Low-Dose Ketamine in the Rapid Relief of hyperalgesic vaso-occlusive Bone Crises in Sickle Cell Disease Patients
Owono Etoundi Paul12*, Esiéné Agnès12, Bengono Bengono Roddy2, Tochie Joël2 and Ze Minkandé Jacqueline2
1Department of Anaesthesiology, Yaoundé Central Hospital, Cameroon
2Department of Surgery and Specialties/Anaesthesiology, University of Yaoundé 1, Cameroon
Submission: January 02, 2018; Published: January 22, 2018
*Corresponding author: Owono Etoundi Paul, Department of Surgery and Specialties/Anaesthesiology, University of Yaoundé 1, P.O. Box 1364 Yaounde, Cameroon, Tel: +237-677-981-951; Email: owonop@gmail.com
How to cite this article: Owono E, Esi�n� A, Bengono B, Tochie J, Ze Minkand� J. Low-Dose Ketamine in the Rapid Relief of hyperalgesic vaso-occlusive Bone Crises in Sickle Cell Disease Patients. J Anest & Inten Care Med. 2018; 5(2) : 555656.DOI:10.19080/JAICM.2018.05.555656
Abstract
Background: Evidence abounds on the efficacy of ketamine in the management of acute nociceptive pain. However, there is scant data portraying its analgesic effects in the management of vaso-occlusive crises in sickle cell disease (SCD) patients. The aim of this study was to assess the quality of analgesia procured by low doses of ketamine in the management of hyperalgesic vaso-occlusive bone crises in SCD patients.
Methods: We enrolled 64 SCD patients with mean age of 16.42 ± 5.17 years admitted for multifocal vaso-occlusive bone crises. After assessment of pain on admission using the visual analogue scale (VAS), a bolus of 0.2mg/kg of ketamine followed by a continuous infusion of0. 04mg/kg/h (1mg/kg/24h) was administered. Pain intensity and relief were evaluated one hour after the start of the treatment, then six hourly with adjuvant analgesics till the 24th hour. Variables studied were the variations in pain intensity, pain relief, and the consumption of analgesics and the occurrence of side effects.
Results: On admission, all patients presented severe pain with a mean VAS of 8.3 ± 0.7 cm. One hour following the debut of ketamine administration, 30 (46.9 %) patients had a VAS ≤ 3 (mean: 2.9 ± 0.1 cm), and 46 (71.9 %) reported pain relief with a mean VAS of 3.3 ± 0.6 cm. Based on VAS, a reduction of pain intensity was observed till the 24th hour of therapy. Paracetamol and ketoprofen were the sole analgesic adjuncts to ketamine used for a rapid relief of pain within 24 hours of treatment. Hypersialorrhoea (4.7 %) was the lone side effect observed.
Conclusion: Low-dose ketamine is effective and ensures a rapid optimal pain resolution with well tolerated side effects and a reduction in adjuvant analgesic consumption in the management of vaso-occlusive sickle cell crises.
Keywords: Sickle cell disease; Vaso-occlusive bone crises; Ketamine
Introduction
Worldwide, sickle cell disease (SCD) represents the most common genetic disorder of haemoglobin and disproportionately affects Africa [1-3]. This disease is associated with a profound clinical polymorphism entailing three main categories of clinical presentations; chronic haemolytic anaemia with episodes of acute exacerbation, vaso-occlusive crises and an increased susceptibility to bacterial infections [1-3,4]. Vaso-occlusive crises account for the first cause of hospital admissions in SCD patients. Vaso-occlusion and its consequences, at the core origin ofpain in SCD complications, clinically present as paroxystic and hyperalgesic pain crises particularly affecting long bones. Several protocols entailing the use of paracetamol, non-steroidal anti-inflammatory drugs, and morphine-like drugs have been advocated in the management of vaso-occlusive bone crises [4-7]. Considering the nociceptive and hyperalgesic characteristics of the pain of vaso-occlusive crises, would ketamine be effective in the management of these crises? Hence, we conducted this study to assess the quality of analgesia induced by low doses of ketamine in the management of hyperalgesic vaso-occlusive bone crises in SCD patients.
Patients and Methods
This was an open prospective study that was conducted from January 2012 to June 2016 at the Emergency Department of the Yaounde Central Hospital in Cameroon. After taking approval from the National Ethics Committee, and obtaining a written informed consent from all patients, we included 64 SCD patients, aged above six years, and admitted for a vaso-occlusive bone crisis whose pain intensity assessed using the visual analogue scale (VAS) was greater than five. Patients who did not understand the VAS, those with contra-indications to the drugs used and patients who refused to participate in the study were not included. Any patient with presumed complications of SCD as acute chest syndrome, stroke, splenic sequestration, priapism, sepsis and acute osteomyelitis were not included.
On admission into the Emergency Department, pain intensity was evaluated using the VAS graduated from 0 to 10 cm. Thereafter, all patients received an intravenous bolus of 0.2mg/kg of ketamine, followed by continuous ketamine intravenous injection of 0.04 mg/kg/h [1mg/kg/24h) using an electric syringe. All patients were oxygenated through a mask (3-5l/min), hyperhydrated using polyionic glucose solution [50 ml/kg/24h), and warmed using isothermic blankets. Blood transfusion was indicated in case of poorly tolerated anaemia. Pain intensity was re-evaluated after 30 minutes, 60 minutes, and then six hourly till the 24th hour where the patient was transferred to the Haematology Department for further management. At the 60th minute, the efficacy of the treatment was assessed by the number of SCD patients with a la VAS less than or equal to three [VAS60≤3). Furthermore, every patient had to respond by "yes" or "no" to the question "has your pain been relieved?"After the 60th minute, the electric syringe administration of ketamine was continued (0.04mg/kg/h) and analgesics were added to treatment with respect to the VAS. When the VAS was zero, between 1 and 3, 4 and 6 or greater than 7, the patient received respectively: no analgesic, paracetamol(15mg/ kg) slow intravenous[SIV), paracetamol[15mg/kg) and ketoprofen[1mg/kg, SIV), paracetamol(15mg/kg) and ketoprofen (1mg/kg) plus morphine in titrations at 0.025 mg/kg [SIV) every five minutes until the pain subsided. The interval of administration of analgesics was in conformity to their kinetics: paracetamol [15mg/kg/6 hours in children and 1g/6 hours in adults), ketoprofen (1mg/kg/8 hours) and morphine [analgesic doses after titration every 8 hours). The same anaesthesiologist physician performed the evaluation of pain intensity.
Variables studied were: the number of patients with a VAS60≤ 3(primary endpoint), the number of patients relieved at the 60th minute [secondary endpoint). Two groups of patients were constituted and compared using the primary endpoint. The consumption of analgesics and the occurrence of side effects were also studied. Data analysis was performed using Epi info 3.5.4 statistical software. Means and standard deviations of numerical variables were reported. Categorical variables were analysed using the Fisher's exact test or the Pearson's Chi-square test where appropriate. Qualitative variables were analysed using the Student t-test or the Kruskal-Wallis test where appropriate. The threshold for statistical significance was set a p-value less than 0.05.
Results
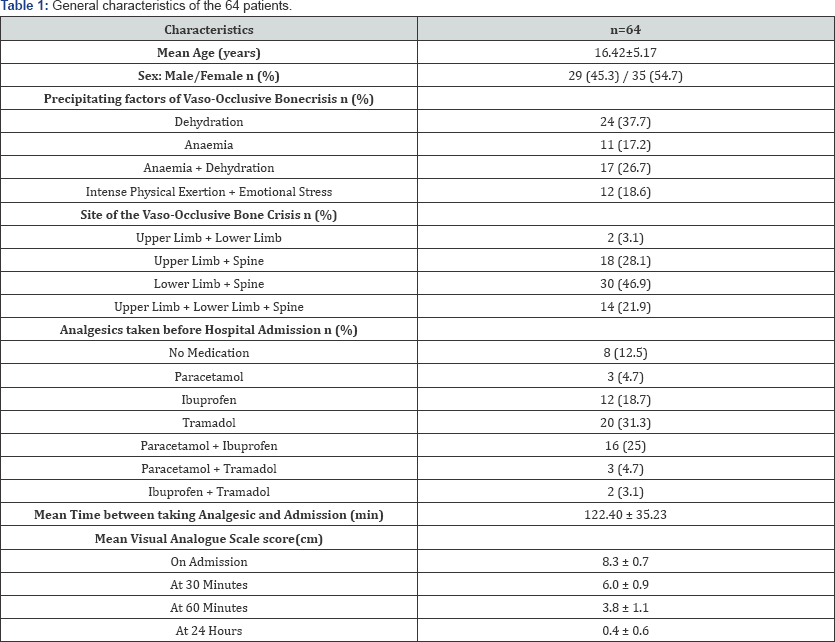
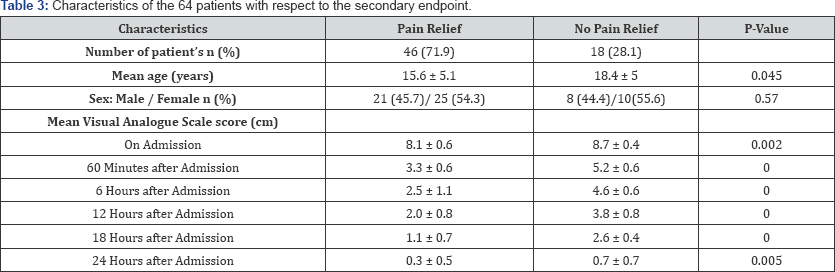
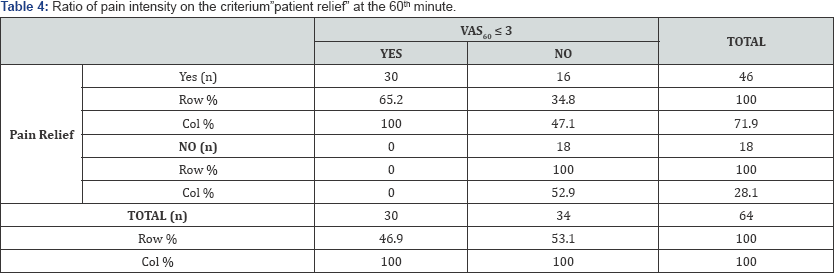
During the study period, 64 SCD patients with multifocal vaso-occlusive osteo-articular crises were enrolled. The general characteristics of these patients are illustrated in Table 1. Sixty minutes following the initiation of treatment with ketamine, two groups of patients were constituted based on the primary endpoint (Table 2). No statistically significant difference was observed between the two groups regarding the number of patients, their age and gender. However, there was a statistically significant difference between the VAS scores observed in the two groups one hour after the debut of ketamine administration (Table 2). With regards to the secondary endpoint, 46 [71.9%) patients reported pain relief 60 minutes after the start of treatment with ketamine (Table 3). The reduction of pain intensity observed on the VAS60 coupled with "a pain relief respond" at the 60th minute of treatment helped deduce a VAS sensibility of 100%, a specificity of 52.9%, a positive predictive value of 65.2% for the endpoint "patient relief" and a negative predictive value of zero (Table 4). Paracetamol and ketoprofen were the sole analgesic adjuncts to ketamine used for a rapid relief of pain within 24 hours of treatment (Table 2). Hypersialorrhoea [4.7 %) was the lone side effect observed.
Discussion
Ketamine at infra-anesthetic doses has an antagonist action on N-Methyl-D-Aspartate [NMDA) receptors. Indeed, in blocking NMDA receptors of glutamate, ketamine reduces central sensitisation induced by opioids and tissue lesions, with resultant inhibition of hyperalgesia leading to a reduction in pain intensity and minute consumption of analgesics. Hence, ketamine is indicated in the management of acute pain where a central sensitisation is implicated [8-10]. The present study aimed at evaluating the quality of analgesia induced by a bolus of ketamine followed by a continuous infusion, in the rapid relief of pain of hyperalgesic vaso-occlusive bone crises in SCD patients. Our findings portray a significant reduction in the intensity of pain perceived by SCD patients following the commencement of ketamine administration (Table 1). Indeed, one hour following the onset of treatment, 46.9 % of patients had a VAS ≤ 3 and 71.9 % parallelly reported pain relief (Table 2 & 3). The inhibition of central sensitisation due to the fixation of ketamine on NMDA receptors certainly led to a reduction in the hyperalgesia phenomenon in these patients who presented severe multifocal bone pain on admission (Table 1). Thus, ketamine appears as an alternative in the management of hyperalgesic vaso-occlusive bone crises in SCD patients. While several authors recommend a combined first-line analgesic therapy using paracetamol, nonsteroidal anti-inflammatory drugs and opioids in the management of vaso-occlusive sickle cell crises [5-10], ketamine could be an invaluable option with a positive predictive value of 65.2 % at the 60th minute (Table 4). Our results concur with those of Uprety et al. [11] & Neriet al. [12] who affirmed that low-dose ketamine was safe and effective in SCD patients with severe painful vaso- occlusive bone crises.
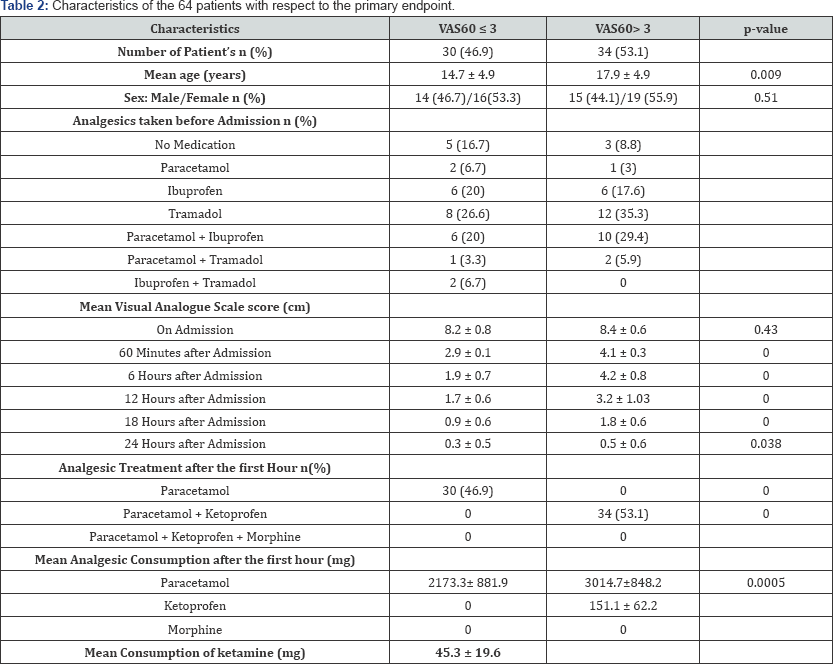
After the first hour of treatment with ketamine, 34 (53.1 %) patients had a VAS60> 3 and among them, 18 [28.1 %) were not relieved (Table 2 & 3). These were mainly female patients with habitual tramadol consumption and in whom the last administration of tramadol dated less than two hours prior to hospital admission (Table 2). In these patients, after the 60th minute, the management of pain entailed the use of analgesic adjuncts with paracetamol and ketoprofen to achieve a VAS of 0.4 ± 0.6 cm at the 24th hour. Meanwhile patients with a VAS60 ≤ 3 had only benefited from the addition of paracetamol to achieve the same score at the discharge (Table 2 & 3)Hence, the present study depicts that ketamine at low doses associated with paracetamol and ketoprofen led to the rapid relief of vaso-occlusive bone pain in SCD patients within 24 hours. This analgesic protocol was simultaneously administered with the correction of dehydration and anaemia, which accounted for the main precipitating factors of these vaso-occlusive crises. The time lapse for pain relief in our cohort differs from that of Mbassi et al. [13], who obtained resolution of vaso-occlusive pain crises after a mean duration of 5 ± 3.5 days using the joint administration of paracetamol, nonsteroidal anti-inflammatory drugs (including ketoprofen) and tramadol [or morphine).
Although there is no universal consensus till present date on the management of pain in SCD patients [14], our analgesic protocol with ketamine is peculiar in that it procures rapid and optimal pain relief, which are both obligations of a healthcare provider towards his/her patient in pain agony, and it leads to a saving of analgesics [especially morphine). Thus, despite the absence of consensus on the dose and duration of treatment [15], low-dose ketamine proved to be efficacious in the rapid management of acute hyperalgesicvaso-occlusive bone crises in SCD patients [11,12].
Taking into consideration the deleterious effects of pain on the quality of life of SCD patients, the most important clinical significance of this study is the rapid and optimal management of pain. Moreover, the non-utilisation of opioids is an important asset in our resource-limited setting where morphine is not always available and accessible. Therefore, ketamine, paracetamol and ketoprofen, which are all readily accessible drugs, represent an analgesic option with good tolerance in the management of bone pain crises in SCD patients.
Our study has some limitations; mainly the analgesic drugs taken by patients at home prior to hospital admission may have interfered with our analgesic protocol and influenced the perception of pain in these patients. Much more, the assessment of pain using the VAS was subject to a potential risk of subjectivity that may have either underestimated or overestimated the true pain intensity.
Conclusion
Low doses of ketamine bolus followed by a continuous administration in the management of vaso-occlusive sickle cell crises procures a rapid, effective and optimal pain relief with well- tolerated side effects and a reduction in analgesic consumption. The use of low-dose ketamine should be emphasised in SCD patients with bone pain crises.
Acknowledgment
We would like to acknowledge the study participants for their commitment
Conflict of Interest
The authors declare that they have no competing interests.
References
- Haute Hautorité de Santé (2010) Syndromé drepanocytaire majeurs de l'enfant et l'adolescent. p. 1-69
- World Health Organisation (2011) Sickle Cell: A strategy for the WHO African Region. Report of the General Director.
- Sicheré P (2015) Sickle cell disease and pain. Questions put to Elena Foi's. Douleurs Evaluation Diagnostic Traitement 16: 315-317.
- Wilson BH, Nelson J (2015) Sickle Cell disease pain management in adolescents: a literature review. Pain Manag Nurs 16(2): 146-151.
- Angoulvant F, Redant S, Holvoet L, Millet B, Ferster A, et al. (2011) Pain management of children with sickle cell disease in the emergency department: recommendations and current situation in the FrenchSpeaking Mother and Child Network. Reanimation 20(6): 516-524.
- Mousa SA, Al Momen A, Al Sayegh F, Al Jaouni S, Nasrullah Z, et al. (2010) Management of painful vaso-occlusive crisis of sickle cell anemia: consensus opinion. Clin Appl Thromb Hemost1 6(4): 365-376.
- Serraj K, Mecili M, Housni B, Andres E (2012) Complications aigues de la drepanocytose de l’adulte: de la physiopathologie au traitement. mt 18(4): 239-250.
- Richebe P, Rivat C, Rivalan B, Maurette P, Simonnet G (2005). Low doses ketamine: antihyperalgesic drug, non-analgesic. Ann Fr Anesth Reanim 24(11-12): 1349-1359.
- Chauvin M (2005) Ketamine in the management of acute pains: from pharmacology to clinical applications. Reanimation 14: 686-691.
- Mion G (2015) Ketamine: hypnotique, analgesique et anti- hyperalgesique. Conference d'essentiel. SFAR 2015 p. 18.
- Uprety D, Baber A, Foy M (2014) Ketamine infusion for sickle cell pain crisis refractory to opioids: a case report and review of literature. Ann Hematol 93(5): 769-771.
- Neri CM, Pestieau SR, Darbari DS (2013) Low-dose ketamine as a potential adjuvant therapy for painful vaso-occlusive crises in sickle cell disease. Peadiatr Anaesth 23(8): 684-689.
- Mbassi Awa HD, Dongmo F, Ngo Um S, Mafo Fonkwo V, Alima Yanda A, et al. (2017) Epidemiological, clinical and therapeutic aspects related to the occurrence of vaso-occlusive crises in homozygous sickle cell children in three hospitals in Yaounde. Health Sci Dis 18(4): 89-97.
- Hildenbrand AK, Nicholls EG, Daly BP, Marsac ML, Tarazi R, et al. (2014) Psychosocial and pharmacological management of pain in pediatric sickle disease. Postgrad Med 126(2): 123-133.
- Martinez V, Derivaux B, Beloeil H (2015) Ketamine for pain management in France, an observational survey. Anaesth Crit Care Pain Med 34(6): 357-361.






























