 798-804.
- Sidiropoulou T, Buonomo O, Fabbi E, Silvi MB, Kostopanagiotou G, et al. (2008)A prospective comparison of continuous wound infiltration with ropivacaine versus single-injection paravertebral block after modified radical mastectomy. AnesthAnalg106(3): 997-1001.
- Wang K, Zhang X, Zhang T, Yue H, Sun S, et al.(2018)The Efficacy of Ultrasound-guided Type II Pectoral Nerve Blocks in Perioperative Pain Management for Immediate Reconstruction After Modified Radical Mastectomy: A Prospective, Randomized Study. Clin J Pain34(3): 231-236.
- Zhao J, Han F, Yang Y, Li H, Li Z(2019) Pectoral nerve block in anesthesia for modified radical mastectomy: A meta-analysis based on randomized controlled trials. Medicine (Baltimore) 98(18):
- Kim S, Avila J, Lee J, Lee T, Macres S, et al.(2020)Impact of Preoperative Pectoralis Plane Nerve Blocks for Mastectomy on Perioperative Opioid Consumption: A Retrospective Study. Pain Manag10(3): 159-165.
- Fancellu A, Perra T, Ninniri C, Cottu P, Deiana G, et al. (2020)The Emerging Role of Pectoral Nerve Block (PECS Block) in Breast Surgery: A Case-Matched Analysis Breast J26(9):1784-1787.
- Thomas M, Philip FA, Mathew AP, Jagathnath Krishna KM(2018)Intraoperative pectoral nerve block (Pec) for breast cancer surgery: A randomized controlled trial. J Anaesthesiol Clin Pharmacol34(3): 318-323.
- Sun Q, Liu S, Wu H, Kang W, Dong S, et al.(2020)Clinical Analgesic Efficacy of Pectoral Nerve Block in Patients Undergoing Breast Cancer Surgery: A Systematic Review and Meta-Analysis. Medicine (Baltimore)99(14):
- Rahimzadeh P, Imani F, Faiz SHR, Boroujeni BV(2018)Impact of the Ultrasound-Guided Serratus Anterior Plane Block on Post-Mastectomy Pain: A Randomised Clinical Study. Turk J AnaesthesiolReanim46(5): 388-392.
- Yoon H, Yu B, Kim Y, Lee J, Koh W, et al.(2019)Serratus anterior plane block combined with monitored anesthesia care for surgery of lateral side of breast -a case report. Korean J Anesthesiol72(5): 500-503.
- Ahiskalioglu A, Yayik A, Demir U, Ahiskalioglu E, Celik E, et al.(2020)Preemptive Analgesic Efficacy of the Ultrasound-Guided Bilateral Superficial Serratus Plane Block on Postoperative Pain in Breast Reduction Surgery: A Prospective Randomized Controlled Study. Aesthetic Plast Surg44(1): 37-44.
- Abdallah FW, MacLean D, Madjdpour C, Cil T, Bhatia A, et al.(2017)Pectoralis and Serratus Fascial Plane Blocks Each Provide Early Analgesic Benefits Following Ambulatory Breast Cancer Surgery: A Retrospective Propensity-Matched Cohort Study. AnesthAnalg125(1): 294-302.
- Versyck B, van Geffen GJ, Chin KJ(2019) Analgesic efficacy of the Pecs II block: a systematic review and meta-analysis. Anaesthesia74(5): 663-673.
- Singh PM, Borle A, Kaur M, Trikha A, Sinha A(2018)Opioid-sparing effects of the thoracic interfascial plane blocks: A meta-analysis of randomized controlled trials. Saudi J Anaesth12(1): 103-111.
- Grape S, El-Boghdadly K, Albrecht E(2020)Analgesic Efficacy of PECS vs Paravertebral Blocks After Radical Mastectomy: A Systematic Review, Meta-Analysis and Trial Sequential Analysis. J Clin Anesth63: 109745.
- Gupta K, Srikanth K, Girdhar KK, Chan V(2017)Analgesic efficacy of ultrasound-guided paravertebral block versus serratus plane block for modified radical mastectomy: A randomised, controlled trial. Indian J Anaesth61: 381-386.
- Matsumoto M, Flores EM, Kimachi PP, Gouveia FV, Kuroki MA, et al. (2018)Benefits in radical mastectomy protocol: a randomized trial evaluating the use of regional anesthesia. Sci Rep 8(1): 7815.
- Wang W, Song W, Yang C, Sun Q, Chen H, et al.(2019)Ultrasound-Guided Pectoral Nerve Block I and Serratus-Intercostal Plane Block Alleviate Postoperative Pain in Patients Undergoing Modified Radical Mastectomy. Pain Physician22(4): E315-E323.
- Grasso A, Orsaria P, Costa F, D'Avino V, Caredda E, et al.(2020)Ultrasound-guided Interfascial Plane Blocks for Non-anesthesiologists in Breast Cancer Surgery: Functional Outcomes and Benefits. Anticancer Res40(4): 2231-2238.
- Song W, Wang W, Yang Y, Sun Q, Chen H, et al.(2020)Parasternal Intercostal Block Complementation Contributes to Postoperative Pain Relief in Modified Radical Mastectomy Employing Pectoral Nerve Block I and Serratus-Intercostal Block: A Randomized Trial. J Pain Res13: 865-871.
- Kubodera K, Fujii T, Akane A, Aoki W, Sekiguchi A, et al.(2020)<Editors' Choice> Efficacy of Pectoral Nerve Block type-2 (Pecs II Block) Versus Serratus Plane Block for Postoperative Analgesia in Breast Cancer Surgery: A Retrospective Study. Nagoya J Med Sci82(1): 93-99.






























