Ropivacaine - Fentanyl an Alternative to Bupivacaine - Fentanyl for Major Lower Limb and Lower Abdominal Surgeries - A Comparative Study
Shilpashri AM*, Keerthana DS and Priya R
Department of Anesthesiology, JJM Medical College, India
Submission: February 01, 2019; Published: February 06, 2019
*Corresponding author: Shilpashri AM, Department of Anesthesiology, JJM Medical College, Davangere, Karnataka, 577004, India
How to cite this article: Shilpashri A, Keerthana D, Priya R. Ropivacaine - Fentanyl an Alternative to Bupivacaine - Fentanyl for Major Lower Limb and Lower Abdominal Surgeries - A Comparative Study. J Anest & Inten Care Med. 2019; 8(3): 555736. DOI: 10.19080/JAICM.2019.08.555736
Abstract
Background: Spinal anesthesia is the most convenient anesthetic technique that offers many advantages over general anesthesia, including reduced stress response and improved post-operative pain relief. The administration of local anesthetics in combination with opioids intrathecally is an excellent technique for managing postoperative pain following abdominal, pelvic, orthopedic procedures on lower extremities. Ropivacaine, a newer amide local anesthetic produces similar sensory block to that of an equivalent dose of bupivacaine, with a reduced degree of motor block. It has an improved safety profile over bupivacaine with reduced central nervous system and cardiotoxic potential and hence is gaining favor. Objective: To compare the clinical effects of intrathecal ropivacaine-fentanyl with bupivacaine-fentanyl for major lower limb and lower abdominal surgeries. Methods: 100 patients belonging to ASA physical status I & II scheduled for lower abdominal and lower limb surgeries were randomly selected for the study and were divided into two groups of 50 each. Group RF patients received 2ml of 0.75% isobaric (15mg) ropivacaine +0.5ml (25 mcg) fentanyl+ 1ml of 25% dextrose intrathecally. Group BF patients received 3ml of 0.5% hyperbaric (15mg) bupivacaine + 0.5 ml (25 mcg) fentanyl intrathecally. The following parameters were monitored - onset and duration of sensory block, onset and duration of motor block, height of sensory block, hemodynamic parameters and adverse effects. Results: Both the groups were similar in demographic attributes. Both the groups had almost similar onset of peak sensory block, and maximum sensory height. Duration of sensory and motor block were significantly less in RF group. Quality of intraoperative analgesia, hemodynamic parameters were comparable in both groups, incidence of side effects were higher with group BF. Conclusion: Ropivacaine can be used successfully as an alternative to Bupivacaine for surgeries of lower abdomen and lower limb where early ambulation, decreased hospital stays, and decreased morbidity are appreciated.
Keywords: Ropivacaine; Bupivacaine; Fentanyl; Intrathecal
Introduction
Central neuraxial blockade in the form of spinal/epidural is very popular for lower abdominal and lower limb surgeries as these techniques avoid the disadvantages associated with general Anaesthesia like airway manipulation, poly pharmacy and other untoward effects like postoperative nausea, vomiting, need for supplemental intravenous analgesics. Presently the most widely used drug Bupivacaine 0.5% is cardiotoxic and also produces motor blockade of prolonged duration.
Ropivacaine is a relatively newer amide (s-enantiomer) local anesthetic with high pka and low lipid solubility, and it is considered to block sensory nerves to greater degree than motor nerves and has similar local anesthetic properties and chemical structure to that of bupivacaine [1]. The newer drug ropivacaine being comparatively less cardiotoxic, also produces minimal motor blockade of shorter duration [2] which relieves the psychological distress of being immobile for a longer period of time after surgery compared to intrathecal bupivacaine during lower abdominal and lower limb surgeries [3]. Intrathecal opioids are commonly combined with local anesthetics to improve the onset time of block, duration and quality of analgesia both intraoperatively and postoperatively. Fentanyl being the latest, is hundred times more potent than morphine has been the latest tool in the armory of modern-day anesthesiologists [4]. Hence this study is designed to assess the onset and duration of sensory and motor blockade of Ropivacaine- Fentanyl and side effects if any compared to intrathecal Bupivacaine -Fentanyl during lower abdominal and lower limb surgeries.
Material and Methods
Methodology
This clinical study was conducted on hundred adult patients of ASA physical status I & II in the age group of 18 to 65 years, of either sex, posted for elective major lower limb & lower abdominal surgeries under spinal Anaesthesia after taking informed consent at Chigateri General Hospital, Woman and Children Hospital, and Bapuji Hospital attached to J.J.M. Medical College, Davangere
After institutional committee approval and written informed consent, a comparative study was carried out on hundred adult patients. Patients were randomly divided on an alternative basis into two groups of fifty each. Group RF (Ropivacaine – Fentanyl): Received 2ml of 0.75% Isobaric Ropivacaine(15mg) + 0.5ml Fentanyl(25mcg) + 1ml 25% dextrose and Group BF (Bupivacaine - Fentanyl): Received 3ml of 0.5% Hyperbaric Bupivacaine(15mg) + 0.5ml Fentanyl (25mcg).
A detailed history, general physical examination, systemic examination, airway assessment and spine examination were done. Routine laboratory investigations like complete blood picture, bleeding and clotting time, serological status for HIV and Hepatitis B were done. a) Inclusion criteria i. Age: 18 - 65years. ii. Gender: Males and Females. iii. A patient who fits into American society of anesthesiologists (ASA) physical status criteria I and II scheduled for elective major lower limb and lower abdominal surgery under subarachnoid block. iv. Patients who are willing and able to give informed written consent. v. Concomitant medications: The patient can take relevant medication for concomitant diseases like diabetes, hypertension etc. b) Exclusion criteria i. Patient refusal. ii. Age> 65 years or <18 years. iii. ASA Grade III or IV. iv. Patient with pre-existing neurological and spine deformities. v. Pregnant women and lactating mother. vi. Patients allergic to Local Anesthetics and Opioids. vii. Patient on anticoagulants/known coagulation disorder. viii. Local infection at the site of proposed puncture for spinal Anaesthesia.
Technique
Patient was shifted onto the OT table. ECG, non-invasive blood pressure, pulse oximeter monitors were attached, and baseline parameters was recorded. Lactated Ringer’s solution 8-10ml/kg was infused intravenously before the block. With the patient in sitting or left lateral position, under aseptic precautions subarachnoid block was performed by midline approach using 23 G Quinke Babcock spinal needle at L3-L4 intervertebral space and the patient received one of the two study drugs
[Group RF: 2ml 0.75% isobaric ropivacaine(15mg) + 1ml 25% dextrose +0.5ml fentanyl (25mcg)] [Group BF: 3ml 0.5% hyperbaric bupivacaine(15mg) + 0.5ml fentanyl (25mcg)]
Sensory blockade was assessed as the loss of pin-prick sensation at the site of surgical incision. Onset and duration of motor blockade was assessed using modified bromage scale. Highest level of sensory block and duration of analgesia (sensory block) which is the time from onset of analgesia to time of request for rescue analgesics were noted. Complications such as bradycardia, hypotension, nausea & vomiting, pruritis, shivering, if any were noted intra operatively. Postoperatively, monitoring of vital signs was continued every 30 minutes upto 6 hours.
Statistical Methods
Descriptive and inferential statistical analysis has been carried out in the present study. Results on continuous measurements are presented on Mean ± SD (Min-Max) and results on categorical measurements are presented in Number (%). Significance is assessed at 5 % level of significance. Student t test (two tailed, independent) has been used to find the significance of study parameters on continuous scale between two groups (Inter group analysis) on metric parameters. Chi-square/Fisher Exact test has been used to find the significance of study parameters on categorical scale between two or more groups.
Statistical software
The Statistical software namely SAS 9.2, SPSS 15.0, Stata 10.1, Med Calc 9.0.1, Systat 12.0 and R environment ver.2.11.1 were used for the analysis of the data and Microsoft word and Excel have been used to generate graphs, tables etc.
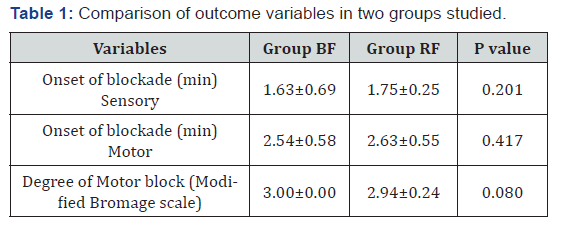
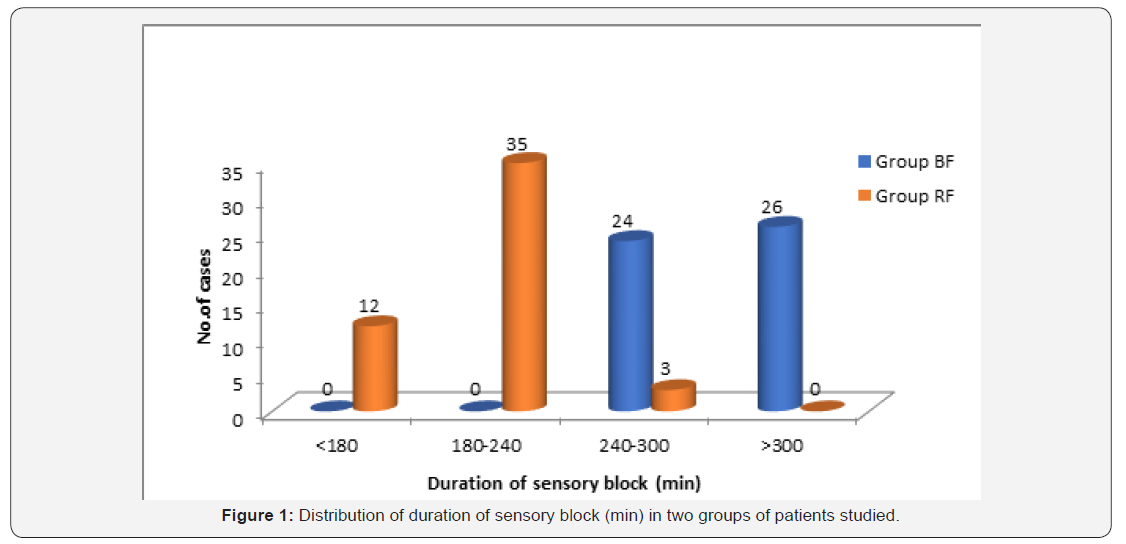
100 patients completed the study. 50 of them received 0.75% Isobaric Ropivacaine with Fentanyl 25mcg and 1ml 25% dextrose. 50 of them received 0.5% Hyperbaric Bupivacaine with Fentanyl 25mcg. Demographic data such as age, height, weight between two groups were comparable (Table 1). 84% of the patients in group BF and 80% of the patients in group RF achieved a sensory block of T6. 12% of patients in group BF and 16% of patients in group RF achieved a sensory block of upto T8. 4% of patients in both groups achieved a sensory block upto T10. These findings were clinically and statistically not significant. Complete motor blockade was observed in all patients in Group BF and 94% of patients in Group RF. The mean value for duration of sensory block was 309.82±31.09 minutes in Group BF and 203.08±29.36 minutes in Group RF with p value <0.001.
76% of patients in Group BF and 88% of patients in Group RF had a duration of motor block ranging from 120–180 minutes. The average duration of motor blockade was 180.50±50.84 minutes in Group BF and 158.82±24.55 minutes in Group RF with p value 0.008. There was no significant change in heart rate following subarachnoid block in both groups. The heart rates were comparable in both groups without any clinical or statistical significance (Figure 1). There was fall in systolic blood pressure following spinal Anaesthesia in both groups. The magnitude of fall was more in group BF compared to group RF. There was fall in diastolic blood pressure following spinal Anaesthesia in both groups. The magnitude of fall was similar in both groups and it was not clinically or statistically significant.
Hypotension was seen in 14% of patients in group BF and 4% of patients in Group RF. Bradycardia was seen in 10% of patients in Group BF and 4% of patients in Group RF. Shivering was seen in 4% of patients in group BF and not seen in group RF. Nausea and vomiting was seen in 2% of patients in group RF and not seen in Group BF. Pruritis was seen in 6% of patients in group BF and not seen in group RF.
Discussion
In our study the demographic details profile and the type of surgeries were kept identical in both groups to avoid variations in intraoperative and postoperative outcome of patients
The mean time for onset of sensory block in group RF was 1.75±0.25 minutes and in group BF was 1.63±0.69 minutes, with p value 0.201. The mean time for onset of motor blockade in group RF was 2.63±0.55 minutes and in group BF was 2.54±0.58 minutes with a p value of 0.417. Both the above values are statistically insignificant. There is no significant difference in onset of sensory and motor block. This observation was comparable to a study done by Koltka et al. [5], who compared equipotent doses of ropivacaine - fentanyl and bupivacaine – fentanyl for spinal Anaesthesia for lower abdominal surgery found no significant difference in onset of sensory and motor block. In another study done by Luck et al. [6], who compared hyperbaric solutions of racemic bupivacaine, levobupivacaine, and ropivacaine for spinal Anaesthesia, they concluded that there was no significant difference between the groups with regard to mean time to onset of sensory and motor block. Malinovsky et al. [7] found that onset of motor blockade was similar in the two groups receiving ropivacaine and bupivacaine intrathecally. Helena Kallio et al. [8] & Mc Namee et al. [9] also found similar time to onset of complete motor block.
80 % of patients in group BF and 84 % of patients in group RF achieved a sensory block up to T6 level. 16 % of patients in group BF and 12 % of patients in group RF achieved a sensory block up to T8, and 4% of patients in both groups achieved a level up to T10 which was comparable. In a study conducted by Lee et al. [10], who conducted a randomized double-blind comparison of ropivacaine-fentanyl and bupivacaine-fentanyl for spinal Anaesthesia noted both groups attained similar level of sensory block.
94 % of patients in group RF and 100 % of patients in group BF developed complete motor block. Chan Jong Chung et al. [11] observed complete motor block in all patients receiving either bupivacaine or ropivacaine for caesarean section. N Boztug [12] and others observed complete motor blockade in 88 % of patients receiving ropivacaine and 100 % patients receiving bupivacaine
Chung et al. [13], studied the effects of addition of intrathecal fentanyl to hyperbaric ropivacaine and concluded that duration of sensory block was prolonged when an opioid was added to the local anesthetic. According to a study by Marret et al. [14] in comparison to bupivacaine, ropivacaine produced a shorter duration of sensory block when given intrathecally. In our study duration of sensory blockade in group BF was 309.82±31.09 minutes which was longer than duration of sensory blockade in group RF which was 203.08±29.36 minutes which is statistically significant.
Koltka et al. [5], compared equipotent doses of isobaric ropivacaine and bupivacaine, both with fentanyl for the subarachnoid block and found that the RF group is associated with a shorter duration of motor block of 90 minutes versus 130 minutes in group BF. In our study, the duration of motor block in group RF was 158.82±24.55 minutes and was shorter than group BF with motor block of 180.50±50.84 minutes which is statistically insignificant.
In another study by Lee et al. [10], equal doses of intrathecal ropivacaine and bupivacaine with fentanyl were used for urology surgeries, and it was reported that ropivacaine provided shorter duration of motor block of 126 minutes compared to bupivacaine with 189 minutes. Boztug et al. [15] also stated that ropivacaine -fentanyl group had a shorter duration of motor block. Because of this differential blockade, ropivacaine with fentanyl is found to be favorable for surgeries which prevents morbidities related to bladder catheterization and early ambulation prevents deep vein thrombosis.
The hemodynamic parameters heart rate, systolic blood pressure, diastolic blood pressure was comparable between both the groups and no significant hemodynamic alteration was seen in the two groups. Group RF is haemodynamically more stable than group BF. This correlates with the study done by Mc Namee et al. [9]
In a study conducted by Sheetal et al. [16] incidence of hypotension was 3.3 % of patients in group RF, and 10 % of patients in group BF which correlates with our study. Hypotension occurred in 4 % of the cases in the RF group and 14 % of cases in group BF in our study and was easily managed by ephedrine boluses. 6% of patients in the BF group and none in the RF group experienced pruritis. This incidence is much lower compared to the incidence reported by Patra et al. [17] (46%) and Khanna & Singh [18] (20%) who also used fentanyl as adjuvant intrathecally
Conclusion
Intrathecal Ropivacaine -Fentanyl is similar to Bupivacaine - Fentanyl in onset of sensory and motor block, degree of motor block, height of sensory block. Ropivacaine - Fentanyl group is hemodynamically more stable than Bupivacaine - Fentanyl group. But there is a shorter duration of sensory and motor block with Ropivacaine compared to Bupivacaine. Hence, Ropivacaine can be used successfully as an alternative to Bupivacaine for surgeries of lower abdomen and lower limb where early ambulation, decreased hospital stays, and decreased morbidity are appreciated.
References
- Feldman HS, Arthur GR, Pitkanen M, Hurley R, Doucette AM, et al. (1991) Treatment of acute systemic toxicity after the rapid intravenous injection of ropivacaine, bupivacaine and lidocaine in the conscious dog. Anesth Analg 73(4): 373-384.
- Cpogna G, Cellono D, Fusco P, Lyons G, Columb M (1999) Relative potencies of bupivacaine and ropivacaine for analgesia in labor. Br J Anaesth 82(3): 371-373.
- Yamashita A, Matsumoto M, Matsumoto S, Itoh M, Kawai K, et al. (2003) A comparison of the neurotoxic effects on the spinal cord of tetracaine, lidocaine, bupivacaine, and ropivacaine administered intrathecally in rabbits. Anesth Analg 97(2): 512-519.
- Brunton LL, Lazou JS, Parker LL (2007) Goodman & Gilman's. The Pharmacological Basis of Therapeutics. 11th Edition, McGraw Hill Medical Publications, USA, pp. 571-582.
- Koltka K, Uludag E, Senturk M, Yavru A, Karadeniz M, et al. (2009) Comparison of equipotent doses of ropivacaine-fentanyl and bupivacaine-fentanyl in spinal anaesthesia for lower abdominal surgery. Anaesth Intensive Care 37(6): 923-928.
- Luck JF, Fettes PD, Wildsmith JA (2008) Spinal anaesthesia for elective surgery: a comparison of hyperbaric solutions of racemic bupivacaine, levobupivacaine and ropivacaine. Br J Anaesth 101(5): 705-710.
- Malinovsky, F Charles, Ottmar Kick, Lepage JY, Malinge M, et al. (2000) Intrathecal Anaesthesia: ropivacaine versus bupivacaine. Anesth analg 91(6): 1457-1460.
- Kallio H, Snäll EV, Kero MP, Rosenberg PH (2004) Comparision of intrathecal plain solutions containing ropivacaine 20mg or 15 mg versus bupivacaine 10mg. Anesth analg 99(3): 713-717.
- McNamee DA, McClelland AM, Scott S, Milligan KR, Westman L, et al. (2002) comparison of plain ropivacaine 5mg/ml with bupivacaine 5mg/ml for orthopaedic surgery. Br J Anaesth 89(5): 702-706.
- Lee YY, Ngan Kee WD, Muchhal K, Chan CK (2005) Randomized double-blind comparison of ropivacaine-fentanyl and bupivacaine-fentanyl for spinal anaesthesia for urological surgery. Acta Anaesthesiol Scand 49(10): 1477-1482.
- Chan Jong Chung, So Ron Choi, Kwang Hwan Yeo, Han Suk Park, Soo II Lee, et al. (2001) Hyperbaric bupivacaine. Anesthesia and analgesia. 93: 157-161.
- Boztuğ N1, Bigat Z, Karsli B, Saykal N, Ertok E (2006) Comparison of ropivacaine and bupivacaine for intrathecal anaesthesia during outpatient arthroscopic surgery. J Clin Anesth 18(7): 521-525.
- Chung CJ, Yun SH, Hwang GB, Park JS, Chin YJ (2002) Intrathecal fentanyl added to hyperbaric ropivacaine for caesarean delivery. Reg Anesth Pain Med 27(6): 600-603.
- Marret E, Thevenin A, Gentili M, Bonnet F (2011) Comparison of intrathecal bupivacaine and ropivacaine with different doses of sufentanil. Acta Anaesthesiol Scand 55(6): 670-676.
- Boztuğ N, Bigat Z, Ertok E, Erman M (2005) Intrathecal ropivacaine versus ropivacaine plus fentanyl for out-patient arthroscopic knee surgery. J Int Med Res 33(4): 365-371.
- Jagtap S, Chhabra A, Dawoodi S, Jain A (2014) Comparison of intrathecal ropivacaine-fentanyl and bupivacaine-fentanyl for major lower limb orthopaedic surgery: A randomised double-blind study. Indian J Anaesth 58(4): 442-446.
- Patra P, Kapoor MC, Nair TG (2005) Spinal Anaesthesia with low dose bupivacaine and fentanyl for endoscopic urological surgeries. J Anaesth Clin Pharmacol 21(2): 147-154.
- Kanna MS, Singh IK (2002) Comparative evaluation of bupivacaine plain versus bupivacaine with fentanyl in spinal anaesthesia in geriatric patients. Indian J Anaesth 46(3): 199-203.






























