Effect of Pre-emptive Pregabalin on Deliberate Hypotension, Postoperative Pain, and Analgesic requirements for Patients Undergoing Dacryocystorhinostomy Surgery under Local Anesthesia
Sherif Kamal Arafa and Amir Abouzkry Elsayed*
Department of Anesthesia and Surgical Intensive Care, Kafrelsheikh University, Egypt
Submission: July 05, 2020; Published: August 20, 2020
*Corresponding author: Amir Abouzkry Elsayed, Department of anesthesia and Surgical Intensive Care, Faculty of Medicine, Kafrelsheikh university, Egypt, Tel: 002010016326544
How to cite this article: Sherif Kamal A, Amir A E. Effect of Pre-emptive Pregabalin on Deliberate Hypotension, Postoperative Pain, and Analgesic requirements for Patients Undergoing Dacryocystorhinostomy Surgery under Local Anesthesia. J Anest & Inten care med. 2020; 11(1): 555802. DOI: 10.19080/JAICM.2020.11.555802
Abstart
Background: Preoperative use of oral pregabalin was a recommended option for managing acute postoperative pain, a promising way to induce hypotension and reduce postoperative analgesic requirements during dacryocystorhinostomy operation.
Objectives: Study was designed to estimate the effect of oral pregabalin on deliberate hypotension, postoperative pain and total postoperative analgesic requirements during dacryocystorhinostomy surgery under local anesthesia.
Methods: This double blind randomized clinical study included 80 patients, ASA I-II patients prepared for dacryocystorhinostomy under local anesthesia. The study enrolled two groups, Group I where patients received 300mg pregabalin capsule orally, one hour before surgery. Group II (control group) where patients received placebo capsule orally, one hour before surgery. Mean arterial blood pressure was maintained within no more than 20% to 30% lower than baseline with co-administration of nitroglycerin. We assessed acute postoperative pain using visual analogue scale until 24 hours after surgery. Also, intraoperative bleeding was evaluated by the visibility of the operative field during dacryocystorhinostomy operation by Fromm and Boezaart scale. Duration from the end of surgery till first requirement of analgesia of pethidine and the overall dose of pethidine used in the first 24 hours and side effects were recorded. Total requirement of nitroglycerin administration and undesirable side effects of pregabalin were also recorded. Data were analyzed using Student’s t-test and chi-square test. P<0.05 was considered significant.
Results: Decreased postoperative pain, minimal Fromm and Boezaart scale of bleeding, lower total dose of nitroglycerin required, low dose of pethidine, less side effects and less number of patients needed analgesia were observed in group I (pregabalin group) than in group II (control group).
Conclusion: Pre-emptive oral Pregabalin had the efficacy of reducing the intensity of pain during dacryocystorhinostomy, reducing consumption of opioids with its unwanted side effects after the operation, and minimizing the need for intraoperative uses of hypotensive agents with enhancement of surgical field visibility
Keywords:Pregabalin, Dacryocystorhinostomy, Local anesthesia, Postoperative pain, Deliberate hypotension
Introduction
Dacryocystorhinostomy is the most frequent lacrimal drainage procedure and it is a process that fistulizes the lacrimal sac and nasal cavity [1]. It is the method of choice designed to manage anatomical lacrimal gland obstruction. The target of surgery is to produce mucosa to mucosa anastomosis between the lateral wall of the nose and the lacrimal sac [2]. Histamine released during surgical injuries with other inflammatory mediators. Noxious stimuli are transmitted through the spinoreticular and spinothalamic tract to the dorsal horn of the spinal cord and high centers from peripheral visceral and somatic sites by A and C fibers [3]. Uncontrolled postoperative pain may produce unwanted deleterious effects as elevated blood pressure, increased heart rate, increased myocardial oxygen consumption, myocardial infarction, deep vein thrombosis, delayed discharge from hospital and insufficient depth of breathing with wide range of different pain modalities [4]. Nowadays, opioids are the mainstay for management of postoperative pain, despite of the expected side effects of the opioids; new discoveries of non-opioid drugs were established with acceptable costs, prolonged duration and less side effects [5]. Pregabalin is a potent gabapentin analogue and is considered as a ligand for α2-δ subunit. Pregabalin attenuates the excitatory neurotransmitters release and blocks central sensitization development [6]. Pregabalin is an amino acid substitution, which permits high lipid solubility and diffusion across blood brain barrier [7]. Pregabalin decreases the entry of calcium into the central nervous system nerve terminals and reduces the amounts of glutamate, noradrenalin and substance P that produce the feeling of pain [8]. Also, it reduces the tissue damage induced stimulation of posterior horn neurons [9]. Pregabalin is anticonvulsant, analgesic and anxiolytic and its role in treatment of neuropathic pain control through its action on the presynaptic voltage gated calcium channel, suppressing the production of glutamate [10]. Plasma level of pregabalin reaches its peak within 30 minutes to 2 hours after its administration [11]. Most of DCR surgeries were performed under general anesthesia. However new trend is employed to achieve these surgeries under local anesthesia due to advantages of local anesthesia in DCR operation as adequate hemostasis of surgical field, proper dissection of fibrous tissues that obstruct the pathway of lacrimal gland and good control of severe postoperative pain that may affect the outcome of patients and surgery. Also avoiding the complications of general anesthesia as nausea, vomiting, airway obstruction, delayed recovery, hemodynamic instability during and after operation, agitation of patients that may cause removal of nasal packs and straining of patients during recovery that may increase the bleeding per nose with massive pain postoperatively that require potent analgesia and opioids that may cause unwanted respiratory depression in wards [12]. Recent studies showed the usefulness of pregabalin in restraining postoperative pain intensity and minimizing opioid needs with its related side effects [13]. Our study target was deigned to assess the impact of pre-emptive pregabalin on postoperative pain, induced hypotension, analgesic requirements, and side effects (nausea, vomiting, dizziness, sedation and visual disturbance if occurred) on patients underwent dacryocystorhinostomy surgery under local anesthesia.
Methods
This randomized, double blind and placebo-controlled study was achieved after approval of local ethical committee and informed consents were taken from all patients in our research. This study was achieved in Aswan university hospital from April 2019 to February 2020. Eighty patients were enrolled in our study, aged 20-60 years old, American society of anesthesiologist (ASA) physical status I-II. All participants were planned for dacryocystorhinostomy (DCR) operation under local anesthesia. While those with hypersensitivity to pregabalin or to its analogue, ASA III or IV, hepatic, renal insufficiency, uncontrolled respiratory disorders, history of taking antihypertensive or β blockers without control or on any cardiac medication, coagulation disorders, previous seizure, history of taking pregabalin previously, drug abuse, cognitive disorders and patients refused to share in study protocol; all were excluded from our research.
In order to create random number list, computer generated block randomization was done. Each number refers to one category. Every number was then put in a sealed opaque envelope. All patients freely chose an envelope and sent it to the anesthesiologist, who added the number to the computer list and allocated it to a group. The anesthesiologist and surgeon were blinded to the randomization like the participants.
The day before surgery, a pre-operative history taking, and physical examination were done. Also, the patients were overlooked to standard 0-10 visual analogue score (VAS) to be familiar with it during assessment (0 indicates no pain and 10 indicates worst imaginable pain). Random allocation of the patients into two groups (40each) was performed:
Group I (40 patients): where patients received pregabalin oral capsule 300 mg (Amoun pharmaceutical company, Egypt) one hour before surgery with few sips of water.
Group II (40 patients): where patients received placebo oral capsule one hour before surgery with few sips of water.
After arrival to operating theatre, an intravenous access was inserted, 2mg midazolam as a sedative was given. Patients were attached to standard monitoring (ECG, pulse oximeter, non-invasive arterial blood pressure). In addition, all participants received ringer’s infusion. Also, local anesthetic solution (a mixture of 2% lidocaine, 0.5% bupivacaine and 1:200,000 adrenaline) was prepared and given at the incision site by insertion of needle through the caruncle over the posterior lacrimal crest and anterior ethmoidal nerve. Two small gauzes were soaked into a 0.1% adrenaline solution and put up in the nasal space, on the operated side, after putting lignocaine nasal spray in the nasal space. Head ring placed under the head to keep the head slightly elevated above chest plane to enhance the venous drainage. All cases enrolled in our study were performed similar technique of DCR operation by single occulo-plastic surgeon. Before starting the operation, nitroglycerin titration was started at rate 0.5-10μg/kg/min to maintain the mean arterial blood pressure of no more than 20% to 30% lower than baseline. Titration of nitroglycerin was stopped if mean arterial blood pressure reduced below 55 mmHg in healthy young adult patients. Ten minutes before the end of surgery, nitroglycerin infusion was completely stopped to resume the preoperative (basic) mean arterial blood pressure (to detect any bleeding sources if present after finishing the operation). After completion of the operation, patients were transferred to post anesthesia care unit. Pain scores were recorded postoperatively by using 0-10 VAS. Patients with VAS≥4 received rescue analgesia in the form of 0.5-1mg/kg pethidine. Time to first postoperative rescue analgesic request, and total analgesic consumption in the first 24h postoperatively were recorded. Incidence of complications were recorded during first 24 hours postoperatively.
Primary outcome: Postoperative pain was assessed using 0-10 VAS which were measured at 1, 2, 4, 8, 12, and 24h postoperative.
Secondary outcome:
- The total dose of nitroglycerin (mg) used for each patients.
- The quality of surgical field was also recorded using Fromm and Boezaart scale [14], where 0 grade represented no bleeding, 1 grade represented slight bleeding & no need for blood suction, 2 grade represented slight bleeding & sometimes blood had to be suctioned, 3 grade represented slight bleeding & blood had to be often suctioned (operative field was clear for few seconds after suction), 4 grade represented average bleeding & blood had to be frequent suctioned (operative field was clearly visible immediately after suction), 5 grade represented massive bleeding& regular blood suction required (continuous non stopped bleeding that may be faster than suction and required another suction and multiple gauze ; hence surgical field became more obscured and non-visible that made the operation so hard and might be difficult).
- Time to first postoperative rescue analgesic request was recorded.
- Total analgesic consumption in the first 24 h postoperatively was recorded.
- Incidence of complications including postoperative nausea and vomiting (PONV), dizziness, visual disturbance, headache, urine retention, and sedation were recorded during first 24 hours postoperatively.
Sample size calculation
Based on the results of the previous study [15], the sample size calculation revealed that a minimum of 37 patients should be enrolled for detecting a clinically significant difference in VAS between the two groups of 1.3 at standard deviation of 1.5, α error of 0.05 and study power of 80%. Assuming a 10% dropout rate, we decided to include 40 patients in each group.
Statistical analysis
Statistical analysis was done by SPSS version 16 (SPSS Inc., Chicago, IL, USA). The normality of data was checked by Kolmogorov– Smirnov test. The continuous data were presented as mean ± standard deviation (SD) or median with interquartile range and were compared by using Student’s t-test or the Mann-Whitney U-test as appropriate. While the categorical data were expressed as number (n) or percentage (%) and compared using the chisquare test. P< 0.05 was considered significant.
Results
Our study enrolled 80 patients scheduled for dacryocystorhinostomy surgery under local anesthesia; 40 patients in each group were included. No patients were excluded from our study (Figure 1). No statistically significant differences found as regarding demographic data as age, sex, body weight, ASA physical status class I&II and duration of operation (Table 1).

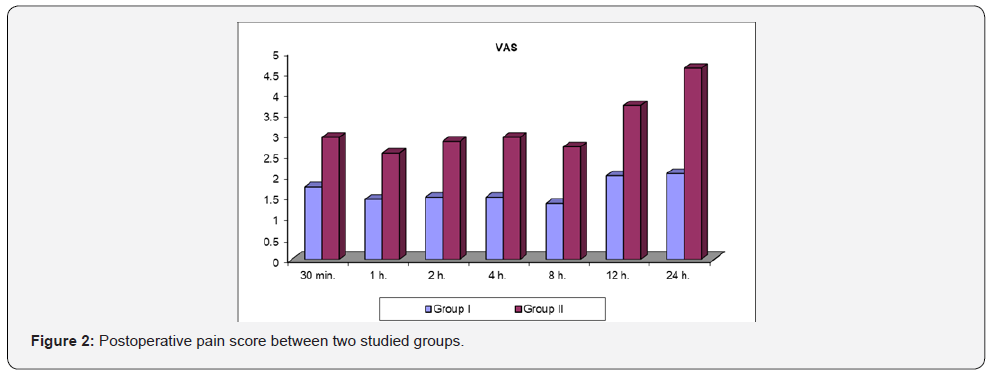
As regarding pain intensity variations based on VAS, there was significant difference between both groups; pain score was much lower in group I than in group II at 30 min, 1st, 2nd, 4th, 8th, 12th and 24th hours postoperative (Table 2, Figure 2).

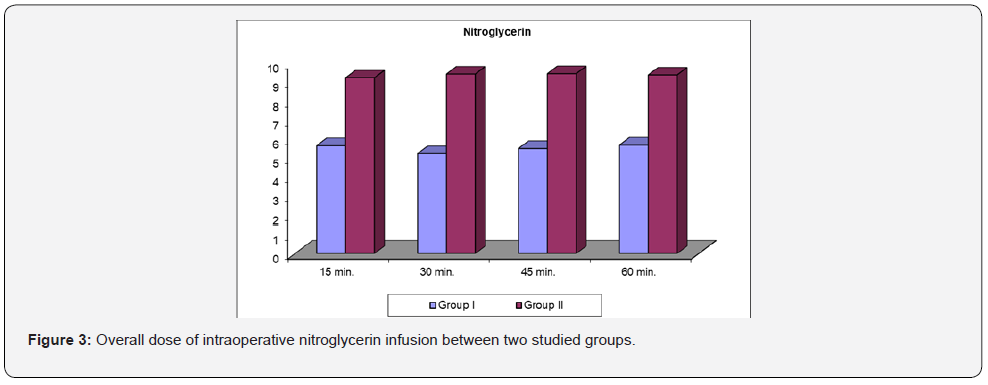
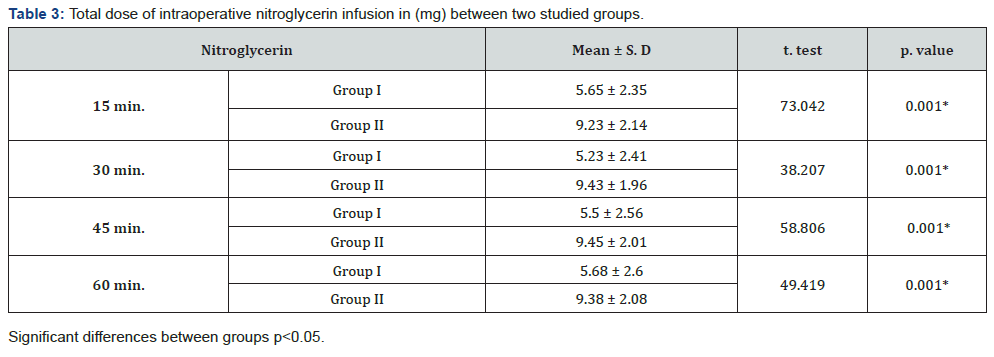
Pregabalin group (group I) had significant difference than placebo group (group II) as regarding infusion rates of nitroglycerine throughout the whole procedure at all measured intervals (Table 3, Figure 3).
Operative field conditions were better in group I than in group II; as Fromm Boezaart scale was significantly lower in group I compared to group II, P value 0.007 (Figure 4).
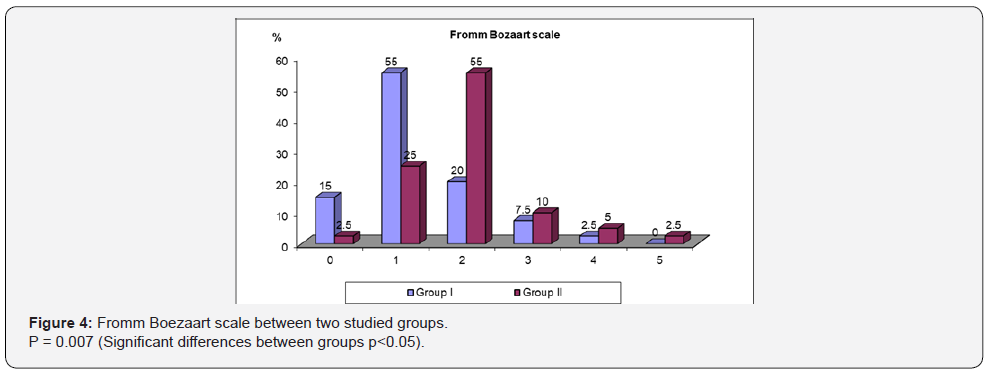
As regarding total percentage of patients underwent operative field suction were much lower significantly in group I than group II, p value= 0.001 (Table 4).

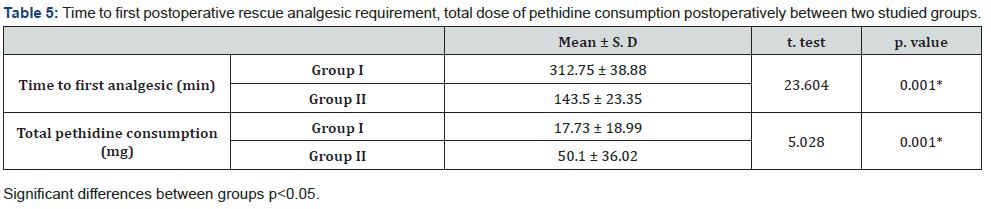
Time to 1st postoperative analgesic requirement was longer in pregabalin group (312.75±38.88min) than in placebo group (143.50±23.35min) with significant difference. The dose of total pethidine consumption (mg) during 1st 24 hours was significantly decreased in pregabalin group (17.73±18.99mg) than in placebo group (50.10±36.02mg) (Table 5).
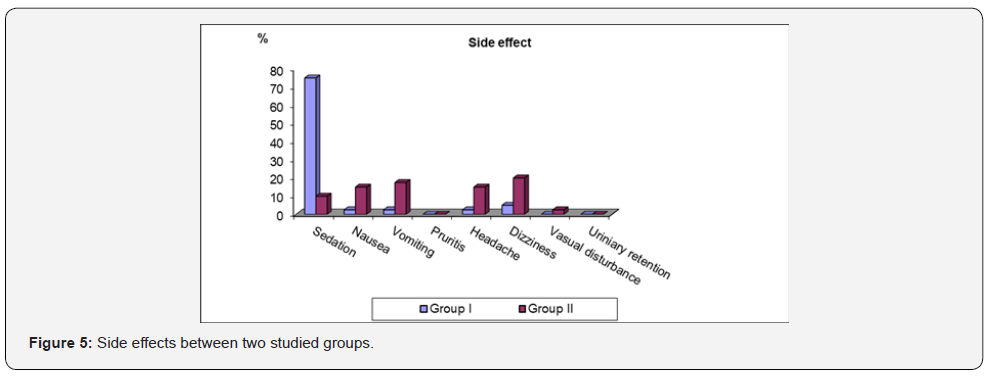
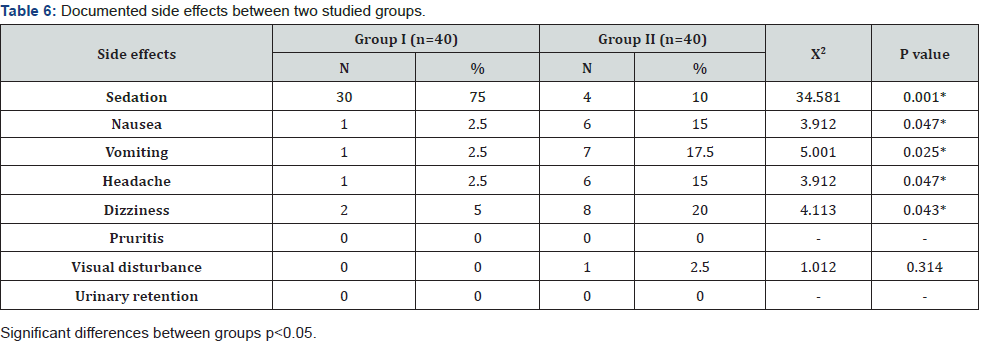
As regarding sedation, the patients in pregabalin groups were sedated than patients in placebo groups with significant differences between both groups. Incidence of side effects as nausea, vomiting, headache and dizziness were much lower in group I than in group II with significant differences between both groups. While other documented side effects as pruritus, visual disturbance and urinary retention; there was no significant differences between two groups (Table 6, Figure 5).
Discussion
Pregabalin is gamma amino butyric acid analogue that could control postoperative pain and reduce postoperative complication that can lead to reduction in consumption of postoperative analgesia and facilitate early discharge from hospital [4]. Our present study was used to evaluate the effect of preoperative administration of oral pregabalin on postoperative pain, deliberate hypotension and postoperative analgesic requirement on patients underwent DCR under local anesthesia. Our present study approved that postoperative pain intensity based on VAS, total dose of nitroglycerine infusion intra-operatively, Fromm and Boezaart scale guiding the quality of surgical field, total consumption of pethidine postoperative and incidence of complications were much lower in pregabalin group than the placebo group, with longer time to 1st postoperative rescue analgesic request in pregabalin group. This was attributed to the inhibitory effect of gabapentiniod on membrane voltage dependent calcium channels, which reduced calcium influx at nerve terminal and consequently reduced the neurotransmitters release producing analgesia [16]. Our results as regarding postoperative pain intensity were in line with several studies; study conducted by Eskandar et al. [17] that determined that oral 300mg pregabalin reduced VAS score significantly and total consumption of pethidine also reduced. Also, study conducted by Alimian et al. [20], observed that postoperative pain intensity were much lower in patients received oral 300mg pregabalin an hour before surgery. Postoperative opioid consumption was lower in the pregabalin group than control group. As concept of reduction of total nitroglycerin infusion intraoperative in pregabalin group than placebo group, this was supported by study conducted by Adel et al [21] who used gabapentin (pregabalin derivatives) preoperatively during functioning endoscopic sinus surgery and noticed the reduction of hypotensive agents used intraoperative with potentiated deliberate hypotension that caused minimal blood loss achieving clear surgical field. Also our results were in line with study recorded by Suneel et al. [20] who compared two hours preoperative administration of gabapentin on hemodynamic alterations in response to intubation and pin insertion in the skull during elective craniotomy and showed that gabapentin attenuated the alteration in heart rate and mean arterial blood pressure due to pin insertion. Controversy to our results; study by Chang et al. [21] who reported that 300mg of pregabalin in two separate doses, one dose of 150mg before the operation and another dose of 150mg 12 hours after surgery; he found no significant difference in the pain intensity of cholecystectomy patients between pregabalin group and placebo group after the operation. Also, in contrast to our study regarding the dose of pregabalin, study conducted by Paech et al. [10] who did not notice any reduction in pain intensity after gynecological operation after preoperative pregabalin administration. Other study conducted by White et al. [22] was in contrast to our study who reported that pregabalin in dose 75mg up to 300mg as preoperative premedication (anxiolytic) in patients underwent elective surgery versus placebo group, showed that pregabalin did not reduce the pain intensity postoperative although pregabalin increase the level of sedation. As regarding analgesic consumption and time to first postoperative rescue analgesic request; our results reported prolonged time for first analgesic requirement and reduction of postoperative opioid consumption in pregabalin group. Parallel to our study; a study conducted by Menda et al. [23]. Who reported that use of single dose of gabapentin in patients underwent cardiac surgery; there was reduction in pain intensity and reduction of morphine requirement postoperative. Also in line with our results, study by Jokela et al. [6] who used two different studies on pregabalin; in 1st study; 300mg oral pregabalin given in patients underwent laparoscopic hysterectomy, he concluded that perioperative pregabalin reduced postoperative oxycodone consumption with enhanced analgesia. In 2nd study by the same author; 150mg of oral pregabalin was given in patients underwent minor gynecological surgery; he found that there was no difference in the amount of postoperative required analgesia. Also, in line with our study; study by Ghai et al. [24] who approved that time to 1st analgesic requirement was longer in pregabalin group versus gabapentin group that may be attributed to quicker onset and enhanced analgesic effects of pregabalin. In contrast to our results, study by Mathiesen, et al. [25] documented that combined use of pregabalin with paracetamol or dexamethasone wasn’t associated with reduced pain intensity or opioid consumption after abdominal hysterectomy. In our study, side effects reported were sedation, nausea, dizziness, vomiting and headache that were significantly lower in pregabalin group than placebo group, this may be attributed to use of pethidine in placebo group; whereas for pruritus, visual disturbance and urinary retention there were no significant differences between both groups. In line with our results, a study conducted by Sharaswat et al. [26] who concluded that the common side effects that were reported with pregabalin were sedation and somnolence in the early postoperative period that subsided throughout 2-3 hours. In contrast to our results; a study conducted by Safari et al. [15] who concluded that apart from sedation, nausea and vomiting were also seen in pregabalin patients but much less in placebo group that was with no statistically difference between both groups of pregabalin and control group.
Conclusion
Preoperative administration of oral pregabalin has a prominently significant outcome in reducing postoperative pain, inducing hypotensive effects achieving proper visualization of surgical field, producing higher degree of sedation for patients, prolonging the duration of postoperative rescue analgesia and decreasing the total dose of postoperative pethidine requirement with minimal unwanted postoperative complications.
Limitations of the Study
Few limitations of our study were firstly the need to recognize the long term effects on chronic pain as pregabalin was administrated in a single dose that its half-life was 5-7 hours; this resulted in reduction of the effects over time, so calculated optimal dose couldn’t be fully recognized. Secondly, we did not compare different doses of pregabalin that might produce the maximum effects and the least side effects which need a bigger sample size and can determine sedation score and its relation to increased doses. For these previous points further investigations were recommended for better future results.
References
- Patrinely JR, Gigantelli JW (1988) Dacryocystorhinostomy. In: Linberg JV (Ed.) Lacrimal surgery. vol. 5, Churchil Livingstone, New York, USA, p. 151.
- McNab AA (1988) Dacryocystorhinostomy. Manual of orbital and lacrimal surgery. 2nd edn, Butterworth- Heine-Mann, Oxford. London, UK, Pp. 105-116.
- Julius D, Basbaum AI (2001) Molecular mechanisms of nociception. Nature 413(6852): 203-210.
- Robert WH and Christoher LW (2001) Acute postoperative pain. In: Ronald DM, Millers Anesthesia. 7th edn, Churcchil Livingstone, Philadelphia, USA, Pp. 2758-2760.
- Imani F, Safari S (2011) Pain relief is an essential human right’’, we should be concerned about it. Anesth Pain 1(2): 55-57.
- Jokela R, Ahonen J, Taligren M, Haanpaa M, Kortilla K (2008) A randomized controlled trial of perioperative administration of pregabalin for pain after laparoscopic hysterectomy. Pain 134(1-2): 106-112.
- Mathiesen O, Jacobsen LS, Holm HE, Randall S, Adamiec-Malmstroem L, et al. (2008) Pregabalin dexamethasone for postoperative pain control: a randomized control study in hip varthroplasty. Br J Anesth 101(4): 535-541.
- Ben-Menachem F (2004) Pregabalin pharmacology and its relevance to clinical practice. Epilepsia 45(Suppl 6): 13-18.
- Gilron I (2007) Gabapentin and pregabalin for chronic neuropathic and early postsurgical pain: current evidence and future directions. Curr Opin Anaesthesiol 20(5): 456-472.
- Michael JP, Raymond G, Sebastian C, Karen S, Tracey C, et al. (2007) Doherty, A Randomized, Placebo-controlled trial of preoperative oral pregabalin for postoperative pain relief after minor gynecology surgery. Anesth Analg 105(5): 1449-1453.
- Gajraj NM (2007) Pregabalin its pharmacology and use in pain management. Anesth Analg 105(6): 1805-1815.
- Bahram N, Siamak R, Abtin H (2014) Pre-emptive gabapentin versus pregabalin for acute postoperative pain after external dacryocystorhinostomy surgery under local anesthesia: A randomized placebo- controlled trial. Nautilus 128: 43-51.
- Turan A, Kaya G, Karamanlioglu B, Pamukcu Z, Apfel C (2006) Effect of oral gabapentin on postoperative epidural analgesia. Br J Anaesth 96: 242-246.
- Jacobi KE, Bohm BE, Rickauer AJ, Jacobi C, Hemmerling TM (2000) Moderate controlled hypotension with sodium nitroprusside does not improve surgical condition or decrease blood loss in endoscopic sinus surgery. J Clin Anesth 12(3): 202-207.
- Mahzad A, Farnad I, Valiollah H, Poupak R, Mahshid S, et al. (2012) Effects of Single-Dose Pregabalin on Postoperative Pain in Dacryocystorhinostomy surgery. Anesth Pain Med 2(2): 72-76.
- Todd RD, McDavid SM, Brindley RL, Jewell ML, Currie KP (2012) Gabapentin inhibit catecholamine release from adrenal chromaffin cells. Anesthesiology 116(5): 1013-1024.
- Eskandar AM., Ebeid AM (2013) Effect of pregabalin on postoperative pain after shoulder arthroscopy. Egyptian J Anaesth 29(4): 363-367.
- Alimian M, Imani F, Faiz SH, Pournajafian A, Navadegi SF, et al. (2012) Effects of oral pregabalin premedication on postoperative pain in laparoscopic gastric bypass surgery. Anaesthesiol Pain Med 2(1): 12-16.
- Fahymy AM, Kamal KY, Mohamed MH (2012) Preoperative gabapentin augments intraoperative hypotension and reduces postoperative opioid requirements with functional endoscopic sinus surgery. Egypt J Anaesth 28(3): 189-192.
- Suneel PR, Unnikrishnan KP, Koshy T (2011) Gabapentin premedication decrease the hemodynamic response to skull pin insertion in patients undergoing craniotomy. J Neurosurg Anesthesiol 23: 110-117.
- Chang SH, Lee HW, Kim HK, Kim SH, Kim DK (2009) An evaluation of perioperative pregabalin for prevention and attenuation of postoperative shoulder pain after laparoscopic cholecystectomy. Anesth Analg 109(4): 1284-1286.
- White PF, Tufanogullari B, Tylor J, Klein K (2009) The effect of pregabalin on preoperative anxiety and sedation level: a dose ranging study. Anesth Analg 108(4): 1140-1145.
- Menda F, Koner O, Sayin M, Ergenoglu M, Kucukaksu S, et al. (2010) Effects of single dose gabapentin on postoperative pain and morphine consumption after cardiac surgery. J Cardiothoracic Vasc Anesth 24(5): 808-813.
- Jokela R, Ahonken J, Tallgren M, Haanpaa M, Korttila K (2008) Premedication with pregabalin 75 0r 150 mg with ibuprofen to control pain after day care gynecological laparoscopic surgery. Br J Anaesth 100(6): 834-840.
- Mathiesen O, Rasmussen ML, Dierking G, Lech K, Hilsted KL, et al. (2009) Pregabalin and dexamethasone in combination with paracetamol for postoperative pain control after abdominal hysterectomy. A randomized clinical trial. Acta Anaesthesiol Scand 53(2): 227-235.
- Sharaswat V, Arora V (2008) Pre-emptive gabapentin versus pregabalin for acute postoperative pain after surgery under spinal anesthesia. Indian journal of anesthesia 52(6): 829-834.






























