Anaesthetic Recommendations for Stiff Person Syndrome
Darren Yak Leong Chan* and Robyn Gillies
The Royal Melbourne Hospital, Australia
Submission: April 17, 2017; Published: August 07, 2017
*Corresponding author: Darren Yak Leong Chan, The Royal Melbourne Hospital, 300 Grattan St Parkville, VIC 305, Australia, Email: ylcha22mon@gmail.com
How to cite this article: Darren Y L C, Robyn G. Anaesthetic Recommendations for Stiff Person Syndrome. J Anest & Inten Care Med. 2017; 3(3) : 555615. DOI: 10.19080/JAICM.2017.03.555615
Abstract
Background: Stiff person syndrome (SPS) is a neurological condition with serious implications during anaesthesia if overlooked.
Objective: Our purpose was to highlight the issues encountered during anaesthesia in patients with SPS and to evaluate the most appropriate anaesthetic management during surgery.
Methods: A structured search was performed throughout various databases such as Ovid medline, Pubmed, Embase and Cochrane Collaboration for articles published from 1950s and after. The search included only humans and those who underwent procedures with anaesthesia.
Results: Only 13 of such case studies were found due to the rarity of the condition. Amongst these 13 patients, most were in the middle to elderly aged groups and they underwent different procedures. Their response to different drugs used for induction, neuromuscular blockade or maintenance of anaesthesia also varied with some leading to life-threatening complications especially due to postoperative hypotonia. Route of anaesthesia also had a role in changing the outcomes.
Conclusion: SPS is challenging to manage and the use of drugs like midazolam, propofol, rocuronium is recommended to improve patient outcomes. Volatile agents are safe if their doses are kept to a minimum with bispectral index monitoring. Alternative routes of anaesthesia may be better but this is not always feasible.
Keywords: Stiff person syndrome; General anaesthesia; Neuromuscular blockers; Inhalational anaesthetics; Surgery
Introduction
Stiff person syndrome (SPS) is a unique neurological disorder first described in 1956 by Moersch & Woltman [1]. It has no known genetic predisposition [2] but an association with certain HLA genes exists [3]. SPS is slowly progressive with insidious onset, which commonly begins in the middle-age [4-6]. It is typified by stiffness and rigidity of the axial and proximal limb musculature, with superimposed painful spasms [2,3,6]. In more severe cases, the muscles of respiration and swallowing are affected and may cause respiratory distress [5,7].
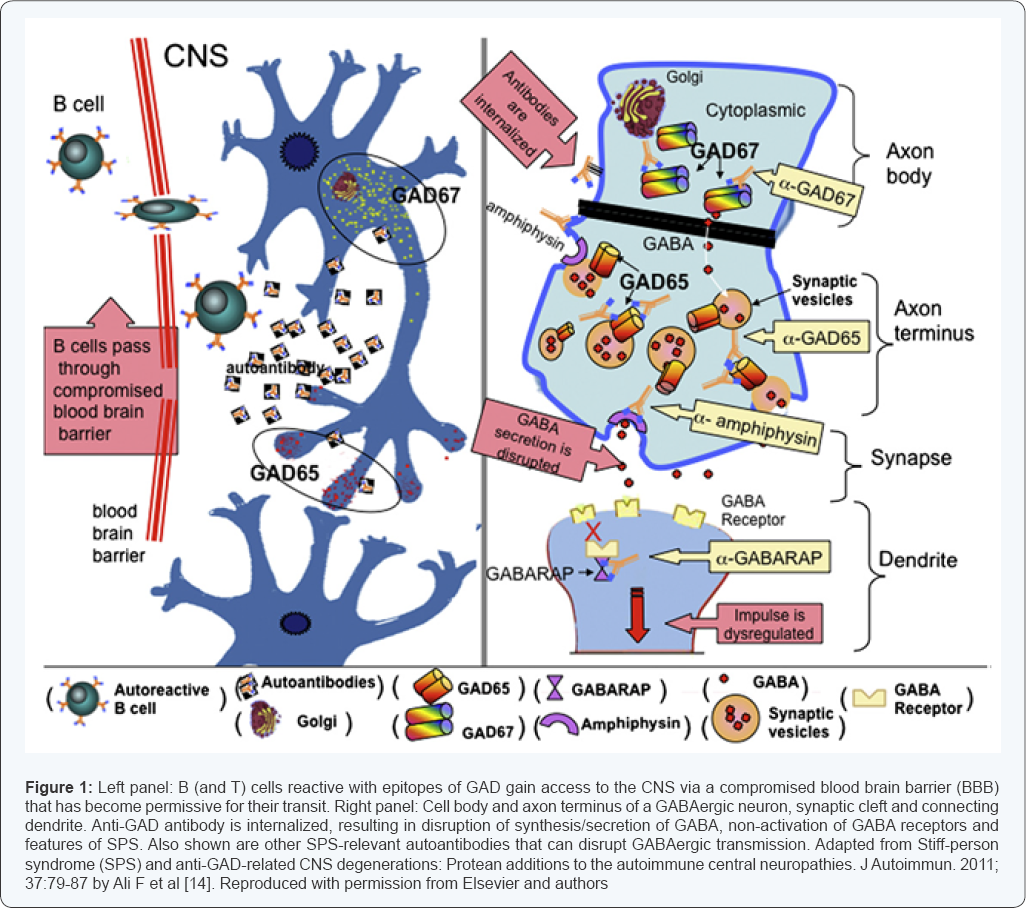
The painful spasms can be triggered by external sensory stimuli, voluntary movement, fear, anxiety [8,9] and appear to arise from the brain or spinal cord because they stop during general anaesthesia (GA) or sleep. The aetiology of SPS seems to be autoimmune as circulating autoantibodies reactive with glutamic acid decarboxylase (GAD) have been found in SPS patients [10,11]. GAD is an enzyme necessary for the production of gamma-aminobutyric acid (GABA). GABA has an inhibitory (gabanergic) input to muscles causing a muscle relaxant effect. Reduction in GABA production upsets the balance of excitatory inputs in various areas of the brain, specifically the gamma- motor neuron system, leading to continual motor neuron activity and spasms [12,13]. Figure 1 illustrates the action of anti-GAD antibodies [14].
Drugs enhancing central gabanergic neurotransmission such as diazepam are used in treating SPS because it increases the frequency that GABA receptors are activated. Baclofen synergises with diazepam and is prescribed together. Similarly useful drugs include clonazepam and sodium valproate [5,15]. Other treatments inducing remission involve immunosupression with steroids [5] or rituximab [16].
SPS if overlooked may lead to serious problems with anaesthesia. The mechanism of rigidity involved is different from malignant hyperthermia which has a rapid onset of symptoms often triggered by various anaesthetic agents [17,18] and SPS should not be a contraindication for surgery. Careful monitoring and choice of anaesthesia is still essential.
The principal aim of this review is to provide recommendations in the anaesthetic management of a patient with Stiff-Person Syndrome (SPS) during surgery. Additionally, a literature review and suggestions on how to choose anaesthetic drugs in order to avoid postoperative complications will be discussed.
Methods
A structured search was performed through Ovid medline, Pubmed, Embase and Cochrane Collaboration; this includes articles in English language published from 1950s until the present. A Medical Subject Headings (MeSH) search within titles and abstracts with keywords such as "Stiff man syndrome", "Stiff person syndrome", "SPS", "SMS", "Anaesthesia", 'Anesthesia", "Anaesthetics" and "Anesthetics" was done.
The search was limited to include only studies involving humans.
Results
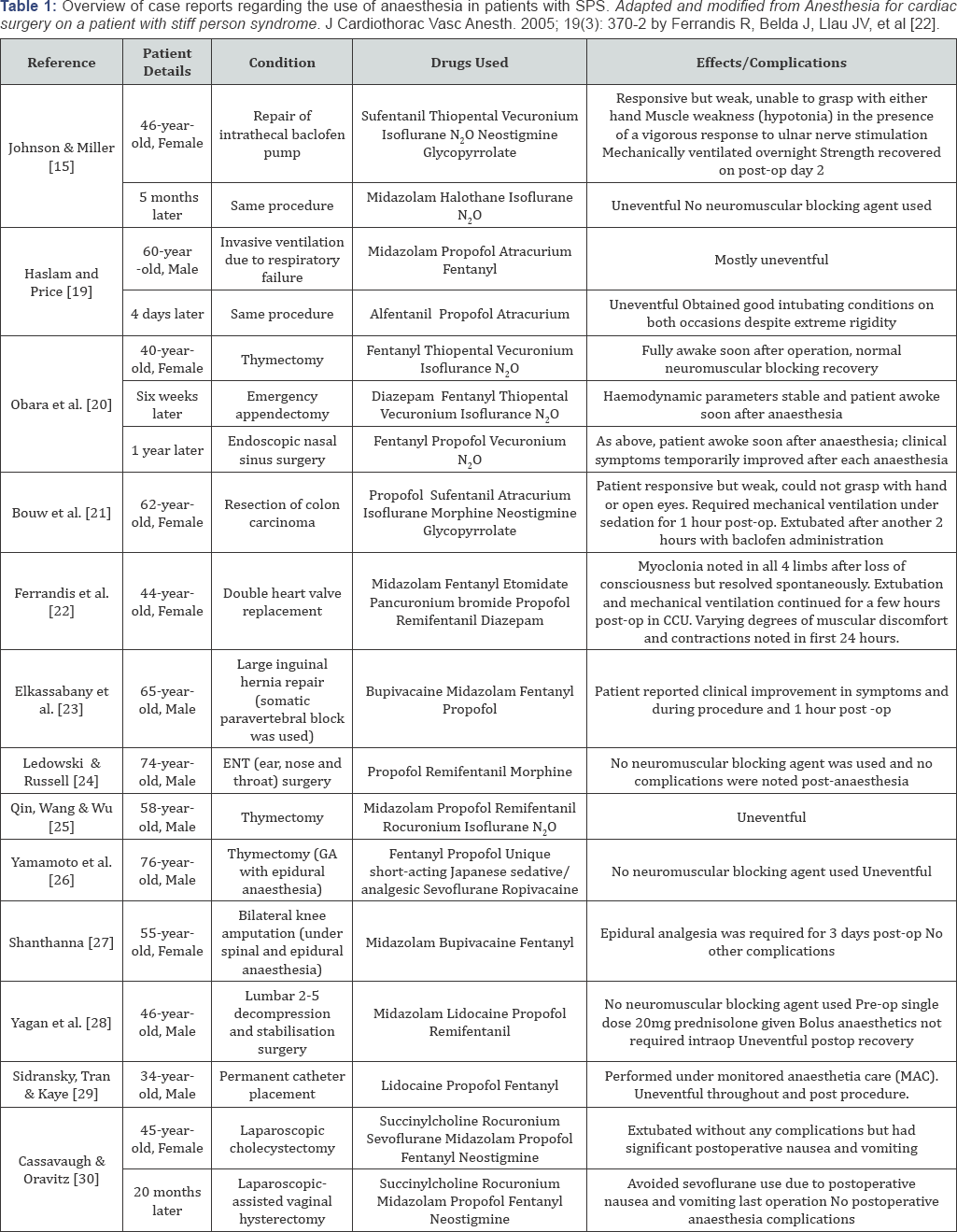
There are no randomised controlled trials or case-control studies involving the effect of anaesthetic drugs in SPS patients or recommended anaesthetic drugs of choice. Nevertheless, there were 13 case reports describing peri- and intraoperative management of SPS patients; with some studies highlighting the increased risk of postoperative hypotonia as shown in Table 1 below.
Discussion
Firstly, the use of appropriate temperature monitoring and regulation during surgery for SPS patients with the aid of a Bair hugger is recommended. As baclofen is the mainstay therapy for SPS, such patients would have poor temperature perception. Oliviero et al. [31] showed that long-term baclofen therapy would impair temperature perception as it increases both the threshold for warm and cold stimuli. This occurs because baclofen activates receptors for GABA-B which modulates temperature perception.
For induction, propofol is a safe choice and other alternatives include halogenated gases, thiopental, propofol and etomidate [32] which act via the gabanergic pathway. Such agents should reduce postoperative muscle spasm or pain in SPS patients, who have decreased gabanergic input. Etomidate has been reported by Ferrandis et al. [22] to have a higher risk of intraoperative myoclonus. This reflects neuromuscular hyperexcitability but it is unclear whether SPS perpetuated the myoclonus [22], or if etomidate had an idiosyncratic effect. Diazepam, fentanyl and atropine have been prescribed as pre-medication [33] to overcome myoclonus in non-SPS patients but Ferrandis et al. [22] reported that these were ineffective in their SPS patient. A higher dose of benzodiazepine could have been useful but there is insufficient literature to support this [22].
Propofol has also been implicated in case reports to cause intraoperative myoclonus [34-36] but it has a lower risk. A randomised controlled trial by Miner et al. [37] reported that 18.2 % more (95% CI 10.1% to 26.2%) non-SPS patients who received etomidate had intraoperative myoclonus compared to those on propofol. Moreover, propofol improves postoperative muscle rigidity and spasms as reported by Obara et al. [20]. The published literature suggests that propofol reduces spinal activity [38] by acting primarily on GABA-A receptors [39-41] with some partial effect on central GABA-B receptors [42-44] unlike baclofen, which is a selective GABA-B receptor agonist [45-47].
Propofol would be the drug of choice for anaesthesia induction in SPS patients with the concomitant use of midazolam, which also modulates GABA-A receptor activity [43]. Pre-medication is not necessary since these SPS patients would have already been managed with diazepam and baclofen.
Muscle rigidity in SPS patients can make it difficult to position a patient for intubation [19] during general anaesthesia. Thus there is a role for neuromuscular blocking drugs. However, Johnson and Miller reported that the use of vecuronium, (a non-depolarising neuromuscular blocking drug) caused postoperative hypotonia [15]. This led to their patient requiring mechanical ventilation for 48 hours despite attempts to reverse the neuromuscular blocking drug. This complication was not observed by Obara et al. [20], Haslam & Price [19]. Haslam and Price used atracurium but did not encounter similar complications as described by Johnson and Miller. Johnson and Miller reported that the mechanism behind their patient's postoperative hypotonia was unclear but claimed that it did not occur when they performed the same procedure without neuromuscular blocking drugs. Their patient also had a past surgical history of prolonged postoperative weakness when she had her baclofen pump inserted but this was attributed to baclofen overdose [15].
This particular patient could be idiosyncratic for having very sensitive GABA-B receptors. Moreover, the dose of thiopental used in their patient was 5.8mg/kg compared to Obara et al. [20] who only administered 3mg/kg even though they used the same amount of vecuronium (8mg) in their respective patients [15,20]. The additive effect of using a higher dose of anaesthesia at induction combined with their patient's idiosyncrasy could explain the cause behind the complications that Johnson and Miller experienced.
Anti-GAD antibodies have no action at the neuromuscular junction, according to Figure 1 [14], hence, neuromuscular blocking drugs would not potentiate their effect. Obara et al. [20] confirmed that their patient achieved a 25% twitch recovery time (which was within their patient's normal range) while on vecuronium. Their patient's train-of-four (TOF) ratio (which indicates depth of neuromuscular blockade) monitored in the ulnar nerve also recovered to 100% postoperatively. This suggests that the neuromuscular junction was not affected by SPS [20]. Yamamoto et al. [26] who did not administer neuromuscular blocking drugs as they were using epidural anaesthesia in conjunction with GA, also ascertained that the neuromuscular junction was unlikely to be affected in SPS as their patient’s TOF ratio remained above 90% throughout the anaesthesia.
Ferrandis et al. [22] found that the pharmacodynamics of neuromuscular blocking drugs in SPS was not clearly described in literature. They added that the effect of neuromuscular blockers used in the cases reported by Johnson and Miller, Obara et al. [20] was neither greater nor longer lasting than normal. In contrast, Ferrandis et al. [22] reported longer response and recovery time to the TOF after the administration of a second dose of 4mg of pancuronium, before ending extracorporeal circulation for cardiac surgery. They had earlier given 8mg of pancuronium for intubation with normal response and recovery time to the TOF. Ferrandis et al. [22] claimed that extracorporeal circulation could possibly have prolonged the effect of neuromuscular blocking agents. It could also explain why their patient was mechanically ventilated for a few more hours postoperatively.
There does not appear to be any anaesthetic interactions or additional contraindications to use neuromuscular blocking agents in SPS patients. A recent case reported by Cassavaugh and Oravitz had successfully managed a patient with both depolarising and non-depolarising neuromuscular blocking agents on separate procedures with TOF monitoring [30]. The patient did not experience any postoperative complications. Careful individual monitoring of neuromuscular response in the form of TOF is more important and rocuronium/ vecuronium would be the recommended drug of choice which can be reversed promptly by sugammadex even in situations of profound neuromuscular blockade [48].
Regarding the hypotonia in Johnson and Miller's patient, Bouw et al. [21] attributed this to baclofen amplifying the gabanergic effects of volatile agents during GA. Bouw et al. [21] reported that their patient who was usually on baclofen developed muscle weakness and required mechanical ventilation for 1 hour postoperatively and suggested the 0.6-1.0% isoflurane as the cause. Similar postoperative complications were described in a patient who did not have SPS and received the same drugs [49]. Animal studies have also proved that baclofen potentiates the effects of halogenated agents [50]. Volatile anaesthetics enhance gabanergic input by extending postsynaptic inhibitory currents when GABA is released [51,52]. Since SPS patients are on baclofen for treatment, the doses of such anaesthetic agents should be adjusted. Bouw et al. [21] also confirmed on pharmacokinetic analyses that neuromuscular blocking agents and opioids did not play a role in the complications observed.
Not all reported cases had significant adverse outcomes; Cassavaugh and Oravitz did not encounter any respiratory problems with sevoflurane use [30]. Qin, Wang and Wu also reported a case of paraneoplastic SPS requiring thymectomy which did not develop any prolonged postoperative hypotonia or weakness. They attributed this mainly to the low concentration of isoflurane used (0.2-0.4%) as they used a target-controlled infusion of remifentanil and nitrous oxide for maintenance [25] . This is a useful method of minimising the concentration of volatile agents but it is not tailored to individual patients. A better strategy to overcome this was reflected in the case reported by Yamamoto et al. [26] who used the bispectral index (BIS) to monitor the minimum concentration needed. These gases may cause postoperative hypotonia when used in combination with ongoing baclofen therapy but their concentration can be kept to a minimum with BIS monitoring. This approach would allow the continued use of these agents with reduced risk of respiratory failure.
Different routes of anaesthesia may help as suggested by Yamamoto et al. [26] and Shanthanna [27] who both used epidural anaesthesia which alleviated postoperative pain effectively in their SPS patients. Adequate pre-medication is necessary to prevent spasms caused by the pain on needle insertion [26,27], although therapeutic medications for SPS such as baclofen and diazepam may be sufficient. Yamamoto et al. [26] reported that explaining epidural anaesthesia to the patient preoperatively reduces fear and anxiety which can induce SPS symptoms. Shanthanna [27] advocated that using conscious sedation would also keep the patient calm. Elkassabany et al. [23] demonstrated that somatic paravertebral blockade in their SPS patient, supplemented with conscious sedation, also prevented postoperative hypotonia. Spinal anaesthesia is an alternative but Shanthanna suggested using lower doses to reduce the risk of respiratory distress from a high spinal anaesthesia, especially in SPS patients who have rigid chest wall muscles [27]. Great care should be taken when administering spinal or epidural anaesthesia in SPS patients who have an intrathecal baclofen pump.
Lastly, another route of anaesthesia that has successfully managed a SPS patient requiring GA was total intravenous anaesthesia (TIVA). Ledowski and Russell reported that it did not lead to any postoperative hypotonia or SPS symptoms of muscle rigidity or spasms [24]. Their patient was undergoing ENT surgery and was administrated propofol with high-dose opioids which obviated the need for neuromuscular blocking drugs [24]. Yagan et al. [28] also followed a similar routine for an orthopaedic procedure without neuromuscular blocking drugs for intubation and achieved good outcomes. However, this method may not be applicable in all kinds of surgery, especially abdominal surgery.
Conclusion
SPS is a rare disease that can present challenges in anaesthesia due to its effects on the GABA pathway. While minor procedures can be performed under monitored anaesthetic care with IV sedation [29], major cases would require TIVA and RA (with or without conscious sedation) or a combination of both are possible ways to prevent postoperative hypotonia or mechanical ventilation but may not be feasible in all types of surgery. Explaining the procedure and surgery to the patient with the use of midazolam at induction can keep the patient calm and relaxed to prevent triggering any SPS symptoms. The use of propofol at induction with the regular opioids for maintenance of anaesthesia would be a suitable combination for SPS patients. Volatile gases may be safe for maintenance too. Rocuronium can also be utilised especially for difficult intubations with sugammadex at hand if necessary.
Another recommendation would also be the need for continuous monitoring of patient parameters such as TOF and BIS which aid in keeping the doses of neuromuscular blockers and volatile agents/propofol to a minimum respectively. This is particularly crucial for patients on long-term baclofen who would also require appropriate temperature regulation during surgery. Admission to ICU postoperatively would be pertinent for any major or complicated procedures to check for any respiratory or muscular complications and to regulate the readministration of preoperative doses of benzodiazepines.
The data on SPS is limited (only 150 cases from 1980 to 2005 have been described in literature [22]). Other factors to consider during anaesthesia would be comorbidities and complexity of surgery performed since it may affect choice of drugs and route. As all the case reports highlighted in this review involved a different surgery, more detailed trials would be required to confirm their findings but the incidence of this disease remains extremely low.
Acknowledgment
The authors acknowledge the valuable editorial input of Professor Ian Mackay.
References
- Moersch FP, Woltman HW (1956) Progressive fluctuating muscular rigidity and spasm (stiff-man syndrome): Report of a case and some observations in 13 other cases. Proc Staff Meet Mayo Clin 31(15): 421427.
- Goldstein JM, DiCapua D, Patwa H, et al. (2013) Stiff-Man syndrome. New Haven, CT: Yale School of Medicine; c2009-2013.
- Hadavi S, Noyce AJ, Leslie RD, Giovannoni G (2011) Stiff person syndrome. Pract Neurol 11: 272-282.
- Murinson BB (2004) Stiff-person syndrome. Neurologist 10: 131-137.
- Ropper AH, Samuels MA (2009) Adams & Victor's principles of neurology (9th edn). McGraw-Hill Medical, New York, USA.
- Levy LM, Dalakas MC, Floeter MK (1999) The stiff-person syndrome: an autoimmune disorder affecting neurotransmission of gamma- aminobutyric acid. Ann Intern Med 131(7): 522-530.
- Stoelting RK, Dierdorf SF (2002) Anesthesia and co-existing disease. (4th edn). Churchill Livingstone, Philadelphia, USA.
- Dalakas MC (1999) Clinical symptomatology of stiff-person syndrome moderator. In: Levy LM (Ed.), The stiff-person syndrome: an autoimmune disorder affecting neurotransmission of gamma- aminobutyric acid. Ann Intern Med 131: 522-30.
- Brown P, Marsden CD (1994) The stiff man and stiff man plus syndromes. J Neurol 246(8): 648-652.
- Solimena M, Folli F, Aparisi R, Pozza G, De Camilli P (1990) Autoantibodies to GABA-ergic neurons and pancreatic beta cells in stiff-man syndrome. N Engl J Med 322(22): 1555-1560.
- Solimena M, Folli F, Denis-Donini S, Comi GC, Pozza G, et al. (1988) Autoantibodies to glutamic acid decarboxylase in a patient with stiff- man syndrome, epilepsy, and type I diabetes mellitus. N Engl J Med 318(16): 1012-1020.
- Meinck HM, Ricker K, Conrad B (1984) The stiff-man syndrome: new pathophysiological aspects from abnormal exteroceptive reflexes and the response to clomipramine, clonidine, and tizanidine. J Neurol Neurosurg Psychiatry 47(3): 280-287.
- Sandbrink F, Syed NA, Fujii MD, Dalakas MC, Floeter MK (2000) Motor cortex excitability in stiff-person syndrome. Brain 123(pt 11): 22312239.
- Ali F, Rowley M, Jayakrishnan B, Teuber S, Gershwin ME, et al. (2011) Stiff-person syndrome (SPS) and anti-GAD-related CNS degenerations: Protean additions to the autoimmune central neuropathies. J Autoimmun 37(2): 79-87.
- Johnson JO, Miller KA (1995) Anesthetic implications in stiff-person syndrome. Anesth Analg 80: 612-613.
- Baker MR, Das M, Isaacs J, P Fawcett, D Bates (2005) Treatment of stiff person syndrome with rituximab. J Neurol Neurosurg Psychiatry 76(7): 999-1001.
- Kipps CM, Fung VSC, Grattan-Smith P, et al. (2005) Movement disorder emergencies. Mov Disord 20(3): 322-334.
- Levenson JL (2009) Medical aspects of catatonia. Prim psychiatry 16(3): 23-26.
- Haslam N, Price K (2002) Anaesthesia for stiff-person syndrome. Anaesthesia 57: 298-299.
- Obara M, Chinzei M, Komatsu K, et al. (2002) Anesthetic management of a patient with Stiff-person syndrome. Anaesthesia 57: 511.
- Bouw J, Leendertse K, Tijssen MA, Dzoljic M (2003) Stiff person syndrome and anesthesia: case report. Anesth Analg 97: 486-487.
- Ferrandis R, Belda J, Llau JV, Belda C, Bahamonde JA (2005) Anesthesia for cardiac surgery on a patient with stiff person syndrome. J Cardiothorac Vasc Anesth 19(3): 370-372.
- Elkassabany N, Tetzlaff JE, Argalious M (2006) Anesthetic management of a patient with stiff person syndrome. J Clin Anesth 18(3): 218-220.
- Ledowski T, Russell P (2006) Anaesthesia for stiff person syndrome: successful use of total intravenous anaesthesia. Anaesthesia 61(7): 725.
- Qin X, Wang D, Wu X (2006) Anesthetic management of a patient with stiff-person syndrome and thymoma: a case report. Chin Med J 119(11): 963-965.
- Yamamoto K, Hara K, Horishita T, Sata, T (2007) Considerations for general anesthesia combined with epidural anesthesia in a patient with stiff-person syndrome. J Anesth 21: 490-492.
- Shanthanna H (2010) Stiff man syndrome and anaesthetic considerations: successful management using combined spinal epidural anaesthesia. J Anaesth Clin Pharmacol 26(4): 547-548.
- Yagan O, Özyilmaza K, Özmadena A, , Sayin Ö, Hanci V (2016) Anesthesia in a patient with Stiff Person Syndrome Braz J Anesthesiol 66(5): 543-545.
- Sidransky MA, Tran NV, Kaye AD (2013) Anesthesia considerations in stiff person syndrome. Middle East J Anaesthesiol 22(2): 217-221.
- Cassavaugh JM, Oravitz TM (2016) Multiple anesthetics for a patient with stiff-person syndrome. J Clin Anesth 31: 197-199.
- Oliviero A, Rubio-Esteban M, Foffani G, Aguilar J, Lopez-Dolado E, et al. (2007) Effects of baclofen on temperature perception in humans. Neurosci Res 59(1): 89-92.
- Longoni B, Demontis GC, Olsen RW (1993) Enhancement of γ-aminobutyric acidA receptor function and binding by the volatile anesthetic halothane. J Pharmacol Exp Ther 266(1): 153-159.
- Carlos R, Innerarity S (1979) Effect of premedication on etomidate anesthesia. Br J Anaesth 51: 1159-1162.
- Kiyama S, Yoshikawa T (1998) Persistent intraoperative myoclonus during propofol-fentanyl anaesthesia. Can J Anaesth 45(3): 283-284.
- Dearlove JC, Dearlove OR (2002) Cortical reflex myoclonus after propofol anaesthesia. Anaesthesia 57(8): 834-835.
- Nimmaanrat S (2005) Myoclonic movements following induction of anaesthesia with propofol: a case report. J Med Assoc Thai 88(12): 1955-1957.
- Miner JR, Danahy M, Moch A, Biros M (2007) Randomized clinical trial of etomidate versus propofol for procedural sedation in the emergency department. Ann Emerg Med 49(1): 15-22.
- Guertin PA, Hounsgaard J (1999) Non-volatile general anaesthetics reduce spinal activity by suppressing plateau potentials. Neuroscience 88(2): 353-358.
- Trapani G, Altomare C, Sanna E, Biggio G (2000) Propofol in anesthesia. Mechanism of action, structure-activity relationships, and drug delivery. Curr Med Chem 7(2): 249-271.
- Hattan E, Angle MR, Chalk C (2008) Unexpected benefit of propofol in stiff-person syndrome. Neurology 70(18): 1641-1642.
- Vernino S, McEvoy K (2008) Propofol for stiff-person syndrome: learning new tricks from an old dog. Neurology 70(18): 1584-1585.
- Schwieler L, Delbro DS, Engberg G, Erhardt S (2003) The anaesthetic agent propofol interacts with GABAB-receptors: an electrophysiological study in rat. Life Sci 72(24): 2793-2801.
- Kotani Y, Shimazawa M, Yoshimura S, Iwama T, Hara H (2008) The experimental and clinical pharmacology of propofol, an anesthetic agent with neuroprotective properties. CNS Neurosci Ther 14(2): 95106.
- Yang B, Wang BF, Lai MJ, Zhang FQ, Yang XW, et al. (2011) Differential involvement of GABAA and GABAB receptors in propofol selfadministration in rats. Acta Pharmacol Sin 32(12): 1460-1465.
- Bowery NG, Doble A, Hill DR, et al. (1981) Bicuculline-insensitive GABA receptors on peripheral autoimmune nerve terminals. Eur J Pharmacol 71:53-70.
- Price GW, Wilkin GP, Turnbull MJ, Bowery NG (1984) Are baclofen- sensitive GABAB receptors present on primary afferent terminals of the spinal cord? Nature 307(5946): 71-74.
- Misgeld U, Bijak M, Jarolimek W (1995) A physiological role for GABAB receptors and the effects of baclofen in the mammalian central nervous system. Prog Neurobiol 46(4): 423-462.
- Chambers D, Paulden M, Paton F, et al. (2010) Sugammadex for the reversal of muscle relaxation in general anaesthesia: a systematic review and economic assessment. Health Technol Assess 14(39): 1-211.
- Gomar C, Carrero EJ (1994) Delayed arousal after general anesthesia associated with baclofen. Anesthesiology 81(5): 1306-1307.
- Sugimura M, Kitayama S, Morita K, et al. (2002) Effects of GABAergic agents on anesthesia induced by halothane, isoflurane and thiamylal in mice. Pharmacol Biochem Behav 72(1-2): 111-116.
- Hall A, Rowan K, Stevens R, et al. (2004) The effects of isoflurane on desensitized wild-type and a1 (S270H) y-aminobutyric acid type A receptors. Anesth Analg 98: 1297-1304.
- Nishikawa K, Harrison NL (2003) The actions of sevoflurane and desflurane on the gamma-aminobutyric acid receptor type A: Effects of TM2 mutations in the alpha and beta subunits. Anesthesiology 99(3): 678-684.






























