Quality Indicators to Assess the End-of-Life Care in the Intensive Care Unit
Anne Kit-Hung Leung1*, Sylvia Ka-Yi Yeung2, Kitty Kam-Yuk Leung2, Kin Wah Au-Yeung1 and Kang Yiu Lai3
1Consultant Intensive Care Unit, Queen Elizabeth Hospital, Hong Kong
2Advanced Practicing Nurse, Intensive Care Unit, Queen Elizabeth Hospital, Hong Kong
3Chief of Service, Intensive Care Unit, Queen Elizabeth Hospital, Hong Kong
Submission: February 02, 2017; Published: March 06, 2017
*Corresponding author: Dr. Anne KH Leung, Consultant, Intensive Care Unit, 30 Gascoigne Road, Queen Elizabeth Hospital, Kowloon, Hong Kong SAR, Tel: [852) 35067310; Fax: (852)2388-1231; Email: leungkha@yahoo.com; leungkha@ha.org.hk
How to cite this article: Anne K-H L, Sylvia K-Y Y, Kitty K-Y L, Kin W A-Y, Kang Y L. Quality Indicators to Assess the End-of-Life Care in the Intensive Care Unit. J Anest & Inten Care Med. 2017; 1(5) : 555572. DOI: 10.19080/JAICM.2017.01.555573.
Abstract
Objectives: Intensive Care Units (ICU) in Hong Kong incorporated palliative care in the daily practice. We would like to evaluate the quality of end-of-life care (EoLC) in the ICU.
Design, setting and participants: Quality indicators consist of 4 domains and 12 indicators were devised. The four domains were early identification of dying patients; communication and information; end-of-life care to the patient and care after death. Next, we applied these indicators to assess the EoLC of patients who died in a 20-beds mixed ICU from 1st Jul to 30th Sep 2012.
Main outcome measures: The 12 EoL quality indicators
Results: Out of the 38 patient records, 33 were included for analysis. There were no objective criteria to identify dying patients. All the studied families received an EoL physician-family conference. Although high documentation rate (90.9%) of the treatment plan and resuscitation status; only 3.0% of the family conferences addressed the psychological, social and religious needs. No written information was used. Medication was prescribed in 46.7% for symptom control and life-sustaining treatments (LST) were withheld and withdrawn in 90.9% and 45.5%, respectively. In indicated patients, only 66.6% had the process reviewed. Lastly, care after death was acknowledged in 48.4%.
Conclusion: These 12 EoL quality indicators were specific designed for ICU patients and easy to implement. Areas for improvement included early identification of dying patients; training on assessment of the social, psychological and religious needs of the patient's family; distribution of information leaflets; assessment and management of symptoms; and regular review of the process.
Keywords: End-of-life issues; Intensive care; EoLC
Abbreviations: VHA: Veterans Health Administration; LCP: Liverpool Care Pathway; EoL: End of Life; LST: Life-Sustaining Treatment
Introduction
End-of-life care is an integral part of care in ICU especially when treatments fail to accomplish the original goal of treatment. Uncertainty of disease prognostication was one of the challenges in EoLC in ICU, and the decision was usually based on the number of organ failures or selected diagnosis like global cerebral ischemia after cardiac arrest [1,2]. As most critically ill patients were either sedated or unconscious, the decision making process invariably involved the patient's family. Symptom assessment and management in ventilated and sedated patients posed another challenge of EoLC in the ICU. In order not to unduly prolong the dying process, withholding or withdrawal of life-sustaining treatment (LST) usually preceded the death of patients in ICU and it varied from 0-70% [1,3,4]. In Hong Kong, the EoLC was provided by the ICU team who incorporated palliative care in the daily practice. In order to evaluate the quality of the care provided to the dying patients in the ICU, we search for quality indicators used for this particular group of patients.
In United States (US), "Care and Communication Bundle" proposed by Veterans Health Administration (VHA) had been used to assess the quality of EoLC in the ICU [2,5]. In this bundle, they used Day of ICU admission as the trigger for initiation of end-of-life discussion (Figure 1). However, this practice might not suit our local setting. In Unit Kingdom (UK), the Liverpool Care Pathway (LCP) [6] had served as the main mechanism to ensure quality of EoLC, especially in the last days of life. The LCP had 3 key sessions (initial assessment, ongoing assessment and care after death) and 4 key domains of care (Physical, psychological, social and spiritual). As LCP had attracted a lot of criticism, the Independent Review Panel recommended its use be abandoned [7]. By referring to the quality indicators used from these two countries, we try to devise a quality tool comprising of 4 domains, namely
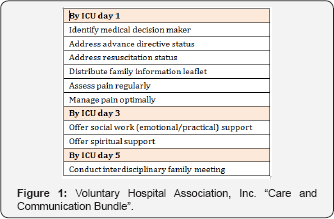

Domain One: Identification of the patients approaching end-of-life in timely manner
Domain Two: Communication and information to patient or patient's family
Domain Three: End-of-life care to the patient
Domain Four: Care after death
Under these 4 domains, there were total of 12 indicators as shown in Figure 2. We then applied these 12 indicators to assess the EoLC in a group of dying patients in the ICU.

Method
Prior Ethics Committee approval was obtained to retrieve the records of patients who died in ICU from 1st Jul to 30th Sep 2012. End of life (EoL) physician-family conference was defined as the family interview in which the ICU doctor brought up the issue of comfort care with the patient's family and the signing of the hospital DNAR (Do Not Attempt Resuscitation) form. Patients excluded from the analysis were those who had no close relatives identified; those families who refused the end-of-life care and patients with unexpected deterioration in the ICU.
The other data collected include the demographic data, the APACHE II and IV score, the SOFA score at the time of the EoL decision, the time from ICU admission to the decision of EoLC, and the time from activation of EoLC to the death of the patients.
We used these 12 indicators to assess the quality of EoLC in the ICU. Descriptive statistics were used when appropriate. The results were expressed as percentages. The denominator was all the ICU patients with EoLC in the ICU and the numerator refers to the episodes that fulfilled the criteria.
Result
A total of 38 patients died in the ICU and 5 were excluded from analysis. Three patients had unanticipated deterioration; one patient had no close relatives in Hong Kong and one family requested active treatment until the patient succumbed.
The demographic, APACHE II and IV score of the 33 patients were shown in Table 1. The median SOFA score at the time of the decision for EoLC was 35 (IQR=27-39); signifying the patients had high probability of dying at time of decision.
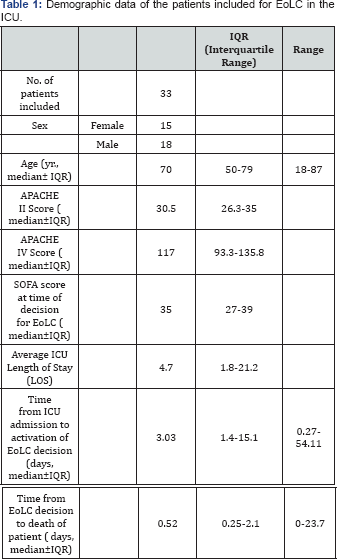
There were no objective criteria for early identification of patients approaching end-of-life. The median time from ICU admission to decision of EoLC was 3.0 days (IQR = 1.4-15.1). The median time from decision of the EoL to death of patient was short and variable (median of 0.52 days, range from 0 to 23.7 days). Although EoL physician-family interviews were provided to the family of the dying patients in the ICU, 84.8% were conducted by an ICU specialist or higher ICU trainees. There was high rate (90.9%) of documentation of the treatment plan and resuscitation status of the patients (Table2).
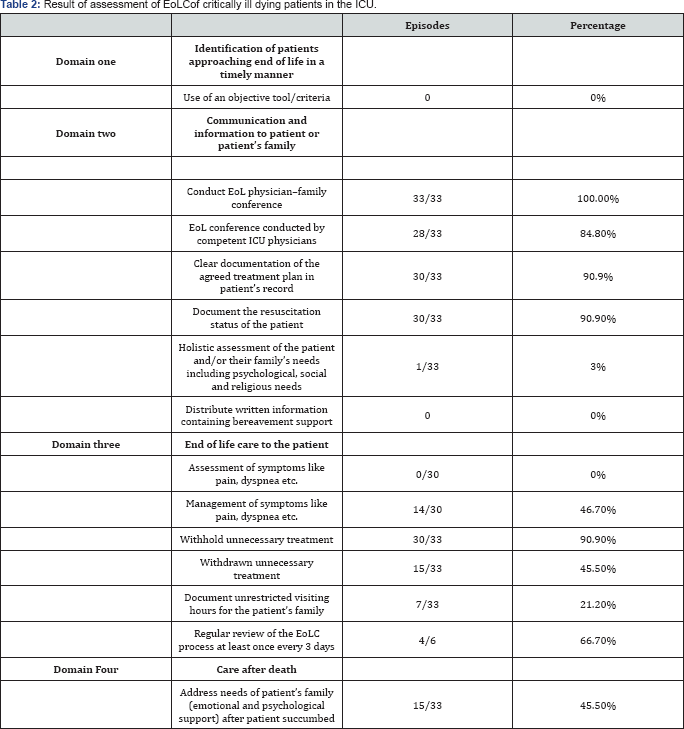
For management of symptoms, 3 patients were excluded because of severe brain injury. Out of 30 patients, 14 (46.7%) were prescribed medication for symptom control. There was no formal assessment of symptoms. Treatment were withheld in 90% of patients had and less than half (45.5%) had treatment withdrawn. Among the patients with treatment withdrawn, 5 had ventilator support decreased; 5 had inotrope decreased; 8 had stopped dialysis support and 6 had unnecessary medications stopped. Six patients survived more than 3 days after initiation of the EoLC; 4 of them (66.7%) had the process reviewed again (Table 2).
As for the patients' families; the areas that were least assessed were the psychological, social and religious needs of the patients’ families. We did not have any written information to provide to the patients' families to explain the meaning of end- of-life care. Although unrestricted visiting hours were allowed for the family, this was recorded in the documentation in 7 out of 33 EoL records. After the patient succumbed, the hospital had its own policy on last offices and handling of the deceased’s body. However, the needs of the patient's family was acknowledged in less than half of the cases (45.5%) (Table 2).
Discussion
Between the "Consultative Model" and the "Integrated Model" of palliative care service provision in the ICU [2], most Hong Kong ICUs have adopted the latter model. In a study by Yap et al, almost all ICU doctors in Hong Kong would apply the "Do-Not-Resuscitate" order; 99% and 89% of them would withhold or withdraw therapy in dying patients, respectively [8]. In general, limitation of therapy was applied when we were quite confident that the patient would die or had no chance of meaningful recovery. In order to evaluate the EoLC in the ICU, we need to identify the quality indicators that reflect the whole process of care; from identification of dying patients to care after death. Indeed, implementation of palliative care quality measures had been regarded as one of the most promising strategies to improve EoLC service [5].
In the UK before 2014, the Liverpool Care Pathway (LCP) [6] had served as the main mechanism to ensure quality of EoLC, especially in the last days of life [9]. However, there were limited experiences of using the LCP for EoLC in the critically ill patient [10] . For indicators that were specific to ICU, the Robert Wood Johnson Foundation Critical Care End-of-life Peer Workgroup proposed the use of seven domains and 53 quality indicators [11]. To facilitate the use of these indicators in daily practice, the Veterans Health Administration (VHA) developed the "Care and Communication Bundle" and narrow down to nine measures [2]. In contrast to most ICU in US,ICU admission in Hong Kong was limited by bed availability [1,8]. Hence, the use ICU stay Days 1, 3 and 5, as the trigger for EoLC might not be applicable to us. With some modification, we chose 4 basic domains and 12 indicators to assess the quality of EoLC in our local settings.
The importance of the "diagnosis of dying" has been brought up by the recent independent review of the LCP and another study [7,9,12]. In Buckley's study, instead of listing the objective criteria to identify the dying patients in the ICU, they retrospectively reported the reasons for initiating a discussion on limitation of therapy with the family [1]. In Buckley study, the mean time from ICU admission to the EoLC decision was 7.8 +/- 13 days. In our study, the median time for ICU admission to the decision for activation of EoLC was 3 days (IQR=1.4-15.1 days). Both studies shown a wide variation in the timing of bringing up the EoL discussion. The inherited uncertainty in disease trajectories and prognostication of non-malignant disease [13] has made the identification of triggering factors rather difficult in critical illness. Although there were reported triggering criteria for activation of palliative care consultation [2,14], there were no unifying objective criteria for early identification of dying patients among critically ill patients. This may lead to wide variation in the decision to activate EoLC.
After the implementation of the Care and Communication Bundle in ICUs in the US, the overall reported pain assessment and management in three ICUs had improved to 76% and 81% respectively [15]. In this current study, all the patients were intubated, rendering the assessment of pain and other symptoms more difficult. In 46.7% of indicated patients, medications were prescribed for symptom relief. Assessment of symptoms was important as some patients (e.g. those with severe brain injury) might not need medication for pain relief while those who needed them might not have the medication prescribed to meet their need. Lastly, after the start of the EoL care program, it was important to have regular reviews of the patients who survived longer than expected.
In the ICUs at US, the assessment or offering of social and spiritual support ranged from 30-61 % [15-17]. In this study, there was a scarcity of such support to patients' families both before and after the death of the patient. One study has shown that the use of a brochure on the subject of bereavement together with a proactive family conference could enable the families to feel supported and to decrease the Post-Traumatic Stress Score 3 months after the death of the patient [18]. Holistic care for the family of critically ill patients during EoLC was one of the major areas for improvement in our ICU.
The limitations of this study were it was a small retrospective case series; the indicators used were not validated in other studies; and it only reflected the perspective and practice of EoLC among the Chinese at Hong Kong. Easy to implement quality indicators were important as they might help to highlight the quality gap in EoLC in the ICU. With the use of these indicators, it helped to identify any missing links between the translation of guideline or policy into quality care to critically ill dying patients in the ICU.
References
- Buckley TA, Joynt GM, Tan PY, Cheng CA, Yap FH (2004) Limitation of life support: frequency and practice in a Hong Kong intensive care unit. Crit Care Med 32: 415-420.
- Nelson JE, Bassett R, Boss RD, Brasel KJ, Campbell ML, et al. (2010) Models for structuring a clinical initiative to enhance palliative care in the intensive care unit: a report from the IPAL-ICU Project (Improving Palliative Care in the ICU). Crit Care Med 38(9): 1765-1772.
- Cook D, Rocker G, Marshall J, Sjokvist P, Dodek P, et al. (2003) Withdrawal of mechanical ventilation in anticipation of death in the intensive care unit. N Engl J Med 349(12): 1123-1132.
- Prendergast TJ, Claessens MT, Luce JM (1998) A national survey of end-of-life care for critically ill patients. Am J Respir Crit Care Med 158(4): 1163-1167.
- Nelson JE (2006) Identifying and overcoming the barriers to high- quality palliative care in the intensive care unit. Crit Care Med 34(Suppl 11): S324-331.
- Liverpool MCPCI (2009) Marie Curie Palliative Care Institute Liverpool. The Liveroool Care Pathway for the Dying Patient (LCP)_ Core_Documentation.
- More care, Less Pathway (2013) A Review of The Liverpool Care Pathway.
- Yap HY, Joynt GM, Gomersall CD (2004) Ethical attitudes of intensive care physicians in Hong Kong: questionnaire survey. Hong Kong Med J 10: 244-250.
- Department of Health (2008) End of Life Care Strategy. Promoting high quality care for all adults at the end of life.
- Walker R, Read S (2010) The Liverpool Care Pathway in intensive care: an exploratory study of doctor and nurse perceptions. Int J Palliat Nurs 16(6): 267-273.
- Clarke EB, Curtis JR, Luce JM, Levy M, Danis M, et al. (2003) Quality indicators for end-of-life care in the intensive care unit. Crit Care Med 31(9): 2255-2262.
- Coombs M, Long T (2008) Managing a good death in critical care: can health policy help? Nurs Crit Care 13(4): 208-214.
- Murray SA, Kendall M, Boyd K, Sheikh A (2005) Illness trajectories and palliative care. BMJ 330(7498): 1007-1011.
- Bradley CT, Brasel KJ (2009) Developing guidelines that identify patients who would benefit from palliative care services in the surgical intensive care unit. Crit Care Med 37(3): 946-950.
- Penrod JD, Pronovost PJ, Livote EE, Puntillo KA, Walker AS, et al. Meeting standards of high-quality intensive care unit palliative care: clinical performance and predictors. Crit Care Med 40(4): 1105-1112.
- Curtis JR, Nielsen EL, Treece PD, Downey L, Dotolo D, et al. (2011) Effect of a quality-improvement intervention on end-of-life care in the intensive care unit: a randomized trial. Am J Respir Crit Care Med 183(3): 348-355.
- Nelson JE, Mulkerin CM, Adams LL, Pronovost PJ (2006) Improving comfort and communication in the ICU: a practical new tool for palliative care performance measurement and feedback. Qual Saf Health Care 15(4): 264-271.
- Lautrette A, Darmon M, Megarbane B, Joly LM, Chevret S, et al. (2007) A communication strategy and brochure for relatives of patients dying in the ICU. N Engl J Med 356(5): 469-478.






