An Evaluation of Medication Reconciliation and Medication Errors from Electronic Medical Records (EMR) Records in a Large Urban Family Medicine Outpatient Setting
Aulia Shariat1, Mohammad S Alzahrani2, Mary K Maneno2* and Monika Daftary2
1Pharmacist, Howard University Hospital, US
2Department of Clinical & Administrative Pharmacy Sciences, Howard University College of Pharmacy, US
Submission: November 07, 2018; Published: December 11, 2018
*Corresponding author: Mary K Maneno, Associate Professor, Department of Clinical & Administrative Pharmacy Sciences, Howard University College of Pharmacy, 2300 4th Street, NW, Washington, DC 20059
How to cite this article: Mary K M, Mohammad S A, Monika N D, Aulia S. An Evaluation of Medication Reconciliation and Medication Errors from Electronic Medical Records (EMR) Records in a Large Urban Family Medicine Outpatient Setting. Glob J Pharmaceu Sci. 2018; 6(4): 555695. DOI: 10.19080/GJPPS.2018.06.555695.
Abstract
Background: Electronic medical records (EMR) allow providers to document and maintain comprehensive medication lists for patients. Comprehensive EMR also provides medication reconciliation functionalities which can be used to identify potential medication errors.
Objectives: The objectives of the study were to determine the prevalence of medication errors by type and to determine the effect of medication reconciliation on the occurrence of any medication error in a large outpatient setting in an urban teaching hospital.
Methods: A retrospective chart review was conducted in a large family medicine outpatient clinic at an urban teaching hospital from September 1, 2015 – August 31, 2016. The primary outcome of this study was the occurrence of any medication error. Other study variables included patient socio-demographics, clinical data, current medications, and medication reconciliation. Descriptive statistics were estimated for all variables. Logistic regression analyses were used to determine the effect of medication reconciliation and other factors on the occurrence of a medication error.
Results: There were 1,000 unique patients from the EMR records included in this analysis. The prevalence of medication errors was 36.6% and that of completed medication reconciliations in the EMR was 47.7% respectively. The three most common medication error types were drug-drug interactions (202, 20.2%), errors of omission (180, 18%), and duplication of therapy (123, 12.3%). Total number of medications and (OR= 1.30 (1.24 – 1.37)) and completed medication reconciliation (0.18 (0.13 – 0.26)) were predictive factors of an occurrence of a medication error.
Conclusion: At least a third of the patients had at least one reported medication error in this study. Completed medication reconciliation can significantly reduce the potential for medication errors in an outpatient setting in this era of EMR proliferation.
Keywords: Medication; Electronic; Urban; Records; Medicine
Introduction
The adoption of electronic medical records (EMR) has allowed health care providers the ability to document clinical activity, do e-prescribing and maintain a comprehensive medication list for each patient [1]. Periodic medication reconciliation using a patient’s EMR should be done to ensure a complete, up to date and correct medication profile. Additionally, it should also be done in order to check drug-drug interaction issues, correct dosing, dosage adjustment needs, accuracy of allergy information, therapeutic duplications, and status of inactive medications.
One of the main advantages of medication reconciliation is the reduction of medication errors during the care continuum [2]. After the Health Information Technology for Economic and Clinical Health (HITECH) Act in 2009, broad EMR adoption was expected. This policy driven adoption of EMR was expected to further increase reduction of medication errors. Thus far the benefit of EMR-facilitated medication reconciliation on medication error reduction has not been comprehensively explored in the outpatient setting. Furthermore, recent reports indicate that challenges with full adoption of medication reconciliation within EMR continue to prevail [3]. These challenges may be leaving room for medication errors or discrepancies to persist. Estimates of medication errors in the post HITECH era are estimated to be between 7.6%- 39.6% in the outpatient setting [4,5]. While the National Coordinating Council for Medication Error Reporting and Prevention (NCCMERP) discourages comparison of medication error estimates across care settings and institutions, it does emphasize the need for their reduction [6,7].
Pharmacists are a critical part of the health care team and have been part of beneficial medication reconciliation interventions [8,9]. however, more formalized efforts in the implementation of pharmacist-driven medication reconciliation interventions are needed in outpatient care settings. A review of the literature points to a gap in medication error estimates from large studies in urban outpatient settings in the post HITECH era. As these care settings are likely to serve more diverse and complicated types of patients, a closer examination of patterns of medication errors is warranted to prevent further errors from occurring.
Medication reconciliation can be done using a health care team approach or dedicated team member approach using pharmacists or nurses. Presently data is lacking on the prevalence of medication errors using both approaches. To fill this knowledge gap, this study evaluated the prevalence of medication errors by type and an estimated of the effect of team-based medication reconciliation on medication errors in a large urban outpatient care setting [10].
Methods
Study Design and Setting
A retrospective chart review was conducted in a large family medicine outpatient clinic at an urban teaching hospital from September 1, 2015 – August 31, 2016. Eligibility was limited to patients aged 18 years and older who had at least one clinic visit during the study period. If a patient had multiple visits to the Family Medicine Clinic, only the first clinic visit was included within the study population. This study was approved by the Institutional Review Board at Howard University.
Sample size calculation
A sample size calculation based upon an exact test for a difference in proportion of medication errors from a constant value was done. The constant value was estimated from existing prevalence estimates in the literature. 4,5 A power of 80% and small effect size (g=0.1) was used in the calculation. Based upon this calculation our achieved sample size of 1000 was more than enough (>N=155) to find a difference.
Study Variables
The primary outcome of the study was the occurrence of a medication error. Other study variables included medication reconciliation patient socio-demographics, clinical data, and comorbid conditions.
Data Collection
A uniform data collection tool was developed to abstract information from the Family Medicine clinic electronic medical record program (Allscripts®). The collected socio-demographic data included age, gender, insurance, date of birth, race, weight, and height. Clinical data collected included documented allergies, renal function, liver function tests (AST, ALT, T. Bili, and Alk. Phos.), date of visit, comorbidities, current medications, and occurrence of medication reconciliation. All the data was collected by a single investigator, a sub sample validated by a separate investigator.
Operational Definitions
Operationally, types of medication errors were categorized as follows: incorrect dosing, renal adjustment, hepatic adjustment, duplication of therapy, incorrect frequency, drug-drug interaction, contraindication, allergy, lack of indication, and errors of omission and commission. Medication reconciliation was determined to occur at the visit reviewed, if each prescription was valid (not expired) and a complete medication record was documented to include drug name, dose, route, and frequency.
Medication errors related to renal and hepatic adjustment were identified through review of renal and hepatic function and appropriate dosing for each individual medication listed as a “current medication” in the chart. Drug interactions were evaluated using both Micromedex® and Lexicomp® and were documented if noted to be “severe” on both programs.
Statistical Analysis
Descriptive statistics, including means and proportions were used to analyze all patient characteristics and medication error types. Simple and multiple logistic regression analysis was used to examine the predictive effect of medication reconciliation and other factors on the occurrence of a medication error. Variables included in the final model included age, gender, number of medications, insurance type, comorbidities and medication reconciliation. All analyses were conducted using IBM-SPSS statistical software, version 24 at an alpha of value of 0.05.
Results
Demographic and Clinical Characteristics
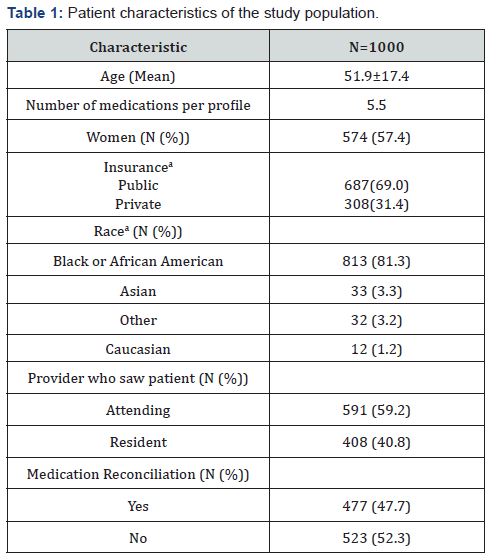
There were 5,306 patients who visited the Family Medicine Clinic from September 1, 2015 to August 31, 2016. From this eligible group, 1000 were included in for this analysis. The demographic and clinical characteristics of the study participants are presented below in (Table 1). As shown, the mean age of the study population was 51.9 ±17.4). Majority of the population were African American (81.3%) and were on public insurance (69.0%).
Medication Error Types
The overall prevalence of medication errors in this study was 36.6%. Of the records that had completed medication reconciliation, 12.8% had a medication error, while 58.3% of those that did not have completed medication had a documented medication error. A distribution of the error types is summarized on (Table 2). As shown, the most prevalent medication error type was drug-drug interactions found in 202 (20.2%) patients. Common drug-drug interactions seen in profiles were amlodipine/ simvastatin where the simvastatin dose was greater than 20 mg daily; multiple narcotic prescriptions and concomitant use of benzodiazepines (for example Oxycodone/Acetaminophen, Oxycodone, Cyclobenzaprine, Acetaminophen with Codeine, Tramadol, Diazepam, etc.)
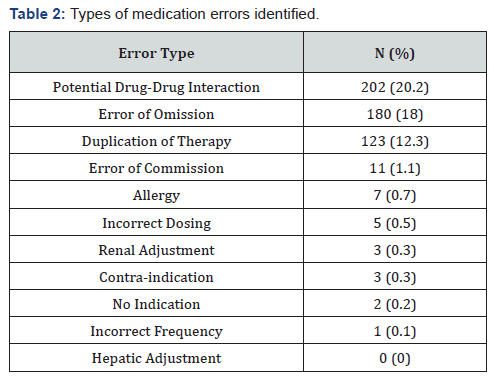
The second most common medication error identified was errors of omission, found in 180 patients (18%). These errors of omission included incomplete medication records that did not contain the full drug name, dose, route and instructions. Commonly noted prescription medications with incomplete regimens were “Proair AERS HFA” that did not contain common instructions such as “take 1 – 2 puffs Q4-6 H PRN” or Insulin prescriptions with instructions written, “as directed”. Over the counter medications did not always have a complete record and examples included: Advil Jr., Prilosec OTC, or Vitamin B6 tabs. The third most common medication error type identified was duplication of therapy, found in 123 patients (12.3%). This was seen in current medication profiles containing two medications in the same drug class or a medication that was prescribed with two different dosages or instructions. Commonly observed errors related to duplication of therapy included Gabapentin 300 mg TID vs. 400 mg TID, two proton-pump inhibitors listed (i.e. omeprazole and lansoprazole), or Viagra and Cialis both appearing on the current medication list (Table 2).
Predictors of the occurrence of medication errors
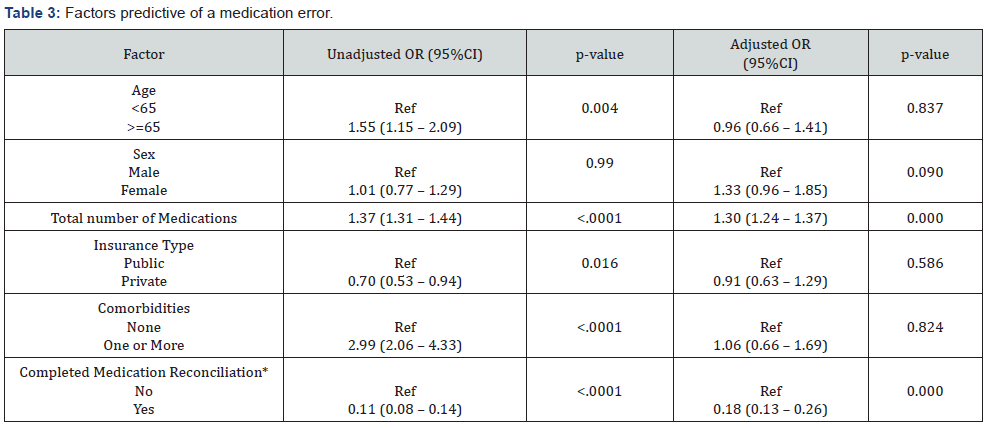
Predictive factors of medication errors are summarized in (Table 3). The significant predictors in the bivariable analysis were age, total number of medications, insurance type, comorbidities, and medication reconciliation (p< 0.05). The adjusted multivariable model showed that total number of medications and medication reconciliation remained significant predictors of medication errors occurrence (Table 3). The findings showed that for each additional medication a patient was taking, the odds of medication errors increased (adjusted OR=1.30 [95%CI: 1.24 – 1.37]). Also, the study found that profiles that were reconciled were less likely to have medication errors compared to profiles that were not reconciled (adjusted OR=0.18 [95%CI: 0.13 – 0.26]).
Discussion
This study evaluated the prevalence of medication errors in a large outpatient care setting in an urban teaching hospital. Nearly 1 in 3 patients included in the study was associated with at least one medication error. Other outpatient settings in the EMR proliferation era have estimated medication error rates from 7.6%- 39.6% 4,5 Since estimate comparison is unsuitable because varying definitions of medication errors, differences in safety culture and variations in patient population served,6 direct comparison with literature estimates will not be done. Instead, this discussion will focus on the potential for harm reduction that these estimates point to.
According to NCCMERP, there is no ideal medication error estimate and all efforts should be focused on reducing whatever estimates are obtained to improve patient outcomes.6 In conducting this study, the investigators chose not to distinguish between errors that reached the patient or those that did not reach the patient in order to get a more comprehensive perspective on the prevalence of medication errors. This study findings point to a need to further reduce medication errors in this care setting. Based upon these findings our study shows a significant potential to reduce the occurrence of medication errors in similar urban outpatient care settings and a need to seek dedicated involvement of a pharmacists to facilitate this process.
Of the types of medication errors reported, potential drugdrug interactions, errors of omission, and duplication of therapy were the most common. Other studies in the outpatient setting have noted slightly different findings. A study in an outpatient academic family medicine clinic in Oklahoma identified common prescribing errors as incomplete/inadequate prescription, dosing outside recommended guideline, and drug selection errors in an outpatient academic family medicine clinic in Oklahoma [4].
Explanations for our findings on the high prevalence of potential drug-drug interactions, and duplication of therapy could be attributed to the lack of consistent medication reconciliation conducted at patient visits. In this scenario updating of current medication lists may have led to capturing of artefactual versus actual drug-drug interactions, and duplication of therapy errors. These findings again point to the need to have a dedicated pharmacist with the time and expertise to ensure that the medication lists are appropriately updated. Findings related to less than optimal medication reconciliation also potentially point out to a lack of training on how to execute these functions in the EMR. Literature evidence points to a resistance and lag to fully use EMR among providers.3 Based upon these findings future solutions could include additional efforts in the EMR training for incoming residents, attending physicians and the rest of the health care team. Such training could include efficient updating of medication lists, use of the drug-drug interaction clinical decision support tools to identify potential drug-drug interactions at the time a new prescription is being added to the list.
Limitations
There were several limitations that should be pointed out in this study. First the reliance on the chart notes documented within the EMR was retrospective. As such some medication errors may have been corrected but not documented in the EMR. Similarly, labs that were out of date may not have reflected the true renal or hepatic function for a patient when it came to classify renal dosing errors. Secondly as an outpatient clinic in a teaching hospital, there could have been possible inconsistencies in documentation and medication reconciliation efforts between different providers. Further explained differences in medication reconciliation efforts between multiple residents (years of practice) as well as attending physicians could have occurred. Thirdly, this study did not interview patients or the pharmacy to determine the most current and accurate list of medications taken. As such there could be the possibility of over-estimation on the number of medications per patient profile and drug-drug interactions. Fourthly this study only examined first patient visit of the year and so our estimates should be examined in this context.
Conclusion
Through this analysis, there appears to be a need for a multipronged approach to reduction of medication errors in outpatient care settings. First the addition of a dedicated pharmacist or other health care provider on-site to provide medication reconciliation and interventions during clinic visits would aid in the reduction of the medication errors reported. Secondly this evaluation points to persisting gaps in the use of EMR for clinical decision support and use of medication reconciliation functionalities in the post EMR proliferation era. Future studies could continue to explore whether full use of these functionalities can aid reduce the gap in medication errors.
Acknowledgement
This project was supported (in part) by the National Institute on Minority Health and Health Disparities of the National Institutes of Health under Award Number G12MD007597. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Conflict of Interest
The authors certify that there is no conflict of interest with any organization regarding the material discussed in this manuscript.
References
- Orrico, Kathleen B (2008) Sources and Types of Discrepancies Between Electronic Medical Records and Actual Outpatient Medication Use. J Manag Care Spec Pharm 14(7): 626-631.
- Geurts MM, Talsma J, Brouwers JR, De Gier JJ (2012) Medication review and reconciliation with cooperation between pharmacist and general practitioner and the benefit for the patient: a systematic review. Br J Clin Pharmacol 74(1): 16-33
- Grossman JM, Gourevitch R, Cross DA (2014) Hospital Experiences Using Electronic Health Records to Support Medication Reconciliation. National Institute for Health Care Reform Research Brief Number 17.
- Winder, Marquita B (2015) “The Impact of Pharmacist-led Educational and Error Notification Interventions on Prescribing Errors in a Family Medicine Clinic.” J Am Pharm Assoc. 55(3): 238–245.
- Kuo GM, Touchette DR, Marinac JS (2013) Drug errors and related interventions reported by United States clinical pharmacists: the American College of Clinical Pharmacy practice-based research network medication error detection, amelioration and prevention study. Pharmacotherapy 33(3): 253-265.
- NCCMERP (2008) Statement on Medication Error Rates.
- Coletti DJ, Stephanou H, Mazzola N, Conigliaro J, Gottridge J, et al. (2015) Patterns and predictors of medication discrepancies in primary care. J Eval Clin Pract 21(5): 831-839.
- Andrus, MR., Anthony D. Anderson (2015) A Retrospective Review of Student Pharmacist Medication Reconciliation Activities in an Outpatient Family Medicine Center. Pharmacy Practice 13(1): 518.
- Philbrick, Ann M, Ila M Harris, Jon C Schommer, Christopher J, et al. (2015) Medication Discrepancies Associated with Subsequent Pharmacist-Performed Medication Reconciliations in an Ambulatory Clinic. J Am Pharm Assoc 55(1): 77–80.
- ASHP Statement on the Pharmacist’s Role in Medication Reconciliation (2016) Medication Therapy and Patient Care: Specific Practice Areas – Statements. N.p. n.d.






























