Isolated Submandibular Gland Enlargement as A Sole Presentation of Mumps: A Case Report
Abdul Ahad Wani, Sharik Mehraj, Junaid Altaf and Aamir Shafi*
Department of General Medicine, Skims Medical College, India
Submission: December 21, 2023; Published: January 26, 2024
*Corresponding author: Aamir Shafi Registrar Department of General Medicine Skims Mch Srinagar Jammu and Kashmir India
How to cite this article: Abdul Ahad Wani, Sharik Mehraj, Junaid Altaf and Aamir Shafi*. Isolated Submandibular Gland Enlargement as A Sole Presentation of Mumps: A Case Report. Glob J Oto, 2024; 26 (4): 556191. DOI: 10.19080/GJO.2024.26.556191
Abstract
Mumps is a common viral infection caused by a paramyxovirus that presents with painful swelling of salivary glands. In almost all cases there occurs enlargement of parotid glands with some percentage of patients having simultaneous enlargement of parotid as well as submandibular glands. We report a case of isolated submandibular gland enlargement as a sole presentation of mumps of which very few cases have been reported in literature. The condition needs urgent attention in view of associated laryngeal edema which can be life threatening at times.
Keywords: Mumps; Submandibular gland; Viral infection; Paramyxovirus, Swellings
Introduction
Mumps is a common viral infection caused by a paramyxovirus that presents with painful swelling of salivary glands. The most prevalent symptom parotid gland enlargements are seen in 95% of cases and is typically bilateral in 90% of cases [1]. In 11% of the cases simultaneous enlargement of both the submandibular and parotid glands is seen [2]. The submandibular glands rarely have isolated involvement [3,4]. The same way that colds and the flu are transmitted, mumps is spread by infectious saliva droplets that can be breathed or picked up from surfaces and put into the mouth or nose. A person is most contagious in the first few days prior to the onset of symptoms and in the few days after the symptom onset.
Mumps can frequently cause a number of issues. Although they can be concerning these are rarely dangerous and often get better as the infection settles down. Swollen testicles (orchitis), swollen ovaries, viral meningitis and pancreatitis are common complications. Mumps can also cause uncommon complications like encephalitis and hearing loss. Submandibular gland swelling should be taken into consideration as a diagnosis of mumps in the absence of typical parotid gland swelling. Submandibular gland mumps is associated with laryngeal edema which is a life-threatening condition if not anticipated and treated in time [5]. Here we report a rare case of mumps with bilateral submandibular gland enlargement.
Case Presentation
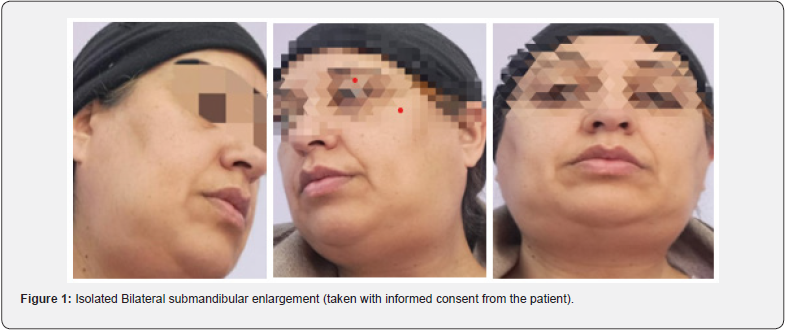
A 55 year-old female otherwise previously healthy with no co-morbidities presented acutely with a high grade fever and bilateral submandibular firm to hard swellings with altered taste and reduced salivary secretions which resulted in dry mouth. On examination there was no parotid, tonsillar or submental swelling with no sore throat and lymphadenopathy. There was no prior history of coryza or prodromal symptoms. On clinical assessment she had a tender, widespread swelling in the submandibular region on both sides with no obvious abnormality of palate or oral cavity (Figure 1). She had tachycardia of 118 beats per minute and a fever of 38.7°C rest all other clinical findings were within normal range. The results of the serology revealed neutrophilic leukocytosis with counts of 12.1/microlitre and an elevated C reactive protein measuring 33mg/L (reference range <5mg/L).
Although autoimmune markers were negative, IgG for the mumps was raised at 29.10 AU/ml (<9 AU/ml) confirming an infection although IgM was within normal range at 0.26 AU/ml (<0.9 AU/ml. Salivary volume was decreased despite the Shirmer test being negative. Mumps RT-PCR could not be done due to non availability in hospital laboratory. An ultrasound scan revealed swelling and inflammation of the submandibular glands on both sides; the parotid glands were found to be normal. To rule out a deep space abscess a CT scan with contrast was ordered which confirmed the presence of a bilateral submandibular salivary gland enlargement with normal parotid glands.
Treatment
Treatment was initiated with good oral fluids, antipyretics and adequate analgesia. Antivirals were not given in view of no well defined role. An advice regarding good oral hygiene was given and Submandibular gland size reduced to normal s in 3 weeks with return of taste sensation and saliva volume to normal in 6 weeks.
Discussion
Around 40% to 85% of people with mumps experience parotid gland inflammation [6,7]. Clinical diagnosis can be made based on parotid swelling however this feature is not present in all cases of mumps. Worldwide it peaks in Late winter or early spring although sporadic outbreaks are Common in any time of the year. Most commonly seen in school going children and less common in adults especially after vaccination [8]. Meningitis, encephalitis, orchitis in post pubertal males, pancreatitis and pericarditis are some of the complications associated with mumps infection [6,9]. However, by making sure that these individuals receive booster shots, the spread of the virus can be curbed. Although the vaccine is very effective unfortunately it does not always provide complete immunity [10].
The virus has an incubation period of 12 to 24 days and the most noticeable symptom is typically swelling of the salivary glands which peaks in 48 hours and goes away in 3 to 7 days [6,9]. The mumps infection is often self-limiting although patients may need supportive or more targeted therapy if the symptoms are extremely bothersome or if there are any secondary complications [6].To diagnose mumps infection elevated IgM and IgG antibodies are required [11].The diagnosis is supported by the characteristic clinical signs in the form of parotitis or other swollen salivary glands, orchitis, oophoritis or relevant epidemiological exposure [12]. The diagnosis could be made using:
A) RT-PCR analysis of serum or oral swabs for the presence of mumps virus RNA. It is possible to use the same specimen for viral culture.
B) Positive mumps immunoglobulins IgM (positive for up to 4 weeks) performed on oral swab particularly after parotid massage and sample taken near Stensons duct. Regardless of when the samples was collected 50% of vaccine cases tested negative for IgM. In circumstances where a patient was immunized RT-PCR results could be falsely negative.
A case study in Korea reported a young adult male with isolated bilateral submandibular gland involvement with subsequent orchitis and meningitis [7]. Another case described mumps with simultaneous parotid and submandibular gland enlargement which was later on diagnosed as lymphoma [9]. These studies are helpful for doctors to be vigilant and lookout for unusual submandibular swellings. Isolated submandibular gland mumps is rare and is seen in 10% of cases of mumps and usually associated with laryngeal edema which if not anticipated in time and treated in time may prove life threatening for the patient.
Conclusion
After reviewing the cases and the literature on this viral illness a conclusion was made that mumps should be suspected even when isolated submandibular gland enlargement occurs without the usual parotid gland swelling that is consistent with mumps.
References
- Gupta RK, Best J, MacMahon E (2005) Mumps and the UK epidemic 2005. BMJ 330(7500): 1132-1135.
- Ishida M, Fushiki H, Morijiri M, Maruyama M, Motoshima H, et al. (2006) Mumps virus infection in adults: three cases of supraglotticedema. Laryngoscope 116(12): 2221-2223.
- Cheung L, Henderson AH, Banfield G, Carswell A (2017) Bilateral isolated submandibular gland mumps. BMJ Case Rep 2017: bcr-2017-220103.
- Moulin G, Andre P, Chagnaud C, Cheynet F, Harle JR, et al. (1993) Extravasation of salivary secretions and mumps infection of the submandibular gland. Eur J Radiol 17(3): 195-197.
- M Ohki, Y Baba, S Kikuchi, A Ohata, T Tsutsumi, et al. (2015) Potentially lethal pharryngeo laryngeal edema with dyspnea in adult patients with mumps: a case series of 5 cases. Ear Nose Throat J 94(4-5): 184-186.
- Lalwani A Current diagnosis & treatment: otolaryngology head and neck surgery. 3rdedn: McGraw-Hill Lange 2011: 1-1008.
- Myung NS, Kim YJ, Kim YJ, Soo KK (2013) Complicated mumps viral infection: an unusual presentation affecting only submandibular gland. Am J Otolaryngol 34(5): 600-602.
- Center for disease control and prevention. Mumps cases and outbreaks.
- Cole AS, Trotter MI, O’Connell J (2007) Follicular lymphoma presenting as mumps, with persistent cervical lymphadenopathy. J LaryngolOtol 121(5): 501-502.
- Centers for Disease Control and Prevention, United States Department of Health & Human Services. Mumps vaccination. 2016.
- Linder TE, Brestel R, Schlegel C (1996) Mumps virus infection: case report of an unusual head and neck manifestation. Am J Otolaryngol 17(6): 420-423.
- Center for disease control and prevention. Manual for surveillance of vaccine preventable diseases Chapter 9 Mumps.





























