Does Socioeconomic Status Affect the Time of Diagnosis of Prelingually Deaf Children?
Yazeed Al-Shawi1, Rayan Alfallaj2, Lulu S Aldhwaihy2, Amerah M Bin Zuair2, Mohammed Alobayli3 and Fida Almuhawas4*
1ORL-HNS Senior registrar at Prince Sultan Medical Military City and Otology/Neurology fellow at King Abdullah Ear Specialist Center, Riyadh, Saudi Arabia
2Medical Student, Collage of Medicine, King Saud University, Riyadh, Saudi Arabia
3Otorhinolaryngology, Head and Neck Surgery Senior Resident at King Saud Medical City, Riyadh, Saudi Arabia
4Assistant Professor at KSU, Consultant of ORL-HNS at KAUH, King Abdulaziz University Hospital, Saudi Arabia
Submission: July 18, 2019; Published:August 06, 2019
*Corresponding author:Fida Almuhawas, Assistant Professor at KSU, Consultant of ORL-HNS at KAUH, King Abdulaziz University Hospital, Saudi
How to cite this article: Yazeed A-S, Rayan A, Lulu S A, Amerah M B Z, Mohammed A, et al. Does Socioeconomic Status Affect the Time of Diagnosis of Prelingually Deaf Children?. Glob J Oto, 2019; 20(4): 556044. DOI: 10.19080/GJO.2019.20.556044
Abstract
Aim: Evaluate the impact of the SES of the family on the time of presentation, diagnosis, hearing aid fitting, and decision for CI in children with congenital SNHL.
Material and Methods: Retrospective cross- sectional study on 221 Patients with SNHL. using convenient sampling technique, we include all patients who presented to CI committee and fulfilled our inclusion and exclusion criteria
Results: The results of the analysis revealed that low SES group showed delayed presentation to the hospital for audiological testing and hearing aid fitting, as well as to the CI committee discussion compared to the average and good SES groups (p <0.05).
Conclusion: Even in government (free of charge) hospitals, low SES might delay seeking implant surgery, thereby affecting the post implantation performance of such patients.
Keywords: Socioeconomic Status; Sensorineural Hearing loss (SNHL); Cochlear Implant (CI); Delayed Presentation; Deafness
Abbrevations: SNHL: Sensorineural Hearing Loss; CI: Cochlear Implants; SES: Socioeconomic Status IRB: Institutional Research Board; SPSS: Statistical Package for Social Sciences; JCIH: Joint Committee on Infant Hearing; IRB: Institutional Research Board
Introduction
The incidence of sensorineural hearing loss (SNHL) in children is approximately 1 in 1,000 worldwide. An early diagnosis of congenital hearing loss is crucial to avoid speech and language delay [1]. Digital hearing aids and cochlear implants (CI) have been reported to help attain functional hearing in many deaf children [2,3]. CI is an effective tool that enables deaf children to develop communication skills and improve auditory-oral performance and is beneficial for higher academic achievement and quality of life [1,4,5]. Socioeconomic status (SES) is widely considered to be one of the main determinants of the quality of health [6]. Despite the high SNHL prevalence among children from low SES families, studies have shown that deaf child from high SES families are more likely to receive CI than are children from low SES families [1,7]. Furthermore, other studies have suggested that high SES parents tend to be more self-efficient and capable of providing the optimal care for their children with SNHL[6,8,9]. On the other hand, high SES children tend to have lower complication rates compared to low SES children. Moreover, low SES families tend to be less compliant with post-implant follow-ups, which are considered to be one of the main determinants of CI outcomes [1]. The significance of this study is to evaluate the effect of the socioeconomic status of the family on multiple aspects of cochlear implant journey despite the equality in the access to cochlear implant among all socioeconomics groups. This study aimed to determine the impact of family’s SES on multiple variables associated with CI, such as age of detection, diagnosis, and presentation to the CI committee
Methods
Objectives of the Study
The primary objective of this study was to evaluate the impact of family’s SES on age of presentation, diagnosis, hearing aid fitGlobalting and decision for CI in children with congenital SNHL. The secondary objectives of the study were as follows: (1) To examine our sample’s mean age of hearing loss suspicion, presentation to the hospital for audiological evaluation, hearing aid fitting, diagnosis, and decision for CI by the cochlear implant committee; to better understand the delays and time intervals between each step in the CI process.
Materials and Methods
Materials and Methods This cross-sectional, retrospective study was conducted at a tertiary hospital (King Abdullah ear specialist center at King Abdulaziz University Hospital), Riyadh, Saudi Arabia.
Study Sample
Subjects were 221 patients who met the study inclusion and exclusion criteria. We included all patients who consulted the CI committee, between March 2016 and March 2018. The inclusion criteria for this study were pediatric patients with severe-to-profound, prelingual, bilateral SNHL who were presented to the CI committee for the first time. The exclusion criteria included the following: (1) adult patients; (2) patients who were presented for hearing loss of the second ear; (3) patients with unilateral SNHL; (4) patients who had developed language pre-implant; (5) presence of any psychological and neurological issues.
Data collection
Instruments
A self-designed data collection sheet was used to collect data via phone calls (obtained from parents or direct caregiver for children whose parents were deceased) and patients’ files. The data collection sheet were divided into two section : section A and section B. Section A included age of the presentation to the cochlear implant committee, gender, pre-implant language status, status of the other ear, hearing aid use and benefits and presence of anypsychological or neurological issues., section B included information about the study subject demographic information including SES of the family, family’s income.
Study Groups
Patients were classified into the following categories based on their total household income per month: (1) Low SES (below 5,000 Saudi Riyals); (2) Average SES (5,001–10,000 Saudi Riyals); (3) Above average SES: (10,001–15,000 Saudi Riyals); Good SES (more than 15,000 Saudi Riyals). patients were grouped based on housing type (Room, apartment, one-floored villa, full villa, and whether it was rented or owned). based on individual family member’s income per month (total income of the family/number of family members), patients were categorized into four groups: Low SES (below 1500 Saudi Riyal); Average SES (1,500-1,999 Saudi Riyals); Above average SES (2,000–2,499 Saudi Riyals); Good SES: (above 2,500 Saudi Riyals).
Statistical Analysis
The collected data were entered into Microsoft Excel and analyzed by using the Statistical Package for Social Sciences (SPSS). The ANOVA and Post hoc tests were used to examine significant associations between study variables. P-value less than 0.05 was considered statistically significant.
Ethical Consideration
Institutional research board (IRB) ethical approval was obtained from the Ethics Committee of the Faculty of Medicine. Participants were assured that the data would be kept confidential. The purpose of the study was fully explained to all patient relatives, and a verbal informed consent was obtained from them during the phone-call. Patient parents were also informed that they were free to withdraw participation at any point of the study and that their data will not be included in the study.
Results
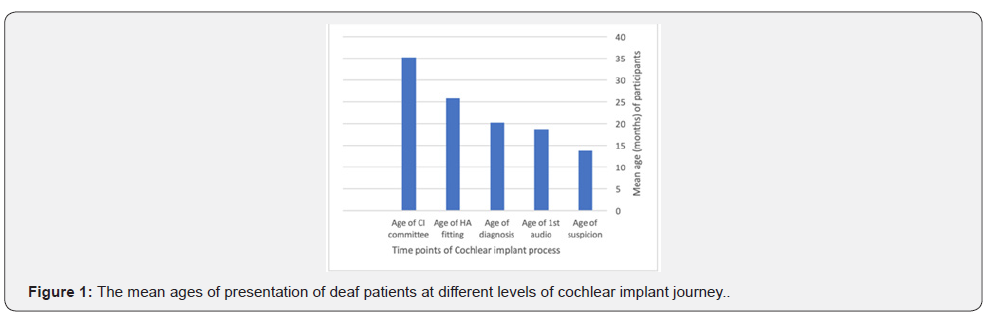
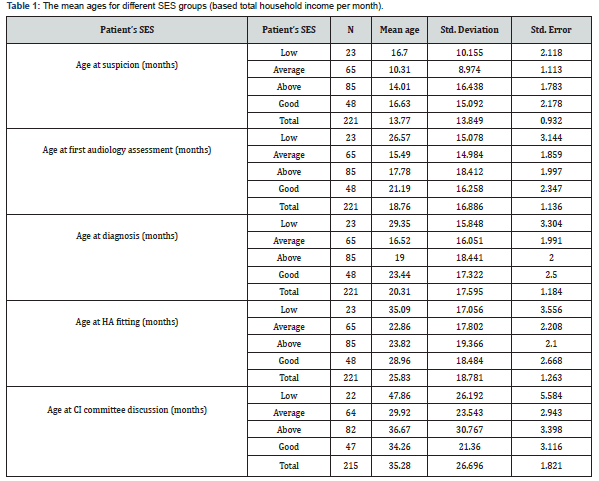
A total of 221 patients who met the inclusion and exclusion criteria were included in the analysis. Regarding patients’ family characteristics, 65, 85, 48, and 23 families were categorized into average SES, above average SES, good SES, and below average SES groups, respectively. Further, 85.1% of the fathers were currently working and the main earner of the family, while 72.4% of the mothers were housewives. Regarding education level, 54.8 % of the fathers and 49.5% of the mothers had a bachelor’s degree or higher. The mean ages at the onset of hearing loss, presentation to the hospital for audiological evaluation, hearing aid fitting, diagnosis, and discussion regarding CI at cochlear implant committee are shown in Figure 1. The mean ages of the different socioeconomic status groups are shown in (Table 1). The analysis of variance oneway (ANOVA) of patients’ ages showed significant between-group differences with respect to the age of first audiological testing (p= 0.034), diagnosis (p = 0.011), hearing aid fitting (p = 0.022), and discussion at CI committee (0.050). A post hoc test was performed to isolate specific group differences, and its results are shown in (Table 2).
Regarding the housing type of the patient families, 77 patients lived in a rented apartment, 27 patients in a rented villa, 21 patients in an owned apartment, 83 in an owned villa, and 13 patients lived in single rooms. With respect to the housing type, no significant difference in patients’ ages at onset of hearing loss, presentation to the hospital for audiological evaluation, hearing aid fitting, diagnosis, and discussion at CI committee were found. Regarding the income of individual family member’s income (Figures 2-5) a significant between-group difference was found for age at CI committee discussion (p = 0.014). A post hoc test was performed to isolate specific group differences, which showed that families with an income of less than 1,499 SR per member were found to significantly exhibit delay in hearing aid fitting compared to those with an income of more than 2,500 SR per member (a delayof 8.4 months; p = 0.035) and CI committee discussion (a delay of 16.2 months; p = 0.02l).



Discussion
Delaying the treatment for congenital deafness in children might affect their post-treatment performance in terms of auditory processing and speech intelligibility [3]. Therefore, identifying the factors that contribute to this delay is crucial [10]. Low SES has been found in the literature to play a rule in delaying the presentation to care centers, higher complication rates post implantation, less compliance with post-implant follow-ups and worse outcomes post implantation[11,12] Knowing that, The public health system in Saudi Arabia is free of cost, we aimed to study if low SES can still have a rule in delaying presentation to care centers which might contribute in delaying the onset of interventionand hence worse outcomes. In terms of patients’ mean ages at presentation, diagnosis, HA fitting, and decision to receive CI, we found that our patients fall behind the Joint Committee on Infant Hearing (JCIH) recommendations. As shown in (Table 2), when looking at the mean ages of presentation of deaf patient at different stages of assessment for cochlear implant candidacy patient of families from the low SES group were later than patient of families of the average SES group at the first audiological evaluation, diagnosis, HA fitting, and decision for cochlear implant at cochlear implant committee (11.1, 12.8, 12.2, 17.9 months, respectively), and were also late for diagnosis and HA fitting (10.3, 11.3 months, respectively) compared to those of families of the above average SES group.
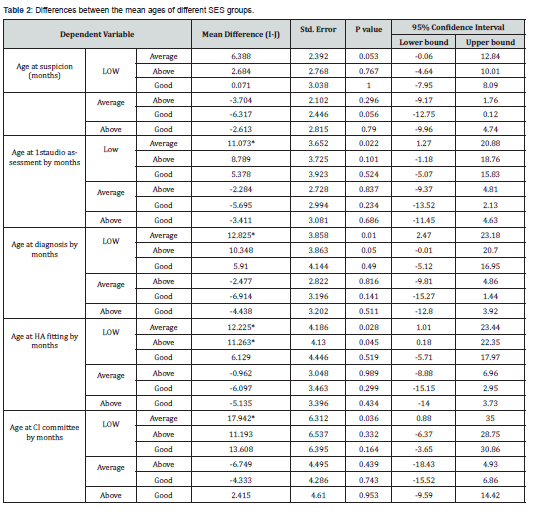
With respect to individual member’s income, a significant difference in the age of presentation to the hospital was found between low and good SES groups. The low SES group completed the CI process 16.2 months later than the good SES group. What is unique in our study that our study subject from different socioeconomic status groups were had an equal access to cochlear implant, however cochlear implant and audiology and rehabilitative speech services can be only provided in a tertiary care hospitals, therefore families who are living in peripheral cities away from these centers have to afford the transportation and temporary living measures costs which unaffordable by multiple families from low SES groups leading to increasing rate of missed follow up appointment and low rate of compliance to speech therapy courses affecting negatively the performance of CI children from thesegroups parents were asked about if they are compliant to speech therapy following implant and their satisfaction, one mother said: “we have to travel 1000 km and leave our jobs and children to reach to the hospital for my child speech course we can’t anymore afford these costs !”
Further, hospitals providing free healthcare services entail considerable time consumption and paperwork, whereas paid health services are more easily available to and affordable for families with better SES. Thus, the higher the SES level, the earlier the age of HA fitting. Another explanation for delayed treatment onset among low SES groups might be the high cost of living in a big city with accessible tertiary hospitals. This might be more expensive for low SES families given the travelling expenses due to frequenthospital visits. Future studies should examine this in more detail. Even in government hospitals, which provide free healthcare services, low SES might play a role in delay in seeking implant surgery, thereby affecting the post-implant performance in terms of language development of such patients. Different types of logistic support for families with low socioeconomic status might facilitate the process of early implant surgery for the patients. Future studies should examine the effect of different socioeconomic statuses using a larger sample size to better understand the relationship between the socioeconomic status and CI performance.
Key Messages
Low SES can still have a rule in delaying presentation to care centers.
Low SES group were later than patient of families of the average SES group at the first audiological evaluation, diagnosis, HA fitting, and decision for cochlear implant at cochlear implant committee.
c) Regarding the income of individual family member’s income, a significant between-group difference was found for age at CI committee discussion
Key Messages
Acknowledgement
The authors are grateful to Anas Alzahrani medical students for his contribution in data collection
References
- Stern RE, Yueh B, Lewis C, Norton S, Sie KCY (2005) Recent Epidemiology of Pediatric Cochlear Implantation in the United States: Disparity Among Children of Different Ethnicity and Socioeconomic Status. Laryngoscope 115(1): 125-31.
- Barajas C, González Cuenca AM (2016) Comprehension of texts by deaf elementary school students: The role of grammatical understanding. Res Dev Disabil 59: 8-23.
- Sharma S, Bhatia K, Singh S, Lahiri AK, Aggarwal A (2017) Impact of socioeconomic factors on paediatric cochlear implant outcomes. Int J Pediatr Otorhinolaryngol 102: 90-97.
- Meinzen Derr J (2009) Access to cochlear implant candidacy evaluations: Who is not making it to the team evaluations? AU - Wiley, Susan. Int J Audiol 48(2): 74-99.
- Stacey PC, Fortnum HM, Barton GR, Summerfield AQ (2006) Hearing- Impaired Children in the United Kingdom, I: Auditory Performance, Communication Skills, Educational Achievements, Quality of Life, and Cochlear Implantation. Ear Hear 27(2): 161-186.
- Kirkham E, Sacks C, Baroody F, Siddique J, Nevins ME, et al. (2009) Health Disparities in Pediatric Cochlear Implantation: An Audiologic Perspective. Ear Hear 30(5): 515-525.
- Sorkin DL, Zwolan TA (2017) Parental Perspectives Regarding Early Intervention and Its Role in Cochlear Implantation in Children. Otol Neurotol 29(2): 137-141.
- Chang DT, Ko AB, Murray GS, Arnold JE, Megerian CA (2010) Lack of Financial Barriers to Pediatric Cochlear Implantation: Impact of Socioeconomic Status on Access and Outcomes Pediatric Cochlear Implantation. Arch Otolaryngol Neck Surg 136(7): 648-657
- Geers A (2009) Background and educational characteristics of prelingually deaf children implanted by five years of age. Ear Hear 24(1): 2S-14S.
- Lu X, Qin Z (2018) Auditory and language development in Mandarinspeaking children after cochlear implantation. Int J Pediatr Otorhinolaryngol 107:183-189.
- Noblitt B, Alfonso KP, Adkins M, Bush ML (2018) Barriers to Rehabilitation Care in Pediatric Cochlear Implant Recipients. Otol Neurotol 39(5): e307-e313.
- Yehudai N, Tzach N, Shpak T, Most T, Luntz M (2011) Demographic Factors Influencing Educational Placement of the Hearing-Impaired Child with a Cochlear Implant. Otol Neurotol 32(6): 943-947.





























