Abstract
Human bite injuries to the face pose significant challenges due to high infection risk, tissue loss, and aesthetic and functional concerns. The polymicrobial nature of human oral flora predisposes these wounds to complications such as cellulitis and abscess formation. A 34-year-old Middle Eastern male presented with nasal tissue loss after being bitten by a mentally unstable relative. The amputated tissue was chewed, destroyed, and spat out, rendering replantation impossible. Although no systemic infection was evident on admission, wound culture later grew Staphylococcus aureus. Hospitalization and delayed reconstruction were advised; however, the patient declined surgical intervention due to psychosocial concerns and fear of visible scarring. Therefore, conservative management was implemented, including meticulous wound care, prophylactic broad-spectrum antibiotics, and close outpatient follow-up. The wound healed satisfactorily without major complications. This case underscores the importance of individualized, patient-centered decision-making in managing facial bite injuries.
Keywords:Human bite injury; Nasal trauma; Facial reconstruction; Infection
Introduction
Bite injuries are most commonly caused by mammals and account for approximately 1% of emergency department visits [1]. Dog bites are the most frequent, followed by cat bites, while human bites constitute nearly 3% of all cases [2]. Notably, up to 57% of bite injuries involve the facial region [1,2]. Because the nose is the most protruding facial structure, it is particularly vulnerable to bite-related trauma. Avulsion and crush injuries, especially when associated with necrosis and tissue loss, may result in severe functional and aesthetic consequences. The primary goals of nasal reconstruction include restoration of normal anatomy, preservation of airway patency, and achievement of acceptable cosmetic outcomes. Nasal amputations caused by human, dog, and even donkey bites have been reported in the literature [1,3]. This report presents a rare case of nasal tip and ala tissue loss caused by a human bite inflicted by a mentally impaired relative, in which immediate reconstruction was not feasible due to severe tissue destruction.
Case Report
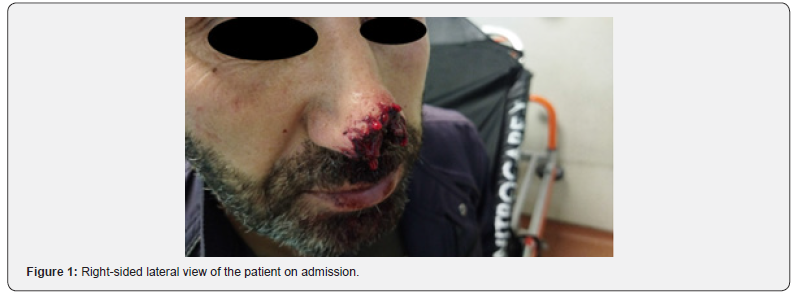
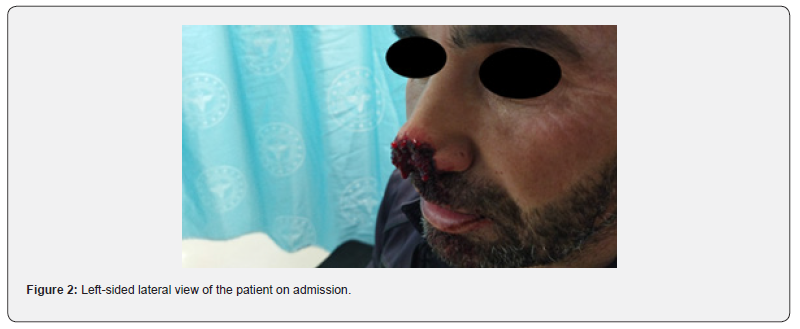
A 34-year-old male with no known comorbidities or regular medication use presented to the emergency department with an actively bleeding nasal tissue defect. He was conscious, and vital signs were within normal limits. The medical history revealed that approximately 30 minutes prior to admission, he had been suddenly bitten on the nose while playing with his mentally impaired relative. Initial management included copious irrigation of the wound with saline solution. No foreign bodies or tooth fragments were identified. Hemostasis was achieved with local pressure. Physical examination demonstrated full-thickness skin loss and partial loss of the lower lateral cartilage involving the nasal tip and right ala, resulting in an approximately 4 × 3 cm soft tissue defect. According to the Rueff classification, the injury was classified as Grade 2 [4]. There were no signs of epistaxis or nasal bone fracture. The patient’s initial clinical appearance is shown in Figure 1 & 2.
After confirmation that the relative had no known infectious diseases, rabies and tetanus prophylaxis were administered. Empiric oral amoxicillin–clavulanate (2 × 1000mg/day) and anti-inflammatory treatment were initiated following infectious disease consultation. A wound culture sample was obtained. The patient was referred to the Department of Plastic, Reconstructive and Aesthetic Surgery for further evaluation. Upon inquiry, the patient reported that the amputated nasal tissue had been chewed, destroyed, and spat out, rendering replantation impossible. Hospitalization and delayed reconstruction were recommended; however, the patient declined further intervention, citing psychosocial concerns and unwillingness to pursue legal action against his relative. After local wound dressing was applied, the patient was discharged with oral antibiotic therapy and close outpatient follow-up. Subsequent wound culture revealed Staphylococcus aureus. Written and verbal informed consent was obtained.
Discussion
Human bite injuries are generally classified into closed fist injuries and occlusive bite injuries [2,5]. Closed fist injuries most commonly affect the hand, whereas occlusive bites frequently result in avulsion-type wounds due to soft tissue entrapment between the teeth. Although approximately 15% of bite injuries involve the face, the ear and nose are particularly susceptible because of their protruding anatomy [5]. In nasal trauma, the distal one-third of the nose is most commonly affected, with frequent involvement of the tip, columella, and alar regions, often leading to loss of nasal projection [1,2,6]. The nasal ala represents a particularly challenging reconstructive unit due to its complex composition of skin, cartilage, fibrofatty tissue, and internal mucosa, all of which are essential for maintaining nasal valve function [6]. Reconstructive options for nasal tip and ala defects include nasolabial, Melo labial, and forehead flaps. Nasolabial and Melo labial flaps are generally preferred for smaller defects, whereas the forehead flap remains the optimal choice for larger or composite defects due to its reliable vascularity, tissue availability, and excellent color and texture match [2,3]. However, the forehead flap typically requires multiple surgical stages and may result in donor-site scarring.
For alar defects smaller than 1.5 cm, composite grafts harvested from the ear may be considered. Skin grafts, rhomboid flaps, and bilobed flaps are additional options for selected nasal tip defects. In cases of total nasal tip and ala amputation, microsurgical replantation may provide the best aesthetic outcome, although it is technically demanding and requires significant expertise [7,8]. In the present case, delayed reconstruction with a forehead flap was considered the most appropriate option; however, patient refusal precluded surgical intervention. Human oral flora is polymicrobial, with saliva bacterial concentrations reaching up to 10⁸/mL, significantly increasing the risk of infection in bite wounds [5]. Commonly isolated pathogens include viridans streptococci, Staphylococcus species, and Eike Nella corrodens, the latter being characteristic of human bite injuries [9,10]. Viral transmission, including herpes simplex virus, hepatitis B and C, tetanus, rabies, and HIV, has also been reported [5,9,10]. Therefore, all bite wounds should undergo thorough irrigation with saline and antiseptic cleansing. Debridement of devitalized tissue should be performed cautiously, particularly in the head and neck region. Rabies and tetanus prophylaxis, along with empiric broad-spectrum antibiotics, are mandatory. Wound cultures should be obtained, and antibiotic therapy should be adjusted accordingly. In cases with abscess formation, treatment duration may be extended up to two weeks [5]. In this patient, prolonged exposure of the amputated tissue to saliva rendered it unsuitable for replantation.
The timing of facial wound repair after human bites remains controversial. Delayed presentation-typically 6 to 12 hours after injury-increases infection risk [2]. Despite the relatively rich vascular supply of the face, primary closure is not recommended in the presence of infection, edema, necrosis, or gross contamination. In selected clean wounds with minimal contamination, early reconstruction may be successful. However, delayed reconstruction is generally preferred when cartilage grafting is required or when infection risk is high [5,8]. Although this case occurred in southeastern Turkey, similar injuries are encountered worldwide, particularly in developing regions where delays in presentation and limited access to specialized reconstructive care are common. Increased awareness of appropriate initial management and timely referral for delayed reconstruction is crucial in such settings. Human bite injuries to the face can result in significant aesthetic, functional, and psychological morbidity, with reported infection rates of up to 20–25% [5,9]. Due to tissue loss, contamination, and complex facial anatomy, management remains challenging. While early repair may be appropriate in selected low-risk cases, delayed reconstruction-most commonly with forehead flap-remains the gold standard in high-risk patients. Infection continues to be the leading cause of reconstructive failure and must be carefully considered in treatment planning [2,10].
References
- Shipkov CD (2004) Nasal amputation due to donkey bite: immediate and late reconstruction with a forehead flap. Injury extra 35(11): 85-90.
- Singh K, Aggarwal K (2023) Human Bites Over Nose: Management and Reconstruction. Archives of Plastic Surgery 50(02): 171-176.
- Bahadirli N, Bahadirli S, Keskin M (2019) Nasal Tip Avulsion due to Dog Bite. Turkish Journal of Plastic Surgery 27(4): 220-221.
- Rueff F, Bedacht R, Schury G (1967) Bite Wounds. Journal of Trauma and Acute Care Surgery 7(5): 803.
- Stathopoulos P, Ameerally P (2020) Reconstructing the nasal tip after a human bite: a challenge for the reconstructive surgeon. J Maxillofac Oral Surg 19(1): 17-20.
- Corradino B, Di Lorenzo S, Cascino AP (2023) Chondro-Cutaneous Autograft for Reconstruction of the Nasal Ala After a Human Bite. Am J Case Rep 24: e939242-1.
- Stillaert F, Roche N, Zeltzer A, Monstrey S (2012) Artery only microanastomosis in nose replantation: a report of two cases. Journal of plastic, reconstructive & aesthetic surgery 65(4): 513-516.
- Yim Y, Kwan H, Oh DY, Lee JY, Jung S-N (2005) Replantation of Nose Amputation by Use of Medical Leech. Archives of Plastic Surgery 32(1): 124-130.
- Griego RD, Rosen T, Orengo IF, Wolf JE (1995) Dog, cat, and human bites: a review. Journal of the American Academy of Dermatology 33(6): 1019-1029.
- Rothe K, Tsokos M, Handrick W (2015) Animal and human bite wounds. Deutsches Ärzteblatt International 112(25): 433.





























