Delayed Facial Nerve Palsy After Head Trauma: A Case Report
Essa Tawfeeq*, Bodour Al Abdulrahim, Ammar Saleem and Mutlaq Al Sihan
Department of Otolaryngology, Zain Hospital, Kuwait
Submission: August 01, 2023; Published: September 05, 2023
*Corresponding author: Essa Tawfeeq, Department of Otolaryngology, Head and Neck Surgery, Zain Hospital, Kuwait
How to cite this article: Essa T, Bodour Al Abdulrahim, Ammar S, Mutlaq Al S. Delayed Facial Nerve Palsy After Head Trauma: A Case Report. Glob J Oto, 2023; 26 (2): 556182. DOI: 10.19080/GJO.2023.26.556182
Abstract
Delayed facial nerve palsy due to head injury is considered very rare. The pathogenesis remains unknown. We report a case of a 3 year old female, presented with 1 day history of right facial palsy (House-Brackmann grade IV), after being discharged following a head trauma a week before. Computed Tomography Scan (CT) of the head showed, a fracture of the right temporal bone extending to the right parietal bone, in addition to a right temporal subgaleal hematoma. The patient showed improvement after receiving a high dose of steroids. This case illustrates the rarity of having delayed facial nerve palsy due to head injury. Early recognition and management of such cases is the key to a better outcome.
Keywords: Facial nerve palsy; Delayed; Head trauma; Cranial nerves; Fractures
Abbreviations: CT: Computed Tomography; HRCT: High-Resolution Computed Tomography
Introduction
Facial nerve palsy due to head injury is uncommon in children. The incidence of such cases is 1.5-5% in children, and the onset is usually immediate [1]. Developing facial nerve palsy after head trauma, which is not noticed immediately is considered as delayed. The incidence of delayed facial nerve palsy after head trauma in children is 0.6-2.2% [1]. The definite pathophysiology behind delayed facial nerve palsy due to head trauma, remains not clearly known.
Case presentation
A 3 year old female presented with 1 day history of right sided facial weakness, after being discharged following a head trauma a week before. At that time, the patient had 5 episodes of vomiting. The patient denied any history of loss of consciousness, seizures, fever, or otological symptoms. On examination, the patient was conscious, alert and oriented to time, place and person. Her blood pressure and heart rate were within normal (BP: 98/54 Pulse:132), and she was afebrile (Temperature: 36). Examination of the nose, throat, paranasal sinuses and tympanic membranes was normal. Tuning fork tests (Rinnie and weber tests) were normal. Clinically, she had no neurological deficits and cranial nerves were intact. Seven days later, she presented with 1 day history of right facial nerve palsy. Examination of the facial nerve revealed incomplete eye closure, no forehead movement, asymmetrical mouth movement and synkinesis (House-Brackmann grade IV). The rest of cranial nerves were intact. Her laboratory tests showed WBC: 10.9 Hb: 13.9 Plt: 395. The remaining labs were all normal.
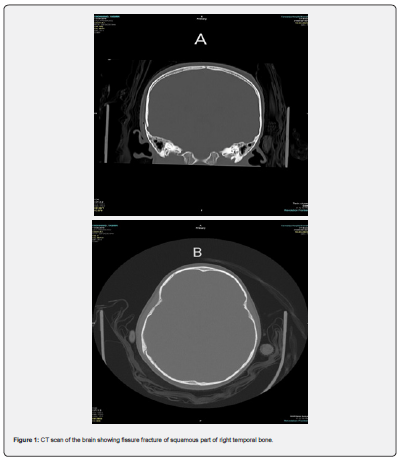
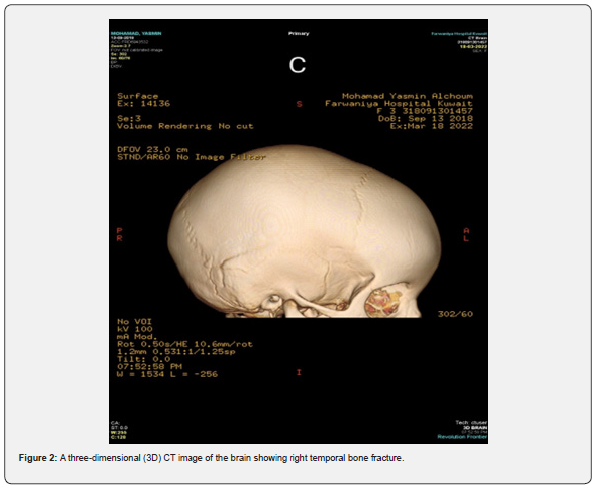
Computed tomography (CT) scan of the head showed a fissure fracture of squamous part of the right temporal bone extending to the right parietal bone. CT scan also showed a right temporal subgaleal hematoma. A final decision was to proceed with conservative management. The patient received prednisolone for one week followed by a reducing regimen over 3 weeks. Her eye was closed with a patch and ciprofloxacin eye drops with artificial tear drops were prescribed and was discharged home. At the second week follow up visit, the patient’s right sided facial weakness started to improve (House-Brackmann grade II) (Table 1) (Figure 1-3).
Discussion
Facial nerve palsy due to head injury is considered very rare in children compared to adults. The incidence of facial nerve palsy due to head trauma is 2.7/100.000 in children [1]. Temporal bone fracture resulting in facial palsy is uncommon. The incidence of facial palsy due to temporal bone fracture that is usually immediate in onset is 1.5-5% [1], whereas delayed facial nerve palsy due to temporal bone fracture is considered extremely rare. The incidence of delayed facial nerve palsy after traumatic head injury is 0.6-2,2% [1]. Temporal bone fractures are classified as longitudinal, transverse and mixed fractures. Longitudinal fractures are the most common type of temporal bone fractures and account for 80% of fractures [1]. Transverse fractures are rare and account for 15% of temporal bone fractures. Mixed fractures account for 5% of temporal bone fractures.
Facial nerve palsy occurs in 10-20% in cases of longitudinal fractures, and 88% of these cases present as delayed facial nerve palsy [2], whereas facial palsy occurs in 50% in cases of transverse fractures, and the presentation is usually immediate [1]. The pathophysiology behind the delayed presentation of facial palsy is not known. However, there are some theories that might justify this issue. Bleeding into the facial canal, which is the space that occupies 30-50% of the facial nerve, including blood vessels and the tissues surrounding it [2]. The increasing size of hematoma can compress the facial nerve and causes ischemic changes. The degree of pressure on the facial nerve might be mild and causes neuropraxia and conduction block due to segmental demyelination, while higher pressures could cause axonal damage with subsequent denervation [1]. Other causes include facial nerve edema, delayed arterial spasm or external compression of the facial nerve by bony fragments [2].


Since delayed facial nerve palsy due to traumatic head injury is uncommon, other causes of facial palsy must be ruled out, so that an appropriate treatment can be offered. The differential diagnoses of facial nerve palsy include Herpes Simplex Type I, varicella zoster virus, Ebstein-Barr virus, hemophilus influenza, tuberculosis, Lyme disease, adenovirus, rhinovirus, acute and/ or chronic otitis media, ear infection with cholesteatoma, mastoiditis, vasculitis, inflammatory disease such as Henoch- Schönlein purpura, Kawasaki syndrome and neoplastic tumors [1]. The initial assessment of a patient with facial, head, and neck trauma begins with a primary and secondary survey, as with all cases of significant trauma. Securing the airway, breathing, and circulation are imperative. Wound cleaning and irrigation and antibiotic therapy are carried out when necessary.
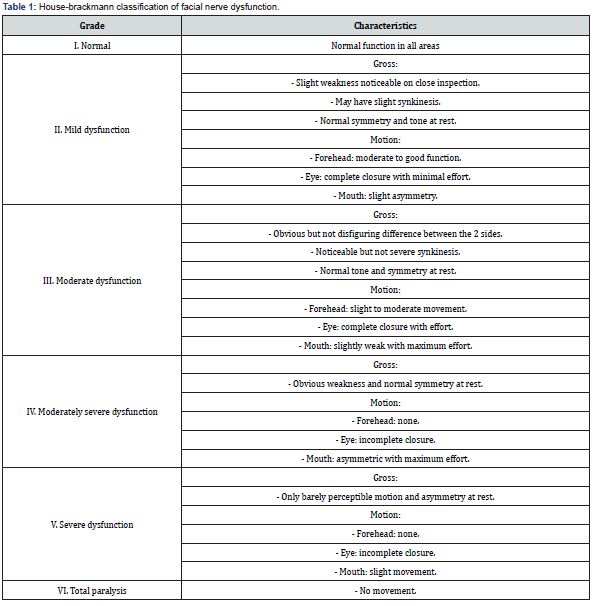
Once the patient has been stabilized, only then should a detailed examination of facial movement be performed and documented to establish a baseline. This includes eyebrow movement, eye closure, smiling, and puckering lips to assess critical branches of the facial nerve. It is helpful to grade a partial or incomplete nerve injury on an established grading system [3]. The House-Brackmann scale is a 6-point scale used for the assessment of facial nerve recovery and is widely used [4]. Radiological evaluation of the temporal bone via high-resolution computed tomography (HRCT) with fine cuts (1-mm thick slices) is helpful in assessing fallopian canal disruption. The region around the geniculate ganglion fossa should also be inspected [3]. Electrodiagnostic testing can further aid in clinical decision making when considering intervention in a traumatic facial nerve injury [3].
When indicated, the surgical treatment of post-traumatic facial nerve palsy is beneficial, especially in young and psychologically affected patients [5]. Surgery should be performed as soon as possible in patients with immediate and electro physiologically severe facial palsy, along with a clear-cut fracture line of the fallopian canal on HRCT. Facial nerve repair is achieved by direct anastomosis of the severed ends or by the use of cable grafts if loss of nerve tissue was significant. Donor sites for cable graft include the greater auricular nerve, the sural nerve, and the cervical plexus [5]. In patients with immediate facial palsy with the absence of a visible fracture line on HRCT, medical treatment in the form of steroids should be initiated. The patient should be followed over a period of 3-6 months with electrophysiological testing. If there is no recovery in terms of electrophysiological testing and clinical tests in 6 months, surgery may be considered [1]. In Patients who develop facial palsy a few days after trauma, regardless of fracture line presence on HRCT, steroids should be started to reduce edema and swelling in the nerve [1].
In patients with incomplete or delayed facial nerve palsy, prognosis is excellent, with 90% of patients reporting recovery with conservative management [6]. Electrodiagnostic studies can help determine prognosis depending on the type of nerve injury: neuropraxia, axonotmesis, or neurotmesis. In neuropraxia, the myelin sheath is damaged, but the axon is spared. Recovery is rapid and complete. Axonotmesis involves transection of the axon with sparing of the nerve sheath. Approximately 7 days after injury, Wallerian degeneration occurs in the distal axon. Recovery ensues upon regeneration of the distal axon within the intact sheath. In the case of neurotmesis, the nerve is severed with complete loss of axon continuity, requiring surgical management [7].
Conclusion
This case delineates the rarity of delayed facial nerve palsy due to head injury. Such cases require thorough investigations and prompt management, to avoid permanent nerve damage. The pathophysiology of post traumatic delayed facial nerve palsy is most likely related to bleeding into the facial canal. Early management leads to better outcomes.
References
- Leyla Kansu (2018) Post-Traumatic Delayed Peripheral Facial Palsy. The Journal of Pediatric Research 5(3): 164-167.
- Habeeb A (2022) Delayed Lower Motor Neurone Facial Nerve Palsy Following a Traumatic Head Injury. Cureus 14(6): e25753.
- Lee LN, Lyford-Pike S, Boahene KD (2013) Traumatic facial nerve injury. Otolaryngol Clin North Am 46(5): 825-839.
- House JW (1983) Facial nerve grading systems. Laryngoscope 93(8): 1056-1069.
- Darrouzet V, Duclos JY, Liguoro D, Truilhe Y, De Bonfils C, et al. (2001) Management of facial paralysis resulting from temporal bone fractures: Our experience in 115 cases. Otolaryngol Head Neck Surg 125(1): 77-84.
- Li J, Goldberg G, Munin MC, Wagner A, Zafonte R (2004) Post-traumatic bilateral facial palsy: a case report and literature review. Brain Inj 18(3): 315-320.
- Baumann BM, Jarecki J (2008) Posttraumatic delayed facial nerve palsy. Am J Emerg Med 26(1): 115.e1-2.





























