The Effect of Different Intrathecal Doses of Meperidine on Postoperative Pain Relief in Patients Undergoing TURP Surgery
Ebru Canakci1*, Nilay Tas1, Ozgur Yagan2, Tugce Mutlu3, Erdal Benli4 and Abdullah Cirakoglu4
1Department of Anaesthesiology and Reanimation, Ordu University, Turkey
2Department of Anaesthesiology and Reanimation, Hitit University, Turkey
3Department of Anaesthesiology and Reanimation, Giresun University, Turkey
4Department of Urological Surgery, Ordu University, Turkey
Submission: February 20, 2017; Published: April 03, 2017
*Corresponding author: Ebru Canakci, Department of Anaesthesiology and Reanimation, School of Medicine, Ordu University, Ordu, Turkey, Email: canakciebru@gmail.com
How to cite this article: Ebru C, Nilay T, Ozgur Y, Tugce M, Erdal B, Abdullah C. The Effect of Different Intrathecal Doses of Meperidine on Postoperative Pain Relief in Patients Undergoing TURP Surgery. J Anest & Inten Care Med. 2017; 2(1) : 555580. DOI: 10.19080/JAICM.2017.02.555580
Abstract
Introduction: The purpose of this study was to investigate the effect of adding different doses of meperidine to intrathecal hyperbaric bupivacaine on anesthetic characteristics and postoperative pain relief in patients undergoing elective transurethral resection of prostate (TURP) surgery.
Methods: ASA I-III 90 patients undergoing elective transurethral resection surgery with spinal anesthesia were included in this prospective, randomized, double-blinded study. Following a spinal tap, patients were randomly divided into 3 equal groups: In group B; 12.5 mg of 0.5% hyperbaric bupivacaine was given intrathecally. In BM15 and BM30 groups, meperidine with dose of 15 mg or 30 mg was added to 10 mg hyperbaric bupivacaine, respectively.
Results: The maximum sensory block level is T8 in all groups and the duration time to reach to T8 was found shortest in Group B (Compared to Group BM 30 and Group BM 15) (p = 0.029, p = 0.017 respectiveliy). In Group B, motor block level is higher and termination time of motor block is longer compared to both meperidin added groups (p = 0.019, p = 0.022). Sensory block levels of Group BM 15 and Group BM 30 were found longer compared to Group B (p = 0.004, p = 0.006 respectively) and motor block levels of theese groups were found more shorter compared to Group B (p=0,048). In BM15 and BM30 Groups, postoperative pain scores were found lower (p≤0,001) and side effects and complications were similar between theese groups.
Discussion and Conclusion: Combination of hyperbaric bupivacaine with meperidine may offers the advantage of better postoperative analgesia and it may be used as an alternative to pure hyperbaric bupivacaine solution in spinal anesthesia, for TURP surgery.
Keywords: Spinal anaesthesia; Transurethral resection of the prostate; Meperidine.
Introduction
Transurethral resection of prostate (TURP) surgery has still continued to be the gold standard among the surgical treatments applied for benign prostatic hyperplasia (BPH), today [1]. TURP operations, it is more commonly preferred compared to general anaesthesia since it allows the early diagnosis of negativities such as regional anaesthesia fluid loading, bladder perforation, and TURP Sydrome. When the local anaesthetics are used appropriately and attentively in spinal anaesthesia, they have very few side effects. [2-4] Most of the patients who underwent a TUR-P operation are in their advanced ages and have respiratory and cardiac comorbidities. Therefore, it is important for such patients to prevent hypotension, bradycardia, and respiratory distress related to spinal anaesthesia [4]. (4) In order to achieve an efficient anaesthesia for the TUR-P operation, it is required to form the block at T10 level. Insufficient anaesthesia causes additional problems for the patient. Injection of low dose opioids together with local anaesthetics in regional blocks increases the potency of analgesia [5-7].
One of postoperative pain treatment methods is intrathecal multimodal analgesia [8]. It has been shown through experimental studies that the application of analgesia before the surgical trauma may reduce post-traumatic sensitivity and secondary hyperalgesia in the spinal cord [9,10]. For this purpose, multimodal or balance analgesia occupies a significant place recently in the postoperative pain treatment [11,12]. The main purpose of postoperative pain treatment is to reduce and eliminate the discomfort, contribute to the recovery period, reduce the side effects caused by the treatment or control them efficiently and reduce the costs of the treatment. Nowadays, spinal anaesthesia has still maintained its popularity method in lower abdominal, orthopaedic, obstetric and gynaecologic surgeries, elective, emergency or ambulatory surgery [13].
Sensory block level is important for a successful spinal anaesthesia. As is known, sensory block is affected by these factors: baricity, dose, volume, concentration, and injection rate of the local anaesthetic, patient's position, barbotage, patient's characteristics (such as height, body weight, and age) and other adjuvant agents. Among these factors; the baricity of the local anaesthetic which is associated with the patient’s position is defined as the most important factor in the distribution of the local anaesthetic [14]. An undesirable hypotension is encountered as a result of the cardiovascular effect associated with the sympathetic blockage caused by the spinal anaesthesia, and this rate is reported to be 33% in a study [15]. This creates a secondary ischemia risk especially in the advanced age group with high incidence of coronary disease [16]. Considering that most of cases undergoing TURP operations are old patients with low cardiac reserves, this presents importance. Therefore, dose of the local anaesthetic used for protection from hypotension was reduced; however, this time the aimed sensory block could not be reached. Due to this problem, the aimed sensory block was tried to be reached through minimal hemodynamic exposure by providing synergistic analgesia after adding opioid into the local anaesthetic agent used intrathecally [17,18].
The purpose of this study was to investigate the effect of adding different doses of meperidine to intrathecal hyperbaric bupivacaine on anesthetic characteristics and postoperative pain relief in patients undergoing elective TURP surgery.
Materials and Methods
After receiving an ethical committee approval from Ondokuz Mayis University and written consents of patients, a total of 90 male patients between 50-80 years of age and ASA (American Society of Anesthesiologists) I-III undergone elective endoscopic TUR surgery under spinal anaesthesia were included in the study. Patients, who refused the spinal anaesthesia, with motor or sensory deficit and contraindications to spinal anesthesia such as coagulaton disorder and infection at the puncture site were excluded from the study. It was also planned to exclude the patients, who demonstrated insufficient block after the practice, whose preoperative VAS score was 4 and above, or who needed the use of additional analgesic during surgery and were required to be transferred to general anaesthesia, from the study. Preoperatively, 10ml/kg of 0.9% NaCl solution was infused to patients before spinal anaesthesia and no additional premedication was used. In the operating room, standard monitoring including non-invasive arterial pressure, electrocardiography (ECG) and pulse oximetry (SPO2) was established for all patients. Spinal anaesthesia was applied using a midline approach from the 4th-5th lumbar segment in sitting position with a 22 G Quincke type spinal needle (B Braun, Spinocan, Melsungen, Germany). Patients were divided into 3 groups randomly using a computer generated random number table: In group B (n=30); 12.5 mg of 0.5% hyperbaric bupivacaine (Bustesin® Spinal Heavy 0.5%, VEM llaf, Istanbul, Turkey) was given intrathecally.In group BM15 (n=30), 15 mg meperidine (Aldolan®, 100 mg, G.L. Pharma GmbH, Lannach, Austria) and in group BM30 (n=30), 30 mg meperidine with 10 mg of 0.5% hyperbaric was administered intrathecally. Patients' blood pressure, heart rate and oxygen saturation were monitored and recorded every 5 minutes during the operation. While sensory block level was evaluated by using pin prick test, motor block degree was assessed by using Bromage scale. (Bromage scale 0: no motor block; 1: cannot move hip, can move knees and feet; 2: cannot move knees and hip, can move feet; 3: cannot move hip, knees and feet). Disintegration of the motor block was recorded as the period that Bromage scale regressed to point 0. Sensory block's duration of reaching to T8 dermatome, the maximum sensory block level, the maximum motor block level and the duration of reaching to this level were recorded. Surgery was initiated when sensory block formed at T8 level. At the beginning of the surgery, the pain level was scored with VAS scale. After spinal anaesthesia, the decrease of the Mean Arterial Pressure (MAP) above the rate of 25% compared to the measurement before administration or the decrease of systolic blood pressure below 90mmHg considered as hypotension and 5mg iv ephedrine doses were injected in order to bring the blood pressure to normal limits. The decrease of heart apex beat under 40 beats/minute was accepted as bradycardia and atropine doses of 0.5mg were injected in order to increase the heart beat rates above 50 beats/minute. Within the period until the sensory and motor block effects of spinal anaesthesia disappeared; patients were followed up in terms of side effects such as hypotension, bradycardia, nausea, vomiting, uneasiness, and shivering; and problems such as headache, back and leg pain, loss of strength, urination and fecal incontinence until being discharged from the hospital. In the first 24 postoperative hours, VAS scores of patients were assessed for 7 times in post-operative 1st, 2nd, 4th, 6th, 12th and 24th hours with the first assessment being in the hour 0 in the recovery unit; patients who needed additional analgesic, the first minute that the need for analgesic was arisen and the total amount of analgesic used as mg were recorded. 50 mg of dexketoprofen trometamol was administered intravenously to patients who needed analgesic (Leodex 50 mg /2ml ampoules, Bilim llaf, Istanbul, Turkey). SPSS (Statistical Package for Social Sciences) for Windows 19.0 program was used to conduct statistical analyses. Regarding assessment of the data of the study; along with descriptive statistical methods (mean, Standard deviation), Oneway Anova test was used to compare parameters demonstrating normal distribution among groups for comparing quantitative data, and Tukey HDS test was used for the determination of the group that caused difference. On the other hand, Chi-Square test was used to compare qualitative data. While the presence of a difference between groups in terms of VAS was examined by using MannWhitney U-test, changes within groups were assessed by using Friedman test. Significance level was accepted as p<0.05.
Results
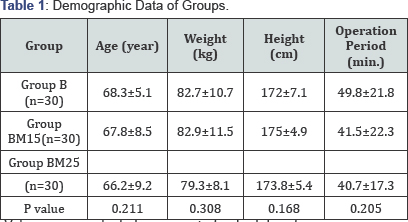
Values were evaluated as mean � standard deviation.
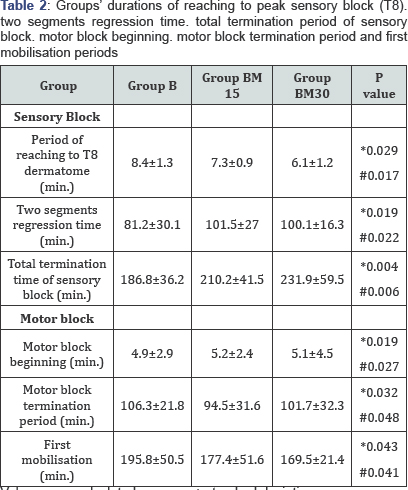
The demographic data of patients and surgery periods were found to be similar among groups. It is shown in Table 1. (p>0.05) The maximum sensory block level was T8 in all 3 groups. Sensory block’s duration of reaching to T8 dermatome and the total sensory block duration were 8.4±1.3 minute and 186.8±36.2 minute in Group B; 7.3±0.9 minute and 210.2±41.5 minute in Group BM15; and 6.1±1.2 minute and 231.9±59.5 minute in Group BM30. The durations of reaching T8 dermatome of Group B were moderate higher than Group BM15 (p=0.029) and Group BM 30 (p=0.017). Sensory block duration of Group B was lower than Group BM15 and Group BM30 (p=0.004, p=0.006; respectively). The longest sensory block duration was found in Group BM30. The sensory block duration in Group BM 15 was shorter than Group BM30 and longer than Group B (Table 2). Post-operative average VAS (Visual analogue scale) values were significantly lower in Group BM15 and Group BM30 compared to Group B in second, fourth, sixth and twelfth hours. (p< 0.001) (Table 3) VAS scores were found to be similar in all 3 groups in recovery unit (hour 0) and post-operative 1st and 24th hours (Figure 1).

**p: Comparison of Group B-Group BM15
***p: Comparison of Group B-Group Group BM 30
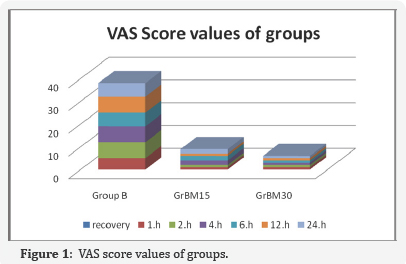
Our perioperative vital results, MAP; heart rate (HR) values,were recorded separately for all 3 groups. Measurement times of vital results were realised for 6 times with 15-minute intervals. The first measurement time was preoperative value; measurement value right after applying spinal anaesthesia was accepted as minute 0 of the operation. Following measurements were recorded as perioperative results of 0. ,15th, 30th, 45th, 60th minutes. Postoperative results were recorded as 60th, and 70th minutes in the recovery unit. Mean Arterial Pressure (MAP) was similar among the groups in all measurement times (Figure 2). Similarly, heart rate (HR) values have also been found to be similar in all measurement times among groups (Figure 3). Perioperative hemodynamic findings were observed to be more stable in the groups to which intrathecal meperidine was administered as a clinical observation in Groups BM15 and BM30. Especially after spinal anaesthesia was used, the bradycardia and hypotension appearing depending on sympathetic blockage were not observed at all in Groups BM15 and BM30. Postoperative pain scores were significantly low in terms of both statistics and clinical observation in the groups to which intrathecal meperidine was added.
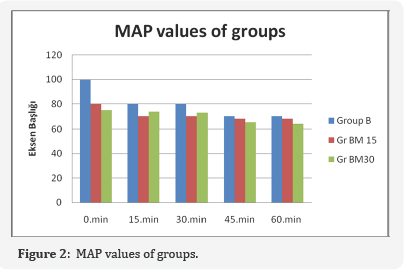

Satisfaction level was very good among all cases and surgeons in Group BM30. One surgeon reported a moderate level of satisfaction and two cases again reported a moderate level of satisfaction in Group B. One surgeon reported a moderate level of satisfaction and patient satisfaction was very good among all patients in Group BM15. Bradycardia and hypotension developed in three patients in the 13th, 16th and 21st minutes of the operation in perioperative Group B, 5 mg ephedrine i.v was administered and fast responses were received. No significant perioperative side effect was observed in other groups. Serious side effects such as nausea, vomiting, itching, and hypotension were not observed in all 3 groups in the postoperative period. Itching complication was observed in only one case in Group BM30 and itching was recovered with administration of 10 mg oral antihistaminic cetirizine. 3 patients needed additional analgesic (10%) in Group BM15 within the first 24 hours in the postoperative period; whereas, only 2 patients (6.6%) in Group BM30 and 18 patients (60%) in Group B needed additional parenteral analgesic.
Discussion
This study has revealed that meperidine added intrathecally in TURP operations ensured a significant hemodynamic stabilisation in the perioperative period and allowed the patient to feel less pain in the postoperative period and therefore ensured a comfortable postoperative period.
In a study conducted by Anaraki et al. [19] 77 cases to undergo open prostatectomy received spinal anaesthesia with hyperbaric lidocaine and half of the cases also received intrathecally 0.3mg/kg meperidine in addition to hyperbaric lidocaine. In the group with a low dose of meperidine; it was observed that there was no difference in terms of hemodynamic stability in the perioprative period; however, there were long painless periods in the postoperative period and blood loss reduced evidently [19]. The study conducted by Anaraki et al., had totally parallel results with our study, because similarly in our study, no difference was observed in terms of hemodynamic stability in groups to which a low dose of meperidine was added; whereas, these groups had a significant advantage in terms of postoperative analgesia (Table 3). In another study conducted by Patel et al. [20] 42 cases, who were planned to undergo endoscopic urological surgery, were divided into two groups; and while one group received intrathecal 0.5 mg/kg 5% lidocaine, the other group received 0.5 mg/kg meperidine intrathecally. The duration of reaching the peak sensory level was found to be significantly short in the group that received lidocaine, and when sensory block termination times and motor block beginning and motor block termination periods were compared, no difference was observed between the two groups. When compared in terms of hemodynamic stability; while the group administered with meperidine was more stabile in hemodynamic aspect, a more significant decrease was observed in mean arterial pressures in the group that received lidocaine and it was observed that there were many patients that needed intervention with intravenous ephedrine [20]. Our clinical observation results showed that hemodynamics were more stabile in groups that received meperidine; because bradycardia and hypotension developed in 3 patients in the group that received 12.5 mg hyperbaric bupivacaine were intervened with 5 mg of ephedrine i.v. In this study, the reason for not finding any significant difference in terms of hemodynamic stability may be associated with the fact that we used hyperbaric agents in all groups. In this study, no bradycardia and hypotension cases that needed intervention with ephedrine were encountered in groups where we added meperidine, because this may be related to the fact that the added meperidine increased bupivacaine baricity even more [21]. In a study conducted by Murto et al., 42 patients to undergo TUR-P operations were divided into three equal groups; one group was administered with 5% lidocaine 75 mg intrathecally, the second group received 0.15 mg /kg meperidine in addition to 75 mg of 5% lidocaine, and the third group received 0.30 mg/kg meperidine along with the same dose of lidocaine. Sensory block's duration of reaching T10 dermatome level was only found faster in the group that received lidocaine, and slower in groups administered with meperidine. In a study conducted by Chun et al., 0.2 mg /kg and 0,4 mg / kg meperidine with 8 mg of 0.5% hyperbaric bupivacaine for 25 cases to undergo TUR-P operation was reported to prevent considerably shivering, which may be a commonly encountered situation of TUR-P operations, in the postoperative period [21]. When Chun et al. [21] compared the group which received only 8 mg of 0.5% hyperbaric bupivacaine with the groups which received meperidine in terms of other side effects, it was observed that there were more itching complication in the group that received meperidine [21]. In our study, only one patient had an itching complication in group BM30, which was recovered by one oral dose of Cetirizine 10mg (Zyrtec®, 10 mg tablets, UCB Pharma, England). In a study conducted by Movafegh et al., [22] 56 patients to undergo an inguinal hernia repair received 15 mg meperidine in addition to 15mg of 0.5% hyperbaric bupivacaine intrathecally and the patients were divided into two equal groups. No premedication was given to the control group while the study group received premedication with 0.1 mg/kg i.v dexamethasone. Possible side effect profiles of the groups (nausea, vomiting, pruritus, and respiratory depression) were observed in the postoperative period. In cases premedicated with dexamethasone, all possible side effects were less observed in the postoperative period and even the patients were reported to have much higher postoperative pain scores [22]. Although it was emphasized that premedication with dexamethasone may not be reliable for every patient (particularly for the patients with diabetes); it was stated that it may have created a synergism with meperidine in the postoperative pain control [22]. In our study, no additional premedication was administered on any of the patients and no serious side effect was observed in all the groups. No respiratory depression was observed in any of 56 cases in the study conducted by Movafegh et al. [22]. Similarly in our study, no respiratory depression was observed among the cases; however when we reviewed the literature, it has been reported that isolated cases have had the respiratory depression with a dose of intrathecal meperidine above 0.5 mg/kg [23].
Comparative studies have been conducted on the elective caesarean section cases related to the use of meperidine as intrathecally isolated or in combination with local anaesthetics. In a study conducted by Kafle, 50 pregnant women who reached the last stage (mature gravida) were divided into two groups and one group received 5% meperidine intrathecally with a dose of 1mgs/kg; whereas, the other group received 5% lidocaine with a volume of 1.2-1.4 ml intrathecally. While pruritus and tendency to sleep were more commonly observed in the group to which meperidine was administered, the hypotension was more commonly encountered in the lidocaine group. The minimum postoperative painless period was 6 hours in the meperidine group; whereas, the postoperative painless period was limited with only one hour in the lidocaine group and therefore, there was a high need for analgesic in the lidocaine group [24]. Similarly, Atalay et al., [25] divided 80 pregnant women, in their term stages among elective caesarean section cases, into 4 equal groups; 10 mg hyperbaric bupivacaine was administered to the first group, 5 mg isobaric bupivacaine and 25 mg meperidine to the 2nd group, and 30 and 35 mg meperidine respectively along with 5 mg isobaric bupivacaine to the last two groups. Hemodynamic stabilities of groups in the perioperative period were noted, and their motor block levels, sensory block levels, side effects such as nausea, vomiting and itching and the Apgar scores of the newborns were compared in the postoperative period by using Bromage scale. Motor block time was found to be better in groups that received meperidine. Postoperative analgesia quality was once again found to be higher in groups that received meperidine; however, no additional benefit was reported when the group receiving 35 and 30 mg meperidine and the group receiving 25 mg meperidine as the lowest dose were compared. Additionally, the group that received a low dose of meperidine (25 mg meperidine) was emphasized to be more advantageous in terms of postoperative side effect profile compared to all groups. These results are in parallel with our study because the group BM15 achieved a postoperative analgesia quality as high as the group BM30, and did not provide any additional advantage in terms of perioperative hemodynamic stability [25]. In a study conducted by YektaŞ [26] for the purpose of intrathecal multimodal analgesia; 100 male cases to undergo inguinal hernia repair were divided into 5 groups that consisted of 20 patients and, 15 mg hyperbaric bupivacaine and 0.5 ml physiological saline solution were administered to the first group, 17.5 mg hyperbaric bupivacaine the 2nd group, 25 mcg fentanyl and 15 mg hyperbaric bupivacaine to the 3rd group, and 2.5 mcg sufentanyl to the 4th group; whereas, the last group received TIVA (Total Intravenous Anaesthesia). When the postoperative pain scores of groups were compared, they were better in the groups, which received fentanyl and sufentanyl (3rd and 4th groups) with the purpose of intrathecal multimodal analgesia, compared to all groups [26]. Similar results were obtained in our study; postoperative analgesia quality was higher in groups in which meperidine was added to intrathecal hyperbaric bupivacaine.
Consequently, low dose of meperidine added to bupivacaine by reducing the hyperbaric bupivacaine dose in TURP operations ensured more reliable hemodynamic conditions in perioperative terms and increased analgesia quality in the postoperative period. Endoscopic urologic interventions are commonly performed on the population of geriatric patients with poor cardiac reserves; therefore, the combination of a low dose of bupivacaine with a low dose of meperidine may be a good option for this patient population. At the same time; it may be an alternative option for lower extremity surgery, inguinal hernia repair, obstetrics and gynaecology for the purpose of intrathecal multimodal analgesia. In our study and in similar studies, it has been reported that the intrathecal use of a high dose of meperidine does not provide any additional advantage; nevertheless future studies are required in order to research the optimum intrathecal dose of meperidine.
References
- Gordon NS, Hadlow G, Knight E, Mohan P (1997) Transurethral resection of the prostate: Still the gold standart. Aust N Z J Surg 67(6): 354-357.
- Tucker GT, Mather LE (1998) Properties, absorption and disposition of local anesthetic agents. In: Cousins MJ. Bridenbaugh PO (Eds.), Neural Blockade in Clinical Anaesthesia and Management of Pain (3rd edn). Lippincott-Raven, Philadelphia, USA, p: 55-95.
- Collins VJ (1993) Local anesthetics. In: Principles of Anesthesiology. Lea&Febiger, Philadelphia, USA, pp. 1232-1281.
- Glaser C, Marhofer P, Zimpfer G, Heinz MT, Sitzwohl C, et al. (2002) Levobupivacaine versus racemic bupivacaine for spinal anesthesia. Anesth Analg 94(1): 194-198.
- Chung CJ, Yun SH, Hwang GB, Park JS, Chin YJ (2002) Intratecal fentanyl added to hyperbaric ropivacaine for caesarean delivery. Reg Anesth Pain Med 27(6): 600-603.
- Goel S, Bhardwaj N, Grover VK (2003) Intrathecal fentanyl added to intrathecal bupivacaine for day case surgery: a randomized study. Eur J Anaesthesiol 20(4): 294-297.
- Ben-David B, Solomon E, Levin H, Admoni H, Goldik Z (1997) Intrathecal fentanyl with small dose dilute bupivacain: better anaesthesia without prolonging recovery. Anesth Analg 85(3): 560-565.
- Staats SP, Dougherty MP (2000) Practical management of pain. In: P Prithvi Raj (Ed.), Spinal Analgesics: Present and future (3rd edn). Mosby, inc., St Louis, Missouri, USA, pp. 513-528.
- Woolf CJ (1995) Somatic pain-pathogenesis and prevention. Br J Anesth 75(2): 169-176.
- Abram SE, Winne RP (1995) Intrathecal acetylcholinesterase inhibitors produce analgesia that is synergistic with morphine and clonidine in rats. Anesth Analg 81(3): 501-507.
- Klamt JG, Garcia LV, Prado WA (1999) Analgesic and adverse effects of a low dose of intrathecally administrated hyperbaric neostigmine alone or combined with morphine in patient submitted to spinal anaesthesia pilot studies. Anaesthesia 54(1): 27-31.
- Murali Krishna T, Panda NB, Batra YK, Rajeev S (2008) Combination of low doses of intrathecal ketamine and midazolam with bupivacaine improves postoperative analgesia in orthopaedic surgery. Eur J Anesthesiol 25(4): 299-306.
- Whiteside JB, Wildsmith JAW (2005) Spinal anaesthesia: an update. Continuing Education in Anaesthesia, Critical Care & Pain 5: 37-40.
- Bernards CM (2001) Epidural and Spinal Anesthesia. In: Barash PG, et al. (4th edn), Clinical Anesthesia. Lippincott Williams & Wilkins, Philadelphia, USA, pp. 689-713.
- Martyr JW, Clark MX (2001) Hypotension in elderly patients undergoing spinal anaesthesia for repair of fractured neck of femur. A comparison of two different spinal solutions. Anaesth Intensive Care 29(5): 501-505.
- Juelsgaard P, Sand NP, Felsby S, Dalsgaard J, Jakobsen KB, et al. (1998) Perioperative myocardial ischaemia in patients undergoing surgery for fractured hip randomized to incremental spinal, single-dose spinal or general anaesthesia. Eur J Anaesthesiol 15(6): 656-663.
- Maves TJ, Gebhart GF (1992) Antinociceptive synergy between intrathecal morphine and lidocaine during visceral and somatic nociception in the rat. Anaesthesiology 76: 91-99.
- Tejwani GA, Rattan AK, McDonald JS (1992) Role of spinal opioid receptors in the antinociceptive interactions between intrathecal morphine and bupivacaine. Anesth Analg 74(5): 726-734.
- Anaraki AN, Abbasi M, Anvarypou A, Motamed N (2012) The effects of Adding Meperidine to Heavy Intrathecal Lidocaine on Hemodynamic Changes and Blood Loss in Open Prostatectomy: A Randomized Double-Blind Clinical Trial. Iran J Med Sci 37(1): 15-22.
- Patel D, Janardhan Y, Merai B, Robalino J, Shevde K (1990) Comparison of intrathecal meperidine and lidocaine in endoscopic urological procedures. Can J Anaesth 37(5): 567-570.
- Chun DH, Kil HK, Kim HJ, Park C, Chung KH (2010) Intrathecal meperidine reduces intraoperative shivering during transurethral prostatectomy in elderly patients. Korean J Anesthesiol 59(6): 389393.
- Movafegh A, Soroush AR, Navi A, Sadeghi M, Esfehani F, et al. (2007) The Effect of Intravenous Administration of Dexamethasone on Postoperative Pain, Nausea, and Vomiting After Intrathecal Injection of Meperidine. Anesth Analg 104(4): 987-989.
- Ong B, Segstro R (1994) Respiratory depression associated with meperidine spinal anaesthesia .Clinical Reports. Can J Anaesth 41(8): 725-727.
- Kafle SK (1993) Intrathecal meperidine for elective Caesarean section: a comparison with lidocaine. Can J Anaesth 40(8): 718-721.
- Atalay C, Aksoy M, Aksoy AN, Dogan N, Kürsad H (2010) Combining Intrathecal Bupivacaine and Meperidine during Caesarean Section to Prevent Spinal Anaesthesia-induced Hypotension and Other Side- effects. J Int Med Res 38(5): 1626-1636.
- Yektaç A, Belli E (2014) Intratekal Hiperbarik Bupivakaine Eklenen Farkli Adjuvan Ajanlarin ve Total Intravenöz Anestezinin, Postoperatif Analjezik Özelikler Üzerine Etkileri. ACU Saglik Bil Derg 2: 113-120.






























