Vestibular Evoked Myogenic Potentials of Asymptomatic Covid-19 PCR-Positive Cases
Mustafa MWM1* and Taya UK2
1 Associate Professor of Audiovestibular Medicine, Department of Otorhinolaryngology, Qena Faculty of Medicine, South Valley University, Egypt
2 Lecturer of Otorhinolryngology, Department of Otorhinolaryngology, Qena Faculty of Medicine, South Valley University, Egypt
Submission:June 23, 2020; Published:July 07, 2020
*Corresponding author:Mustafa MWM, Associate Professor of Audiovestibular Medicine, Otorhinolaryngology Department, Qena Faculty of Medicine, South Valley University, Egypt
How to cite this article: Mustafa M, Taya U. Vestibular Evoked Myogenic Potentials of Asymptomatic Covid-19 PCR-Positive Cases. Glob J Oto, 2020; 22(5): 556097. DOI: 10.19080/GJO.2020.22.556097
Abstract
Background: World Health Organization (WHO) officially announced the COVID-19 epidemic as a pandemic. Coronavirus disease (COVID-19) is an infectious disease caused by a newly discovered coronavirus. Little direct evidence suggests a viral cause for labyrinthitis; however, a wealth of epidemiologic evidence implicates several viruses as potentially causing inflammation of the labyrinth. Viral labyrinthitis is often preceded by an upper respiratory tract infection and occurs in epidemics.
Aims/Objectives: This study compared latencies of vestibular evoked myogenic potentials (VEMPs) between asymptomatic COVID-19 PCR-positive cases and normal non-infected subjects.
Material & methods: Twenty cases who were confirmed positive for COVID-19 and had none of the known symptoms for this viral infection formed the test group for 2 full weeks. Their age ranged between 20-50 years to avoid any age-related hearing affection. Patients who had definite symptoms of COVID-19 infection as well as those who had a history of hearing loss or a history of any known cause of hearing loss were excluded from the examined sample. VEMPs latencies were measured for all participants.
Results: Deterioration of saccular hair cell functions was detected by the significantly increased latency of the VEMPs compared to controls.
Conclusions and significance: COVID-19 infection could have drastic effects on vestibular hair cell functions despite being asymptomatic. COVID-19 patients should be followed up to detect any complaints regarding their vestibular performance. The mechanism of these effects requires further research.
Keywords:COVID-19; Corona virus; VEMP; Vestibular function
Background
An acute respiratory disease, caused by a novel coronavirus (SARS-CoV-2, previously known as 2019-nCoV), the coronavirus disease 2019 (COVID-19) has spread throughout China and received worldwide attention. On 30 January 2020, World Health Organization (WHO) officially declared the COVID-19 epidemic as a public health emergency of international concern. Coronavirus disease (COVID-19) is an infectious disease caused by a newly discovered coronavirus. Most people infected with the COVID-19 virus experience mild to moderate respiratory illness and recover without requiring special treatment [1].
COVID-19 infection symptoms may appear 2-14 days after exposure (based on the incubation period of COVID-19 virus). The clinical symptoms of COVID-19 patients include fever, cough, fatigue, and a small population of patients had gastrointestinal infection symptoms. The elderly and people with underlying diseases are susceptible to infection and prone to serious outcomes, which may be associated with acute respiratory distress syndrome (ARDS) and cytokine storm [1,2]. Currently, there are few specific antiviral strategies, but several potent candidates of antivirals and repurposed drugs are under urgent investigation. There are multiple scenarios COVID-19 patients may follow: Some get serious respiratory distress, some improve with medical treatment, the rest recover with no intervention [2].
Viral infections can cause congenital and acquired hearing loss. Rubella and cytomegalovirus are the best-recognized viral causes of prenatal hearing loss. Virally induced hearing loss in the postnatal period is usually due to mumps or measles. Viral infections are also implicated in idiopathic, sudden sensorineural hearing loss (SNHL). Experimental evidence suggests that inflammatory proteins play a critical role in the pathogenesis of cytomegalovirus-induced hearing loss [3].
A unique form of viral labyrinthitis is herpes zoster oticus, or Ramsay-Hunt syndrome. The cause of this disorder is reactivation of a latent varicella-zoster virus infection occurring years after the primary infection. Evidence suggests that the virus may attack the spiral and vestibular ganglion in addition to the cochlear and vestibular nerves [3]. Auditory and vestibular symptoms develop in approximately 25% of patients with herpes oticus, in addition to the facial paralysis and vesicular rash that characterize the disease [4].
Little direct evidence suggests a viral cause for labyrinthitis; however, a wealth of epidemiologic evidence implicates several viruses as potentially causing inflammation of the labyrinth. Viral labyrinthitis is often preceded by an upper respiratory tract infection and occurs in epidemics. The histologic finding of axonal degeneration in the vestibular nerve suggests a viral etiology for vestibular neuritis [5].
Potential viral causes of labyrinthitis include the following:
a) Cytomegalovirus
b) Mumps virus
c) Varicella-zoster virus
d) Rubeola virus
e) Influenza virus
f) Parainfluenza virus
g) Rubella virus
h) Herpes simplex virus 1
i) Adenovirus
j) Coxsackievirus
k) Respiratory syncytial virus
Asymptomatic infection at time of laboratory confirmation has been reported from many settings [2]; a large proportion of these cases developed some symptoms at a later stage of infection. There are, however, also reports of cases remaining asymptomatic throughout the whole duration of laboratory and clinical monitoring. Viral RNA and infectious virus particles were detected in throat swabs from some COVID-19 patients, but they developed none of the symptoms listed above [1]. Although several viral infections may lead to hearing loss only or as a part of a labyrinthitis, it is still unknown whether COVID-19 has effects on the vestibular system or not. Therefore, this research was designed to address the impact of this novel viral infection on the saccular vestibular system.
Material & Methods
Twenty cases who were confirmed positive for COVID-19 and had none of the known symptoms for this viral infection formed the test group for 2 full weeks. Their age ranged between 20-50 years to avoid any age-related hearing affection. Patients who had definite symptoms of COVID-19 infection as well as those who had a history of hearing loss or a history of any known cause of hearing loss were excluded from the examined sample. Twenty subjects who had normal hearing (All subjects had audiometric thresholds at or better than 15dB HL) with no history of a known cause of hearing loss were used as a control group.
All the following procedures was conducted for both study (at the 14th day after being confirmed COVID-19 positive but asymptomatic) and control groups:
a) Meticulous history taking and full ENT examination were carried out on all subjects before audiological testing
b) Basic Audiological evaluation. Audiometric thresholds were measured using a calibrated Amplaid 309 clinical audiometer [6]. Air conduction thresholds were measured for frequencies from 250 to 8000Hz using Telephonics TDH39 earphones. Bone conduction thresholds were obtained for frequencies from 250 to 4000Hz using a Radio Ear B71 bone vibrator. The audiometric thresholds were measured using the modified Hughson-Westlake method [7].
c) Immittance evaluation. Tympanometry was carried out using an Amplaid 775 middle ear analyzer to rule out middle ear pathology.
d) Vestibular evoked myogenic potentials. Vestibular evoked myogenic potentials (VEMPs) were recorded in all subjects using an evoked potential system Spirit Nicolet. Monaural alternating acoustic click stimuli at an intensity of 90dB nHL were used. EMG activity was recorded on the sternocleidomastoid muscles (SCM) with the patient in the sitting position. The mean peak latency (in ms) of the two early waves (P13-N23) of the VEMP was measured.
An informed consent was obtained from all participants. The study was approved from the Egyptian Central Unit of Medical Service (ECUMS). EMMS also helped the research team to connect with the study subjects. EMMS secured a totally aseptic environment for this research including subjects and equipment.
Results
Pure-tone audiometry
Paired t-test test was used to compare the pure-tone thresholds between the test and the control groups. No significant difference (p> 0.05) was found at all octave and mid-octave frequencies (250, 500, 750, 1000, 1500, 2000, 3000), 4000. Significant difference was found (P< 0.05) at 4000,6000, and 8000Hz between both groups (Figure 1).
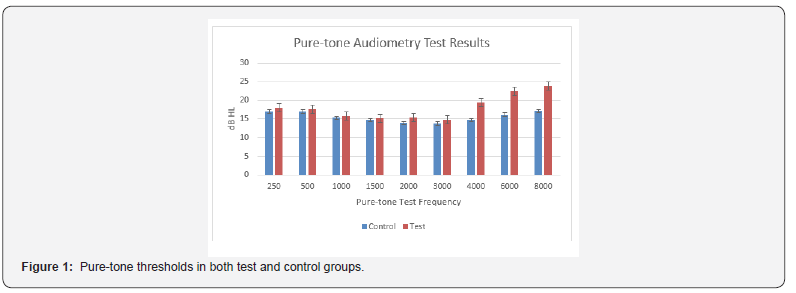
Vestibular evoked myogenic potentials (VEMPs)
Paired t-test was used to compare the VEMPs latencies of waves P13 and N23 among the control and test groups. A highly significant (p< 0.001) difference was found between the control group and the test groups (Figure 2).
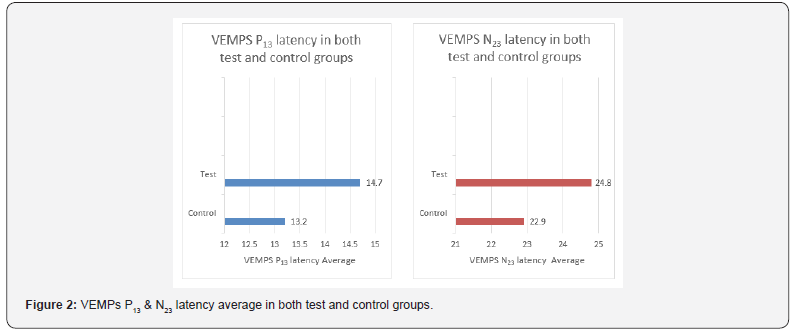
Discussion
A highly significant (p< 0.001) difference was found between the control group and the test groups as regards the latencies of VEMPs P13 & N23 latency average. The high frequency pure-tone thresholds were significantly worse in the test group. Similar results of a previous study showed that COVID-19 infection had deleterious effects on the hair cells in the cochlea [8]. Moreover, the absence of the major symptoms does not guarantee a safe healthy labyrinthine function. The damage to the outer hair cells was evidenced by the reduced amplitude of the TEOAEs in test group when compared with control group. Additionally, the harm to the saccular vestibular cells was detected by the marked delayed VEMPs waves.
Auditory system damage secondary to viral infections is typically intracochlear or intralabyrinthine; however, some viruses can affect the auditory brainstem as well. Mechanisms of injury to the peripheral auditory system can include direct viral damage to the organ of Corti, stria vascularis, or spiral ganglion; damage mediated by the patient’s immune system against virally expressed proteins (Cytomegalovirus); and immunocompromise leading to secondary bacterial infection of the ear (Human Immunodeficiency Virus & measles) [3]. The deterioration saccular vestibular functions could be attributed to the generalized damaging effects of the viral infection on the labyrinthine hair cells, but the mechanism is still unknown. The results of the present study also demonstrated that the absence of major symptoms may hide unknown impact on the delicate sensory organs taking the labyrinth as an example.
Conclusion
In conclusion, COVID-19 infection could have drastic effects on saccular vestibular hair cell functions despite being asymptomatic. The mechanism of these effects requires further research as well as close follow-up.
Acknowledgement
I am deeply grateful to Egyptian Central Unit of Medical Service (ECUMS). I am also thankful for the technical support of Sigma incorporation for Audiological Services and the great help and cooperation of Dr. Marwa El Hawary (Alfayoum general hospital) in conducting this research.
References
- Cao ZH, Yuan YT, Shou DC, Zhong Si Hong, Yuan Yang, et al. (2020) The origin, transmission, and clinical therapies on coronavirus disease 2019 (COVID-19) outbreak-an update on the status. Mil Med Res 7-11.
- Coronavirus disease 2019 (COVID-19) pandemic: increased transmission in the EU/EEA and the UK-seventh update, ECDC, 2020.
- Wu JF, Jin Z, Yang JM, Liu YH, Duan ML (2012) Extracranial and intracranial complications of otitis media: 22-year clinical experience and analysis. Acta Otolaryngol 132(3): 261-265.
- Nadol JB (1978) Hearing loss as a sequela of meningitis. Laryngoscope 88(5): 739-755.
- Schuknecht HF, Kitamura K (1981) Second Louis H Clerf Lecture. Vestibular neuritis. Ann Otol Rhinol Laryngol Suppl 90(1 Pt 2): 1-19.
- ANSI S3. 6-2004 specification for audiometers. ANSI 2004.
- Carhart R, Jerger JF (1959) Preferred method for clinical determination of pure tone thresholds. Journal of Speech & Hearing Disorders 24: 330-345.
- Mustafa MWM (2020) Audiological Profile of Asymptomatic Covid-19 PCR- positive cases. Am J Otolaryngol 10: 102483.





























