Pleomorphic Adenoma Presented as Hard Palatal Mass: A Case Report
Lageju Nabin*
ENT consultant, Department of ENT-HNS, Nepal Police Hospital, Nepal
Submission: January 04, 2019; Published: January 12, 2019
*Corresponding author: Nabin Lageju, Department of ENT-HNS, Nepal Police Hospital, Nepal
How to cite this article: Lageju N. Pleomorphic Adenoma Presented as Hard Palatal Mass: A Case Report. Glob J Oto, 2019; 19(1): 556004. DOI: 10.19080/GJO.2019.19.556004
Abstract
Objective: To consider one of the differential diagnoses of palatal mass as pleomorphic adenoma
Case presentation: 21-year-old female patient presented in ENT department with painless mass in right side of hard palate for 2 years which was gradually progressive and slight discomfort on tongue movement and chewing food which on examination found to be 2*2cm swelling in right hard palate with normal overlying mucosa. On radiological examination, there was heterogenous swelling with intact hard palate. With provisional diagnosis of pleomorphic adenoma, excision of mass with overlying mucosa and periosteum was done. Histopathological report confirmed the diagnosis.
Keywords: Palatal mass; Pleomorphic adenoma; Excision
Introduction
Pleomorphic adenoma is the most common salivary gland tumours accounting for 40-70% of all major and minor salivary gland tumours [1]. It is also commonest minor salivary gland benign tumours accounting 70% of all tumours [2]. Hard palate is the commonest site followed by upper lip, buccal mucosa, tongue, floor of mouth, retromolartrigone [3,4]. Common age of presentation is second decade of life [5] with slight female preference [3]. Presenting symptoms are painless slow growing mass without ulceration and surrounding inflammation which on palpation feels non-tender, firm, rubbery [6]. In this paper, we present a case of pleomorphic adenoma of minor salivary gland in hard palate who treated with wide local excision.
Case Report
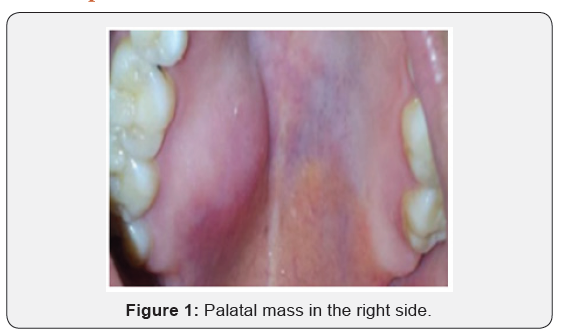
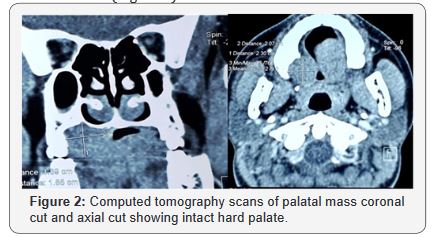
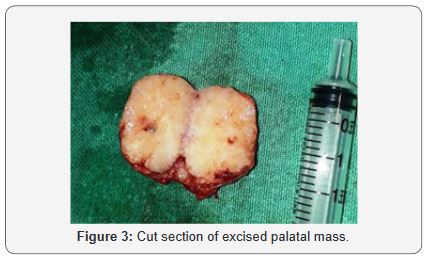
21 year old female patient presented in ENT department with painless mass in right side of hard palate for 2 years which was gradually progressive and slight discomfort on tongue movement and chewing food but there was no history of ulceration, bleeding, difficulty in swallowing, breathing and swelling in neck. On examination there was single swelling in the posterior part of the right hard palate measuring 2*2cm with normal overlying mucosa which on palpation firm, non-tenderand well defined swelling (Figure 1). On radiological investigation, there was solitary heterogenous swelling in the right hard palate without calcification and bony erosion. There was scalloping of bone of hard palate due to pressure effect (Figure 2). With all this finding provisional diagnosis of pleomorphic adenoma of hard palate was made and planned for surgical excision. Surgical excision of the mass was done in total along with the overlying mucosa and taking margin from surrounding mucosa. The wound was left open to let itself heal by granulation. The per-operative findings were 2*1.5cm single well encapsulated swelling in the hard palate extending to its posterior border and on cut section it was found to be yellowish white in colour (Figure 3).
Discussion
Pleomorphic adenoma has different embryological origin. It arises from both epithelial and mesenchymal origin. They arise from intercalated and myoepithelial cells. The mass is well demarcated from surroundings by fibrous capsule [6]. Formation of the capsule is a result of fibrosis of the surrounding salivary parenchyma which is composed of the tumor and is referred to as false capsule [7]. The pleomorphic adenoma is typically a well circumscribed, encapsulated tumor. The capsule may be incomplete which is more common in minor salivary gland tumours [8]. Most of the pleomorphic adenoma occurs in major salivary glands and parotid is the commonest. It is also the commonest tumour of minor salivary glands [9]. Palate has the highest number of minor salivary glands in upper aerodigestive tract [10]. So, palate is the commonest site of minor salivary gland tumours. It is followed by lips, buccal mucosa, tongue, retromolar area, pharynx, tonsils. In palate, most common location is posterolateral aspect [11].
The tumour is cellular with background stroma which can be mucoid, myxoid, cartilaginous or hyaline [12]. In “cellular” type of pleomorphic adenoma the epithelial element is dominant and “myxoid” type possess myxomatous element. Typical pleomorphic adenoma is of mixed type. Different epithelial cell types are spindle, clear, squamous, basaloid, cuboidal, plasmacytoid, oncocytic, mucous and sebaceous [13]. It can occur in any age group, but common presentation is in age group of 30-60 years with slight female predominance. Usual presentation of palatal pleomorphic adenoma is painless, slow growing smooth dome shaped [11], rubbery, submucosal mass without mucosal ulceration [14]. If ulceration present, it may be due to trauma or biopsy or malignancy. Due to expansion of mass against bone, there can be cupped out bone resorption [15,16].
Diagnosis of pleomorphic adenoma is based on history, clinical examination and histopathology. Computed tomography scan is an adjuvant diagnostic aid helpful in revealing about the size and extension of the tumour to the adjacent structures and to rule out bony involvement. Confirmatory diagnosis will depend on histopathological examination. Treatment of palatal pleomorphic adenoma involves wide local excision of the tumor together with clear margins involving the periosteum and associated mucosa, followed by curettage or excision of the underlying bone if involved to avoid recurrence. Palatal periosteom is an effective barrier to spread [16]. As simple excision of this tumour has high rate of recurrence, it is best avoided [6]. If palate needs to be excised, it needs to be closed with island flaps. Prognosis of palatal pleomorphic adenoma is usually good with cure rate of 95%, does not recur after adequate surgical removal. The risk of recurrence is low for tumours of minor glands [17]. Tumors with a predominantly myxoid appearance are more susceptible to recur than those with other features. Other causes of recurrence are pseudopodia, capsular penetration, and tumour rupture [18]. The risk of malignant degeneration into carcinoma ex pleomorphic adenoma is rare, occurring only in 5% of all cases [19].
Conclusion
Pleomorphic adenoma is one of differential diagnoses of palatal mass. Excision of mass with adequate margin is the treatment of choice.
References
- Jorge J, Pires F, Alves F, Perez D, Kowalski L, Lopes M, et al. (2002) Juvenile intraoral pleomorphic adenoma: report of five cases and review of the literature. International journal of oral and maxillofacial surgery 31(3): 273-275.
- Sahoo NK, Rangan MN, Gadad RD (2013) Pleomorphic adenoma palate: Major tumor in a minor gland. Annals of maxillofacial surgery 3(2): 195-197.
- Byakodi S, Charanthimath S, Hiremath S, Kashalikar JJ (2011) Pleomorphic adenoma of palate: a case report. Int J Dent Case Reports 1: 36-40.
- Spiro RH (1986) Salivary neoplasms: overview of a 35‐year experience with 2,807 patients. Head & neck surgery 8(3): 177-184.
- Austin JR, Crockett DM (1992) Pleomorphic adenoma of the palate in a child. Head & neck 14(1): 58-61.
- Mubeen K, Vijayalakshmi K, Pati AR, Giraddi GB (2011) Beningn pleomorphic adenoma of minor salivary gland of palate. Journal of Dentistry and Oral Hygiene 3(6): 82-88.
- Chau M, Radden B (1989) A clinical-pathological study of 53 intra-oral pleomorphic adenomas. International journal of oral and maxillofacial surgery 18(3): 158-162.
- Vellios F, Shafer WG (1959) Tumors of the intraoral accessory salivary glands. Surgery, gynecology & obstetrics 108(4): 450-456.
- Waldron CA, El-Mofty SK, Gnepp DR (1988) Tumors of the intraoral minor salivary glands: a demographic and histologic study of 426 cases. Oral Surgery, Oral Medicine, Oral Pathology 66(3): 323-333.
- Tian Z, Li L, Wang L, Hu Y, Li J (2010) Salivary gland neoplasms in oral and maxillofacial regions: a 23-year retrospective study of 6982 cases in an eastern Chinese population. International journal of oral and maxillofacial surgery 39(3): 235-242.
- Tian Z, Li L, Wang L, Hu Y, Li J (2010) Salivary gland neoplasms in oral and maxillofacial regions: a 23-year retrospective study of 6982 cases in an eastern Chinese population. International journal of oral and maxillofacial surgery 39(3): 235-242.
- Ogata H, Ebihara S, Mukai K (1994) Salivary gland neoplasms in children. Japanese journal of clinical oncology 24(2): 88-93.
- Kawahara A, Harada H, Kage M, Yokoyama T, Kojiro M (2002) Characterization of the epithelial components in pleomorphic adenoma of the salivary gland. Acta cytologica 46(6): 1095-1100.
- Mendenhall WM, Mendenhall CM, Werning JW, Malyapa RS, Mendenhall NP (2008) Salivary gland pleomorphic adenoma. American Journal of Clinical Oncology 31(1): 95-99.
- Rahnama M, Orzędała-Koszel U, Czupkałło Ł, Łobacz M (2013) Pleomorphic adenoma of the palate: a case report and review of the literature. Contemporary oncology 17(1): 103-106.
- Marx RE, Stern D (2012) Oral and maxillofacial pathology: a rationale for diagnosis and treatment: Hanover Park, IL: Quintessence Pub. Co.
- Sharma Y, Maria A, Chhabria A (2011) Pleomorphic adenoma of the palate. National journal of maxillofacial surgery 2(2): 169-171.
- Frable WJ, Elzay RP (1970) Tumors of minor salivary glands. A report of 73 cases. Cancer 25(4): 932-941.
- Chaudhari S, Hatwal D, Suri V (2013) Pleomorphic adenoma of hard palate: A report of four cases. International Journal of Case Reports and Images (IJCRI) 4(2): 90-94.
- Bradley PJ (2001) Recurrent salivary gland pleomorphic adenoma: etiology, management, and results. Current Opinion in Otolaryngology & Head and Neck Surgery 9(2): 100-108.





























