Foreign Bodies: Aspirated or Ingested? Our Experience About One Unusual Case
Matteo Cavaliere*, Rossella Cuofano, Carla De Santis, Maria Spagnuolo and Maurizio Iemma
Department of Otorhinolaryngology, University Hospital ,San Giovanni di Dio e Ruggid’Aragona, Italy
Submission: October 01, 2018; Published: October 09, 2018
*Corresponding author: Cavaliere Matteo, Via Madonna di Fatima 53-84084 Fisciano (Salerno), Italy.
How to cite this article: Matteo Cavaliere, Rossella Cuofano, Carla De Santis, Maria Spagnuolo, Maurizio Iemma. Foreign Bodies: Aspirated or Ingested? Our Experience About One Unusual Case. Glob J Oto, 2018; 17(5): 555973. DOI: 10.19080/GJO.2018.17.555973
Abstract
Foreign bodies in the aerodigestive tract are an important cause of morbidity and mortality and pose diagnostic and therapeutic challenges to otorhinolaryngologists. The ingestion and inhalation of foreign bodies occurs most commonly in children’s population, especially in their first six years of life. Children are naturally susceptible to be involved in foreign body injuries due to lack of molar teeth, the tendency to oral exploration and to play during the time of ingestion, and the poor coordination of swallowing. On the other hand, the elderly are those with thoracic neurological disease, decreased gag reflex due to alcohol seizures, stroke, Parkinsonism, trauma and senile dementia. Aspirated and ingested foreign bodies are often emergencies, leading to inadequate study and poorly prepared, improper attempts at removal. Only a small number of ingested foreign bodies perforate the esophagus and even a smaller fraction migrate extraluminally. Analysis of the literature revealed that an intraluminal penetrating foreign body carried a higher overall mortality than one that migrated extraluminally. Although intraluminal and extraluminal penetrating foreign bodies may remain quiescent for years before presenting a complication, no correlation existed between mortality and the duration of the foreign bodies’ retention. The greatest mortality was seen with vascular complications followed by diffuse and local suppurative processes. The accurate diagnosis of aerodigestive tract foreign bodies may be missed even by an experienced clinician. The delayed symptoms of foreign body in the aerodigestive tract may mimic other common conditions like asthma, recurrent pneumonia, upper respiratory infection and persistent cough. This study was done in our setting to describe our experience with endoscopic procedures versus surgery for the removal of foreign bodies in the aerodigestive tract, with a review of the pertinent literature.
Keywords: Foreign body; Aspiration; Ingestion; Upper aerodigestive tract
Introduction
Aspiration and ingestion of foreign bodies into the upper aero-digestive tract, either accidentally or deliberately, often constitute otolaryngologic emergencies[1-3]. As we encountered ourselves, foreign body aspiration is much more common in children, with a peak incidence in the third year. Oesophageal foreign bodies are more likely in adults. Both males and females are equally affected.More adults than children tend to have impaction of bones in the pharynx and oesophagus. Impacted coins, however, were more seen in children. Ingestion of dentures due to poor masticatory habits is usually seen in old age.In general, the treatment of a foreign body in the upper aero-digestive tract is a reasonably prompt endoscopic removal under conditions of maximum safety and minimum trauma [4].Patients usually present with history of swallowing a foreign body, dysphagia and/or odynophagia. Plain radiographs of neck, chest and abdomen identify radio-opaque foreign bodies, while fluoroscopy using thin barium may be required to delineate non-radio-opaque objects. Potential complications include oesophageal perforation, mediastinitis, cervical or mediastinal abscess, emphysema, oesophago-tracheal fistula and septic complications.
Case Report
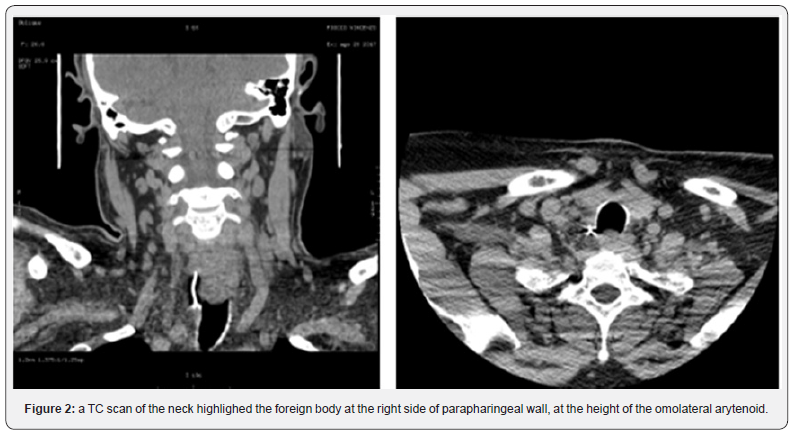
50-year-old men, V.F., presented to our ENT department due to a severe dysphagia that appeared about 5 days earlier after a fish-based lunch. The patient was convinced he had ingested a fish hook. The endoscopic evaluation of the high airways showed an important edema of the right arytenoid; the vocal cords were normal in form and motility, and no foreign body was visible. However, the X-ray of the esophageal-pharyngeal tract Figure 1 showed a suspected extraneous oesophageal body by ingestion of food and signaled, at C5-C6 level on right side of parapharyngeal wall, a 45 mm linear radiopac image. An integration with endoscopic examination was required. However, esophagogastroduodenoscopy was negative for the presence of foreign bodies,but it showed the presence of an extraneous granuloma at the level of the right arytenoid.In the same day, in general anesthesia, apanendoscopy of the superior aero-digestive tract was performed, which does not show any extraneous body at this level, except an important congestion of the right piriform sinus. At the end of the procedure, a nasal-gastric tube was due to a suspected perforation of the esophagus. At this point, the hypothesis that the right piriform sinus was been the point of entry of the foreign body became more and more concrete.A TC scan of the neck (Figure 2) was performed and it highlighted the foreign body at the right side of parapharyngeal wall, at the height of the homolateralarytenoid. Therefore, we decided to undergo a cervicotomicsurgery. In general anesthesia, cutaneous incision was performed along the margin of the sternocleidomastoid muscle, about 10 cm. The right thyroid lobe was found and lowered from the lateral wall of the trachea to the side wall of the esophagus, which had a millimetric puncture (foreign body output point). In the tracheo-esophageal sulcus, near the right recurrent nerve, the foreign body (metal wire about 5 cm in length) Figure 3 was found and removed.

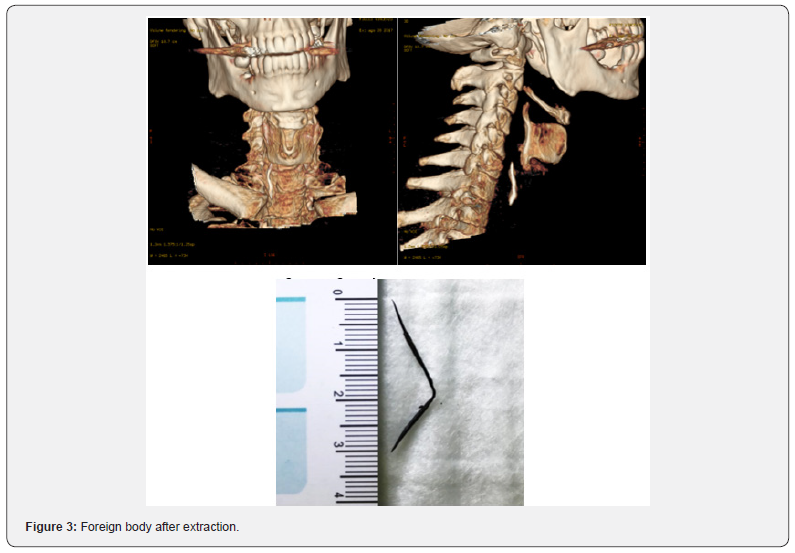
Results
The post-operative clinical course was devoid of complications, with the exception of a dysphonia, probably due to the functional damage from the recurrent right nerve stretch, to the adherence of the extraneous body to this area. The patient was resigned with the following output diagnosis:
a) Extraneous body (metal film) contained in the right tracheoesophageal sulcus;
b) Millimetric perforation of the side wall of the esophagus (input point of the foreign body)
c) Paresis of the right vocal cord.
At first postoperative control, paresis is still present, but the patient has no longer pain or dysphagia.
At the 3-month follow-up, after logopedic rehabilitation therapy, the dysphonia and the paresis had disappeared.
Discussion
The foreign body impaction is considering an emergent situation and it is defined as the presence of any object, material, or food that gets trapped in the upper aerodigestive tract, usually swallowed by accident or in some cases, intentionally. Some data [2,4] reports that around 100.000 of foreign body occur each year in the United States of America. This event can lead to high morbidity and mortality. It is estimated that between 1.500 and 1.600 patients die yearly due to foreign body and esophageal perforation being the most dreaded complication. Foreign body impaction in the esophagus can be a serious condition, which can have a high mortality among children and adults, if appropriate diagnosis and treatment are not instituted urgently. The literature [1-3]reveals that in adults foreign body impaction with food occurs more frequently, especially meat products, fish, or chicken bones. Among the pediatric population, coins and small batteries are the most common objects. An impacted foreign body should be removed as soon as the diagnosis is made, because:
a) the chance of spontaneous passage is less for an impacted object,
b) oedema due to local trauma tends to grip the object more firmly, making later manipulation increasingly difficult, and [3] perforation of the oesophagus is much more serious and dangerous complication[5].
Radiological imaging can allow the clinician to identify the radiopaque object and complications as esophageal perforation. There are various ways to achieve removal of a foreign body; these include nonendoscopic methods and endoscopic methods, which include flexible endoscopy versus rigid endoscopy. Majority of the foreign bodies do not need any kind of intervention or treatment, data reports that around 80 and 90% of the foreign bodies will pass from the esophagus to the stomach without any intervention, the remaining 10-20% will need endoscopic intervention, and 1% of the foreign bodies cases will require surgical intervention and this is the peculiarity and rarity of our clinical case. Foreign bodies, though having a low complication rate, error in diagnosis or the delay in the management of these situations can lead to very critical and life treating situations. The most severe of them is perforation of the esophageal wall, which can lead to mediastinitis, abscess, fistula formation, empyema, sepsis, and death.Foreign bodies trapped in the upper aerodigestive tract are a serious condition that can be fatal if they are not managed correctly. A correct diagnosis and treatment decrease the chances of complications. Whenever possible, endoscopic treatment remains the gold standard for extracting foreign body impaction. In most cases making an accurate diagnosis is simple, as patient presents with the history or has been witnessed, and other times it can be complex, especially in case of very small children or adult with dementia or mental retardation that may not be able to provide adequate history.
References
- Rodríguez H, Passali GC, Gregori D, Chinski A, Tiscornia C, et al. (2012) Management of foreign bodies in the airway and oesophagus. Int J Pediatr Otorhinolaryngol 76(1): S84-S91.
- MurtyP, IngleVS, RamakrishnaS, ShahFA, VargheseP (2001)Foreign bodies in the upper aero-digestive tract. J Sci Res Med Sci 3(2): 117- 120.
- Mosca S, Manes G, Martino R, Amitrano L, Bottino V, et al. (2001) Endoscopic Management of foreign bodies in the upper gastrointestinal tract: Report on a series of 414 adult patients. Endoscopy33(8): 692- 696.
- Sugawa C, Ono H, Taleb M, Lucas CE(2014) Endoscopic management of foreign bodies in the upper gastrointestinal tract: A review.World J Gastrointest Endosc6(10): 475-481.
- GarciaI, VaronJ, SuraniS(2016)Airway complications from an esophageal foreign body. Case Reports in Pulmonology.





























