Surgical Therapy of Advanced Otosclerosis: Does It Have to Be an Implantable Hearing System?
Daniel Boeger*
Department for ENT, SRH Central Hospital Suhl, Germany
Submission: May 05, 2022; Published: May 19, 2022
*Corresponding author: Dr. Daniel Boeger, Department for ENT, SRH Central Hospital Suhl, Albert- Schweitzer- Str.2, 98527 Suhl, Germany E-mail: daniel.boeger@srh.de
How to cite this article: Daniel Boeger. Surgical Therapy of Advanced Otosclerosis: Does It Have to Be an Implantable Hearing System?. Glob J Oto, 2022; 25 (2): 556157. DOI: 10.19080/GJO.2022.25.556157
Keywords: Otosclerosis; Hearing loss disease; Implantable hearing; Audiological; Stapes
Abbreviations: VSB: Vibrant Sound Bridge; BAHA: Bone Anchored Hearing Aid; PTA: Pur Tone Average; BKB: Bamford-Kowal-Bench
A Casuistry
Otosclerosis, as a (mostly) combined hearing loss disease, should usually cause little to no difficulties in the diagnosis of itself nowadays. In the sum of anamnesis, clinical and audiological examination findings, it is usually possible to make the correct diagnosis. The therapy consists of 1) a wait-and-see (Waite and Scan), 2) a conservative (hearing aid fitting) and 3) a surgical treatment. Depending on the severity of the hearing loss, the patient's wishes and general condition, the experienced ENT physician will choose the appropriate therapy strategy. If the general health condition of the patient allows it as well as the hearing aid treatment offered by the surgeon obligatorily as a therapy alternative is not desired by the patient, the stapes operation is carried out in most cases of otosclerosis. This operation, known in its basic execution, although in different variations, e.g., the type of stapedotomy (with laser, perforator or skeeter) or the prostheses used in form (eyelet for clamping, clip prostheses, etc.) and material (titanium, nitinol), is essentially common.
Surgical treatment options for so-called advanced otosclerosis have increased in recent years. Active partially implantable hearing systems like the Vibrant-Sound Bridge (VSB© Fa. Medel, Austria) in combination with a stapesplasty ("Power Stapes"), the active fully implantable system Carina© (Fa. Cochlear Boulder, CO, USA) or passive bone conduction earphones (BAHA, "Bone anchored Hearing Aid") have become popular. In cases of advanced otosclerosis, the cochlear implant may also be considered. The limiting factor for the choice of systems here is the bone conduction threshold: depending on the approval, they can be used. From values of bone conduction hearing threshold worse than 40-45dB (averaged, PTA 4 (Pur Tone Average for frequencies 0.5; 1; 2 and 4kHz)) there are already case reports and series for the use of implantable hearing systems.
With all these possibilities offered by modern implant technology, the resulting difficulties for patients, such as wound infections (BAHA), problems with the actuator or the need for subsequent rehabilitation, must not be ignored and must be explained to the patients. Thus, the question arises whether even advanced otosclerosis with moderate inner ear threshold and maximum conductive block, by means of conventional stapes surgery and subsequent hearing aid fitting represents a good, if not very good, especially audiological result for the affected person.
Case study
We report on a patient who was 74 years old at the time of initial presentation to our outpatient clinic. He reported an increasing hearing loss in both ears that had been present for about 20 years. In the last years the hearing loss had increased again. For about 20 years he has been fitted with hearing aids on both sides. In the last 6 years, these were changed to so-called power hearing aids, which initially enabled good speech comprehension, but now no longer contributed to any significant acoustic understanding. He felt increasingly acoustically isolated. He approached us with the wish for a possible surgical improvement of his hearing.
The question about otitis, trauma and otorrhea was answered in the negative. The findings of the ENT examination concerning the ear showed a gray, non-irritant and intact tympanic membrane. The tuning fork test according to Weber could not be lateralized, the test according to Rinne was negative. The other findings were normal for the patient's age. The pretherapeutic pure tone audiogram showed a moderate to severe combined hearing loss with a conductive block on both sides (Figure 1). The Pur-Tone Average of bone conduction threshold for frequencies 0.5; 1; 2 and 4kHz (PTA 4) was 38.75dB on the right and 45dB on the left. The air-conduction hearing threshold for these frequencies averaged 92.5dB on the right and 85dB on the left, corresponding to profound hearing loss bordering on deafness.
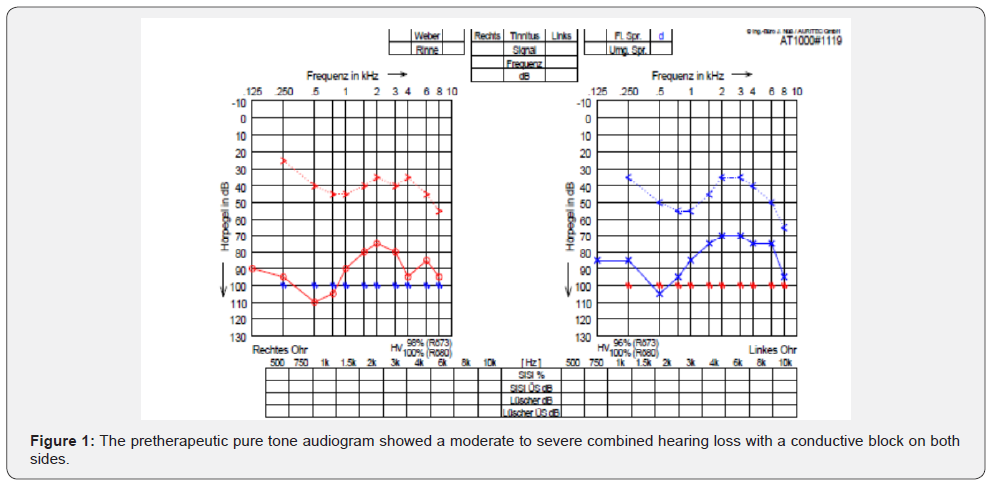
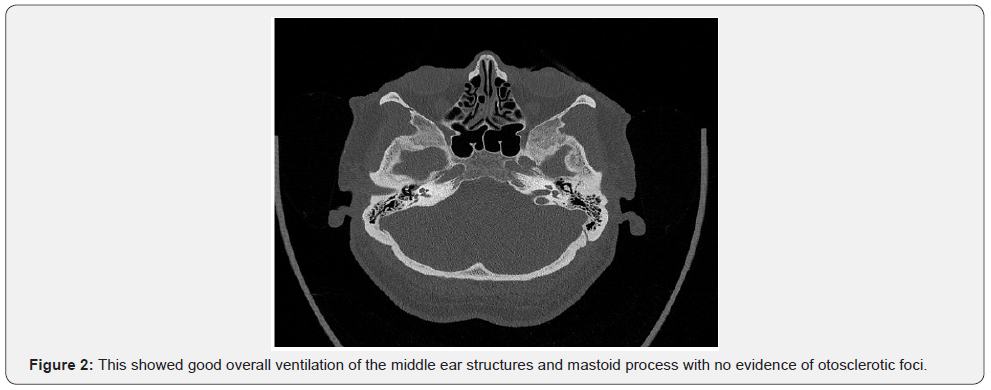
The air-bone gap averaged over the 4 frequencies was 52.5dB on the right and 38.75dB on the left. In each case, the tympanogram showed a peak of pressure in the null passage (type A). The stapedius reflexes were not triggerable bds. ipsi- and contralaterally. Because of the very pronounced almost high-grade combined hearing loss on both sides, we performed a pre-therapeutic HR-CT of the petrous bone. This showed good overall ventilation of the middle ear structures and mastoid process with no evidence of otosclerotic foci (Figure 2). An MRI of the cranium and the cerebellopontine angle region was also without pathologic findings. After discussing all findings with the patient and the surgical options, we decided to perform a trial tympanoscopy with the option of stapesplasty, initially on the right side. The patient was explicitly informed about the possible complications. The need for postoperative hearing aid fitting was communicated.
Intraoperatively, surgery revealed a fixed stapes on the right side with an otherwise mobile ossicular chain, confirming the diagnosis of presumed otosclerosis. After resection of the stapes superstructure, the CO2 laser stapedotomy was followed by the insertion of a 4.5mm titanium soft-clip prosthesis made by Kurz. The immediate postoperative and subsequent course was without complications, so that we decided about 12 months (due to the 1st wave of the SARS-COV II pandemic) to operate on the opposite side. Again, the expected picture of otosclerosis was seen. The procedure was identical, a 4.5mm titanium soft-clip prosthesis was also used. Postoperatively, bone conduction was measured on day 1, and detamponade was performed on postoperative day 14.

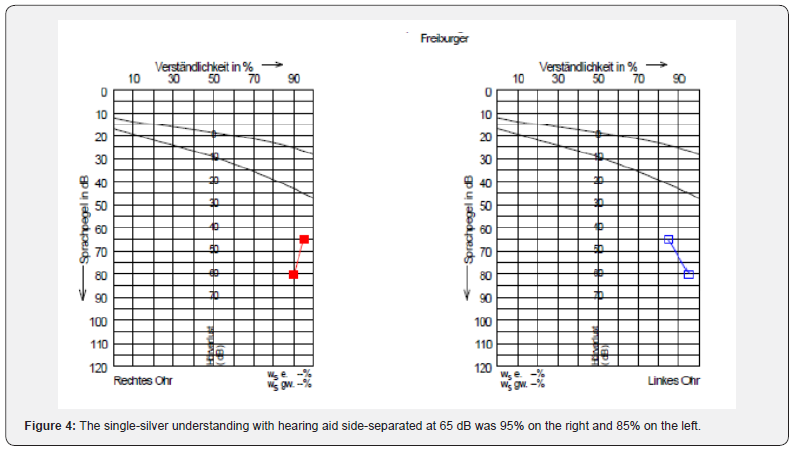
We obtained a pure tone audiogram 15 months after the 1st and 3 months after surgery on the 2nd side (Figure 3). The ABG averaged 4dB on the right side and 4dB on the left side with almost identical bone conduction curves. On the issue of hearing aid readjustment, the patient presented to the referring otolaryngologist. A good 18 months after the initial surgery and 6 months the patient presented with the hearing aids in our outpatient clinic. Here, the patient showed an averaged hearing threshold of 33.75dB on the right side and 37.5dB on the left side. The single-silver understanding with hearing aid side-separated at 65dB was 95% on the right and 85% on the left (Figure 4).
Discussion
Surgical treatment of otosclerosis essentially follows a standard approach with variations in detail. Surgical techniques have evolved over a period of approximately 100 years [1]. With the use of active middle ear implants, such as the Carina system, from Cochlear [2], the Vibrant Sound Bridge (VSB) from Medel, also known as power tapes [3], and even in cases of profound hearing loss with a cochlear implant [4], additional surgical options are also available to achieve a satisfactory hearing situation for patients. A 2018 paper [5] reported on 9 patients with simultaneous stapesplasty and VSB insertion for otosclerosis. All patients were cases with moderate to severe form of otosclerosis, and the bone conduction curve should be at least 40dB (inclusion criterion). The mean value of the bone conduction threshold averaged 45.2dB.
Another group [6] studied 33 patients (35 cases in total) with profound hearing loss due to otosclerosis who were CI candidates according to air conduction criteria (worse than 90dB at 2 and 4kHz and no adequate benefit with conventional hearing aids, defined as Bamford-Kowal-Bench (BKB); 50% at 70dB was not achieved; Louis Dwyer-Hemmings). All patients underwent "conventional" stapesplasty. In 80% of the cases, the air conduction threshold improved and an average of 26.3dB. Thus, conventional hearing aids could be used successfully. The authors also point to the now very safe surgical method of stapesplasty combined with comparatively low costs. Moreover, it does not require rehabilitation and the consequences of CI fitting on sound quality and tonality do not occur.
On the basis of our patient, we were able to show very impressively that even a high-grade combined hearing loss due to bilateral otosclerosis produced good audiological results postoperatively and very good results with conventional hearing aids. The preoperatively measured bone conduction thresholds of 38dB right and 45dB left (PTA4) were not a disadvantage for this procedure. The preoperatively measured air-bone gaps of 52.5dB on the right and 38.7dB on the left could be reduced to postoperative values of 4dB each. After readjustment of the hearing aids, the patient achieved a single-silver understanding of 95% right and 85% left at 65dB.
As a result, we were able to show that despite high-grade combined hearing loss due to otosclerosis, the performed stapesplasty with subsequent hearing aid fitting achieved excellent audiological results, thus a simple and comparatively inexpensive method (both in material use and in postoperative follow-up without rehabilitation) could be used beneficially. Even preoperative bone conduction thresholds worse than 40 dB need not call this approach into question.
Conclusion for Practice
Otosclerosis, if it appears clinically-audiologically, should be operated in the sense of a stapesplasty, even in the presence of a higher degree of hearing loss. Further measures, such as the use of "Powerstapes" or cochlear implants are reserved for revision surgery.
References
- Plontke SK, Metasch M-L, Zirkler J, Thomas Z (2018) Diagnosis and surgical therapy of otosclerosis-Part 2: Indication, Surgical Procedure and Postoperative Treatment]. Laryngorhinootologie 97(10): 717-734.
- Didczuneit-Sandhop B, Langer J (2022) Use of the Carina active middle ear implant in otosclerosis patients. HNO 69(10): 828-834.
- Kontorinis G, Lenarz T, Mojallal H, Anna-Lena H, Burkard S, et al. (2011) Power stapes: an alternative method for treating hearing loss in osteogenesis imperfecta? Otol Neurotol 32(4): 589-595.
- Eshraghi AA, Ila K, Ocak E, Fred FT (2018) Advanced otosclerosis: stapes surgery or cochlear implantation? Otolaryngol Clin North Am 51(2): 429-440.
- Chang C-J, Wen Y-H, Sun C-H, Millo AB, Hung-Pin W, et al. (2019) Treatment of moderate-to-severe otosclerosis with simultaneous piston surgery and incus vibroplasty. Ci Ji Yi Xue Za Zhi 31(2): 96-101.
- Dwyer-Hemmings L, Manjaly JG, Nash R, Abir M, Jeremy AL, et al. (2019) Stapes Surgery for Profound Hearing Loss Secondary to Otosclerosis. Ear Nose Throat J 98(5): 273-278.





























