The Forgotten Rambo Flap for Mastoid Cavity Obliteration
Mehrin Shamim*, Sumit Kumar Gaur and Sunil Narayan Dutt
Department of Otolaryngology and Head Neck Surgery, India
Submission: September 01, 2018; Published: September 07, 2018
*Corresponding author: Mehrin Shamim, Department of Otolaryngology and Head Neck Surgery, Bangalore, India.
How to cite this article: Mehrin S, Sumit K G,Sunil N D. The Forgotten Rambo Flap for Mastoid Cavity Obliteration. Glob J Oto, 2018; 17(4): 555966. DOI: 10.19080/GJO.2018.17.555966
Abstract
Background: Mastoid cavity resulting from a canal-wall-down (CWD) mastoidectomy causes major morbidity in the form of chronic discharge and infection in addition to difficulty in the fitting of hearing aids and giddiness. To overcome these problems, mastoid obliteration is recommended in many cases of canal wall down Mastoidectomy where the size of the cavity may turn out to be large.
Methods: This study demonstrates the authors’ technique of the Rambo flap for mastoid cavity obliteration performed in over 120 cases of CWD mastoidectomies.
Conclusion: The Rambo flap is an effective method of mastoid cavity obliteration that limits the size of the final mastoid bowl in CWD mastoid surgeries minimizing revision rates.
Keywords: Canal-wall-down (CWD); Mastoidectomy; Mastoid Obliteration; Rambo Flap
Introduction
The concept of obliteration of the mastoid cavity was first introduced by Mosher in 1911 to promote healing of a mastoidectomy defect [1]. Mosher originally used a superiorly based post auricular soft tissue flap. Kisch described the use of a pedicled temporalis muscle flap that was further expanded on by Rambo [2,3]. Popper described the use of a periosteal flap used to line, rather than obliterate the mastoid cavity [4]. Palva went on to describe a modification of Popper’s flap as a musculo periosteal flap to obliterate the mastoid bowl [5]. Palva further added the use of bone chips and bone pate´ in combination with a musculo periosteal flap [6]. In addition to bone pate´, other materials that have been described for mastoid obliteration include fat grafts, diced cartilage, fascia, bone chips, and ceramic materials such as hydroxyapatite [7-11].
Large Cavity Problems
The primary goal of surgical intervention for chronic ear disease is the development of a safe, dry, low-maintenance and hearing ear [12,13]. Exteriorization of attic, mastoid and middle ear with a CWD mastoidectomy has a high rate of success in achieving a safe and dry ear [12], but there is a need for continuous inspection of the cavity and a high incidence of moisture resulting in discharge [14], Persistent moisture, infection, and discharge may cause problems in as many as one-third of patients requiring revision surgery following CWD mastoidectomy [14], which may be attributed to mucosalized surfaces, persistent cell tracts, or poorly ventilated areas opening into the mastoid bowl [13].Despite careful observation of best practices including mastoid saucerization, removal of the mastoid tip, lowering of the facial ridge, and creation of an adequate-size meatus [15], moisture may still persist in areas of the mastoid bowl leading to stasis of mucoid exudate, localized areas of infection, and underlying mucosal changes. Open mastoid procedures have been criticized for the unfavorable cosmetic appearance due to a large meatoplasty, the need for regular cleaning, as well as the increased incidence of discharge and recurrent infections [13,16]. These concerns have led some to primarily advocate the use of Canal-Wall-Up (or Intact Canal Wall) mastoidectomies [15] or propose the reconstruction of the ear canal-mastoid partition [17]. or obliteration of the mastoid cavity [13,18-20].
Techniques for Mastoid Obliteration
Many techniques for mastoid obliteration have been described in the literature. Palva described a mentally based musculo periosteal flap in combination with the use of cortical bone chips and bone pate´ for mastoid obliteration [5,6]. Moffat and colleagues described the use of bone pate´ and a superiorly based temporalis mucoperiosteal flap for mastoid obliteration [21]. Some authors even advocated the use of mastoid obliteration for canal wall-up mastoidectomy in an attempt to prevent retraction pockets and recurrent cholesteatoma [22,23]. Montandon and colleagues described the use of cartilage to block the aditus and an abdominal fat graft for the canal wall-up mastoidectomy cavity [22]. Gantz and colleagues described reconstruction of the posterior canal wall and mastoid obliteration [24]. Their technique consisted of removal of the posterior bony canal wall with a micro sagittal saw. The mastoid cavity is obliterated with bone pate´ and bone chips followed by replacement of the posterior canal wall segment. An anteriorly based musculoperiosteal Palva flap is used to cover the obliterated mastoid cavity.
Some authors described the use of the Temporo Parietal Fascial Flap (TPFF) based on the superficial temporal artery for mastoid obliteration. East and colleagues and Cheney and colleagues [25,26] described the successful use of this TPFF flap for mastoid obliteration. It provides an excellent option when standard pedicled muscle or periosteal flaps are not available as in revision cases with scar tissue or in patients with previous irradiation. There are numerous reports in the literature, of the use of calcium phosphate ceramic granules and hydroxyapatite for mastoid obliteration. Hartwein and colleagues described the use of hydroxyapatite to obliterate the mastoid bowl while reconstructing the posterior canal wall with autologous conchal cartilage [27]. Yung and colleagues in their series describe 34 cases of mastoid obliteration using hydroxyapatite granules and an inferiorly based periosteal flap [28]. Proponents of the use of synthetic materials such as hydroxyapatite point out the minimal resorption of these materials over time [29]. Mahendran and colleagues describe the use of hydroxyapatite cement for mastoid obliteration [30]. In their study, however, there was a significant incidence of postoperative infection with 50% of the patients requiring revision surgery and removal of the foreign material (hydroxyapatite).
How we do it

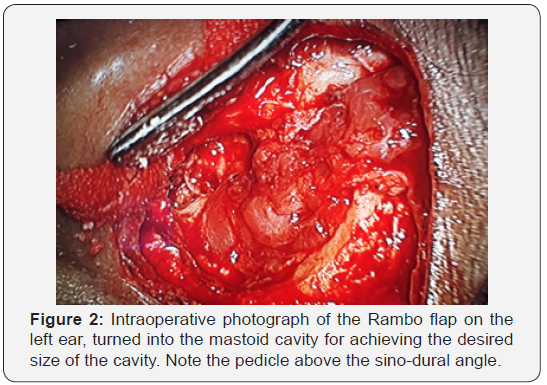
A post auricular incision 5 mm posterior to the post auricular groove is made. A thorough canal-wall down mastoidectomy is performed and saucerized, adequate lowering of the facial ridge and clearance of all mucosa and squamous epithelium in all the mastoid air cell systems is done. The temporalis muscle is exposed. A postero-superiorly based temporalis muscle flap is fashioned (Figure 1). The flap receives abundant blood supply mainly from the posterior deep temporal artery which courses upward and backward in the area of the muscle included in the flap. The flap is now rotated into the mastoid cavity and hence used to obliterate the cavity (Figure 2). The senior author has performed over 950 mastoid surgical procedures which includes about 360 canal-wall-down (CWD) mastoidectomies in a span of 25 years. He has used the Rambo Flap for obliteration of the cavity in about one third (about 120) of the CWD mastoidectomies where the final size of the cavities appeared too large and necessitated obliteration to reduce the size. The temporalis fascia is then placed over the flap and under the tympanic membrane remnant. An adequate meatoplasty is performed to facilitate good inspection of the thus reduced-size cavity.
Conclusion
In the modern era of ear surgeries, mastoid cavities due to canal-wall-down mastoidectomy are obliterated using various techniques and materials. In our experience, the Rambo Flap, described as early as 1958, is an effective method to obliterate the mastoid cavities in CWD mastoidectomies.
References
- Mosher HP (1911) A method of filling the excavated mastoid with a flap from the back of the auricle. Laryngoscope 21(12): 1158-1163.
- Kisch J (1928) Temporal muscle grafts in the radical mastoid operation. J Laryngol 43: 735-736.
- Rambo JHT (1958) Primary closure of the radical mastoidectomy wound a technique to eliminate postoperative care. Laryngoscope 68(7): 1216-1227.
- Popper O (1935) Periosteal flap grafts in mastoid operations S Afr Med J 9(3): 77-78.
- Palva T (1973) Operative technique in mastoid obliteration. Acta Otolaryng 75: 289-290.
- Palva T (1979) Mastoid obliteration. Acta Otolaryngol Suppl 360: 152- 154.
- Dornhoffer JL (1999) Surgical modification of the difficult mastoid cavity. Otolaryngol Head Neck Surg 120(3): 361-367.
- Estrem SA, Highfill G (1999) Hydroxyapatite canal wall reconstruction/ mastoid obliteration. Otolarngol Head Neck Surg 120(3): 345-349.
- D’arc MB, Daculsi G, Emam N (2004) Biphasic ceramics and fibrin sealant for bone reconstruction in ear surgery. Ann Otol Rhinol Laryngol 113(9): 711-720.
- Mills RP (1988) Surgical management of the discharging mastoid cavity. J Laryngol Otol Suppl 16: 1-6.
- Shea MC, Gardner G Jr, Simpson ME (1972) Mastoid obliteration with bone. Otolaryngol Clin North Am 5(1): 161-172.
- Gulya AJ, Minor LB, Glasscock ME, Poe D (2010) Glasscock-Shambaugh Surgery of the Ear. People’s Medical Publishing House.
- Nadol JB Jr (2006) Revision mastoidectomy. Otolaryngol Clin North Am 39(4): 723-740.
- Khalil HS, Windle-Taylor PC (2003) Canal wall down mastoidectomy: A long term commitment to the outpatients BMC Ear Nose Throat Disord 3: 1.
- Sheehy JL (1988) Cholesteatoma surgery Canal wall down procedures. Ann Otol Rhinol Laryngol 97(1): 30-35.
- Thiel G, Rutka JA, Pothier DD (2014) The behavior of mastoidectomy cavities following modified radical mastoidectomy. Laryngoscope 124(10): 2380-2385.
- Della Santina CC, Lee SC (2006) Ceravital reconstruction of canal wall down mastoidectomy Long-term results. Arch Otolaryngol Head Neck Surg 132(6): 617-623.
- Kurien G, Greeff K, Gomaa N (2013) Mastoidectomy and mastoid obliteration with autologous bone graft A quality of life study. J Otolaryngol Head Neck Surg 42(1): 49.
- Ramsey MJ, Merchant SN, McKenna MJ (2004) Postauricular periosteal-pericranial flap for mastoid obliteration and canal wall down tympanomastoidectomy. Otol Neurotol 25(6): 873-878.
- Mehta RP, Harris JP (2006) Mastoid obliteration. Otolaryngol Clin North Am 39(6): 1129-1142.
- Moffat DA, Gray RF, Irving RM (1994) Mastoid obliteration using bone pate Clin Otolaryngol 19(2): 149-157.
- Montandon P, Benchaou M, Guyot JP (1995) Modified canal wall-up mastoidectomy with mastoid obliteration for severe chronic otitis media. 57(4): 198-201.
- Vartiainen E, Harma R (1987) Mastoid obliteration in intact canal wall mastoidectomy. Clin Otolaryngol 12(5): 327-329.
- Gantz BJ, Wilkinson EP, Hansen MR (2005) Canal wall reconstruction tympanomastoidectomy with mastoid obliteration. Laryngoscope 115(10): 1734-1740.
- East CA, Brough MD, Grant HR (1991) Mastoid obliteration with the temporoparietal fascial flap. J Laryngol Otol 105(6): 417-420.
- Cheney ML, Megerian CA, Brown MT (1995) Mastoid obliteration and lining using the temporoparietal fascial flap. Laryngoscope 105(9 Pt 1):1010-1013.
- Hartwein J, Hormann K A technique for the reconstruction of the posterior canal wall and mastoid obliteration in radical cavity surgery. Am J Otol 11(3): 169-173.
- Yung MW (1996) The use of hydroxyapatite granules in mastoid obliteration. Clin Otolaryngol 21(6): 480-484.
- Gyllencreutz T (1992) Reconstruction of the ear canal wall using hydroxylapatite with and without mastoid obliteration and by obliteration with bone chips. Acta Otolaryngol (Stock) 112 (Suppl 492): 144-146.
- Mahendran S, Yung MW (2004) Mastoid obliteration with hydroxyapatite cement the Ipswich experience. Otol Neurotol 25(1): 19-21.





























