Comparative Study Following Addition of Epinephrine (0.2mg) to Spinal Hyperbaric Bupivacine (0.5%) in Normotensive and Pre-Eclamptic Parturients Undergoing Elective Cesarean Section: A Pilot Study
Mohamed Fouad Mohamed Elmeleigy*
Lecturer of anesthesia and intensive care, Banha University, Egypt
Submission: March 03, 2020; Published: March 11, 2020
*Corresponding author: Mohamed Fouad Mohamed Elmeleigy, Lecturer of anesthesia and intensive care, Banha University, Egypt
How to cite this article: Mohamed F M E. Comparative Study Following Addition of Epinephrine (0.2mg) to Spinal Hyperbaric Bupivacine (0.5%) in Normotensive and Pre-Eclamptic Parturients Undergoing Elective Cesarean Section: A Pilot Study . What is the evidence?. J Anest & Inten Care Med. 2020; 10(3): 555793. DOI: 10.19080/JAICM.2020.10.555793
Abstract
Introduction: Study compare effect of adding epinephrine to bupivacine-fentanyl mixture during spinal anesthesia for elective cesarean section in normotensive and pre-eclamptic parturients.
Methods: Twenty parturients who had given their consent and were scheduled for elective cesarean section under spinal anesthesia, where divided into four groups first group contain five normotensive parturients received 0.5% hyperbaric bupivacine plus fentanyl, the second group also contain five normotensive parturients received 0.5% hyper bupivacaine-fentanyl mixture plus epinephrine (0.2mg), the third group contain five severe pre-eclamptic parturients received hyperbaric bupivacine 0.5% plus fentanyl, the fourth group contain five severe pre-eclamptic parturients received hyperbaric bupivacine- fentanyl mixture plus epinephrine (0.2mg). The hemodynamics, anesthesia characteristics and adverse effects were observed.
Results: Mean heart rate didn’t significantly differ between groups either A, B or C and D. there is difference in percentage of drop of mean blood pressure from baseline between group A, B (statistically significance) and drop in C, D (not statistically significance). The anesthesia onset time for sensory block significantly (P=0.03) prolonged in group B than in group A (4.6±1.14 vs 2.8±0.84minute) and the same in group D than group C (4.2±0.45 vs 2.8±0.45min) (P=0.005), the time of sensory block to regress below L1 was significantly (P<0.03) prolonged in group B than group A (158.0±14.41 vs127.0±18.36 minute) and the same in group D than group C (172.0±7.58 vs 141.4±7.4 minute) (P<0.009). No significant difference between groups in incidence of pruritis, nauseas and or vomiting.
Conclusions: Several points emerged from current study first, intrathecal epinephrine (0.2mg) not associated with greater incidence of hypotension in normotensive and pre-eclamptic parturients. Second, intrathecal epinephrine prolongs Time to achieve highest sensory block and affect cephalade spread of the block. Lastly, sensory and motor block time prolonged but at expense of prolongation of length of PACU stay.
Keywords: Prothrombin complex concentrates; Vitamin K antagonists; Warfarin; Coagulopathy; Gastrointestinal hemorrhage
Introduction
The increased popularity of neuraxial block in cesarean section has led to decrease in maternal mortality and morbidity related to general anesthesia complications [1]. It became the preferred technique for majority of anesthesiologists as it offers many advantages including simplicity, rapid onset, reliable and dense block [2]. Pregnancy induced hypertension is major cause of obstetric morbidity and mortality. There is still some controversy about the best anesthetic technique in these patients [3]. Because of risk related to management of difficult airway and hemodynamic response related to laryngoscopy and tracheal intubation, general anesthesia is only chosen when regional anesthesia is contraindicated [4]. Recently, studies proved that spinal anesthesia is an appropriate choice for cesarean section of preeclamptic patients unless neuraxial anesthesia is contraindicated [5]. Neuraxial block in obstetric anesthesia has been emerged as technique of choice because of its better patient outcome, but the limited duration of action of intrathecal local anesthetic can be the limiting disadvantages for the use of this technique by anesthesia providers. To overcome this limitation and obtain better analgesia/anesthesia, opioid and non-opioid drugs added intrathecally in conjunction with local anesthetic [6]. Vasoconstrictors as epinephrine have been added to local anesthetic solution in attempt to maintain cardiovascular stability, increase duration, enhance neural blockade of local anesthetic and enhance analgesic activity of spinal injected opioids. This might be related to local vasoconstriction or direct effect on α-adrenergic receptors in spinal cord [7]. The aim of this Study is to show the effect of addition of epinephrine (0.2mg) to subarachnoid hyperbaric bupivacaine with opioids for cesarean section on hemodynamics and anesthesia characteristics in normotensive and hypertensive parturients.
Methods
This prospective, randomized, double blind pilot study was conducted at Benha university, following approval from Research Ethics committee, 20 non laboring parturients, age 18-40 years BMI <35kg/m2, carrying singleton pregnancy and scheduled to have elective cesarean section under spinal anesthesia were included in our study and all patients gave informed oral consent after detailed explanation of the procedure. Among them 10 women were normotensive (group A, B) and 10 were sever preeclampsia (group C, D) having blood pressure ≥160/110 requiring antihypertensive therapy (Nifedipine 10-20mg BD) parturients with coagulopathy (including those with platelet counts <75000), cardiac disease, chronic hypertension, renal disease, diabetes and those who refused or have contraindications to spinal anesthesia were excluded from the study. All patients in preeclampsia groups received 4gm loading dose of intravenous MgS04 followed by 1gm/h infusion for 24hour for seizure prophylaxis. All patients premedicated with intravenous ondansetron (4mg). In addition, in preeclamptic parturient antihypertensive medication was continued. Prehydration was done with 10ml/kg of lactate ringer over course of 15-20 minutes, the volume of administrated fluid was not restricted in preeclamptic patients because of contracted intravascular volume in these groups of patients and high incidence of hypotension caused by sympathetic block induced by spinal anesthesia. Standard monitor was attached and baseline hemodynamic variables (HR, SBP, DBP, MAP, SPo2) were recorded baseline blood pressure was measured as the mean of 2 readings taken 2 minutes apart after arrival of operation theatre and before doing any procedures. After aseptic measures, skin infiltration with 2% lidocaine a 25G pencil point spinal needle inserted the midline at L 3-4 or L 4-5 vertebral interspace with the patient in sitting position, after confirming a free flow of cerebrospinal fluid, the anesthetic solution were injected over 30 seconds, then patients immediately turned supine and wedge position maintained to minimize aortocaval compression. We didn’t supply oxygen unless spo2 decrease to <92%. Randomization was carried out using a computer-generated schedule and coded envelope were produced. With this system each patient was assigned to one of 4 groups:
a) Group A: 12.5 mg of hyperbaric bupivacine 0.5% (2.5ml) mixed with 20 μg fentanyl (0.2ml).
b) Group B: 12.5mg of hyperbaric bupivacine 0.5% (2.5ml) mixed with 20μg fentanyl (0.2ml) and 200μg epinephrine (0.2ml)
c) Group C: Severe preeclamptic parturients received 12.5mg hyperbaric bupivacine 0.5% (2.5ml) mixed with 20μg fentanyl (0.2ml).
d) Group D: preeclamptic parturients received 12.5mg hyperbaric bupivacine 0.5 (2.5ml) mixed with 20μg fentanyl (0.2ml) and 200μg epinephrine (0.2ml)
The injections were aseptically prepared by anesthesiologist who was not involved in the study. In each case, this was done based on instructions contained in the sealed randomized envelope. the patients, investigators, surgeons and recovery staff were all blinded to the patient’s spinal anesthesia injectate all spinal needles were inserted by the same blinded anesthesiologist. The same investigator was responsible for all intra operative care and for recording all observations during the procedure. Heart rate, blood pressure was recorded at 1-minute interval for the first 20 minutes then every 5 minutes till end of surgery. Hypotension was defined as more than 20% decrease in MAP compared to baseline in all groups (or SBP < 100mmHg in healthy parturients) and was treated with 5-10mg intravenous ephedrine or 50- 100μg phenylephrine boluses at discretion of anesthesiologist. Bradycardia defined as HR<50 bpm and treated with intravenous atropine 0.6 mg. The total amounts of intravenous administrated fluid, total doses of vasopressors and number of hypotensive episodes were recorded as well. The levels of sensory block were evaluated by pin- prick sensation in midline bilaterally at 2-minutes intervals. The following information were collected : Onset of sensory blockade to T6 level, maximum extension of sensory block and time until regression of sensory block below L1 level of motor block assessed using modified Bromage scale (0=no impairment; 1=unable to raise extended legs but able to move knees and ankles; 2=unable to extend legs or flex knees but able to move feet; 3=unable to flex ankles, knees, or hips) at 2 minutes intervals. The degree of motor block, onset Time and duration of block were recorded. Other complications also recorded as nausea, vomiting, purities and respiratory depression (spo2 ≤92% and respiratory rate<10bpm), blood loss (estimated in graded suction bottle and observation of soaked materials) and duration of surgery were also recorded. Post-operative in PACU, hemodynamics and block profile were monitored till sensory level regressed below L1 level and patients freely move the lower limb. The clinical data were recorded on a report from these data were tabulated and analyzed using the computer program SPss (statistical package for social science) version 20 to obtain:
Descriptive data
Descriptive statistics were calculated for the data in the form of:
a) Mean and standard deviation (±SD) quantitative data.
b) Frequency and distribution for qualitative data.
Analytical statistics
In the statistical comparison between the different groups, the significance of difference was tested using one of the following tests:
a) Mann- Whitney test: used to compare mean of two groups of quantitative data (non- parametric)
b) Wilcoxon test: used to compare mean of variables in different time periods of quantitative data (non- parametric).
c) Inter group comparison of categorial data was performed by using fisher exact test (FET)
P value < 0.05 was considered statistically significant (*) while > 0.05 statistically in significant. P value < 0.01 was considered highly significant (**) in all analysis.
Results
Ten normotensive women received hyperbaric bupivacine 0.5% spinal anesthesia, five received 0.5% hyperbaric bupivacinefentanyl mixture (group A), the other five received bupivacinefentanyl mixture plus 0.2ml epinephrine (group B). another ten sever preeclamptic women received hyperbaric bupivacine 0.5% spinal anesthesia, five received bupivacine. Fentanyl mixture (group C) and the other five received bupivacine- fentanyl mixture plus 0.2ml epinephrine (group D) the patients of each two study groups were similar regarding (Age, weight, height, BMI, ASA) (Table 1).
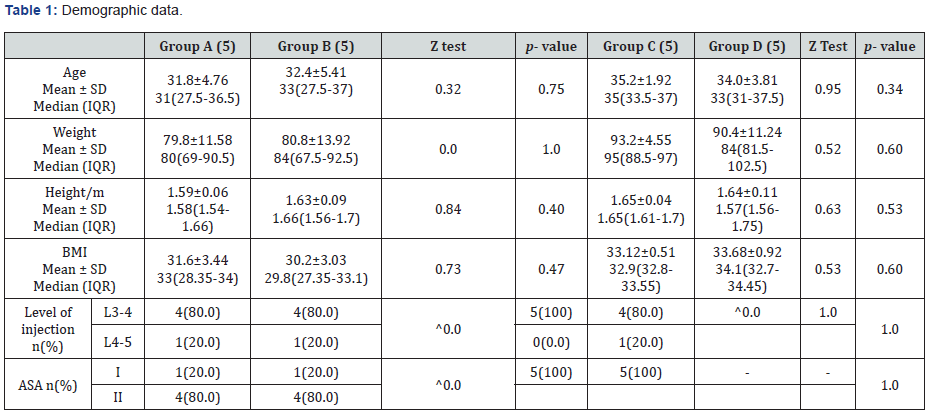
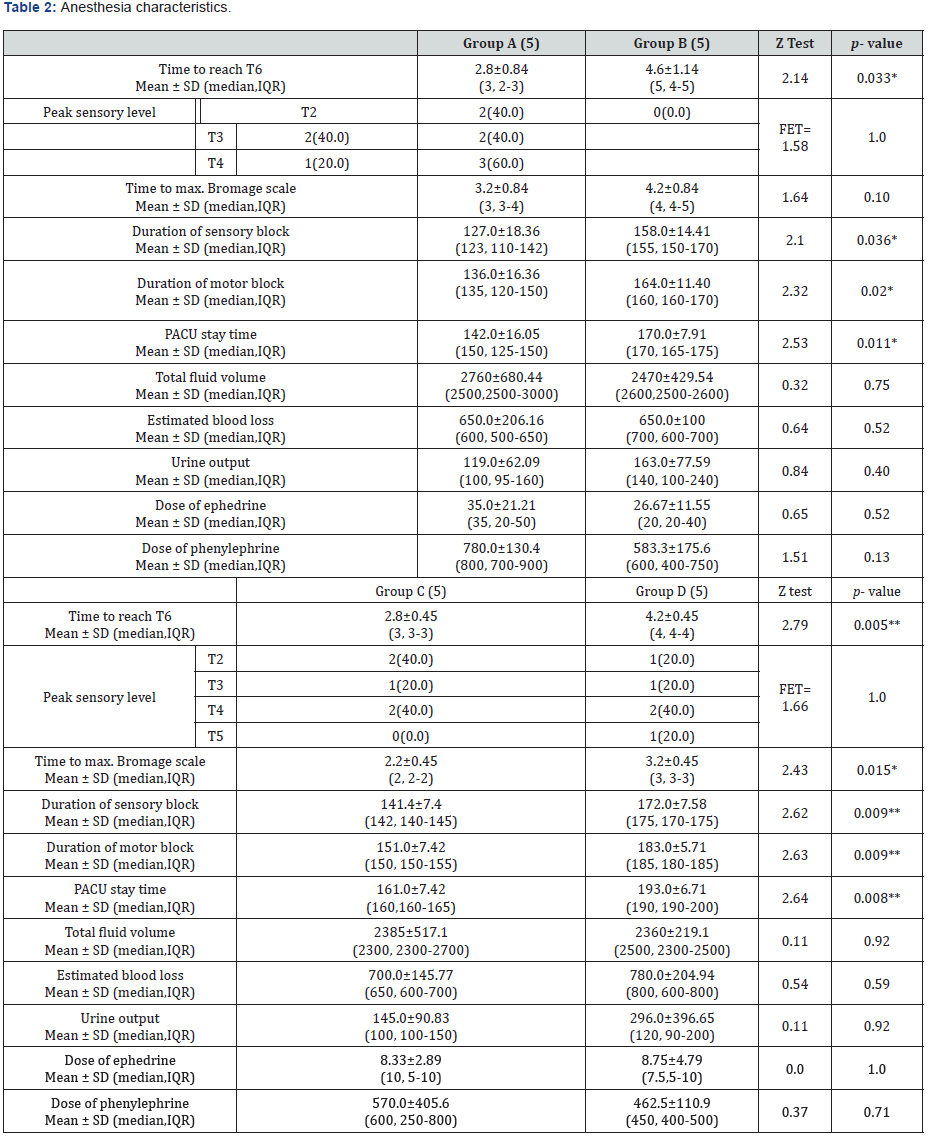
Spinal anesthesia was placed at L3-4 interspace in 80% of patients in group A and B with remainder of patients received anesthesia at L4-5 (P=1), in group C 100% of patients received spinal anesthesia at L3-4 inter space while 80% at same level in group D (P=1). The anesthesia onset time for desired spinal block level T6 was significantly (P=0.03) prolonged in group B than in group A (4.6±1.14 vs 2.8±0.84 minute) and the same in group D than group C (4.2±0.45 vs 2.8±0.45 minute) (p=0.005). in groups A, C (without epinephrine) the maximum block level extended above T3 in 4 patients (40%), with predominance of T2 (40%). In groups B, D (With epinephrine) the maximum block level extended above T3 only in 1 patient (10%), with predominance of T4 (50%) table 2. Time of block to regress below L1 was significantly (p<0.03) prolonged in group B than group A (158.0±14.41 vs 127.0±18.36 minute) and the same in group D than group C (172.0±7.58 vs 141.4±7.4minute) (P<0.009). the time of motor block to reach maximum bromage score was prolonged in group B than A (4.2±0.84 vs 3.2±0.84 minute) , this duration also prolonged in group D than group C but with statistical significance (P<0.01) (3.2±0.45 vs 2.2±0.45 minute) (Table 2).
The time for recovery of motor block significantly longer in group B than A (P<0.02) (164.0±11.4 vs 136.0±16.36 minute) and same in group D than C (183.0±2.7 vs 151.0±7.42 minute) (P<0.009). the length of PACU stay was significantly shorter in group A than group B (P<0.01) (142.0±16.05 vs 170.0±7.91 minute), the same in group C than group D (161.0±7.42 vs 18.3.0±5.71 minute (P<0.008) Table 2. Median number of hypotensive episodes is significantly less in group B than group A (P<0.03) (6 vs 8) and also les in group D than group C (4 vs 6) but without statistical significance (p0.5) table 3 the total dose of vasopressors are less in groups B, D than groups A, C respectively. Total volume of fluid infused were not significantly different between groups table 2. Nausea and/or vomiting occurred in 3 patients in group A, 1 in group B, 2 in group C and 3 in group D. table 3 pruritis noted in all groups with 3 patients in each of groups A, B and D, and 4 in group C developed pruritis the respiratory rate of all patients remained above 10 breaths per minute and oxygen saturation above 92% in all patients, with no reported cases of respiratory depression (Table 3).
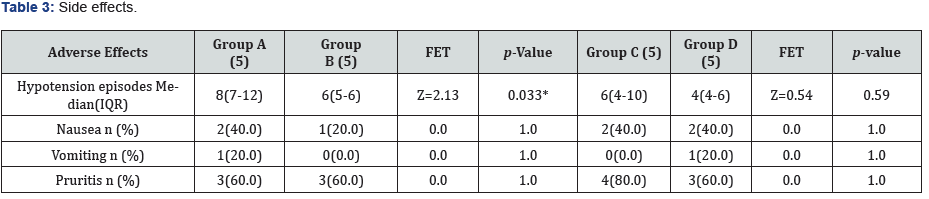
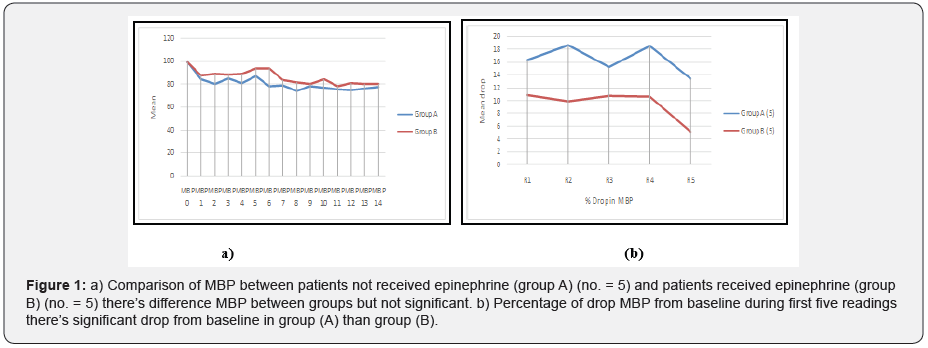
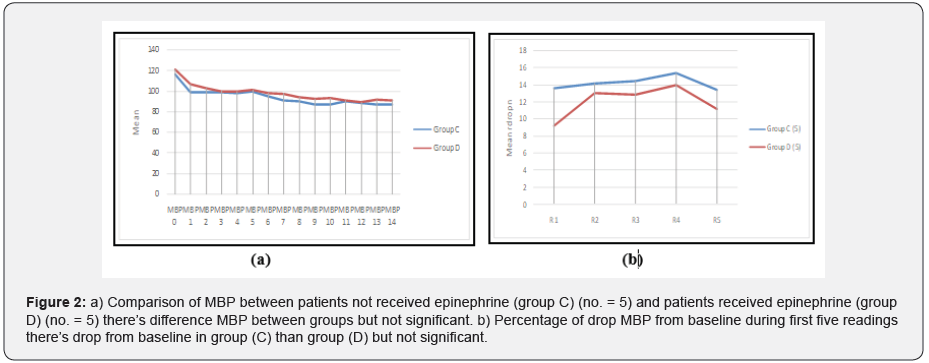
The mean heart rate didn’t significantly differ between groups either A, B or C and D mean blood pressure is higher in group B than A and in group D than C but no significant difference in mean blood pressure between group A, B or C, D but there is difference in percentage of drop of mean blood pressure from baseline between group A, B (Statistically significance) and group C, D (not statistically significance).
This difference in drop from baseline is evident in first 5 readings (25 minutes) (Figure 1 & 2).
Discussion
Spinal anesthesia for cesarean section has been the focus of considerable attention. Balanced subarachnoid anesthesia with combination of local anesthetic, an opioid and adrenergic drug, may be superior to techniques depend only on local anesthetic drugs. The current study was undertaken to determine the effect of addition of epinephrine (0.2mg) to combination of hyperbaric bupivacine 0.5% (12.5mg) and fentanyl (20μg) on hemodynamic stability and anesthesia characteristics for elective cesarean section in normal and severe preeclamptic parturients. The mean duration of sensory and motor block in normotensive and preeclamptic parturients provided by combination of 12.5 mg hyperbaric bupivacine and 20 μg fentanyl was (127, 136 minute), (141, 151 minute) respectively. The addition of 0.2 mg epinephrine to this intrathecal combination significantly prolong sensory, motor duration in normotensive and preeclamptic parturients (158,164 minute), (172 , 183 minute) respectively this prolongation of sensory and motor block at expense of increase the length of PACU stay but our study examine in hospital procedure. For many years it was proposed that epinephrine component of local anesthetic prolong duration of spinal nerve block through vasoconstriction which alters the intrathecal clearance of administrated drugs keeping drugs in contact with nervous tissue for longer period [8]. However, researchers demonstrate that, when epinephrine given into dogs CSF, it causes anesthesia sufficient to perform major surgery [9]. epinephrine alone (200-1000μg), injected in obstetric parturient CSF produce analgesia sufficient for vaginal delivery [10], so it is evident that epinephrine has its own spinal analgesia. Collin’s et al, [11], found 10-100μg subarachnoid epinephrine in decerebrated cats inhibit noxiously evoked activity in wide dynamic range (WDR) of spinal cord dorsal horn cell neurons. Similar work in animals has shown that subarachnoid administrated adrenergic agonists have direct antinociceptive activity, the authors of the research defined this as “spinal adrenergic analgesia” [12].
Others suspect that adrenoreceptors modify specific k channels in peripheral nerve axons, these changes lower impulse transmission safety margin and enhance the impulse blocking actions of any blockers of Na channels (i.e LA) if same occur in spinal nerve roots, epinephrine could have pharmacodynamic interactions with intrathecal injected opioids and local anesthetics by same mechanism [13]. Tejwani et al, [14] have shown that local anesthetics produce conformational changes in spinal cord opioid receptors that potentiate the binding of intrathecal morphine. Antinociceptive conformational changes have been also demonstrated between intrathecal α2 adrenergic receptor agonists (epinephrine) and opioids [15]. These observations beside lack of cross tolerance between α-adrenergic agonists and opioids and inefficiency of naloxone to catagonise α2 against effects [16], suggest the action of each agent at different spinal cord receptor Site (Local anesthetics inhibit Na channels, opioids inhibit voltage dependent Ca channels and epinephrine has α2 adrenergic action) [17]. so, inhibition of overall neuronal excitability may be synergistic rather than simple additive effect. Jean P. Racle et al, [18] show that sensory block of isobaric bupivacine spinal anesthesia can be prolonged with adding sufficient amounts of epinephrine as measured by time of 2 segment regression and time to regression to L2 level. This is in agreement with previous study of same authors on effect of 0.2mg epinephrine added to isobaric bupivacine [19] and with Moore’s results on the effect of 0.2mg epinephrine with hyperbaric bupivacine [20]. However, Chambers et al, [21], found in double blind study, sensory block prolongation that reached statistically significance only in the total duration of anesthesia when adding 0.2mg epinephrine to 3ml bupivacine 0.5% in 8% dextrose. Intrathecal epinephrine prolongs the onset time of sensory block with average 1.5-minute delay between groups with epinephrine to those without epinephrine. It also affects cephalade spread of block with 4 patients develop T2 block in groups without epinephrine while only 1 patient in epinephrine groups with extended block to T2. A study by Moore’s et al, [22] showed that adding epinephrine to mixture of fentanyl and hyperbaric bupivacine for spinal anesthesia delay onset time to achieve T4 sensory block level also Gautier et al, [23], shown that adding epinephrine to bupivacine fentanyl mixture allowed high quality analgesia with low sensory block level. Addition of epinephrine to local anesthetic solutions may provide circulatory support to antagonize undesirable hemodynamic effects of sympathetic block of regional anesthesia this circulatory support effect many be multi factorial. Many factors affect distribution of intrathecal administrated local anesthetic into CSF (e.g. speed of injection, dosage, baricity, concentration) [24]. The pka of local anesthetics and PH of the solution and surrounding medium have greatest effect on amount of free (unionized) drug available which affect the onset time of intrathecal administrated local anesthetic by influencing the extent and speed of diffusion of drug into its site of action [25]. Change in the PH of drug solution or surrounding tissue markedly affect the balance between ionized, unionized from of the drug [26]. The unionized portion of local anesthetic is responsible for penetration of neural tissue membrane while neural block is the function of ionized portion [27]. increase in the PH will favor ionized form while decrease in the PH will shift equilibrium towards unionized form [26].
0.5% hyperbaric bupivacine with 8.25% dextrose commercially prepared has a PH of 5.41, addition of 20μg fentanyl with PH 5.67 cause little change of the PH to 5.45. Epinephrine has a PH of 3.55 when added to the bupivacine Fentanyl mixture, the PH becomes acidic. Epinephrine 100μg decreases the PH to 4.65 and the PH lowers to 4.50 when 200μg epinephrine added. Addition of epinephrine to bupivacine- fentanyl mixture acidified the mixture; this creates less free base (non- ionized) and slow the onset of action. The Henderson-Hassel Bach equation pka=PH + log cations/amines. At PH 5.45 the ratio of unionized to ionized bupivacine 1:198 addition of 100μg epinephrine reduces the PH and the ratio becomes 1:1360. After 200μg epinephrine the ratio becomes 1:2180. The lower concentration of free (unionized base) which is responsible for membrane penetration may be the cause of delayed onset when epinephrine added to intrathecal bupivacine- fentanyl mixture. This delaying of the onset by addition of epinephrine provides greater circulatory and hemodynamic stability during onset of spinal block, besides decrease cephalade spread of local anesthetics with less extensive sympathetic block. The cardiovascular effect of regionally injected epinephrine appears in 3-5 minutes and achieve maximum value in 10-15 minutes, and this maintained for 15-30 minutes and then decrease during the next 30 minutes. This is evident in less drop of MBP from baseline especially in first 4-6 readings (20-30 minutes) of epinephrine injection. This especially obvious in normotensive patients than preedamptic parturients who are already vasoconstricted and respond by less vasodilatation to sympathetic block. this effect may be due to α- agonist effect of epinephrine in this dose (0.2mg) which counterbalance the systemic B adrenergic effects. Bostrom et al, [28], shown that less incidence of hypotension in patients in the group that contained epinephrine (half that in no epinephrine group), suggesting some benefit of adding epinephrine to intrathecal injectate. A meta-analysis of De oliveria J [29], found that less incidence of hypotension with intermediate dose range (100-200μg) of intrathecal epinephrine and referred that to predominant α-agonist effect at this dose range. Opioids administrated intrathecally cause significant pruritis. Despite, many studies as comann study [30] have shown that intrathecal administrated epinephrine decreases incidence of intrathecal opioid induced purities, others as Guiter study [23] which compared labor analgesia using intrathecal bupivacinefentanyl with or without epinephrine, they found no statistically significant reduction in incidence of pruritis in epinephrine group. In our study there is no difference in incidence of pruritis between groups. No significant difference between groups in incidence of nausea and/or vomiting. It is possible that proemetic properties of intrathecal opioids that enhanced by delayed clearance due to intrathecal epinephrine was counterbalanced by hemodynamic stability and maintenance of blood flow to emetogenic areas of the medulla [31]. No reported cases of respiratory depression this may be due to less systemic resorption which will decrease plasma concentration and enhance analgesic effect, besides lipophilic opioids have no rostral migration [32]. The volume of injectate in epinephrine containing groups were 0.2ml larger than other groups, this small volume difference will not affect block extension. Conclusion, several important findings have emerged from current pilot study. First, intrathecal epinephrine (0.2mg) not associated with greater incidence of hypertension in normotensive and preeclamptic parturients as shown by less drop of MBP from baseline which is more oblivions in normotensive than preeclamptic parturients. Seconds, intrathecal epinephrine prolong time to achieve highest sensory block and affect cephalade spread of the block which provide greater hemodynamic stability during the onset of the block. Lastly, the intrathecal epinephrine can also use as adjuvant to prolong time of sensory and motor block but at expense of prolongation of the length of PACU stay. All these findings need further investigations over large sample size and also effect on neonatal outcome should be taken into considerations by assenting fetal Apgar score, blood gases, heart rate and uterine blood flow.
References
- Hawkins JL, Koonin LM, Palmer SK, Gibbs CP (1997) Anesthesia related deaths during obstetric delivery in the united states 1979-1990. Anesthesiology 86(2): 277-284.
- Reisner LS, Lin D (1994) Anesthesia for cesarean section. In : Chestnut DH, (Edt.), Obstetric Anesthesia Principles and Practice, pp. 459-486.
- Flood P, Rolline MD (2015) Anesthesia for obstetrics (8th ), pp. 2344-2348.
- Endler GC, Mariona FG, Sokol RJ, Staven Son LB (1988) Anesthesia- related maternal mortality in Michigan, 1972- 1984. Am J Obstet Gynecol 159(1): 187-193.
- Aya AG, Mangin R, Vialles N, Ferrer JM, Robertc, Ripart J, et al. (2003) Patients with sever preeclampsia experience less hypotention during pinal anesthesia for elective cesarean section delivery than healthy parturients a prospective cohort comparison. Anesth analg 97(3): 867-872
- Salinas FV, Liu SS (2002) Spinal anesthesia local anesthetics and adjuncts in the ambulatory setting. Best pract Resclin anesthesiol 16(2): 195-210.
- Armstrong IR, Littlewood DG, Chambers WA (1983) Spinal anesthesia with tetracine effect of added vasoconstrictors Anesth analg 62(9): 793-795.
- Collins JG, Kithata LM, Homma E, Suzukawa M (1981) Spinal cord effects of epinephrine. Anesth Analg 60(12): 913-914.
- Leimdorfer A, Metzner WRT (1949) Analgesia and anesthesia induced by epinephrine. Am J physiol 157(1): 116-121.
- Priddle HD, Andros GJ (1950) Primary spinal anesthetic effect of epinephrine. Anesth Analg 29(3): 156-162.
- Collins JK, Kitahate LM, Matumoto HE, Suzukawa M (1984) spinally administrated epinephrine supress noxiously evoked activity of WDR neurons in dorsal horn of spinal cord. Anesthesiology 60(4): 269-275.
- Reddy SVR, Maderdrut JL, Yaksh TL (1980) Spinal cord pharmacology of adrenergic agonist mediated antinociception. J pharmacol Expther 213(3): 523-533.
- Sinnott CJ, Cogswell 111 LP, Johnson A (2003) On the mechanism by Which epinephrine poteniate lidocaine peripheral nerve block. Anesthesiology 98(1): 181-188.
- Tejwani GA, Rattan AK, McDonald JS (1992) Role of spinal opioid receptors in antinociceptive interactions between intrathecal morphine and bupivacine. Anesth Analg 74(5): 726-734.
- Ossipov MH, Suarez LJ, Spaulding TC (1989) Antinociceptive interactions between alpha 2 adrenergic and opiate agonists at the spinal level in rodents. Anesth analg 68(3): 194-200.
- Yaksh TL, Reddy SVR (1981) Studies in the primate on analgesic effects associated with intrathecal actions of opiates, a adrenergic agonists and baclofen. Anesthesiology 54(6): 451-467.
- Duggan Aw, North RA (1984) Electrophysiology of opioids pharmacold Rew 35: 219-281.
- Jean P Racle, Abdellatif Bankhadra, Jean Y Poy, Bernard G Leizal (1987) Effect of increasing amounts of epinephrine during isobaric bupivacine spinal anesthesia in alderly patients. Anesth Analg 66(9): 882-886.
- Jean P Racle, Benkhadra A, Poy JY, Gleizal B. Prolongation of isobaric bupivacine spinal anesthesia with epinephnine and clonidine for hip surgery in elderly. Anesth Analg 66(5): 442-446.
- Moore DC (1980) Spinal anesthesia: bupivacine compared with tetracine. Anesth Analg 59: 743-750.
- Chambers WA, Littlewood DG, Scott DB (1982) Spinal anesthesia with hyperbaric bupivacine: effect of added vasoconstrictors. Anesth Analg 61: 219-252.
- Moore CH, Wilhite A, Pan PH, Blass NH (1992) The addition of epinephrine to subarachnoid administrated hyperbaric bupivacine for cesarean delivery: the effect on onset time. Reg Anesth17(4): 202-204.
- Gauteir PE, Debry F, FanardL, van steenberge A, Hody JL (1997) Ambulatory combined spinal- epidural analgesia for labor: influence of epinephrine on bupivacine-sufentanil combination. Reg Anesth 22(2): 143-149.
- Van zundert A, Dewolf A (1988) Extent of anesthesia and haemodynamic effects after subarachnoid administration of bupivacine with epinephrine. Anesth analg 67(8): 784-787.
- Covino BG (1986) Pharmacology of local anesthetic agents. Br J anesthesia 58: 701-716.
- Carpenter RL, Mackey DC (1989) Local anesthetics. In: Barash PG, Cullen BF, stoleing RK, (Edt.), Clinical anesthesia, pp. 371-382.
- Stanton-Hicks M (1988) Pharmacology of local anesthetics In: Waugaman W, Rigor B, Katzl et al. (Edt.), Principles and practices of Nurse Anesthesia Norwalk conneticut, Appleton and lange, pp. 220.
- Bostrom MA, Pakiz AM, Melnyk DL, Benke G, Cohen S (1994) Spinal anesthesia with meperidine will epinephrine prolong its duration? AANA J 62(3): 267-272.
- de Oliveira GS Jr, Balliu B, Nader A, McCarthy RJ (2012) Dose-ranging effects of intrathecal epinephrine on anesthesia/analgesia: a meta-analysis and metaregression of randomized controlled trials. Reg Anesth Pain Med 37(4): 423-432.
- CamannW, Minzter B, Denney R, Dattas (1993) Intrathecal sufentanil for labor analgesia: effects of added epinephrine Anesthesiology 78(5): 870-874.
- Borgeat A, Ekatodramis G, Schenker CA (2003) Postoperative nausea and vomiting in regional anesthesia: a review. Anesthesiology 98(2): 530-547.
- Verborgh C, Van der Auwera, Noorduin H, Camu F (1988) epidural sufentanial for postoperative pain relief: effect of adrenaline. Eur J Anesthesiol 5: 183-191.






























