Effects of Cochlear Implantation on Vestibular Pathway: Follow up Study in Cochlear Implant Children
Nagwa M Hazzaa1, Adel I Abdel Maksoud1, Lobna H Khalil1*, Hassan A Wahba2 and Iman M Galal1
1Department of Otolaryngology, Audiology Unit, Ain Shams University, Egypt
2Department of Otolaryngology, Ain Shams University, Egypt
Submission: June 10, 2017; Published: June 21, 2017
*Corresponding author: Lobna H Khalil, Department of Otolaryngology, Audiology Unit, Ain Shams University, Abbasia st., Egypt, Tel: 00201095041332; Email: Hamedlobna@yahoo.com
How to cite this article: Nagwa M H, Adel I A M, Lobna H K, Hassan A W, Iman M G. Effects of Cochlear Implantation on Vestibular Pathway: Follow up Study in Cochlear Implant Children. Glob J Oto 2017; 8(4): 555743. DOI: 10.19080/GJO.2017.08.555743
Abstract
Background: Many researchers studied the risk of vestibular dysfunction following cochlear implantation (CI). However, they were focused mainly on adults. Yet there is a need to study such effect on children especially that they may have significant vestibular impairment before CI implantation.
Objectives: So this study aimed to investigate the effect of CI on vestibular pathway by measuring VEMPs in children undergoing CI before and after surgery. Also, to study the possible effect of electrical stimulation from CI on vestibular pathway.
Methodology: The study group included forty children undergoing CI and 20 healthy children as control group. Pre-operative evaluation included detailed history, air conduction- cervical and ocular vestibular evoked myogenic potentials (cVEMPs and oVEMPs). Follow up was done at 1st and 6th months postoperatively for the implanted ears. To study the effect of CI stimulation, follow up cVEMPs testing was done without the device and through it using Insert earphone at the microphone with the device on.
Results: Abnormal cVEMPs responses were more frequent (in 55% of cases) than abnormal oVEMPs (in 37% of cases). On Follow up, only 2 cases had deterioration in oVEMPs responses compared to 10 cases in cVEMPs. cVEMPs responses through the device were detected after 1st month in 7 (17%) cases which increased to 17 cases(42.5%) at 6th month. Six cases had cVEMPs responses through the device though they had absent cVEMPs without it.
Conclusion: The saculo-vestibular pathway is likely to be compromised after CI surgery in children. On the other hand, CI might be useful in stimulation of saculo-vestibular pathway.
Abbreviations: VEMP: Vestibular Evoked Myogenic Potentials; CI: Cochlear Implantation; VP: Vestibular Pathway; VEMP: Vestibular Evoked Myogenic Potentials; FNS: Facial Nerve Stimulation
Introduction
Recently, there has been a growing awareness of vestibular dysfunction in children with hearing impairment. Published reports have shown that vestibular dysfunction was found in 20-70% of children with hearing loss of different etiologies [1]. Although cochlear implantation is now considered an effective and safe procedure, the potential effects on vestibular function are of clinical concern [2].Several mechanisms had been proposed such as: traumatic implantation of the electrodes, pressure fibrosis by implanted electrodes or extra-cochlear electrical stimulation caused by the implanted electrodes [3].
Different consequences on vestibular function may occur from post-operative electrical current provided by the implanted electrodes. Abdelghaffar and Elshazly [4] reported infrequent vertiginous sensations or imbalance every time the device was activated. On the contrary, Cushing et al. [5] reported that electrical stimulation of the vestibular system could provide some usable vestibular cues. Most of the studies have focused primarily on the adult population. Moreover, pediatric CI candidates may already have significant vestibular impairment before implantation as a result of underlying inner ear pathology. Accordingly, this study was designed to investigate the effect of CI on vestibular pathway by measuring Vestibular evoked myogenic Potentials (VEMPs) in CI children before and after surgery. In addition to study the possible effects of electrical stimulation from CI on vestibular pathway.
Subjects and Methods
This study that was carried out in the Audiology unit, ENT department, Aim Shams University. The procedures followed? were ethically approved by the ENT Department Board. Caregivers/ parents of participated children in this study were informed and they gave their consent prior to the study.
Subjects
- Study group included forty children undergoing CI. They had severe to profound sensorineural hearing loss of different etiologies (25 females, 15 males). Their age ranged from 3 -14years (mean 5.7±2.5). All children underwent cochlear implantation with same operational technique by the same surgery team.
- Control group included twenty healthy children of matched gender (12 females, 8 males), age (4 -13years, mean 6.6±2.2) and had no history of ear symptoms , vestibular insult or neurological disorders. Exclusion criteria: children with preoperative neurological and visual disorders.
Methods
Preoperative evaluation
Detailed history was taken from all caregivers/ parents of both the study & control groups. It included: history of the motor milestones development, history of hearing loss, medical history, previous ototoxic/ vestibulotoxic drug intake and family history of hearing loss or consanguinity. Otologic examination and Middle ear functions were assessed using Madsen tympanometry model Zodiac 901. Air conduction cervical and ocular vestibular evoked myogenic potentials (cVEMPs and oVEMPs) were examined using four- channel evoked measuring system, ICS Charter EP 200.
Cervical VEMPs (cVEMPs): Gold surface electrodes were applied, with active recording electrode placed at upper third of sternocleidomastoid muscle ipsilateral to the stimulated ear, the reference electrode was placed on the upper sternum and the ground electrode was placed on the forehead. The skin was cleansed with alcohol prior to electrode placement. The electrode impedance was kept under 5 H. Monaural alternating 500Hz tone burst (rise/fall time = 1 ms, plateau time = 2 ms) were presented at 95 dBnHL using calibrated EAR 3A insert earphones at 5 Hz for 150 stimuli.
The response was amplified and bandpass-filtered from 10 Hz to 1 kHz with a recording epoch of 100 msec. Background electromyographic activity was monitored for consistent tonic contraction. Two traces from each side were obtained while the subject was sitting with the head rotating sideways toward one shoulder activate the sternocleidomastoid muscle. The initial positive negative biphasic waveform comprised peaks P13-N23. The latencies of peaks P13 and N23, amplitude P13-N23were measured.
Ocular VEMPs (oVEMPs): Gold surface electrodes were applied with active non-inverting electrode was placed 1 cm centered infra-orbital contralateral to the recorded ear and the reference electrode was placed on the chin. The ground electrode was placed on forehead [6]. The electrode impedance was kept under 5 H. The child was seated and instructed to keep his head at midline and gaze up at a fixed target (eg. stationary pictures or a toy) positioned 30 -35 degrees upward at the midline. Acquisition of about 100- 150 sweeps. The EMG signals were amplified and band pass filtered between 10 and 1000 Hz. Acoustic stimuli were the same as cVEMPs test. The analysis time for each response of 50ms.The initial negative positive biphasic waveform comprised peaks NI and PI. Two runs were performed. VEMPs were termed absent when the biphasic waveform was lacking. The latencies of peaks nI and pI amplitude nI-pI were measured.
Postoperative follow up
- Follow up cVEMPs and oVEMPs was done for the implanted ears of study group at the end of the 1st and the 6th month postoperatively.
- CVEMPs testing through the CI was done using same recording parameters but sound stimulation via Insert earphone was pointed at the the level of microphone of the sound processor when the device was on [7].
Statistical Analysis
IBM SPSS statistics (V. 22.0, IBM Corp., USA, 2013) was used for data analysis. Mean and Standard Deviation (SD) were calculated. Paired't' test was used for two dependent means, Student 't' test was used for two independent means with normal distribution while a comparison between two independent groups for non-parametric data was performed using Wilcoxon Rank Sum test. Ranked Spearman correlation test was used for non-parametric data. P<0.05 was considered significant. Chi- square test for correlation between qualitative data.
Results
Demographic data distribution: There was no statistical difference as regards age and gender distribution between control and study groups (P > 0.05). The most common cause of hearing loss was Heredofamilial (Table 1).

Preoperative findings: History of delayed walking was reported by the parents in (8/40)20% of cases. In addition four cases (10%) had difficulties while walking unsupported or in dim light and had repeated unexpected falls.
cVEMPs results: Abnormal cVEMPs was recorded in 22/40 (55%) children. In 15 children (37.5%) was bilateral and unilateral in 7(17.5%). Of the implanted ears, it was absent in 15/40 (37.5%) ears. Delayed latencies and/or lowered amplitude was in 7/40 (17.5%) ears. There was significant difference between control and the study group regarding cVEMPs parameters (P13 latency and P13-N 23 amplitude) (Table 2).
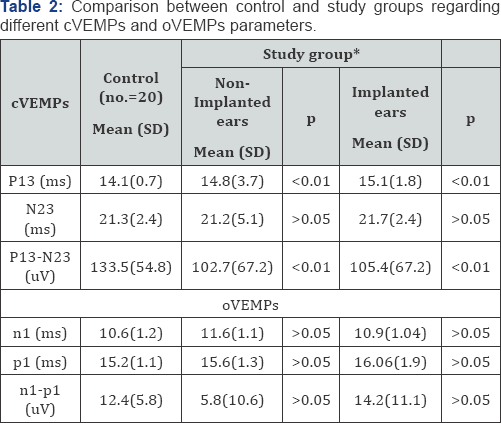
*Study group (no.): cVEMP (no.=40) oVEMP(no.=29)
oVEMPs results: The test was done for 29/ 40 of the study group. It couldn't be done in 11/40 (27.5%), younger age (3-4 years old), as they couldn't maintain the upward gaze efficiently to elicit the response. Abnormal OVEMPs was recorded in 11/29 (37.9%) children. In (8/29) children (27.58%) were bilateral and unilateral in 3 (10.34%).
Of the implanted ears, it was absent in 7/29 (24.13%) ears. Delayed latencies and/or lowered amplitude was in 4 (13.79%). There was no significant difference between control and the study group regarding mean of oVEMPs response (n1 latency and n1-p1amplitude) (Table 2). There was highly significant correlation between history of delayed walking symptom and abnormal cVEMPs responses (P=0.00) and with abnormal oVEMP responses (p=0.03).
Postoperative findings: The same 4 cases with imbalance preoperatively remained with the same complaint postoperatively. Additional case had postoperative imbalance with difficulty in walking in dim light and bicycling which started 3 months postoperative. For implanted ear, the responses were divided into unchanged (stable) response and changed.
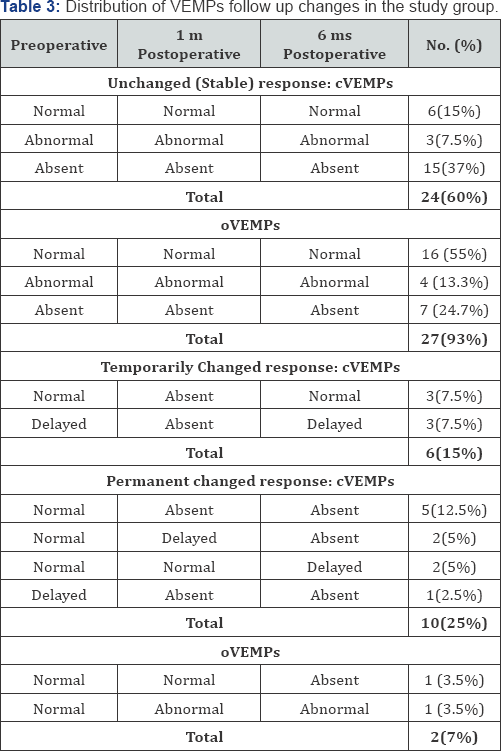
- CVEMPs responses were unchanged (stable) was in 24/40 ears (60%). Changed responses were found in 16/40 (40%). Six of them (15%) showed temporarily absent response that was recovered at 6th month, while the other 10 (25%) showed consistent absent response at 6th months postoperatively.
- OVEMPs responses were unchanged (stable) response in 27/29 ears (93.1%). Changed responses was only in 2/29 (7%) ears. Both had preoperative normal response. One of them had delayed response at 1st month postoperatively and the other had absent response at 6th month. Detailed distribution of oVEMP responses in the implanted ear pre and postoperatively (1 & 6 months) follow up are shown in (Table 3). There was no significant difference between preoperative, 1 and 6 months post-operartive VEMPs (oVEMPs and cVEMPs) parameters (Table 4).

Distribution of cases that had cVEMPs response through the CI Device
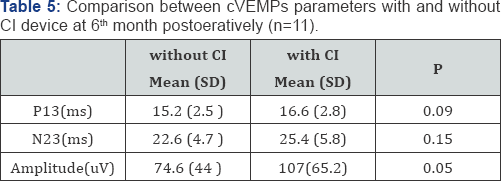
The total no of cases that had cVEMPs response through the device were 18/40 (45%). Six of them (15%) showed consistent response at 1 and 6 months pos-toperatively while eleven of them (27.5%) showed response at 6th month pos-toperatively. Only one showed response at 1st month that disappeared at 6th month. Interestingly 6 patients had response through the device although they initially did not have response without the CI. Facial nerve stimulation was reported in 7 cases, all of them had cVEMPs response through the device. There was no significant difference between cVEMPs parameters with and without the device (Table 5).
Discussion
Preoperative findings
Children with abnormal responses in vestibular tests would show delay in acquisition of gross motor function [8]. In current study, 20% of children with severe sensorineural hearing loss (8/40) had delayed walking as reported by their parents. In addition to four cases (10%) had difficulties while walking unsupported, or in dim light with repeated falls. These findings are In agreement with Masuda and Kaga [9] found that head control and independent walking were delayed in 28 of 97 (28.8 %) children with severe hearing loss. Also, Inoue et al. [8] found that children who showed abnormal responses in vestibular tests showed delay in acquisition of gross motor function in comparison with the normal hearing peers.
The vestibular nuclei provide consistent input to the postural muscle motor neurons particularly during initial postnatal development in the initial 6-12 months of life. The vestibulospinal reflex - through the lateral vestibulospinal tract acts by synapsing directly with motor neurons innervating extensor muscles and indirectly through spinal cord interneurons. Accordingly, the developmental milestones such as walking would be delayed with abnormal vestibular system particularly the vestibulospinal reflexes [10].
VEMPs findings
The current study showed that hearing impaired children with variable etiologies had VEMPs abnormalities, (55%) for cVEMPs and (37.9%) for oVEMPs. Abnormal bilateral responses were more frequent than unilateral abnormalities. The predominant abnormality was absent response. In addition CVEMPs parameters showed significant prolonged P13 latency and lower P13-N23 amplitude compared to the control group. While OVEMPs response parameters showed prolonged mean of n1 latency but did not reach the significant difference with the control group. These findings points to that saccular dysfunction was more frequent than utricular dysfunction. The overall findings was symptomatically reflected in (30%) of case as history of delayed walking or imbalance. Previous studies also found high percentage of abnormality in cVEMPs among hearing impaired children. Shall [10] found 21% of children demonstrated absent cVEMPs response unilaterally, while 67% of children showed bilateral absent response. Jin et al. [11] demonstrated that cVEMP response was abnormal or absent in 50% of cases. To the best of the authors knowledge, no studies was found concerned with oVEMPs in hearing impaired children, except for Xu et al. [12] who found 71% hearing impaired children (22 of 31) had preserved oVEMP response before cochlear implantation.
The high prevalence of vestibular impairments in hearing impaired pediatric patients was explained by the close anatomical and phylogenetic relation between the cochlea and saccule, where they are closely related in terms of innervation and vascular supply. They share the continuous membranous labyrinth of the inner ear and function by means of similar receptor cells. So, it appears plausible that, whatever the cause of damage to the cochlea, the same agent could probably also damage the saccule [13]. Hence, it is reasonable to presume that many children with hearing impairment have concomitant vestibular abnormalities [11]. Meanwhile, the saccule is more vulnerable than utricle for affection in cases with SNHL would be due to the anatomical & embryological proximity of the saccule to the cochlea. The vestibular disturbances are corrected through the process of compensation from proprioceptive, visual, and other sensory systems substitute for the absent peripheral vestibular input [14]. This may explain why only (30%) of cases had delayed walking or imbalance.
Postoperative findings
Vertigo or unsteadiness is not an uncommon adverse effect of CI as stated by several studies. Filipo et al. [15] reported postoperative vertigenous episodes in 12% of adult patients. Bonucci et al. [16] reported worsening in vestibular symptoms in 5% of adult patients. This didn't agree with the present study where vestibular complaint as an adverse effect of CI operation was not present. As postoperative complaints was found in the same 4 cases who had preoperative imbalance. They had the same abnormalities in cVEMPs and oVEMPs tests as preoperatively. Only one child complained of imbalance postoperatively. The child was presented with imbalance and also inability to ride bicycle as she was used to do preoperatively. These symptoms started 3 months postoperative. It is worth mentioning that she had same abnormal findings in cVEMPs & oVEMPs (bilateral absent responses). She developed blurring of vision and diminished visual acuity. So fundus examination was done revealed retinitis pigmentosa. The most probably diagnosis of this case was Usher's syndrome. From these findings CI couldn't be considered the main cause of deterioration in this case.
Postoperative findings of cVEMPs
In the present study, we have found stability of cVEMPs response in 60% and only 25% of children who have permanent deterioration in their respons in the 6th months postoperatively. Among them 8/ 40 (20%) had lost the response. There was non-significant difference between cVEMPs parameters among the cases at different test time among the cases with preserved response confirming the stability of their response post-implantation (Tables 4). The prevalence of postoperative vestibular hypofunction reported by previous studies ranged from 20 - 76% [16]. Studies as Ernst et al. [17] reported postoperative lost cVEMP responses in 42% of adult cases, where absence of cVEMP response changed from 36% preoperatively to 78% postoperatively. Bogle et al [18] demonstrated a change in the presence of the cVEMP response in children from 100% prior to implantation to 53% following surgery. Other studies reported less percentage of abnormality as Licameli et al. [19] showed postoperative absent response in 20% of cases. This wide range could be attributed to the variation among studies regarding the study group, types of electrodes, recording parameters and also operation technique.
This loss of response could be explained anatomically, as the saccule is the closest vestibular end organ to the basal turn of the cochlea, the location that research has previously demonstrated as the area most at risk for damage during implantation. This finding was in accordance with histopathological studies on temporal bones from patients who had been implanted during life. These studies demonstrated structural changes in the saccule mainly, followed by utricule, and semicircular canals [20]. However, the exact mechanism responsible for the vestibular deficits is not yet completely settled. We found that 6/40 (15%) of cases had temporarily absent cVEMPs response in our study. The response was absent in the 1st month but reappeared in the 6th month postoperatively. Similarly this temporarily absence response was found in 28.5% of cases [21]. After an initial impairment, the partial or complete recovery of the vestibular responsiveness with time could be explained by reversible and mild insults inflammatory process following the surgery or perilymphatic imbalance that didn't result in permanent damage in the saccule. So that cVEMPs results should be cautiously interpreted during early months post CI.
Postoperative results of oVEMPs
Unlike cVEMP, oVEMPs showed higher stability in (93%). Permanent deterioration at 6th month post operatively was noted only in 2cases (7%). Few studies assessed utricular function but by measures other than oVEMPs. Basta et al. [22] evaluated utricular function 2 days before and 6 weeks after surgery by Subjective visual vertical test. They found that it remained unchanged. The utricular function was also measured using off vertical axis rotation. Xu et al. [12] reported higher percentage of utricular abnormality measured by oVEMPs in cochlear implant cases. They found that 71% of cases with preserved response preoperatively, reduced significantly to 19.2%. They explained the presence of this high percentage of injury by the cochleostomy approach.
Postoperative cVEMPs response through the CI Sound processor
Since regular cVEMPs can’t discriminate exactly between end organ versus neural pathway abnormality, cVEMP through the CI device was done in an attempt to find out whether CI had an influence on the neural pathway; inferior vestibular nerve. Our study results revealed that 17/40 (42.5%) of cases had cVEMP response through the device at the 6th month postoperatively. One patient (2.5%) showed transient response at 1st month. Wave latencies and amplitude through the CI did not differ than regular cVEMPs. Regarding the influence of co-stimulation as a result of CI, there were no vertiginous symptoms during the study. However, 2 cases had complained of headache and 7 cases had facial nerve stimulation (FNS) when the device was turned on. All of them had CVEMPs response through the CI.
This was also found in Coordes et al. [7] study where 4 /26 (15%) of adult cases had CVEMP response through the CI sound processor. The mechanisms underlying this finding remain speculative. It could be explained by the electric co-stimulation to the vestibular nerve. With the CI turned off, only acoustic stimulation was delivered, but with the cVEMP through CI turned on the acoustic stimulation changed to electrical stimulation in the inner ear. So the cVEMPs response could be caused by the electrical current which probably stimulated the inferior vestibular nerve. They also suggested an interaction of the CI electrode with adjacent nerves as the electrical co-stimulation of the facial nerve. Intraoperative electrically elicited response of the vestibulo-spinal reflex by the CI electrode; cVEMP has been demonstrated by Basta et al. [22] study. They found that the threshold of the apical electrode was lower compared to threshold of the basal electrode. This supported the hypothesis of inferior vestibular nerve co-stimulation by the CI, where electrodes of the apical cochlear part are in close proximity to the nerve. This leads to the assumption that the current spread is seemingly more focused to the inferior vestibular nerve upon apical electrode stimulation.
The current study also noted that among cases who had response through the device, (2/7) in the 1st month and (6/10) in the 6th month, had no response on the regular cVEMPs. This was also found by Jin et al. [11] who reported that 4/12 children (33.3%) showed CVEMPs through cochlear implants activation. Among these four children, 2 showed no CVEMPs. In addition, Jin et al. [23] found that 10/20 children, who showed no cVEMPs response with the CI off, had cVEMPs responses through the CI. They suggested that the inferior vestibular nerve must be intact, although the functions of the saccule were lost in CI patients. In support to this, a human temporal bone pathological study demonstrated that Scarpa's ganglion cell count in the operated ear was the same as that in the non-operated ear; however, saccular collapse was only seen in the operated ear. Our study revealed that all cases suffered from FNS had CVEMPs response through the CI. So the presence of the FNS might predict the co-presence of the vestibular nerve stimulation. However, this needs further research.
Conclusion
Saculo-vestibular pathway is likely to be compromised after CI surgery in children. On the other hand, CI might be useful in stimulation of saculo-vestibular pathway. So we recommend that cVEMPs should be a part of the pre-operative evaluation of CI children and their monitoring post-operatively. Also, VEMPs results should be considered for the selection of implanted ear (affected ear).
References
- Tharwat T, Izquierdo P, Esquena J, Solans C (2004) Formulation and Stability of Nanoemulsions. Adv Colloid Interface Sc 108-109: 303-318.
- Debnath S, Satayanarayana, Vijay Kumar G (2011) Nanoemulsion-A Method to improve the solubility of lipophilic drugs. Int J Advances in Pharmaceutical Sci 2: 2-3.
- Shah P, Bhalodia D, Sheti P (2010) Nanoemulsion: A Pharmaceutical Review. Sys Rev Pharm 1(1): 24-32.
- Doh HJ, Jung Y, Balakrishnan P, Cho HJ, Kim DD (2013) A novel lipid nanoemulsion system for improved permeation of granisetron. Colloids Surf B Biointerfaces 101: 475-480.
- Chouksey RK, Pandey HK, Maithil A, Jain AK (2011) Nanoemulsion: A Review. Inventi Rapid: Pharm Tech 2(1): 1-23.
- Guilatt LR, Lambert G (2005) Cationic emulsion technology for lipophilic drug delivery. Drug Delivery report Autumn winter 71-72.
- Lawrence MJ, Reece GD (2000) Microemulsion-based media as novel drug delivery systems. Adv Drug Deliv Rev 45(1): 89-121.
- Eccleston J (1994) Microemulsions. In: Swarbrick J and Boylan JC (Eds.), Encyclopedia of Pharmaceutical Technology. Marcel Dekker, New York, UK, 9: 375-421.
- Kawakami K, Yoshikawa T, Moroto Y, Kanaoka E, Takahashi K, et al. (2002) Microemulsion formulation for enhanced absorption of poorly soluble drugs II. J Control Release 81(1-2): 75-82.
- Constantinides PP (1995) Lipid microemulsions for improving drug dissolution and oral absorption and biopharmaceutical aspects. Pharm Res 12(11): 1561-1572.
- Chouksey R, Jain AK, Pandey H, Maithil A (2011) Development and bioavailability studies of atorvastatin Nanoemulsion. Int J of Pharm & Life Sci (IJPLS) 2(8): 982-988.
- Baboota S, Shakeel F, Ahuja A, Ali J, Shafiq S (2007) Design development and evaluation of novel nanoemulsion formulations for transdermal potential of celecoxib. Acta Pharm 57(3): 315-332.
- Lakshmana Prabu S, Shnanawaz S, Dinesh Kumar C (2008) Compatibility Studies Between Duloxetine Hydrochloride and Tablet Excipients Using Thermal and Non-thermal Methods. J Pharm Res 7: 20-23.





























