Prospective Study of Ventilator Associated Pneumonia Incidence, Risk Factor, Outcome and its Prevention
Amartej Singh Sohal1, Baljit Singh Bajwa1*, Sharanjit Singh1, Iqbal Singh1 and Vaneet Mahajan2
1Department of Anaesthesia, Punjab Institute of Medical Sciences, India
2Department of Pulmonary Medicines, Punjab Institute of Medical Sciences, India
Submission: January 27, 2018;Published: February 19, 2018
*Corresponding author: Baljit Singh Bajwa, Department Of Anaesthesia, Punjab Institute of Medical Sciences, Jalandhar, India, Tel: 987270673; Email: baljitbajwa7@gmail.com
How to cite this article: Amartej S S, Baljit S B, Sharanjit S, Iqbal S, Vaneet M. Prospective Study of Ventilator Associated Pneumonia Incidence, Risk Factor, Outcome and its Prevention. J Anest & Inten Care Med. 2018; 5(4) : 555666. DOI:10.19080/JAICM.2018.05.555666
Abstract
VAP is a common occurrence in critical patients which is due to nosecomial infections.
Aim and Objective: Prospective study was conducted in patients admited in ICU to investigate the incidence, factors responsible and prevention of VAP in one year period in mechanically ventilated 100 patients requiring ventilation more than 24 hours. Based on accurate physiology and cronic heath variation (Apache Score) and anteral nasogastric feeding (AOR) duration of mechanical ventilation was more in patients who had VAP.
Method: Study was conducted over a period of one year from December 2016 to January 2018 in ICU in our Institution after approval of Ethical Commettee. 100 patients of both sexs on mechanical ventilation were selected in random. Inclusion creteria was based on age more than 18 year and required mechanical ventilation more than 48 hours. Patients with pneumonia and acute respiratory syndrome at the time of admission were excluded from the study .
Results: The study comprised of 100 patients of cases of sepsis, neurological disorders and poisioning. Mean age of patients 45-65 years (35 yrs) with prodominent male population. Of 100 patients 39 developed VAP during ICU hospitalisation. Mean duration of mechanical ventilation was 10days in non-VAP group and 20 days in VAP Group. Who required prolonged ventilatory support (more than 15 days) had higher incidence of VAP (P-value < 0.001) which was significant. Another group of patients in spine position and stupourous and comotosed patients had high incidence of VAP risk and significant statistically (P-value < 0.003 and 0.002 respectively). PaO2 / FiO2 ratio was analysed in VAP patients and found to be < 240 mm Hg in 80𐀥 cases. In 20% cases it was > 240 mm Hg. VAP in early Onset was 30% while it was 80% in late onset VAP. Mortality was 3% in early onset and 16% in late onset VAP (p>0.05). Organisum prevalance was Pseudomonas (40%) Kelebseilla (18%) and MRSA E Coli Acnobactor MSSA and S Pneumoniae.
Conclusion: Intervention during mechanical ventilation may be the cause of VAP. Risk factors should be identified and due prevention should be done to reduce the incidence of VAP. Decreasing ratio of partial pressure to inspired O2 fraction was the earliest sign of VAP. Large number of VAP cases in our institution was due to pseudomonas micro organism. Early onset and late onset VAP were also differenciated and more mortality was found in late onset cases. VAP zero module should be adopted to reduce VAP cases and ultimate impact on stay and cost and mortality in ICU.
Introduction
Ventilator associated pneumonia is defined as pneumonia following endotracheal intubation in mechanically ventilated patients admitted in ICU after 48 hours with new infiltrate, sign of infection, changing colour and consistency of sputum detecting causative agent microbiologically [1] which is responsible for half of the hospital acquired pneumonia [2]. Most common cause of nosocomial infection in ICU is VAP. Risk is high in first four days of mechanical ventilation which declines by 2% per day in the next five to ten days and thereafter 1% per day. Early onset VAP develops in first four days and senstive to antibiotics. Late onset VAP appears after four days which is often multidrug resistant. It is responsible for increased complications and health costs. Other risk factors are male sex, trauma and underlying disease severity [3,4]. Presence of endotracheal tube which results in interference of natural defence mechanism like cough reflex of glottis and larynx against microaspiration around cuff of tube [5,6], virulence of bacteria and immunity of host are determinents of VAP. Bacteria can gain direct access to lower respiratory tract resulting from micro aspiration, development of biofilm laden bacteria and fungi within the endotracheal tube, pooling of secretions around cuff and impairment of mucociliary clearance within respiratory airways [7,8].
Pathogenic collection can occur in surrounding anatomic areas such as stomach, sinuses, nasopharynx, oropharynx replacing normal flora with more virulent strains. Purulant secretions are continously pushed forward with positive pressure exerted with ventilator. Reintubation after extubation also increases VAP rate. Other factors are underlying disease, surgery, antibiotics use and decreased immunity [9,10]. Organisms causing VAP depend upon duration of mechanical ventilation. In early onset VAP, commonly found bacteria are streptococcus pneumonia, haemophillous influenzae, methellin sensitive staphyllococcus arues, gram negative bacilli, E colli, klebsiella pneumonia, enterobacter species, proteus species, serrata marcescens. Late onset VAP is usually resistent bacterial infection due to methellin S .aureus, acinobacter pseudomonas aerogenosa extended beta lactamase producing bacteria streptococcus viridans, coryne bacterium, coagulase -negative staphylococcus ansneiseria species. Patients referred from outside, recieving antibiotics in last 3 days and on haemodialysis are more prone to VAP [11]. Risk of mortality due to VAP in presence of medical ilness decreased to 9% to 13% from 30% by taking precentive measures as reported by different authors [11-13].
Aims and Objectives
To evaluate incidence of Ventilator Associated Pneumonia (VAP) in patients requiring mechanical ventilation more than 48 hours and effect of duration of ventilation, associated risk factors like enteral feeding, repeated suctioning of endotracheal tube and positioning of patient on outcome of VAP. Measures to be taken to reduce the incidence of VAP viz functional and pharmcological.
Material and Methods
This study comprised of 100 patients who require mechanical ventilation for more than 48 hours were taken after valid consent by the patient or relative as appropriate of both gender of age group above 18 years. Random selection of patients on ventilator was made by intensivist not taking part in the study. Study was conducted in intensive care unit PIMS Jalandhar after due approval of Ethical Committee. Patients already having pneumonia or acute respiratory syndrome or developed pneumonia before 48 hours were excluded from the study. Questionare was prepared as per proforma mentioning name, age, sex, date of admission, date of start of mechanical ventilation, patients of VAP were divided into early onset VAP (<96 hours), late onset VAP (> 96 hours) group on the basis of duration of mechanical ventilation. General and systemic examination, complete blood count, arterial blood gas analysis Ecg, X-ray chest, culture/senstivity of tracheal secretions on appearence of fever will be done. Data as per tables will be collected, analysed by ANOVA and chi square test and p value < 0.05 calculated .
Diagnostic Criteria
a. New or progressive radiographic infiltrate
b. Temperture more than 380C
c. Leucocytosis WBC > 12000/ mm or leucopenia < 4000/m
d. Presence of purulent secretion or endotracheal aspirate for microscpic presence of macrophages and neutrophiles in aspirate are considered for culture and sensitivity to confirm. lower respiratory infection (Table 1 & 2)
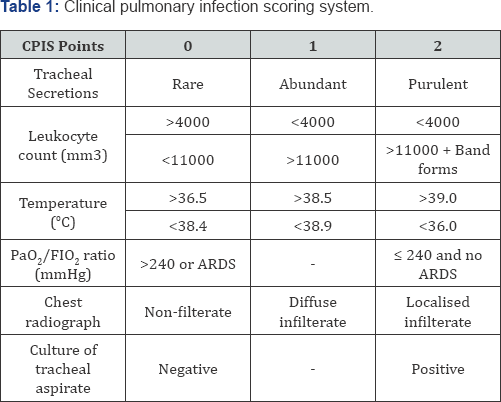
CPIS: Clinical Pulmonary Infection Scoring

P>0.05 not significant VAP
This study was hypothsised to determine the above mentioned facts and their role in incidence of VAP.
Results
The study comprised of 100 patients of cases of septic, neurological disorders and poisioning sepsis. Mean age of patients 45-65 years (35 yrs) with prodominent male population. Of 100 patients 39 developed VAP during ICU hospitalisation . Mean duration of mechanical ventilation was 10days in non-VAP group and 20 days in VAP Group. Who required prolonged ventilatory support (more than 15 days) had higher incidence of VAP (P-value < 0.001) which was significant. Another group of patients in supine position and stupourous and comotosed patients had high incidence of VAP risk and significant statistically (P-value < 0.003 and 0.002 respectively). PaO2 / FiO2 ratio was analysed in VAP patients and found to be < 240 mm Hg in 80% cases. In 20% cases it was > 240 mm Hg. VAP in early Onset was 30% while it was 80% in late onset VAP. Mortality was 3% in early onset and 16% in late onset VAP (p>0.05). Organisum prevalance was Pseudomonas (40%) Kelebseilla (18%) and MRSA E Coli Acnobactor MSSA and S Pneumoniae.
Discussion
In our study of VAP, Male predominance of VAP cases was present but was not significant though VAP incidence was high in males as compared to females population (P = 0.2). Mean age group was 35 years which may be due to addiction drug abuse and poisioning cases were more in this study. The incidence of VAP was 39% of which early onset as compared to the other studies [9,10] as low as 10-30%. High percentage in our study may be due to patient staff ratio 1-4 and required ratio is 1:1. Another reason may be due more cases of drug abuse and organophorous poisioning and prolonged mechanical ventilation (P-value <0.05) (Table 3 & 4). Mean duration of ventilation in our study was 12 days in comparision to other study (10days) which was an important factors of VAP [11,12]. Mean duration of Ventilation can effectively be reduced by proper weaning off. Spontaneous breathing trial is more effective than Intermitant mandatory Ventilation (IMV) on once daily basis to reconditioning of respiratory muscles of patients on Mechanical Ventilation [13]. Intermittent mandatory ventilation causes more respiratory fatigue and sponteneous breathing trial should be given rather than intermittent mandatory ventilation.
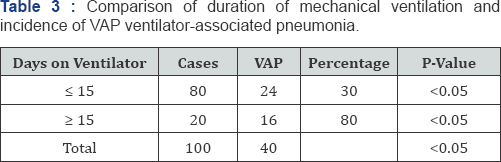
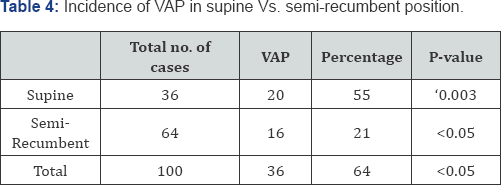
P< 0.05 highly significant
Reintubation results in higher incidence of VAP which causes impairment of cough reflexes hearted sensorrum and risk of espiration in our study. Patient who were not suffering from lung diseases like snake bite, drug overdose and Meningitis have lower incidence of VAP. Position of patient during Mechanical Ventilation also plays an important role in VAP. In Supine position (00) VAP is more as compared to recubent position (30-450). Infection is more when concomittent entral feeding is done during Mechanical Ventilation in supine position. So intubated patient should be kept in recumbent position at the angle of (450) especially during feeding. Level of sensorium also played an important role in development of VAP. In concious patient VAP insidence is less as compared to when patient is in unconcisious stage. In our study VAP was more in Comatose State (64.3% Vs 24.2%) as compared to concisious state. Early tracheostomy should be planned and sucralfate should be given instead of H2 receptor antagonist because they raise PH. Decline in PaO2/FiO2 ratio was diagnostic early sign of development of VAP in Ventilatory suport confirmed by radiography. Fever is non-specific indicator.
Commonest organisum in VAP were Pseudomonas (43%) Klebsiella (18%). Mortality was more in Pseudomonas group while in other study range was 15% - 20%. In Pseudomonas group early onset VAP was 3 while late onset VAP due to multi drug resistant pathogen was 16 in our study. Higher Mortality was reported in late onset VAP which was significant (51%) as compared to non- VAP (41%) which shows VAP does not increase Mortality rate in ICU. Most important single precaution of hand washing measure should be taken with impunity to prevent nosmomial infections before during and after patient handling. Chlorhexidine is proven as effective in Ventilatory associated pneumonia in multi drug resistant cases. Oropharygeal care is another indicator to prevent VAP (Table 5 & 6).
Conclusion
VAP incidence depends on duration of Mechanical Ventilation, promoting nasogastric feeding in semi recubant position at angle of 300-450. Decrease in PaO2 / FiO2 ratio is an early sign of VAP. Commonest micro organisum is Pseudomonas, late onset VAP has higher mortality rate and multi drug resistant cases has poor prognosis in our Institution.
Conflict of Interest
None.
References
- Vincent JL, Bihari DJ, Suter PM, Bruining HA, White J, et al. (1995) The prevalence of noscomal infection in Intensive Care (EPIC) study. EPIC International Advisory Committee. JAMA 274(8): 639-644.
- Trouillet JL, Chastre J, Vuagnat A, Joly Guillou ML, Combaux D (1998) Ventilator-associated Phenumonia caused by potentially drug resistant bacteria. American Journal of Respiratory and Critical Care Medicine 157(2): 531-539.
- Cook DJ, Walter SD, Cook RJ, Griffith LE, Guyatt GH, et al. (1998) Incidence and Risk factor for ventilator Associated Pneumonia in Critically ill patients. Annals of Internal Medicine 129(6): 433-440.
- J Chastre, JY Fagon (2002) Ventilator Associated Pneumonia. American Journal of Respiratory and Critical Care Medicine 165(7).
- GL French, AFB Cheng (1991) Measurement of the costs of hospital infection by prevalance Surveys. J Hosp Infect Suppl A: 65-72.
- Petersen IS, Aru A, Sk0dt V, Behrendt N, Bols B, et al. (1999) Evaluation of Pneumonia diagnosis in Intensive care patients. scand J infect Dis 31(3): 299-303.
- Muscedere J, Rewa O, McKechnie K, Jiang X, Laporta D, et al. (2011) Subglottic secretion drainage for prevention of Ventilator Associated Pneumonia, a systematic review & meta analysis. Crit Care Med 39(8): 1985-1991.
- Zolfaghari PS, Wyncoll DL (2011) The tracheal tube Gateway to Ventilator Associated Pneumonia. Crit care 15(5): 310.
- Crgurich PE, Hiedcova J, Leiy, Sarwar A Craven DE (2013) Diagnosis of Ventilator Associated Pneumonia: controversies and working forwards gold standard. Curr Opin infect Dis 26(2): 140-150.
- Miettoc, pinciroli R, Patel N, Berra L (2013) Ventilator Associated Pneumonia: Evolving definition and preventive measures. Respir Care 58(6): 990-1007.
- Roacha LA, Marques R, da costa, Darini Al, Gontijo Filho PP (2013) Relationship between Nosal Colononisation and Ventilator AssociatedPneumonia and Role of Environment in transmission of staphylococcus aureus in intensive care units Aom. J infect Control 14: 1236-1240.
- (2005) Guidelines for the management of adults with hospital- acquired, Ventilator Associated and healthcare associated pneumonia. AMJ Rep Criti Care Med 2005 171(4): 388-416.
- Ricart M, Lorente C, Diaz E, Kollef MH, Rello J (2003) Nursing adherence with evidence based guidelines for preventing Ventilator Associated Pneumonia, Crit Care Med 31(11): 2693-2696.






























