Estimation of Minimum Effective Volume of Ropivacaine 0.5% in Ultrasound Guided Supraclavicular Brachial Plexus Nerve Block: A Prospective Clinical Trial
Sangwan Pushpender1, Mohammed Sadik1, Chouhan Dilip Singh1, Prateek Prateek1*, Srinivasan Bharath1, Malav Khushboo1 and Ratnawat Anil Kumar1
1Department of Anaesthesiology, Dr. Sampurnan and Medical College, India
2Department of Anaesthesiology, All India Institute of Medical Sciences, India
Submission: February 12, 2018; Published: February 23, 2018
*Corresponding author: Prateek Prateek, Department of Anaesthesiology, Dr. Sampurnan and Medical College, H.no. 888a, ward 27, Azad Nagar, Thanesar, Kurukshetra Haryana, India, Tel: 9462978499; Email: neopatricks@gmail.com
How to cite this article: Sangwan Pushpender, Mohammed Sadik, Chouhan Dilip Singh, Prateek Prateek, Srinivasan Bharath, et al. Estimation of Minimum Effective Volume of Ropivacaine 0.5% in Ultrasound Guided Supraclavicular Brachial Plexus Nerve Block: A Prospective Clinical Trial. J Anest & Inten Care Med. 2018; 5(5) : 555671.DOI10.19080/JAICM.2018.05.555671
Abstract
Background: The introduction of ultrasound (US) in the field of regional anaesthesia (RA) has markedly reduced the volume of local anaesthetic (LA) used. But, still there is insufficient data which clearly defines minimum effective volume (MEV) of LA used in US guided block. Thus, we intended to determine the MEV of ropivacaine 0.5% in US guided supraclavicular brachial plexus block (SCBPB) in our study.
Methods: Step-up/step-down method based on the outcome of the preceding block was used to determine the anaesthetic volume. A successful or failed block resulted in a 1 mL decrease or increase in volume, respectively. The study was stopped, once the secondary stopping rule of 10 consecutive successful SCBPB was effectively achieved with 15 mL of 0.5% ropivacaine. Respiration and analgesia were also assessed perioperatively.
Results: As per our secondary stopping rule, the study was stopped at 15mL of 0.5% ropivacaine (overall success rate 93.1%; 95% CI after 2 noted failures, 83.29%-102.91%). This protocol was met upon enrolment of 29 consecutive patients. Duration of analgesia did not differ between patients with successful blocks at 15mL and those who received >15mL for successful blocks (7.10 ± 0.74 and 7.95 ± 2.22 hours, respectively; P= 0.25).
Conclusion: Our data suggests that successful surgical anaesthesia with US-guided SCBPB can be accomplished with as little as 15 mL of 0. 5% ropivacaine without clinically apparent deterioration in block onset, duration and respiration, further favours and trying to establish the new era of low volume in RA.
Keywords: Ultrasound guided; Supraclavicular brachial plexus block; Local anaesthetic; Ropivacaine; Step-up/step down method; Minimum Effective volume
Introduction
In recent time, rising demand for regional anaesthesia (RA) from patients as well as from surgeons, matches the growing realization that RA can offer superior pain management and perhaps improved patient outcome than general anaesthesia (GA), making it an ideal approach for ambulatory and cost-effective surgery [1,2]. Irrespective of various techniques used, still most anaesthesiologists believe in using higher volume of local anaesthetic (LA) to achieve satisfactory block [3,4]. Introduction of Ultrasound (US) guidance has revolutionized the world of anaesthesia as it facilitates the reduction of volume. Various studies [5] have been performed to estimate minimum effective volume (MEV) of local anaesthetic required for successful block of brachial plexus using different approach (interscelene and axillary), but the MEV in supraclavicular brachial plexus block (SCPBP) is still unspecified. Hence, we performed this study to investigate a clinically relevant MEV of ropivacaine 0.5%, required for successful SCBPB. We hypothesized that SCBPB can be accomplished with a lower volume of LA (<30 mL) than commonly recommended.
Method
This protocol was approved by our institution's research ethics committee (Ref: 46/16) and registered at ctri.nic.in. After written informed patient consent, ASA physical status I or II patients, aged 18 to 60 years and scheduled for forearm & hand surgery under SCBPB, were prospectively enrolled. Patients, who presented with contraindications to this block or were pregnant, excluded from study. On the basis of our institutional clinical practice, we started our study with 30 mL of ropivacaine 0.5% (NEON Lab.) as initial volume. Using a previously validated Dixon's step-up/step-down method [6], volume of LA for block in consecutive patient was decided by the outcome of previous one. In state of failed block, the injection volume was augmented by 1mL. On the contrary, for block success, the volume was reduced by 1 mL. All blocks were performed in the induction room by a single anaesthesiologist, experienced in US-guided peripheral nerve blocks (PNBs). Intravenous (IV) access was secured in the nonoperative arm, and standard monitoring was applied. All patients were premedicated with midazolam 0.03mg/kg IV. Needle placement and injection of LA was guided by ultrasound (M turbo 11 mm broadband linear array, 6-14 MHz Sonosite Bothell, Washington, USA).
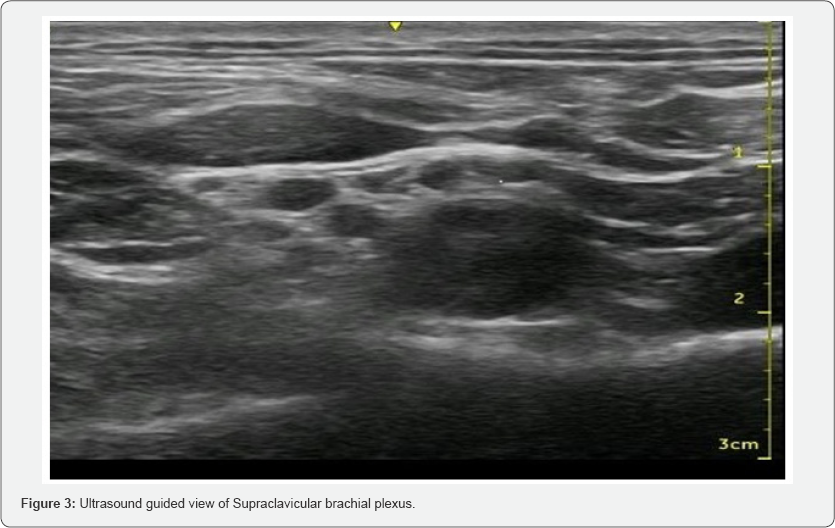
After skin sterilization and anaesthesia, probe covered with sterile cover, placed in the supraclavicular fossa in a coronal-oblique plane above the clavicle, with the patient lying supine and head turned 45° to the contralateral side. The US probe made visualize brachial plexus and subclavian artery in the transverse sectional view (i.e. at approximately 90°) as a cluster of hypoechoic nodules often seen posterolateral to the round pulsating hypoechoic subclavian artery, superior to the hyperechoic first rib. After skin infiltration with local anaesthetic, a 22- gauge 50 mm insulated block needle (Stimuplex; B. Braun Medical, Bethlehem, Pa) was placed on the lateral part of the probe and advanced along with the long axis of the probe under the ultrasound beam. Once the needle reached the brachial plexus cluster, being careful to avoid any sensitive structures, the needle was slowly advanced towards the junctional region of plexus and subclavian artery. Once, careful movement of the needle caused movement on the plexus, drug was injected with single injection method and confirmed as separation of plexus from artery. Special attention paid to look for signs of inadvertent intraneural injection e.g. severe pain during injection and high resistance to injection. Onset of sensory and motor block, duration of surgical procedure, and time for first analgesic requirement, were recorded.
Block Assessment
An examiner blinded to the volume of injectate, had evaluated the presence of motor and sensory blockade in the territory of radial, median and ulnar nerve innervations zones. Assessment of block in each case was performed regularly at 5-minute intervals up to 30 minutes after completion of the last injection. Contralateral limb sensory and motor functions were assessed for comparison purpose in each patient. Sensory block was evaluated by pin prick method with a 23 gauge needle in the regions innervated by median, ulnar and radial nerve and graded as [0 = sharp pin felt; 1 = analgesia (dull sensation felt) and 3 = anaesthesia (no sensation felt)]. Onset of sensory block was defined as time interval between completion of injection and achievement of sensory score of 2 in territories supplied by radial, median and ulnar nerve.
Motor block was evaluated using modified Bromage score [7] and graded as (0: Normal motor function with full flexion and extension of elbow, wrist and fingers; 1: Decreased motor strength with ability to move the fingers only; 2: Complete motor block with inability to move the fingers). Onset of motor block was defined as the time between drug injection and complete loss of motor function in forearm and hand muscle groups. As only forearm and hand surgeries were included in this study. Therefore, assessment of sensory & motor blockade of musculocutaneous nerve was not considered. Overall, the ultimate maximal composite score (motor + sensory) was decided as 12 points. If a minimal composite score of 10 points had achieved, the block was considered successful, provided that sensory block score will be equal or superior to 5 of 6 points. Essential vital parameters were recorded at 5-min intervals. For continuous neurological evaluation (clinical signs and symptoms of LA toxicity), no sedative drugs were administered intraoperatively. During first hour after plexus block, we looked for clinical signs of blockade of phrenic or recurrent laryngeal nerve like chest discomfort (dyspnoea) or hoarseness of voice complaint by patient. Inj. Tramadol 100 mg IV was administered on patient demand in postoperative period. Duration of analgesia was defined as time interval between completion of local anaesthetic injection and administration of tramadol IV in the postoperative period. A chest radiograph was performed within 6 hours of block performance to exclude pneumothorax and elevation of the diaphragm. All patients were observed until complete recovery of sensation.
Study Stopping Rule & Sample Size
Two study-stopping rules were used. First, the minimum effective anaesthetic volume (MEAV50) of 0.5% ropivacaine was defined as the midpoint of pairs of volumes from consecutive cases in which a failed block (inadequate effect within 30 minutes) is followed by a successful one. On the basis of earlier non probability sequential volumes used in studies with similar binary outcomes,[8] we estimated that a minimum of 10 independent negative- positive up and down deflections would be required to compute MEAV50. It was agreed by consensus that reducing the dose below 15mL was not of clinical importance. Hence, the study was stopped on attaining of 10 consecutive successful SCBPB using 15mL of ropivacaine 0.5%, which was our secondary stopping rule.
Statistical Analysis
Summary data were calculated using the SPSS IBM software version 21 (IBM SPSS advanced statistics; Chicago), compiled in the Microsoft Excel sheet (a spreadsheet application by Microsoft Corporation) and represented as median (range) or mean (SD) for all quantitative variables. The frequency of all variables was displayed in charts and tables. Unpaired student t test was applied for comparing quantitative data (mean) and Chi Square test was applied for qualitative data. The test was considered significant if p<0.05 at 95% confidence interval.
Results
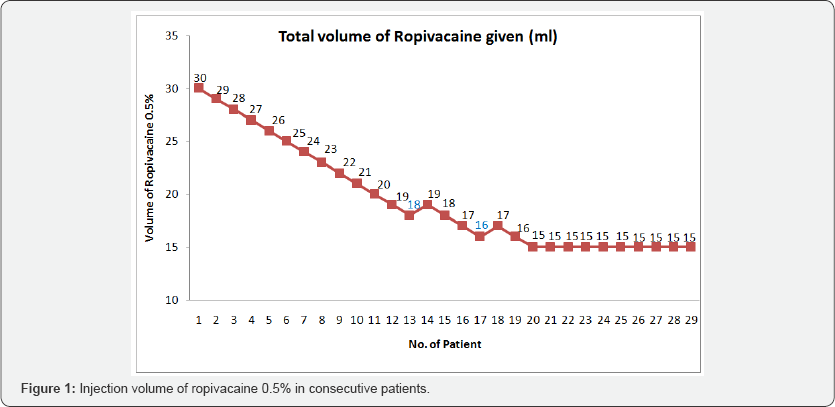
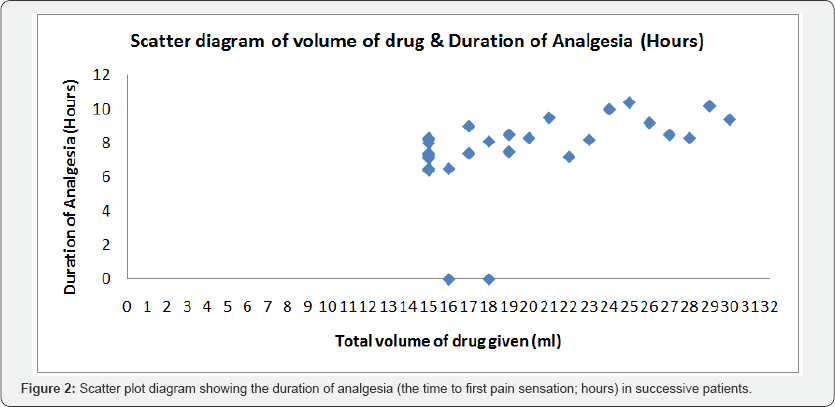
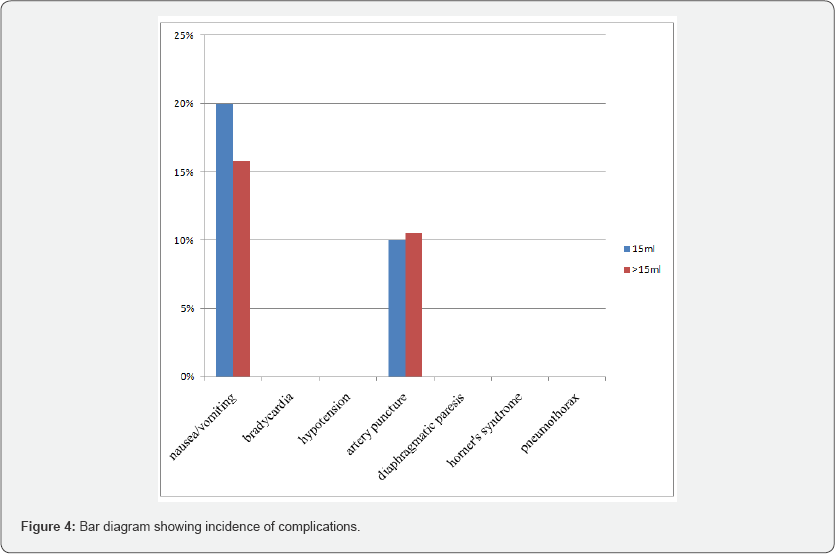
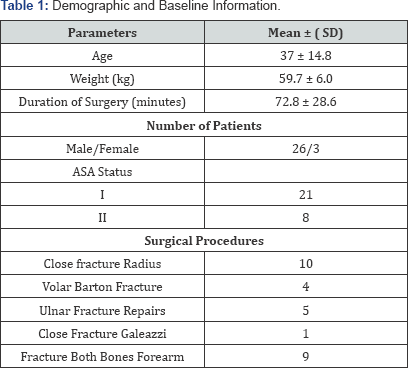
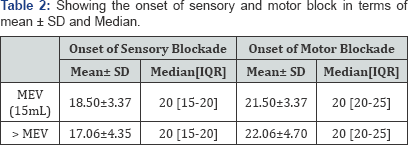
Patient demographics are presented in Table 1. The protocol of performing 10 consecutive successful blocks with 15 mL of LA was met upon enrolment of 29 consecutive patients. There was no significant variation in the hemodynamic variables (Systolic BP, Diastolic BP, Mean BP and SpO2) from baseline during observation period. Overall success rate was 93.1%; 95% CI after 2 noted failures: 83.29%-102.91%. As we achieved secondary stopping rule, thus MEAV50 could not be calculated (Figure 1). For the group as a whole, the median (range) sensory block onset time was 20 (15-20) minutes, the median (range) motor block onset was also 20 (20-25) minutes (Table 2). The median (range) block duration was 8.1 (6.4-10.4) hours while the mean duration of analgesia was 7.6 ± 1.18 hours. Duration of analgesic effect was not related with volume of LA injected (P=0.25). Block duration did not differ between patients with successful blocks at 15mL and those who required >15 mL for successful block (7.10 ± 0.74 and 7.95 ± 2.22 hours, respectively; P = 0.25) as shown in Figure 2. Incidence of adverse effects were not significantly different between patients with successful blocks at 15mL and those who required >15 mL for successful block (Figure 3 & 4).
Discussion
One of the most exciting recent advances in technology relating to RA is the introduction of anatomically-based ultrasound imaging. It certainly helps to inject the drug at exact location as well as contributes to reduce the volume of LA. But still, there are no convincing data available, which clearly defines the MEV, can be used to successfully perform a block. Thus, we intended to find out a clinically relevant MEV for SCBPB. We started our study with conventional 30mL volume of LA. We monitored hemodynamic parameters like systolic BP, diastolic BP, mean arterial pressure and pulse rate, as well as Sp02 level in every patient and we did not find any significant variations from preoperative values (Preblock) during continuous monitoring at five minute intervals for first 30 minutes after block performance. Shobhana Gupta et al. [9] and UshaBafna et al. [10] also had similar findings in their respective studies that ropivacaine 0.5% or 0.75% concentration does not lead to any significant hemodynamic changes.
There are various techniques attempted by anaesthesiologists worldwide to precisely inject the drug at appropriate location. Some authors recommended that a single bolus injection at the junction where the subclavian artery meets the first rib (corner pocket technique) results in more trustworthy blockade of the inferior divisions of the brachial plexus. However, Duggan et al. [11] & Tran et al. [12] could not reduce the volume of LA despite using this same technique. Therefore, we assumed that the corner pocket technique cannot reduce the drug volume effectively. As a result, this technique was not used in our study. Before commencement of this study, we reviewed several articles related to US-guided nerve blocks [13,14-19]. Among them, we found an idea in a study by Bigeleisen et al. [15]. They achieved a 100% success rate with 20 mL of 1% lidocaine in US-guided SCBPB. They injected LA around the deeper parts of the brachial plexus. Though drug was injected intraneurally, which resulted in neurological complications [21,21]. Fortunately, we performed all our blocks without any neurological complication in our study. Jae Gyok Song et al. [22] and Perlas et al. [23] found a significant reduction in incidences of pneumothorax, horner syndrome, unintended vascular punctures, and transient sensory deficits during US guided supraclavicular blocks. We also finished our whole study without any incidence of these complications, owing to clear visibility and precise drug delivery with USG.
Nevertheless, previous studies have reported only 35-60% incidence of ipsilateral diaphragm paresis after SCBPB using conventional volumes of Las [23-26] as compared to ISBPB, which has almost 100% chances of ipsilateral diaphragm paresis. Even then, we were interested to observe respiratory consequences in our patients. Due to limited resources in our institution to perform pulmonary function test (PFT) and limited clinical skills to monitor diaphragm movements by USG, we could monitor, only the SPO2 values in all patients at different intervals (pre block and post block at 5 minutes interval). All the patients had more than 97% SPO2 at room air during all time intervals and didn't resulted in any significant difference (P>0.05). Clinically, no patient among 29 complained of chest discomfort and showed hemi-diaphragmatic paresis on the post-operative chest X-ray (3 hours post block). But these clinical observations alone are not sufficient to support our results. Therefore, we need some more studies for proper evaluation of respiratory changes with help of modern diagnostic tools.
Meanwhile, we found that needle advancement was troublesome in few patients. There seemed to be some unseen obstructions (possibly, because of different density of connective tissue individually) which prevented the needle advancement even if the needle was found in free space between nerves on US image. The LA did not spread freely between divisions in these cases. We could perform only 27 successful blocks out of total 29 patients. Perhaps, our two failed cases fell in this situation. Difference in block quality between high volume and low volume was also assessed. Surprisingly, we could not find any added advantage of using higher volume as compared to lower volume. The time spent for achieving adequate motor block (21.5 min Vs 22.06 min) as well as sensory block (18.5min Vs 17.06min) did not vary significantly between both groups (15mL Vs>15mL). There was also no dissimilarity in pain perception and regain of motor power during postoperative period. Nevertheless, in our sample of patients, average block duration was approx. 1 hour longer for those who received >15mL of LA. It should be noted, however, that the 95% CI is wide, thus no significant statement regarding any variation in the block duration between the patients who received different volumes of LA, could be prepared.
Despite all achievement, this study has several limitations. First, step-up/step-down [6] is designed to calculate the MEV with only a limited number. As a result, some authors suggested to conduct these studies with >20 patients for accuracy [27,28]. Thus, we recruited 29 patients in our study. However, we still think that it has an inadequacy even though we included more patients than recommended. Second, all blocks were performed by a skilled operator. Therefore, this result cannot be applied to general anaesthesiologists. Third, MEV50 could not be calculated as the second study stopping point was reached so more research are required in this field to search the possibility of adequate block with the volume less than 15 ml. Fourth, the follow-up for neurological complications was inadequate. Only 2 to 3 weeks follow-up was maintained by surgeons in the outpatient department. Consequently, late neurological complications cannot be excluded.
Conclusion
Under the settings of our study, successful surgical anaesthesia for forearm & hand surgeries was obtained in 27 out of 29 patients with as little as 15mL of 0.5% ropivacaine. The small number of patients included (n=29), may limit the external validity of the data. Nevertheless, the intended endpoint of achieving successful block with 15mL in 10 consecutive patients was reached. Therefore stopping the study was considered appropriate. Thus we conclude that successful surgical anaesthesia with US-guided SCBPB could be accomplished with as little as 15 mL of 0.5% ropivacaine without clinically apparent deterioration in block onset, duration and respiration, further favours and trying to establish the new era of low volume in RA.
Acknowledgements
None.
Conflict of Interest
None.
References
- Nielsen KC, Steele SM (2002) Outcome after regional anaesthesia in the ambulatory setting--is it really worth it? Best Pract Res Clin Anaesthesiol 16(2): 145-157.
- Broking K, Waurick R (2006) How to teach regional anesthesia. Curr Opin Anaesthesiol 19(5): 526-530.
- Koscielniak Nielsen ZJ, Stens Pedersen HL, Lippert FK(1997) Readiness for surgery after axillary block: single or multiple injection techniques. Eur J Anaesthesiology 14(2): 164-171.
- Borgeat A, Dullenkopf A, Ekatodramis G, Nagy L (2003) Evaluation of the lateral modified approach for continuous interscalene block after shoulder surgery. Anesthesiology 99( 2): 436-442.
- Neal JM, Brull R, Chan VW, Grant SA, Horn JL, et al. (2010) The ASRA evidence-based medicine assessment of ultrasound-guided regional anaesthesia and pain medicine: Executive summary. Reg Anesth Pain Med 35(2 Suppl): S1-S9.
- Dixon WJ (1965) The up-and-down method for small samples. J Am Stat Assoc 60: 967-978.
- Sarkar DJ, Khurana G, A Chaudhary, J P Sharma (2010) A comparative study on the effects of adding fentanyl and buprenorphine to local anaesthetics in brachial plexus block. Journal of Clinical and Diagnostic Research 4(6): 3337-3343.
- O Donnell BD, Iohom G (2009) An estimation of the minimum effective anesthetic volume of 2% lidocaine in ultrasound-guided axillary brachial plexus block. Anesthesiology 111(1): 25-29.
- Gupta S, Gadani HN, Thippeswamy H G (2015) A comparative study between ropivacaine 30 ml (0.75%) and ropivacaine 30 ml (0.75%) with clonidine 150 ^g as an adjuvant in brachial plexus block through supraclavicular approach. Sudan Med Monit 10(1): 11-16.
- Bafna U, Yadav N, Khandelwal M, Mistry T, Chatterjee C S, et al. (2015) Comparison of 0.5% ropivacaine alone and in combination with clonidine in supraclavicular brachial plexus block . Indian J Pain 29(1): 41-45.
- Duggan E, El Beheiry H, PerlasAnahi, Lupu M, Nuica A, et al. (2009) Minimum Effective Volume of Local Anesthetic for Ultrasound-Guided Supraclavicular Brachial Plexus Block: Reg Anesth Pain Med 34(3): 215-218.
- Tran DQ, Dugani S, Correa JA, Dyachenko A, Alsenosy N, et al. (2011) Minimum effective volume of lidocaine for ultrasound-guided supraclavicular block. Reg Anesth Pain Med 36(5): 466-469.
- Kapral S, Krafft P, Eibenberger K (1994) Ultrasound guided supraclavicular approach for regional anesthesia of the brachial plexus. Anesth Analg 78(3): 507-513.
- Perlas A, Lobo G, Lo N, Brull R, Chan VW, et al. (2009) Ultrasound- guided supraclavicular block: outcome of 510 consecutive cases. Reg Anesth Pain Med 34(2): 171-176.
- Bigeleisen PE, Moayeri N, Groen GJ (2009) Extraneural versus intraneural stimulation thresholds during ultrasound-guided supraclavicular block. Anesthesiology 110(6): 1235-1243.
- Williams SR, Chouinard P, Arcand G, Harris P, Ruel M, et al. (2003) Ultrasound guidance speeds execution and improves the qualilty of supraclavicular block. Anesth Analg 97(5): 1518-1523.
- Chan VW, Perlas A, Raw R, Odukoya O (2003) Ultrasound-guided supraclavicular brachial plexus block. Anesth Analg 97: 1514-1517.
- Arcand G, William SR, Chouinard P, Boudreault D, Harris P, et al. (2005) Ultrasound-guided infraclavicular block versus supraclavicular block. Anesth Analg 101(3): 886-890.
- Subramanyam R, Vaishnav V, Chan VW, Brown Shreves D, Brull R (2011) Lateral versus medial needle approach for ultrasound-guided supraclavicular block: a randomized controlled trial. Reg Anesth Pain Med 36(4): 387-392.
- Selander D, Edshage S, Wolff T (1979) Paresthesiae or no paresthesiae? Nerve lesions after axilary blocks. Acta Anaesthesiol Scand 23(1): 2733.
- Hadzic A, Diberovic F, Shah S, Kulenovic A, Kapur E, et al. (2004) Combination of intraneural injection and high injection pressure leads to fascicular injury and neurologic deficits in dogs. Reg Anesth Pain Med 29(5): 417-423.
- Song JG, Jeon DG, Kang BJ, Park KK (2013) Minimum effective volume of mepivacaine for ultrasound-guided supraclavicular block. Korean J Anesthesiol 65(1): 37-41.
- Farrar MD, Scheybani M, Nolte H (1981) Upper extremity block, effectiveness and complications. Reg Anesth 6: 133-134.
- Neal JM, Moore JM, Kopacz DJ, Liu SS, Kramer DJ, et al. (1998) Quantitative analysis of respiratory, motor and sensory function after supraclavicular block. Anesth Analg 86:1239-1244.
- Pham Dang C, Gunst JP, Gouin F, Poirier P, Touchais S, et al. (1997) A novel approach to supraclavicular brahchial plexus block. Anesth Analg 85(1): 111-116.
- Cornish PB, Leaper CJ, Nelson G, Anstis F, McQuillan C, et al. (2007) Avoidance of phrenic nerve paresis during continuous supraclavicular regional anaesthesia. Anaesthesia 62(4): 354-358.
- Pace NL, Stylianou MP (2007) Advances in and limitations of up-and- down methodology. Anesthesiology 107(1): 144-152.
- Fisher D (2007) What if half of your patients moved (or remembered or did something else bad) at incision? Anesthesiology 107: 1-2.






























