Type-I Branchial Cleft Fistula, A Rare Incidence: Treated with Surgical Excision
Pankaj Goyal*, Kishan Kumawat and Praneeth Potluri
Consultant ENT Surgeon, Apollo ENT Hospital, India
Submission: June 07, 2023; Published: June 20, 2023
*Corresponding author: Pankaj Goyal, Consultant ENT and Head-neck Surgeon, Apollo ENT Hospital, pal road, Jodhpur, Rajasthan, India
How to cite this article: Pankaj G, Kishan K, Praneeth P. Type-I Branchial Cleft Fistula, A Rare Incidence: Treated with Surgical Excision. Glob J Oto, 2023; 26 (1): 556179. DOI: 10.19080/GJO.2023.26.556179
Abstract
First branchial cleft anomalies are a subset of congenital head and neck malformations. Cysts, sinuses, or fistulas can be signs of the first branchial cleft, which is a very uncommon condition. It can be difficult to diagnose and needs cautious treatment. This case report describes a 7-year-old patient who had a draining cutaneous pit about 5mm anterior to the right ear lobule and cystic swelling in the parotid region.
Keywords: Branchial cleft; Head and neck; Congenital; Parotid; Surgical excision
Abbreviations: CT: Computed Tomography; MRI: Magnetic Resonance Imaging; SMAS: Superficial Musculo-Aponeurotic System
Introduction
First branchial cleft anomalies are uncommon. They make up less than 8% of all branchial anomalies [1,2], with an annual incidence of 1/10,00,000 [3], and are more prevalent in female than in male [4]. In the fourth and fifth weeks of pregnancy, between the first and second branchial arches, the first branchial cleft is found. This cleft develops abnormally, which leads to several defects [5]. First branchial cleft lesions originate primarily from the ventral part of the first cleft [6], which like the other branchial clefts typically disappears by eight weeks of gestation. The external auditory meatus, cavum conchae, and external tympanic membrane are still present, though, as the other components of the first cleft [6]. Hence, a persistent abnormality of the ventral part will manifest in this area.
Anomalies of the first branchial cleft also have unpredictable relationships with these structures due to the later development of the parotid gland and the migration of the facial nerve to the same region. First branchial cleft anomalies are a diverse set of malformations due to the nature of their development [7]. Although these anomalies can manifest in various ways, they frequently go undiagnosed and managed inadequately [2,3,8]. There can be a wide variety of clinical symptoms, but they almost always point to an infection. Symptoms appear above a horizontal plane passing through the hyoid bone in the preauricular and cervical regions. Management is frequently inadequate as a result of misdiagnosis, and recurrence is common.
Case report
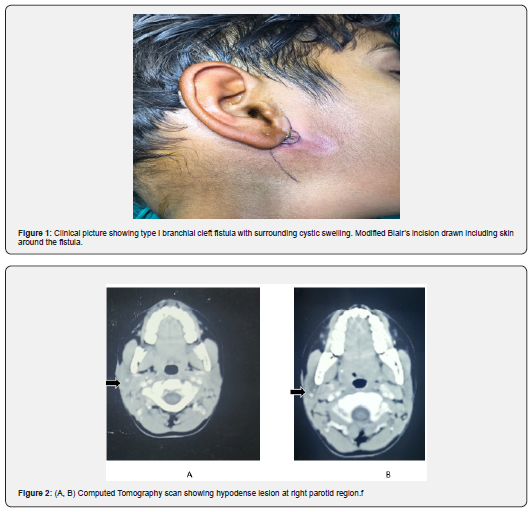
A female patient aged seven years old came to our Apollo ENT hospital in Jodhpur, Rajasthan, complaining of swelling in front of her right ear that has been there since birth. She had previously experienced drainage from a pit over the swelling. There was no prior history of ear discharge, ear pain, or decreased hearing. Her facial muscles showed normal expressiveness. Recurrent fever was not reported. Because pressure was applied to the swelling, there was occasionally pain. Before she arrived at our hospital, her parents repeatedly applied pressure to the bulge. During inspection, a soft cystic swelling measuring 1 x 1cm was found to be 5mm anterior to the ear lobule (Figure 1). Above the swelling, there was a fistula or pit that was crusted over from dried-up secretions. The results of the otoscopy were normal. No signs of facial paresis or palsy were present. The rest of the head and neck exam was clean. Her parents received counselling regarding the issue the child is having, and treatment options were thoroughly outlined.
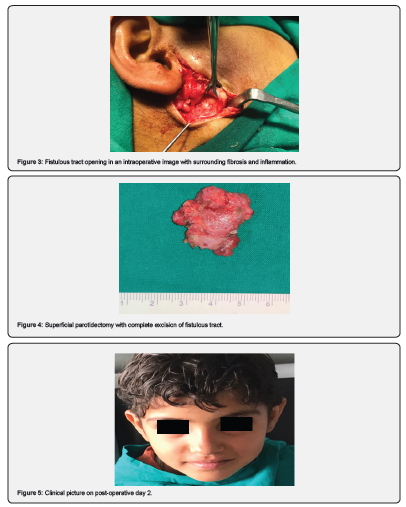
Computed tomography (CT) scan (Figure 2) of the child was performed. The parotid area was found to have a hypodense lesion. She could not afford to get magnetic resonance imaging (MRI). Her entire blood investigation was normal, and she was advised to have a surgical excision under general anesthesia. The patient was scheduled for surgery once the requisite consent was obtained. The skin surrounding the fistulous aperture was demarcated with a modified Blair's incision. The Superficial Musculo-Aponeurotic System (SMAS) flap was elevated (Figure 3). It was seen that a fistulous tract entered the parotid gland. The superficial parotidectomy was performed (Figure 4). The facial nerve was retained in its entirety during surgery. The wound was closed in layers after achieving hemostasis. The patient was extubated after surgery and moved to the recovery area. Two days were spent keeping her on intravenous antibiotics (Figure 5). Patient is doing well till one year of regular follow up without any recurrence.
Discussion
Understanding the development of the head and neck is important because the branchial pouches and arches can be used by medical practitioners to pinpoint the location and origin of certain problems. The branchial arches and clefts, which are the embryologic predecessors to many head and neck structures, start to form around 4-5 weeks of pregnancy [9]. The most common branchial cleft anomaly is caused by the second branchial arch, which accounts for nearly 95% of all defects, followed by the first arch, which accounts for less than 6% of all defects. After the third week of embryonic development, six pairs of branchial arches and clefts begin to appear in the embryo's neck and head.
From these arches, various cartilages and vessels will begin to form. The appearance of the first branchial arch is associated with the embryonic growth of the parotid. Furthermore, the first arch is the precursor of the formation of the maxilla, and the first pharyngeal pouch forms the middle ear, eustachian tube, and mastoid antrum. During the sixth week of gestation, these arches begin to merge and disappear; however, in some rare cases, the first branchial arch does not completely disappear [10], resulting in the first branchial cleft anomaly. Branchial cleft cysts, fistulas, and sinuses can affect people of any age, but they most frequently affect people in their first and second decades of life [11].
According to investigations by Arnot and Work, there are two unique varieties of first branchial cleft: type 1 and type 2. These types are distinguished by the anatomical and histological locations of the cleft, respectively. Type 1 Arnot's lesion is characterised by the presence of a painful cyst or discharging sinus in the parotid gland area, which is frequently associated with the lower branches of the facial nerve and may extend deep into the infratemporal fossa. It usually manifests itself in early or middle adulthood whereas type 2 Arnot's consists of a sinus or superficial cyst in the anterior triangle of the neck with an external opening below the angle of the mandible and a track that extends to and may communicate with the external auditory canal. The relationship with the facial nerve is variable. It appears in infancy or early childhood [12].
Type 1 of the condition, according to Work, is the duplication of the membranous external ear canal running parallel to the normal ear canal, while type 2 involves the duplication of the pinna, which is positioned in the upper neck just below the angle of the mandible [13]. Anomalies of the first branchial cleft are frequently found near the parotid gland, particularly the superficial lobe that overlies the lesion. Many intratympanic cysts are actually embryonic formations that arise from the dorsal portion of the first branchial cleft. Without surgical exploration, diagnosing first branchial cleft cysts/ fistula in or near the parotid gland can be difficult in practice.
In our case, the anatomical, radiological and histological characteristics showed the first branchial fistula of type 1 Arnot. The first branchial cleft fistula is typically misdiagnosed and treated since it is uncommon [14]. For avoiding recurrences and preventing damage to the facial nerve, early diagnosis and appropriate treatment are essential. A branchial cleft cyst is a fluctuant mass that, once diagnosed, should be removed because the cyst can spread and harden over time, becoming a source of infection and drainage [15]. If any tissue residue is left, there is a high chance of recurrence. The main constraint was keeping the facial nerve (marginal mandibular nerve) intact. More than any other type is branchial defect, the facial nerve and the first branchial cleft are inextricably linked.
Conclusion
First branchial cleft abnormality is a very uncommon condition that is frequently misdiagnosed, which can cause inadequate treatment and a delay in receiving appropriate care. In these cases, wide exposure is required, and a standard parotidectomy incision allows adequate exposure of the anomaly while preserving the facial nerve. The ability to identify and protect the facial nerve during resection as well as a thorough understanding of regional embryogenesis, the circumstances surrounding the finding, and the various anatomical presentations are all necessary for a successful removal without complications.
References
- D’Souza AR, Uppal HS, De R, Zeitoun H (2002) Updating concepts of first branchial cleft defects: a literature review. Int J Pediatr Otorhinolaryngol 62(2): 103-109.
- Guo YX and Guo CB (2012) Relation between a first branchial cleft anomaly and the facial nerve. Br J Oral Maxillofac Surg 50(3): 259-263.
- Liu Y, Li T, Xue J, Jia J, Xiao S, et al. (2012) First branchial cleft fistula presenting with internal opening on the Eustachian tube: illustrated cases and literature review. Int J Pediatr Otorhinolaryngol 76(5): 642-645.
- Al Mahdi AH, Al Khurri LE, Atto GZ, Dhaher A (2013) Type II first branchial cleft anomaly. J Craniofac Surg 24(5): 1832-1835.
- 5 Ertas B, Gunaydin RO, Unal OF (2015) The relationship between the fistula tract and the facial nerve in type II first branchial cleft anomalies. Auris Nasus Larynx 42(2): 119-122.
- Bajaj Y, Ifeacho S, Tweedie D, Jephson CG, Albert DM, et al. (2011) Branchial anomalies in children. Int J Pediatr Otorhinolaryngol 75(8): 1020-1023.
- Tham YS, Low WK (2005) First branchial cleft anomalies have relevance in otology and more. Ann Acad Med Singapore 34(4): 335-338.
- Flint PHB, Lund V, Niparko J, Robbins K, Thomas JR, et al. (2015) Cummings Otolaryngology. 6th ed Elsevier.
- Faruque O, Wischhusen JD, Reckley LK, Rooks VJ, Liming BJ (2019) First branchial cleft fistula (Work Type 2) with an internal opening to the Eustachian tube: Case report and review of literature. Radiol Case Rep 14(7): 819-824.
- AJ Sukhun, EM Naggar (2019) Unusual Presentation of a Large Multilocular Second Branchial Cleft Cyst. J Craniofac Surg 30(6): 1772-1773.
- Arnot RS (1971) Defects of the first branchial cleft. S Afr J Surg 9(2): 93-98.
- Liu Y, Li T, Xue J, Jia J, Xiao S, et al. (2012) First branchial cleft fistula presenting with internal opening on the Eustachian tube: Illustrated cases and literature review. Int J Pediatr Otorhinolaryngol 76(5): 642-645.
- Liu H, Cheng A, Ward BB, Wang C, Han Z, et al. (2020) Clinical Manifestations, Diagnosis, and Management of First Branchial Cleft Fistula/Sinus: A Case Series and Literature Review. J Oral Maxillofac Surg 78(5): 749-761.
- Lee HJ, Kim EK, Hong S (2006) Sonographic detection of intrathyroidal branchial cleft cyst: a case report. Korean J Radiol 7(2): 149-151.
- Akakpo K, Luck K, Chun RH (2020) Use of a Cervicofacial Flap in Closing Large Defects Following Wide Local Excision of Complicated Preauricular Lesions. Ann Otol Rhinol Laryngol 129(12): 1163-1167.





























