Transient and Persistent Hypoparathyroidism in Hemi and Total Thyroidectomy Cases
Ibrahim Sumaily*1, Mohammad Alshareef2, Majed Assiri2, Ramzi Daghriri2, Mubarak Alqhtani3 and Fahd Alharbi4
Director, ENT Hospital, Alambagh, Lucknow, India1Department of Otolaryngology-Head and Neck Surgery, King Fahd Central Hospital in Jazan, KSA
2Department of Otolaryngology-Head and Neck Surgery, Asir Central Hospital KSA
3Department of Otolaryngology-Head and Neck Surgery, King Faisal Medical City, KSA
4Department of Otolaryngology-Head and Neck Surgery, Jazan University, KSA
Submission: August 30, 2019; Published: September 20, 2019
*Corresponding author:Department of Otolaryngology-Head and Neck Surgery, King Fahd Central Hospital in Jazan, KSA
How to cite this article: Ibrahim Sumaily, Mohammad Alshareef, Majed Assiri, et al. Transient and Persistent Hypoparathyroidism in Hemi and Total Thyroidectomy Cases. Glob J Oto, 2019; 20(5): 556048. DOI: 10.19080/GJO.2019.20.556048
Abstract
Introduction: Thyroidectomy is one of the most common surgeries conducted daily. Hypoparathyroidism is one of the most common complications of thyroidectomy. Sometimes it causes life threatening sequelae if not detected and managed early. Here in we studied the incidence and persistence of hypoparathyroidism in those who underwent total or partial thyroidectomy.
Method: A retrospective chart review study, we reviewed the records of 214 patients who Underwent thyroid surgery and followed their parathyroid hormone (PTH) and serum calcium (Ca++) results for new onset hypoparathyroidism in early postoperative period and long term follow up.
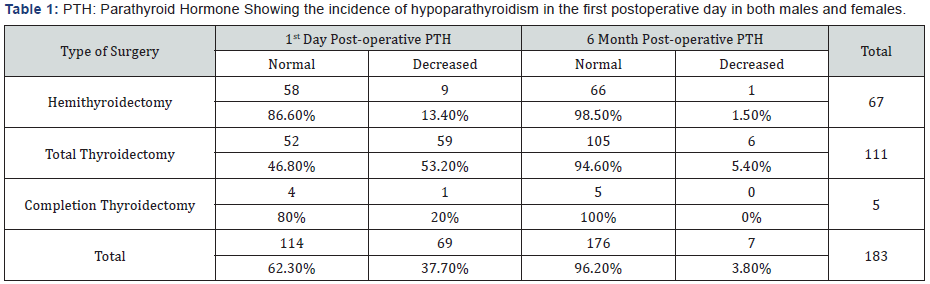
Results: Out of 214 patients, 183 met our criteria. 36.6% underwent hemithyroidectomy, 60.7% total thyroidectomy, and 2.7 % completion thyroidectomy. Hypoparathyroidism found in the 1st post-operative day in 37.7%. it occurs in 13.4% of hemithyroidectomy cases, and 53.2% of total thyroidectomy cases and 20% of completion thyroidectomy cases. 1 case only developed delayed onset hypoparathyroidism. Persistent hypoparathyroidism occurs in 1.5% of hemithyroidectomy cases, and 5.4% in total thyroidectomy cases. Apart from type of surgery, female gender was associated with higher incidence of transient hypoparathyroidism while male gender has higher incidence of persistent hypoparathyroidism.
Conclusion: Transient post-operative Hypoparathyroidism can occur even in hemithyroidectomy, and to much more extent in total thyroidectomy cases. Most of the post-operative hypoparathyroidism are improved within 1 month. Only few patients will need lifelong supplement.
Keywords: Hypoparathyroidism; Thyroidectomy; Transient; Persistent
Introduction
Surgery is the treatment of choice for symptomatic patients with goiter, although associated with a low rate of mortality and morbidity. Hypoparathyroidism is one of the well-known thyroidectomy complications. It sometimes causes life threatening sequelae if not detected and managed early. Hypoparathyroidism occurs more commonly with total thyroidectomy. But it can occur with hemithyroidectomy where the surgeon consider that two parathyroid glands are not touched, and they will work even if the other two are removed and discharging the patient ignoring this risk. However, we conducted this study to report the incidence and persistence of hypoparathyroidism in those who underwent total or hemithyroidectomy.
Method
A retrospective chart review study, we reviewed the records of 214 patients who underwent thyroid surgery in our tertiary health care center between October 2012 and January 2017 looking for the incidence and course of hypoparathyroidism in these cases and the factors associated with this complication. Serum parathyroid hormone (PTH) and serum calcium (Ca++) results pre-operatively, 1st post-operative day and 6 months post operatively reviewed and correlated with the type of surgery. We included all cases of hemithyroidectomy, total thyroidectomy or completion thyroidectomy who has had normal parathyroid hormone preoperatively.. SPSS v.22 used for data analysis.
Results
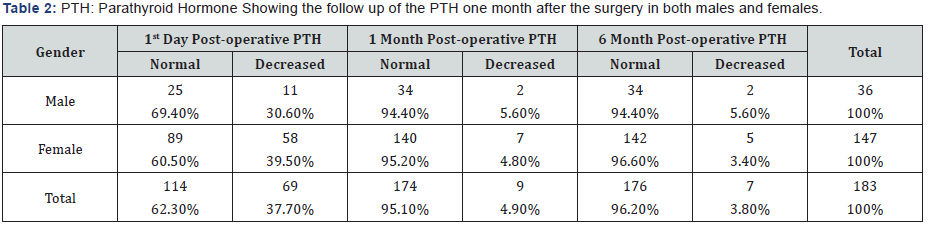
Out of 214 cases, 183 met our criteria, 80.3% female and 19.7% males. Mean age was 40 years (SD:13.1). Regarding the type of surgery, 36.6% was partial thyroidectomy, 60.7% was total thyroidectomy, and 2.7 % was completion thyroidectomy. Hypoparathyroidism found in the 1st post-operative day in 37.7%. this incidence was different according to surgery type, where it occurs in 3.4% in those whom surgery was partial thyroidectomy, 53.2% in total thyroidectomy cases, and 20% in completion thyroidectomy cases. All of cases were followed with PTH and Ca++ in 3 and 6 months. Persistent hypoparathyroidism in partial thyroidectomy case seen in one case only (1.5%). Persistent hypoparathyroidism in total thyroidectomy seen in 5.4%. None of those who underwent completion thyroidectomy developed persistent hypoparathyroidism. Delayed onset persistent hypoparathyroidism after normal post-operative PTH and Ca++ (113 cases), seen in 1 case only. The incidence of both transient and persistent hypoparathyroidism was different among genders; however, it was not statistically significant. In females, the incidence of transient hypoparathyroidism was 39.5% while in males it was 30.6%, while persistent hypoparathyroidism was slightly higher in males (5.6% vs 3.4% in females) (Table 1-2).
Discussion
Postoperative hypoparathyroidism is an ongoing and frequently underestimated complication in thyroid surgery. In total thyroidectomy transitory hypoparathyroidism is the most frequent complication and occurs in 16.5 to 71% of patients [1-4]. Most patients with a low postoperative PTH recover function quickly, but it can take up to 1 year for full resolution [5]. The majority of patients with parathyroid dysfunction after thyroidectomy return to normal function within a few weeks or 1 month of surgery [6,7]. In the English literature, only one study tackled the hypocalcemia in partial thyroidectomy. In that study there was a non-significant decrease in mean calcium concentration from the preoperative determination (9.1mg/dL) to postoperative day one determination (8.4mg/dL) and then a significant mean increases in the calcium concentration from postoperative day one to day seven (9.0mg/dL). There was no statistical difference between the mean preoperative calcium concentration and the day seven mean calcium concentration. therefore, the need for calcium replacement or prolonged hospitalization was generally not necessary [8].
Injury to the parathyroid gland during thyroid surgery may be due to direct trauma to the glands, injury to the feeding vessels, accidental removal of the glands during surgery, or intentional removal for oncologic purpose [9]. In situ preservation of parathyroid gland during surgery is important to reduce the risk of postoperative hypoparathyroidism and hypocalcemia. If parathyroid glands could not be preserved during surgery, they should be auto transplanted in case where the parathyroid glands are not preserved in situ to prevent postoperative hypoparathyroidism [10,11]. Transient hypocalcemia is more in patients with retrosternal goiter than patients with goiter limited to the neck. Attention should be given to localize parathyroid glands especially the inferior parathyroid glands and avoid injury to their blood supply during total thyroidectomy in retrosternal goiter [12].
Identifying all four parathyroid glands is not always possible even by experienced surgeon due to their variable anatomic position. Therefore, surgeons need to be aware that if they are not able to localize the parathyroid glands, they should search the resected thyroid gland for any removed parathyroid glands in order to perform autotransplantation [13]. In our study, the incidence of transient postoperative hypoparathyroidism occurs in more than half of cases of total thyroidectomy and was a common complication of hemithyroidectomy as will. Also, females have higher incidence of transient postoperative hypoparathyroidism than males. The recovery to normal occurs in most of the cases, more in females. Even hemithyroidectomy and completion thyroidectomy cases experienced temporary or persistent hypoparathyroidism, but in minority of cases. All cases of completion thyroidectomy recovered to normal, while only one case of hemithyroidectomy have persistent hypoparathyroidism.
Conclusion
Transient post-operative Hypoparathyroidism can occur even in hemithyroidectomy, and much more in those who underwent total thyroidectomy. Most of the post-operative hypoparathyroidism are improved within 1 months. Only few patients will need lifelong supplement. The risk of transient hypoparathyroidism as a complication of thyroid surgery was slightly higher in female patients, while persistent hypoparathyroidism was slightly higher in males.
References
- Gentileschi P, Gacek IA, Manzelli A, Coscarella G, Sileri P, et al. (2008) Early (1 hour) post-operative parathyroid hormone (PTH) measurement predicts hypocalcaemia after thyroidectomy: a prospective case-control single-institution study. Chir Ital 60(4): 519-528.
- Hermann M, Ott J, Promberger R, Kober F, Karik M, et al. (2008) Kinetics of serum parathyroid hormone during and after thyroid surgery. British Journal of Surgery 95(12): 1480-1487.
- Lindblom P, Westerdahl J, Bergenfelz A (2002) Low parathyroid hor-mone levels after thyroid surgery: a feasible predictor of hypocal-cemia. Surgery 131(5): 515-520.
- Pareed KD, Ananthprabhu K, Moosabba MS (2015) Intact PTH measure-ment 1 hour after total thyroidectomy as a predictor for patients at risk for developing symptomatic hypocalcaemia. Int J Biomed Adv Res 6(1): 11-14.
- Ritter K, Elfenbein D, Schneider DF, Chen H, Sippel RS (2015) Hypoparathyroidism after total thyroidectomy: incidence and resolution. Journal of Surgical Research 197(2): 348-353.
- Youngwirth L, Benavidez J, Sippel R, Chen H (2010) Parathyroid hormone deficiency after total thyroidectomy: incidence and time. J Surg Res 163(1): 69-71.
- Sitges-Serra A, Ruiz S, Girvent M, Manjón H, Dueñas JP, et al. (2010) Outcome of protracted hypoparathyroidism after total thyroidectomy. Br J Surg 97(11): 1687-1695.
- Cannon CR, Replogle WH (2008) Hypocalcemia following hemithyroidectomy. Journal of the Mississippi State Medical Association 49(9): 265-269.
- Maeda SS, Moreira CA, Borba VZC, Bandeira F, Farias MLF, et al. (2018) Diagnosis and treatment of hypoparathyroidism: a position statement from the Brazilian Society of Endocrinology and Metabolism. Arch Endocrinol Metab 62(1): 106-124.
- Luo H, Zhao W, Yang H, Su A, Wang B, (2018) In Situ Preservation Fraction of Parathyroid Gland in Thyroidectomy: A Cohort Retrospective Study. Int J Endocrinol 2018: 7493143.
- Teshima M, Otsuki N, Morita N, Furukawa T, Shinomiya H, et al. (2018) Postoperative hypoparathyroidism after total thyroidectomy for thyroid cancer. Auris Nasus Larynx 45(6): 1233-1238.
- Damiano G, Cocchiara G, Palumbo VD, Fatica F, Caternicchia F, et al. (2018) Latrogenic hypoparathyroidism after surgery for retrosternal goitre. A single centre retrospective analysis. Clin Ter 169(2): e67-e70.
- Gschwandtner E, Seemann R, Bures C, Preldzic L, Szucsik E, et al. (2018) How many parathyroid glands can be identified during thyroidectomy? Evidence-based data for medical experts. Eur Surg 50(1): 14-21.





























