Adenoidectomy- A Historical Review
Dilesh Mogre*
Speciality Medical Officer, Centenary Hospital, India
Submission: June 10, 2017; Published: June 28, 2017;
*Corresponding author: Dilesh Mogre, Speciality Medical Officer, Centenary Hospital, Govandi, Mumbai, India, Tel: 91-9987705784; Email: damogre@gmail.com
How to cite this article: Dilesh M. Adenoidectomy- A Historical Review. Glob J Oto 2017; 8(3): 555740. DOI: 10.19080/GJO.2017.08.555740
Abstract
The adenoids, also known as the Luschka's tonsil or the nasopharyngeal tonsil, is a mass of lymphoid tissue located posterior to the nasal cavity, in the roof of the nasopharynx. The adenoids along with the palatine and lingual tonsils are an integral part of the Waldeyer's ring, which represents 3 to 5 % of the entire lymphatic system.
Introduction
Adeno-tonsillar obstruction of the nasal airway not responding to conservative management is associated with significant morbidity and is an indication for surgery. Adenoidectomy with or without tonsillectomy is the typical management strategy for patients who fail medical line of management. Adenoidectomy was first performed using a ring knife through the nasal cavity by William Meyer in 1867 [1]. Since then the surgical approach to adenoids has evolved in terms of surgical methods, instruments and anesthesia techniques. The present study aims to review the history of adenoidectomy (Figure 1)
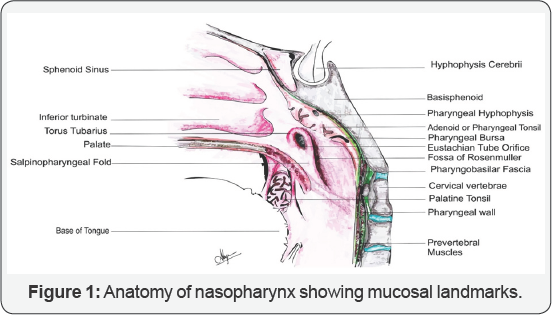
Through the ages
The chronic nasal catarrh is common presentation in children, but it was not realized that this was associated with sinonasal and nasopharyngeal pathologies. The hidden location of the adenoid had an impact on the historical timing of its discovery. In A.D 640 Paul of Aegina was credited with the treatment of projections in the nasal space and upper throat using a ligature passed trans-nasally this is the earliest description of surgery on the adenoids [2].The forgotten works of Conrad Victor Schneider of Wittenberg in the 1600's gave the first anatomical description of the pharyngeal tonsil. The anatomist Hubert von Luschka (1820-1875) in coined the term «pharyngeal tonsil"[3] . Professor Johann Czermak, in 1858, first demonstrated the possibility of the examination of the nasopharynx, by developing and demonstrating the method of performing posterior rhinoscopy after the invention of indirect laryngoscopy mirror [4] . He was the first to diagnose hypertrophic alterations around the tubal orifice and the first to realize that they were the cause of tubal malfunction.
Wilhelm Meyer in Copenhagen in 1867 while examining a young woman with deafness, receiving speech training but was not responding to treatment, noticed that she always breathed with her mouth open. After finding posterior rhinoscopy difficult he made digital examination of her nasopharynx and was very much astonished to find it almost entirely filled up by soft masses, completely blocking the posterior nares. He called them "adenoid vegetations" which felt like a bunch of earthworms, hanging down from the roof of the pharynx [5]. He designeda ring knife andperformed surgery on the patient with excellent results. During 1868 -1874 he described the hypertrophy of the pharyngeal tonsil or «adenoid vegetations» in detail and associated this finding with a syndrome characterized by mouth-breathing, snoring, a typical facial expression, deafness, recurring middle-ear affections, and characteristic alterations of speech. He based his conclusions on 5 year's experience with 175 observations in his office and on examination of 2700 children in Denmark and England [6].
Meyer treated the children suffering from adenoid vegetations with nasal douching, silver nitrate cautery and surgery. Meyer developed various instruments for adenoid resection. During the procedure patient was placed in sitting position with an assistant holding the head, and a basin held in front of the nose. The adenoid tissue were digitally palpated and a specially designed ring knife introduced through the nose while the application of the instrument was assisted trans- orally. The ring knife was moved in downward direction; so that its sharp edge crushes the vegetation off as near their base as possible, under the palpating finger. The surgery was associated with considerable bleeding often compelling suspension of the procedure and hemostasis achieved with cold water irrigation or chemical cauterization. Meyer was of opinion that the lateral layer of the growths is frequently resistant to resection and a single operative sitting rarely succeeded in complete resection. Considerable improvement in hearing and pronunciation with limited benefits in otorrhoea and tympanic perforation healing was observed in his studies.
Voltolini in Breslau in 1865 had observed a few cases of hypertrophy of the pharyngeal tonsil as «stalactite-like growths projecting into the free cavity of the naso-pharynx.» He was the first to treat them by galvanic cauterization. The operation of the adenoids was adopted very eagerly by a great number of nasal surgeons. Among the numerous special instruments that were invented for adenoid resection the most promising was the ring knife invented by Gottstein in 1886. Beckmann [7] in 1897, modified Gottstein's ring knife, and reported the resection of adenoids using on the curette. He performed around 5000 cases using the curette. Sir StClair Thomson developed the curette, and designed a cage, in which entangle the detached fragments of tissue and blood during adenoid resection. This adenoid curette is still used in the conventional curettage adenoidectomy.
This instrument and the surgery has undergone little or no further modification. Punch forceps and adenotome were also developed for adenoid removal. Besides these surgical developments, the use of cocaine for local anesthesia and ether for general anesthesia revolutionized adenotonsillar surgery. The development of general anesthesia was associated with the development of Davis-Boyle mouth gag [8]. This paved the way for the present day adenotonsillar surgery. In the early 20th century, the "focus of infection" theory correlated various systemic disorders to diseased tonsils and adenoids; thus, tonsillectomy and adenoidectomy was performed as a standard treatment for several different conditions such as anorexia, mental retardation and enuresis, or simply as a general measure to promote good health. Kwok & Hawke [9], 1987 initially introduced suction diathermy for hemorrhage control following conventional curettage of the adenoid pad. Subsequently, the whole procedure was performed with this technique, always along a trans-oral approach under indirect visualization by a laryngeal or dental mirror.
Traditional surgical teaching emphasizes on wide tissue exposure for identification of surgical landmarks and safe navigation through the surgical field without damage to surrounding tissues. Since early 1900's many surgeons advocated direct-vision adenoidectomy and assert that the adenoid recurrence was a result of incomplete and blindly performed adenoidectomy. Gyergyai of Budapest in 1910 visualized the post nasal space with a short tube, under topical cocaine anesthesia and Brunings's handle lamp. Sidney Yankauer an American otolaryngologist developed the nasopharyngoscope illuminated by the head-mirror; some authors describe transoral adenoidectomy under indirect vision by a laryngeal or dental mirror. Holmes's developed an electric nasopharyngoscope [10]. Joseph C Beck [11] introduced the method of improving intraoperativevisualization of the nasopharynx by retracting the soft palate with a small catheter introduced through the nose.
In a recent study published by Ark et al. [12] showed that in order to achieve a complete adenoid tissue removal, a direct or indirect visual assistance is necessary. The authors studied a group of patients that underwent conventional adenoidectomy in whom surgical efficacy was confirmed by digital palpation at the end of the procedure; subsequently, the nasopharynx was inspected using an indirect laryngeal mirror. Their finding was that only one-fifth of the patients had no residual adenoid tissue. Instead, in the 81% of the patients a residual lymphatic tissue was still present on the roof of nasopharynx; 11.4% of the patients had a residue along the torus tubarius on either side of the nasopharynx and in 6.3% the residual tissue was located at both cited sites. Dissatisfaction with the traditional curette adenoidectomy in adequately and safely achieving the clearance of adenoid tissue led to the development of alternative techniques that have been made possible by developments in fiber optics and powered instrumentation [13].
Development of Endoscopic Adenoidectomy
- Anatomical difficulties Wide distribution of adenoids; presence of deep fossae and depressions on the posterior wall; cervical spinal abnormalities.
- Adenoidectomy is often performed in a hurry, and sometimes the inadequate anaesthesia could be responsible for an insufficient relaxation of the palatopharyngeal muscles, whose contracture interferes with the manipulations of the adenoid pad.
- In many cases it is a “Surgical operation in the dark”, without visualization of the operating field [14].
In the 1990s, the advent of endoscopic sinus surgerypopularized the use of intranasal scopes and the endoscopicadenoidectomy became the natural evolution of the conventional adenoidectomy, permitting a direct visualization of operative field throughout the procedure. Becker in 1992 while evaluating a 12 year old child with persistent otorrhoea after a revision conventional adenoidectomy with tympanostomy tube placement; performed nasal endoscopy and found mass of adenoid tissue obstructing the Eustachian tube. They performed adenoidectomy under endoscopic vision with adequate lateral resection and the otorrhoea was treated in three months [15]. Canon et al studied 236 children undergoing adenoidectomy with the endoscopic technique. After performing routine transoral adenoidectomy a 2.7 or 4-mm 0 degree telescope was used transnasally, invariably, residual adenoid tissue was found after trans-oral adenoidectomy. The residual adenoid tissue was removed from the nasopharynx under vision. They advocated for use of "endoscope assisted adenoidectomy" as an adjunct to a more complete adenoidectomy [16].
Development of power assisted adenoidectomy
The original design of the microdebrider was patented by Urban in 1969 as a "vacuum rotary dissector". It was used by the House group in 1970 for morselizing acoustic neuromas, and then for arthroscopy. These devices were introduced for nasal surgery in 1994 by Setliff and Parsons [17]. As powered instrumentation became available for a variety of sinonasal procedures and allowed increased precision for performing complex procedures. These powered instruments were introduced for functional endoscopic sinus surgery in children for procedures such as nasal polyps, benign and malignant sinonasal tumors or base of skull lesions, choanal atresia and complicated adenoidectomies [18]. Power-assisted adenoidectomy conducted completely through a transnasal approach and under an endoscopic guidance was first reported by Yanagisawa in 1997 [19]. Koltai et al. [20] 1997 performed power assisted total or partial adenoidectomy with transoral approach along with an indirect visualization through a laryngeal mirror.
The microdebriders have the advantage of continuous suction of blood and dissected tissues out of the surgical field. Clearing the operating field of blood and other secretions is a must for greater visibility during nasal endoscopic surgery as even small amounts of bleeding can significantly impair visibility during endoscopic surgeries. As reported in the literature, the usual approaches to the power-assisted adenoidectomy are: pure transnasal both 0° scope and debrider are passed through the nasal cavity, transorally inserted curved debrider under a transoral control with laryngeal mirrors or with 45° or 70° scopes or transorally inserted curved microdebrider combined with a transnasal endoscopic control or a combination of these. A recognized disadvantage of power-assisted adenoidectomy is the increased patient charge associated with the disposable instrumentation. The elimination of pathological review of routine adenoid specimens may provide a means of offsetting the increased charge by 62% [21].
Plasma-mediated ablation (Coblation) has been recently introduced for adenoidectomyadapted fromarthroscopic surgery. It involves passing radiofrequency energy producing a plasma field at low-temperature (60aC to 70aC). This technology has sufficient energy to break organic molecular bonds, causing molecular disintegration of the tissue. A coblation wand, a bipolar probe, is used accurately to remove the tonsils and adenoid tissue. The ablation method is accompanied with minimal blood loss and damage to surrounding structures at low temperatures reducing postoperative pain and accelerated healing [22]. This present article provides a brief account of adenoid surgery across the ages. The changes in surgical approach and techiniques exemplifies the changing nature of surgical management adapting to the needs and expectations over time.
References
- Robb P, Peter R (2008) The adenoid and adenoidectomy. 3: 1094-1101.
- PEDERSEN PM (1957) Adenoidectomy: An Evaluation of the Original Technique. AMA archives of otolaryngology 66(5): 517-524.
- Tubbs RS, Shane Tubbs R, Payman V, Marios L, Shoja MM, et al. (2011) Hubert von Luschka (1820-1875) His life, discoveries, and contributions to our understanding of the nervous system. J Neurosurg 114(1): 268-272.
- Delavan DB (1929) The Centenary of Johann NepomukCzermak. Bull N Y Acad Med 5(5): 440-443.
- Thomson S (1914) Review of Vitto-Massei R. "Le AffezioniDell"Orecchio Nell' Adenoidismo (Aural Complications of Adenoids)'. The Journal of Laryngology, Rhinology, and Otology 223-224.
- Meyer W (1870) On Adenoid Vegetations in the Naso-pharyngeal Cavity: their Pathology, Diagnosis, and Treatment. Med Chir Trans 53:191-216.
- Feldmann H (1999) The nasopharynx and pharyngeal tonsil in the history of otology and rhinology. Pictures from the history of otorhinolaryngology, presented by instruments from the collection of the Ingolstadt Medical History Museum. Laryngorhinootologi 78(5): 280-289.
- Younis RT, Lazar RH (2002) History and Current Practice of Tonsillectomy. Laryngoscope 112: 3-5.
- Kwok P, Hawke M (1987) The use of suction cautery in adenoidectomy. J Otolaryngol 16(1): 49-50.
- Yearsley PM (1912) Yankauer's New Speculum for the Direct Examination of the Nasopharynx and Eustachian Tube. Proc R Soc Med 5(Otol Sect): 92-93.
- Guggenheim PPG (1952) THE ADENOID PROBLEM. Archives of Otolaryngology. Head and Neck Surgery 55(2): 146-152.
- Ark N, Nebil A, Hanifi K, SerifeUgur K, Turker Y, Ozboduroglu AA, et al. (2010) Comparison of adenoidectomy methods: Examining with digital palpation vs. visualizing the placement of the curette. Int J Pediatr Otorhinolaryngol 74(6): 649-651.
- Tolczynski B (1955) The recurrence of adenoids. Can Med Assoc J 72(9): 672-673.
- Becker SP, Nancy R, Dawn C (1992) Endoscopic Adenoidectomy for Relief of Serous Otitis Media. Laryngoscope 102(12): 1379-1384.
- Cannon C, Replogle WH, SchenkMP (1999) Endoscopic-assisted adenoidectomy. Otolaryngol Head Neck Surg 121(6): 740-744.
- Bruggers S, Seth B, Raj S (2009) Innovations in Microdebrider Technology and Design. Otolaryngol Clin North Am 42(5): 781-787.
- Parsons DS (1996) Rhinologic uses of powered instrumentation in children beyond sinus surgery. OtolaryngolClin North Am 29(1): 105114.
- Yanagisawa E, Weaver E (1997) Endoscopic adenoidectomy with the microdebrider. Ear Nose and Throat Journal 76(2): 72-74.
- Koltai PJ, Kalathia AS, Stanislaw P, Heras HA (1997) Power-Assisted Adenoidectomy. Archives of Otolaryngology. Arch Otolaryngol Head Neck Surgery 123(7): 685-688.
- Gillespie MB, Ingram F, Scarlett M, Hoy M (2003) Value-Based Approach to Power-Assisted Adenoidectomy. Ann Otol Rhinol Laryngol 112(7): 606-610.
- Glade RS, Pearson SE, Zalzal GH (2006) Coblationadenotonsillectomy: an improvement over electrocautery technique? Otolaryngol Head Neck Surg 134(5): 852-855.
- Timms MS, Ghosh S, Roper A (2005) Adenoidectomy with the coblator: a logical extension of radiofrequency tonsillectomy. J Laryngol Otol 119(5): 398-399.





























