Acute Interstitial Pneumonia after Lung Resection in a Patient with Leucocytoclastic Vasculitis but No History of Interstitial Lung Disease. The Importance of Anaesthetic Technique and Early Use of Steroids
Andrea Bille1*, Simon Sparks2, Sangita Agarwal3, Boris Lams4 and Andy Fearnley5
1Department of Thoracic Surgery, Guy's and St Thomas Hospital, UK
2Department of Critical Care Department, Guy's and St Thomas Hospital, UK
3Department of Critical Care Department, Guy's and St Thomas Hospital, UK
4Department of Thoracic Medicine, Guy's and St Thomas Hospital, UK
5Department of Anaesthesia, Guy's and St Thomas Hospital, UK
Submission: December 12, 2017; Published: January 12, 2018
*Corresponding author: Andrea Bille, Department of Thoracic Surgery, Guy's Hospital, 6th Floor Borough Wing, Great Maze Pond, London, SE1 9RT, UK, Tel: +44(0)20-7188-7188, Email: andrea.bille@gstt.nhs.uk
How to cite this article: Andrea Bille, Simon Sparks, Sangita Agarwal, Boris Lams, Andy Fearnley. Acute Interstitial Pneumonia after Lung Resection in a Patient with Leucocytoclastic Vasculitis but No History of Interstitial Lung Disease. The Importance of Anaesthetic Technique and Early Use of Steroids. J Anest & Inten Care Med. 2018; 5(4) : 555654. DOI: 10.19080/JAICM.2018.05.555654
Abstract
Acute interstitial pneumonia (AIP) in individuals with interstitial lung disease (ILD) is a recognised complication following single lung ventilation and lung cancer surgery and is associated with 50% mortality. We present a patient with a diagnosis of leucocytoclastic vasculitis who newly developed an AIP and respiratory failure following a right video assisted thoracic surgery (VATS) upper lobectomy for T1a N2 M0 adenocarcinoma with no previous history of interstitial lung disease (ILD). Treatment with high dose intravenous steroids and lung protective mechanical ventilation produced a rapid resolution of respiratory failure within 24 hours. Anaesthetists should adopt a protectiveventilatory strategy when anaesthetising individuals with leucocytoclastic vasculitis and other forms of vasculitis for lung cancer surgery to minimise the risks of developing AIP. The immunomodulatory properties of halogenated volatile anaesthetic agents may confer additional benefits in comparison to total intravenous anaesthetic techniques in lung resection surgery in these high risk individuals.
Keywords: Lung resection; Lung ARDS; Vasculitis
Introduction
Acute interstitial pneumonia (AIP) as defined by the American Thoracic Society [1] is a recognised complication of lung resection for cancer. The condition is most frequently seen in patients with underlying interstitial lung disease (ILD) and May occurred in 1 to 12% of such patients undergoing elective anatomical lung resection for cancer. The mortality associated with the syndrome is extremely high and exceeds 50% [2-5]. The path physiology is complex with risk factors including preoperative use of steroids, preoperative alcohol abuse, single lung ventilation, high positive pressure ventilation, and high inspired concentrations of oxygen, excessive fluid administration and the volume of lung resected. We present a patient withle ucocytoclastic vasculitis but no previous history of ILD who developed a new onset AIP and severe respiratory failure 48 hours after undergoing a video assisted thoracic surgery (VATS) right upper lobectomy and lymph node dissection for T1a N2 M0 adenocarcinoma necessitating reintubation and mechanical ventilation. Treatment with high dose IV steroids and lung protective mechanical ventilation in intensive care resulted in a rapid improvement in gas exchange within 24 hours.
Case Presentation
A 56 year old female current smoker with a history of hypertension presented to her family doctor with a 6 month history of weight loss, neuropathic pain and fatigue. Referral to a Rheumatology centre facilitated a diagnosed of leukocytoclastic vasculitis and she was commenced upon oral methotrexate 15mg weekly and prednisolone 20mg daily. A routine chest X-ray (CXR) performed as part of her initial investigations revealed a right upper lobe (RUL) lung lesion but no other abnormalities. Positron emission tomography (PET) confirmed a right upper lobe nodule of high FDG uptake (SUV 4.3) and no evidence of nodal and distant metastatic disease. Chest computer tomography (CT) confirmed the lung lesion, with no evidence of other lung abnormalities (Figure 1a-1c). 3 weeks later she underwent a right VATS upper lobectomy and systematic mediastinal lymph node dissection. The patient had ceased her methotrexate a week prior to surgery. The patient was anaesthetised with a Propofol target controlled intravenous infusiontargeted to achieve a Bispectral index of 4060 and Fentanyl 2mcg/kg.
Neuromuscular blockade was achieved using Rocuronium 0.6 mg/kg. The trachea was intubated with a 37Ch left sided double lumen endotracheal tube (Rusch Bronchopart) and lung isolation was confirmed clinically and with a fibreoptic bronchoscope. The patient was turned into the left lateral position and a pre-emptive paravertebral injection was made using 30mls of 0.25% Levo- Bupivacaine under ultrasound guidance. One lung ventilation was commenced using pressure control ventilation with peak inspired pressure of 22cm H2O and 5cm H20 positive end expiratory pressure achieving tidal volumes of approximately 6-8ml/kg. The inspired oxygen concentration was maintained at 100% for 5 minutes after commencing one lung ventilation and then reduced to 80% for the remainder of the case. Oxygen saturations remained at 100% throughout. Surgery was uneventful and lasted approximately 2 hours with blood loss during the procedure estimated to be less than 50mls. Intraoperative intravenous fluid administration totalled 1000mls of balanced crystalloid solution. Additional intraoperative medications included Teicoplanin 400mg, Dexamethasone 6.6mg, Ondansetron 4mg, Paracetamol 1g, Morphine 8mg and Magnesium sulphate 3g. At the conclusion of surgery the patient was extubated and transferred to the recovery unit. The final histology showed a T1a N2 M0 adenocarcinoma with clear surgical margins.
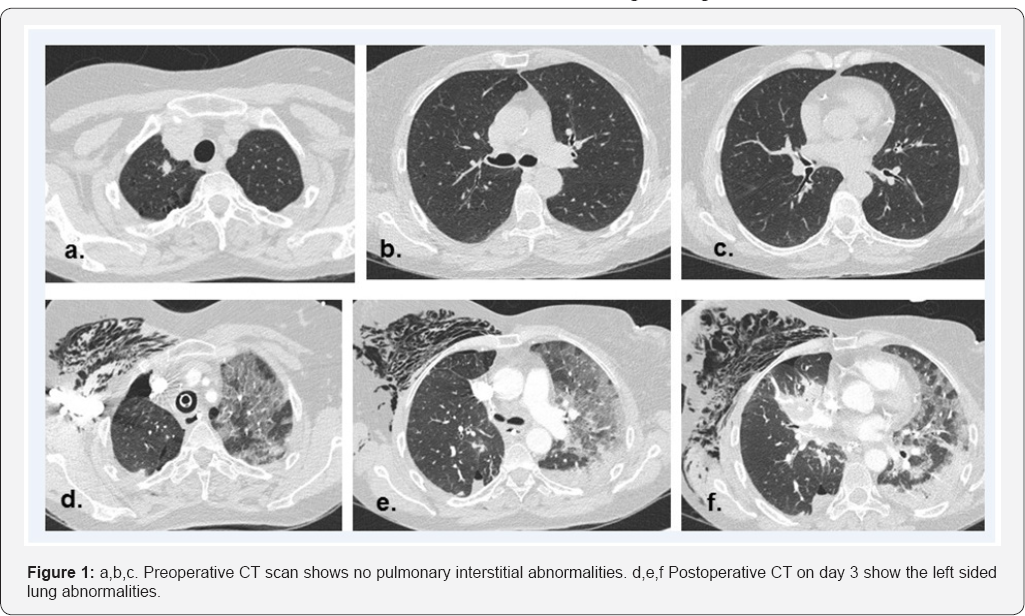
The patient's initial post-operative course was unremarkable. The intercostal drain was removed on the first post-operative day with no evidence of pleural effusion, consolidation or pneumothorax on CXR. On the second postoperative day the patient developed shortness of breath and hypercapnoeic respiratory failure necessitating transfer to the intensive care unit. Treatment with high flow nasal oxygen and aggressive physiotherapy were unsuccessful and in the context of worsening respiratory failure the patient was intubated and mechanically ventilated. Repeat CXR showed severe diffuse left sided infiltrates. The remaining right lung was unaffected. A bronchoscopy was performed and sputum was sent for microscopy culture and sensitivity. Empirical intravenous Clarithromycin and Gentamicin was commenced. A Chest CT was performed that showed extensive left lung interstitial changes and no evidence of pulmonary embolism (Figure 1d-1f). In the absence of any positive microbiology findings the patient was treated with high dose intravenous hydrocortisone.
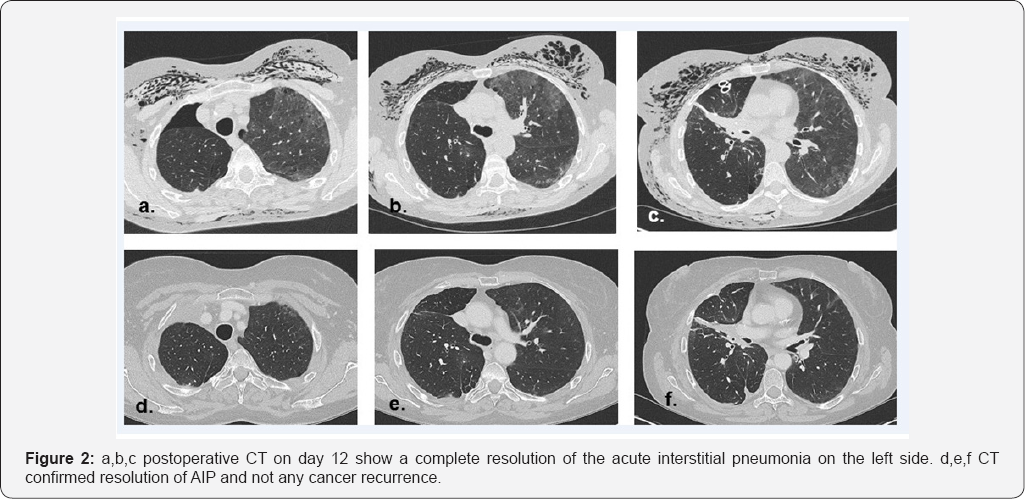
The next 24 hours witnessed a dramatic improvement in the patients respiratory function and radiological findings and it was possible to extubate the patient 24 hours after commencing intravenous steroids (Figure 2a-2c). She was discharged from the intensive care unit the following day and was discharged home on oral prednisolone after a total of 15 days in hospital. The patient is now fully recovered with no evidence of interstitial lung changes on repeat CT scan performed as an outpatient (Figure 2d-2f) and has now started adjuvant chemotherapy.
Discussion and Conclusions
Five to fourteen percent of thoracic patients develop respiratory complications after lung resection surgery. They account for approximately fifty percent of all major post-operative complications and may severely adversely affect operative outcomes. The most frequent complications are atelectasis and pneumonia with the incidence of postoperative interstitial pneumonia reported to be between 1.1% and 11.7% [5]. Most cases of acute interstitial pneumonia (AIP) occurring following lung resection surgery are reported as acute exacerbations in individuals with pre-existing interstitial lung disease (ILD) [2]. In this subgroup of patients the mortality rate exceeds 30% [2,5]. The mechanisms causing AIP after anatomical lung resection in patients with lung cancer are unknown, but appear to be related to preoperative use of steroids, preoperative alcohol abuse, the use of high intraoperative ventilatory pressure, excessive fluid administration, high inspired oxygen concentration and to the volume of lung resected. The latter is believed to contribute to damage to the intrapulmonary vascular endothelium [1].
In order to reduce the risk of acute interstitial pneumonia, treatment of the underlying interstitial lung disease is essential, along with intra operative lung protective strategies including low tidal volume ventilation, permissive hypercapnoea and low positive expiratory pressure (PEEP). There is also increasing evidence that the use of halogenated volatile anaesthetic agents may confer additional beneficial immunomodulatory effects when compared to total intravenous anaesthetic techniques [6]. Postoperative ly ventilator strategies should be similarly protective and include conservative fluid management, incentive spirometry and early mobilisation. Infection is a common cause of unilateral pulmonary infiltrates so the early administration of antibiotic therapy should be considered, however in the presence of inflammatory changes with no evidence of infection high dose intravenous steroids should be administered early in an attempt to reduce the high mortality rate associated with AIP.
This case highlights a possible association between underlying vasculitic disease and AIP. Thoracic anaesthetists should consider such individuals as being at extremely high risk for post-operative respiratory complications such as AIP and modify anaesthetic management accordingly including the use of halogenated anaesthetic agents and strict lung protective strategies. The role of early high dose steroid administration in improving outcomes following the development of AIP in individuals with no previous history of interstitial lung disease is also highlighted. For many years in thoracic surgery, postoperative steroid use has been controversial due to the perceived risk of bronchopleural fistula formation and hospital acquired pneumonia. However, in patients with underlying autoimmune disease, early postoperative respiratory insufficiency can be related to an intense acute inflammatory response to single lung ventilation and other factors and a combination of protective mechanical ventilation and steroids should be considered as an essential part of early treatment. Additional forms of protective ventilatory support such as ECMO may also need to be considered if expertise allows and respiratory failure is severe and refractory to standard protective mechanical ventilation.
To our knowledge this represents the first report showing an association between anatomical lung resection, peripheral vasculitis and postoperative AIP in a patient with no evidence of interstitial lung disease or pulmonary fibrosis. We postulate that this individuals underlying vasculitis predisposed her to severe post-operative respiratory complications following lung resection surgery with single lung ventilation, high inspired oxygen concentrations and total intravenous anaesthesia triggering an intense inflammatory response and AIP. A protective benefit may have been afforded to the patient through the use of lower inspired oxygen concentrations intraoperatively and the use of halogenated volatile anaesthetic agents rather than total intravenous anaesthesia. The future promises a greater understanding of the immune implications of surgical and anaesthetic techniques in lung resection surgery and further studies are needed to clearly delineate strategies that should be employed to minimise the risk of post-operative respiratory complications in high risk individuals when undergoing lung resection surgery.
Acknowledgment
Thanks to Dr Madalina Campianu in helping collecting the clinical data of this patients.
Funding
No funding has been used for this paper.
References
- Raghu G, Collard HR, Egan JJ, Martinez FJ, Behr J, et al. (2011) An official ATS/ERS/JRS/ALAT statement: idiopathic pulmonary fibrosis:evidence-based guidelines for diagnosis and management. Am J Respir Crit Care Med 183(6): 788-824.
- Sato T, Teramukai S, Kondo H, Watanabe A, Ebina M, et al. (2014) Impact and predictors of acute exacerbation of interstitial lung diseases after pulmonary resection for lung cancer. J Thorac Cardiovasc Surg 147(5): 1604-1611.
- Ruffini E, Parola A, Papalia E, Filosso PL, Mancuso M, et al. (2001) Frequency and mortality of acute lung injury and acute respiratory distress syndrome after pulmonary resection for bronchogenic carcinoma. Eur J Cardiothorac Surg 20(1): 30-36.
- Oyama K, Kanzaki M, Kondo M, Maeda H, Sakamoto K, et al. (2017) Early Detection of the Acute Exacerbation of Interstitial Pneumonia after the Surgical Resection of Lung Cancer by Planned Chest Computed Tomography. Korean J Thorac Cardiovasc Surg 50(3): 177-183.
- Chida M, Kobayashi S, Karube Y, Hayama M, Tamura M, et al. (2012) Incidence of acute exacerbation of interstitial pneumonia in operated lung cancer: institutional report and review. Ann Thorac Cardiovasc Surg 18(4): 314-317.
- F de la Gala, P Pineiro, A Reyes, E Vara, L Olmedilla, et al. (2017) Postoperative Pulmonary Complications, Pulmonary and systemic inflammatory responses after lung resection surgery with prolonged one-lung ventilation. Randomized controlled trial comparing intravenous and inhalational anaesthesia. Brit Journal Anaesthesia 119(4): 655-663.






























