Comparison of Quality-of-Life Changes in Otoplasty Patients of Y and Z Generations using the GBI
Ahmet Hamdi Kepekçi1,2*
1Istanbul Yeni Yuzyil University Health Vocational School, Division of Audiometry, Turkey
2Meltem Hospital, Department of Otolaryngology, Turkey
Submission: November 10, 2023; Published: January 19, 2024
*Corresponding author: Ahmet Hamdi Kepekçi, Istanbul Yeni Yuzyil University Health Vocational School, Division of Audiometry and Meltem Hospital, Department of Otolaryngology, Istanbul, Turkey
How to cite this article: Ahmet Hamdi K. Comparison of Quality-of-Life Changes in Otoplasty Patients of Y and Z Generations using the GBI. Glob J Oto, 2024; 26 (3): 556190. DOI: 10.19080/GJO.2024.26.556190
Abstract
Objective: There is a lack of data regarding the impact of otoplasty on health-related quality of life in individuals of the prominent Y and Z generations. This study aimed to investigate the differences in health-related quality of life outcomes between generations in otoplasty patients.
Study Design: Case series with planned chart review.
Setting: Single-center study at Meltem Hospital
Methods: In this retrospective study, patient files of otoplasty cases in the Meltem Hospital database between January 2018 and May 2023 were reviewed. A total of 88 patients, including 46 males and 42 females, were included in the study. Of these patients, 55 belonged to the Y generation, while 33 belonged to the Z generation.
Results: The average Glasgow Benefit Inventory scores were significantly higher for the Z generation than the Y generation (p=0.010). Although the Z generation exhibited higher average benefit scores than the Y generation in the General Benefit subscale, the difference was not statistically significant (p=0.132). For the Physical Benefit and Social Benefit subscales, participants from the Z generation had significantly higher average benefit scores compared to those from the Y generation (p<0.001, p=0.040).
Conclusion: According to the analyses, statistically significant differences were observed in Glasgow Benefit Inventory scores between Y and Z generation otoplasty patients. Patients from the Z generation achieved more positive outcomes following otoplasty. It was observed that patients from the Z generation were more satisfied after the surgery, and otoplasty operations performed at a younger age expedited the return to social life.
Keywords: Average benefit scores; Generation otoplasty patients; Otoplasty operations; Prominent ears; Linear regression
Abbreviations: GBI: Glasgow Benefit Inventory; OB: Overall Benefit subscale; SB: Social Benefit subscale; PB: Physical Benefit subscale; FF: Facial Function
Introduction
Prominent ears are a common congenital ear deformity observed in approximately 5% of the Caucasian population. This deformity follows an autosomal dominant inheritance pattern and can affect both genders equally [1]. Prominent ears are generally considered a mild deformity without significant physiological disadvantages [2]. However, there is limited information available regarding the impact of this condition on an individual's health-related quality of life. Otoplasty can be highly effective in correcting prominent ears. Otoplasty aims to restore the normal shape and position of prominent ears. However, there is limited information available regarding the impact of this surgery on health-related quality of life. Health-related quality of life encompasses a multidimensional concept, including physical, psychological, and social aspects of health.
The aesthetic changes caused by prominent ears can lead to decreased self-esteem, increased anxiety, behavioral issues, and social avoidance [3]. Moreover, the problems associated with prominent ears can result in decreased productivity at work and missed days of work [4]. Prominent ears have the potential to become a subject of ridicule and cause significant emotional distress. Studies have shown that such cosmetic deformities can serve as strong motivating factors for individuals to seek cosmetic surgery due to dissatisfaction with their body image [5-7]. Each generation is generally defined by collective perspectives largely influenced by social changes, economic conditions, and historical developments [8]. With the widespread adoption of technology, the Y and Z generations have learned to multitask using technology while engaging in other activities [9]. Due to growing up with the digital world, the Y and Z generations have been referred to as "Digital Natives."
The Glasgow Benefit Inventory (GBI) is a commonly used patient-reported outcome measure for assessing the benefits of otolaryngological surgery and treatment [10]. GBI is widely accepted in the field of otolaryngology [11]. Linear regression not only tests relationships but also quantifies the direction and strength of these relationships. The regression coefficient defines the average (expected) change in the dependent variable for each unit change in a continuous independent variable [12]. In this study, we compared the quality-of-life changes in the Y and Z generations following otoplasty surgery using the GBI, which is widely used in the field of otorhinolaryngology.
Materials and Methods
Study Design
This retrospective observational study received approval from the Meltem Hospital local ethics committee (Date: 11/03/2023, No: 45). The study was conducted retrospectively by scanning patient records from the Meltem Hospital database between January 2018 and May 2023. A total of 88 patients, including 46 males and 42 females, who underwent otoplasty were included in the study.
Surgical Intervention
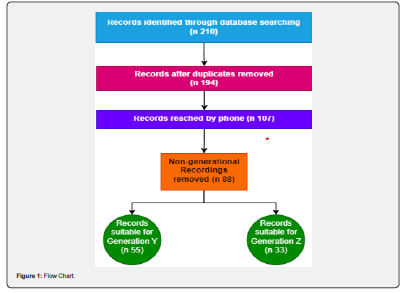
The number of individuals who underwent surgical intervention was 210. After excluding duplicate records and those who could not be reached by phone, 88 records remained. Among them, 55 were from the Y generation (born between 1981 and 1996), and 33 were from the Z generation (born between 1997 and 2012) (Figure 1).
Glasgow Benefit Inventory (GBI)
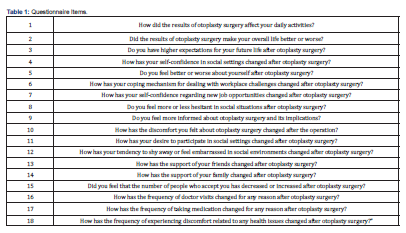
The Glasgow Benefit Inventory (GBI) formed the basis of the questionnaire used to assess the quality of life after otoplasty. Previous clinical studies have demonstrated that GBI is reliable, valid, and sensitive [11]. The GBI questionnaire is divided into three subscales: Overall Benefit subscale (OB) (Table 1, Questions 1-9), Social Benefit subscale (SB) (Table 1, Questions 10-14), and Physical Benefit subscale (PB) (Table 1, Questions 15-18). GBI scores were scaled on a standardized scale from 0 to 100.
Surgical Treatment
Patients with prominent ears underwent surgery using appropriate techniques such as suturing for underdeveloped or absent antihelical folds, conchal bowl hypertrophy, and conchal cartilage resection with conchal mastoid suture technique for prominent or forward-rotated conchae and protruding lobules. The operations were performed by the same surgeon (A.H.K.) using open surgical techniques. After obtaining patient consent, the surgical procedure was performed. Patients were treated as day cases. At the end of the procedure, a bulky head dressing was applied, which was removed on the third postoperative day. The patient was instructed to wear an ear protector during the night for one week and continuously for the following two weeks. Photographs were taken before the intervention and one month after the intervention.
Statistical Analysis
Descriptive statistics were used to describe continuous variables (mean, standard deviation, minimum, median, maximum). Linear regression, confidence analysis, and Mann-Whitney U test were employed for data analysis in this study. Linear regression analysis was used to evaluate the relationship between the dependent variable and other independent variables. Confidence analysis was conducted to determine the reliability of statistical results. The Mann-Whitney U test was used to assess the relationship between non-normally distributed continuous variables. The level of statistical significance was set at 0.05. The statistical analysis of the data was performed using IBM SPSS software version 23.0 for Windows.
Results
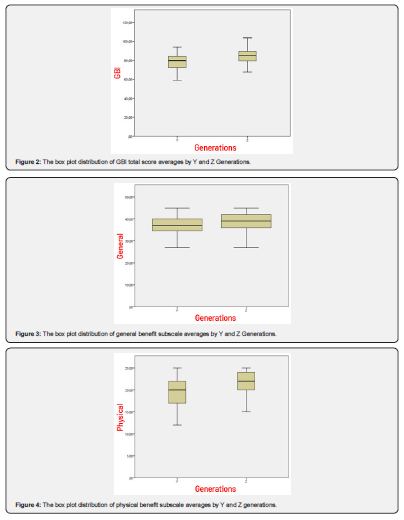
For the total Glasgow Benefit Inventory (GBI) score, the average benefit score of participants from Y generation (51.38) is lower than that of Z generation participants (55.13), and the difference between them is statistically significant (p=0.010) (Figure 2). For the General Benefit subscale (GF), the average benefit score of participants from Y Generation (36.22) is lower than that of Z generation participants (38.03), but the difference between them is not statistically significant (p=0.132) (Figure 3). For the Physical Benefit subscale (FF), the average benefit score of participants from Y Generation (19.42) is lower than that of Z generation participants (21.70), and the difference between them is statistically significant (p<0.001) (Figure 4). For the Social Benefit subscale (SF), the average benefit score of participants from Y generation (13.73) is lower than that of Z generation participants (14.70), and the difference between them is statistically significant (p=0.040) (Figure 5).
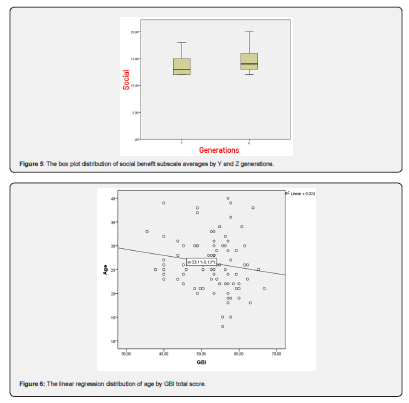
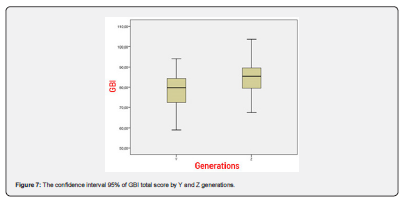
The effect of age variable on the Glasgow Benefit Inventory (GBI) scale was examined using linear regression analysis. The obtained coefficients represent the effect of the generation variable on GBI, and this effect was found to be 0.019. The coefficients and statistical significance of the linear regression model are shown with R2 Linear=0.024 and p=0.011 values (Figure 6). The 95% confidence interval for the GBI score of Y generation is between 75.4647 and 80.5596, while the 95% confidence interval for the GBI score of Z generation is between 81.2779 and 87.6918 (Figure 7).
Discussion
There is a lack of data in the literature regarding the impact of otoplasty on health-related quality of life in distinct ear deformities among the Y and Z generations. This study aimed to examine the differences in health-related quality of life outcomes among generations following otoplasty for prominent ears. Based on subjective evidence and significant results, it can be concluded that otoplasty improves quality of life. The results of this study demonstrated positive changes in quality of life due to surgical intervention. Patients with prominent ears, who we have personally witnessed in clinical practice, often experience peer bullying during childhood. Those who did not have the opportunity to undergo otoplasty during childhood seek ways to have the surgery as soon as possible. In this process, women attempt to hide their ears using their hair, while men are inclined to explore unexpected options. As an example, there is a male patient who used a glue called Cyanoacrylate to stick his ear.
Horlock et al. [13] argue that although there is no vital indication for otoplasty, significant psychological morbidity caused by auricular deformities in adults should be a strong argument for surgical intervention [13]. Braun et al. [14] reported satisfactory quality of life for adults and children using the Glasgow Benefit Inventory (GBI) in a study involving 62 patients [14]. Each successive generation is shaped and created by significant societal changes. Generational trends indicate an ongoing evolution of a population that is better educated, increasingly diverse, and comfortably immersed in the digital world [15]. It is important to be sensitive to the effects of cosmetic and reconstructive procedures like otoplasty on health-related quality of life across generations. Our study not only demonstrated a significant increase in health-related quality of life among Y and Z generation patients with prominent ears after otoplasty but also showed that this effect was greater in the Z generation. The GBI was used to measure individual health-related quality of life after otoplasty for the treatment of prominent ears.
Robinson et al. [11] developed the GBI questionnaire specifically to assess patients' subjective perception of quality-of-life following otolaryngological interventions. The questionnaire has been validated and well-established [11]. The GBI represents a highly sensitive tool for measuring changes in patients' quality of life following surgical interventions, particularly otolaryngological procedures. In this study, the GBI questionnaire was used to measure the impact of otoplasty on quality of life. For the GBI subscale, the average utility score of participants in the Y generation, which was 51.38, was lower than that of participants in the Z generation, which was 55.13, indicating a statistically significant difference (p=0.010). For the general function (GF) subscale, the average utility score of participants in the Y generation, which was 36.22, was lower than that of participants in the Z generation, which was 38.03, but the difference was not statistically significant (p=0.132).
For the social function (SF) subscale, the average utility score of participants in the Y generation, which was 13.73, was lower than that of participants in the Z generation, which was 14.70, indicating a statistically significant difference (p=0.040). For the facial function (FF) subscale, the average utility score of participants in the Y generation, which was 19.42, was lower than that of participants in the Z generation, which was 21.70, indicating a statistically significant difference (p<0.001). These results demonstrate differences between generations. It was found that participants in the Y generation had lower average utility scores than participants in the Z generation. Statistically significant differences were observed for the GBI subscales, except for the GF subscale. Furthermore, the results indicated that the GBI scale significantly predicted the generation variable. The constant term had a positive effect on the generation variable. The R2 Linear value of 0.024 and p=0.011 indicate that the GBI scale accounted for 26.9% of the variance in the generation variable and that this relationship was statistically significant.
The findings of the confidence interval analysis (Figure 4) suggest that the GBI score of the Z generation is significantly higher than that of the Y generation. Being aware of health issues specific to these generations is the first step in effectively assisting young generation patients [15]. Limitations of the study include the retrospective design, which excluded factors such as social status, environment, education level, and others, apart from age, from the evaluation. Additionally, recall bias is possible considering that some surgeries took place up to 5 years before the participation in the study. The sample size may be small, resulting in low statistical power of the obtained results. Another limitation is that our study was conducted using a telephone survey system. Telephone surveys may not represent the entire population due to accessibility issues.
Conclusion
It has been observed that otoplasty enables Z-generation patients to return to social life at an earlier stage. This finding suggests that otoplasty can contribute to increased productivity among individuals with prominent ears and aid in the formation of a healthier population. Conducting these studies on larger populations may also be appropriate in terms of public health and cost savings in healthcare expenditures.
References
- Adamson PA, HD Strecker (1995) Otoplasty techniques. Facial Plast Surg 11(4): 284-300.
- McNeil ML, Steve JA, Manohar B, Jeff RL, Paul H (2013) Can otoplasty impact hearing? A prospective randomized controlled study examining the effects of pinna position on speech reception and intelligibility. J Otolaryngol Head Neck Surg 42(1): 1-10.
- Gasques JL, J Pereira de Godoy, EN Cruz (2008) Psychosocial effects of otoplasty in children with prominent ears. Aesthetic Plast sur 32: 910-914.
- Bowden ML, I Feller, D Tholen, TN Davidson, MH James (1980) Self-esteem of severely burned patients. Arch Phys Med Rehabil 61(10): 449-452.
- Shiffman MA (2013) Advanced cosmetic otoplasty: art, science, and new clinical techniques. Springer Science & Business Media.
- Kapp-Simon KA, DJ Simon, S Kristovich (1992) Self-perception, social skills, adjustment, and inhibition in young adolescents with craniofacial anomalies. Cleft Palate Craniofac J 29(4): 352-356.
- Sarwer DB, Don LaRossa, Scott PB, David WL, Louis PB, et al. (2003) Body image concerns breast augmentation patients. Plast Reconstr Surg 112(1): 83-90.
- Chicca J, T Shellenbarger (2018) Connecting with Generation Z: Approaches in nursing education. Teaching Learning in Nursing 13(3): 180-184.
- Shatto B, K Erwin (2017) Teaching Millennials and Generation Z: Bridging the generational divide. Creat Nurs 23(1): 24-28.
- Prensky M (2001) Digital natives, digital immigrants part 1. On the horizon 9(5): 1-6.
- Robinson K, S Gatehouse, GG Browning (1996) Measuring patient benefit from otorhinolaryngological surgery and therapy. Ann Otol Rhinol Laryngol 105(6): 415-422.
- Schober P, TR Vetter (2020) Linear regression in medical research. Anesthesia Analg 132(1): 108-109.
- Horlock N, Esther V, Eileen TB, Adriaan OG, David TG (2005) Psychosocial outcome of patients after ear reconstruction: a retrospective study of 62 patients. Ann Plast Surg 54(5): 517-524.
- Braun T, Thomas H, Klaus S, Eike K, Alexander B, et al. (2010) Health-related quality of life, patient benefit, and clinical outcome after otoplasty using suture techniques in 62 children and adults. Plast Reconstr Surg 126(6): 2115-2124.
- Johanson LS (2017) Caring for patients of the millennial generation: Considerations for nurses. Nurs Forum 52(3): 207-210.





























