- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
Objective Evaluation of Patients with Vestibular Disorders
Lalsa Shilpa Perepa*
Clinical Audiologist, Hearing First, Canada
Submission: April 22, 2017; Published: May 05, 2017
*Corresponding author: Lalsa Shilpa Perepa, Clinical Audiologist, Hearing First, 1995 Weston Road Unit B, Toronto - M9N 1X2, Canada,Email: lalsashilpa.311@gmail.com
How to cite this article: Lalsa S P. Objective Evaluation of Patients with Vestibular Disorders. Glob J Oto 2017; 7(4): 555716. DOI: 10.19080/GJO.2017.07.555716
- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
Introduction
Vestibular function tests are perceived as being less clinically useful than functional tests of the auditory system and, as a result, underestimate their full potential. Several factors contribute to this perception. The anatomy and physiology of the peripheral and central vestibular system are at least as complex as those of the auditory system, but audiologists in general possess less knowledge and interest in the vestibular system. For many years, audiologists considered it sufficient to separate peripheral vestibular problems from those of CNS origin, treating peripheral lesions and referring non peripheral lesions to neurologists. This no longer is sufficient; today knowledge of the visual and somatosensory systems also is necessary to complement that of the vestibular system if assessment of patients with dizziness or imbalance is to be complete. Proper understanding and interpretation of current tests designed to assess the contributions from all three sensory systems require detailed knowledge of the sensory and motor systems under investigation, as well as an appreciation of the strengths and limitations of each test.
The assessment of patients with balance disorders or dizziness has changed significantly over the past several years[1] . Technical improvements have resulted in the refinement of eye movement analysis (computerized electronystagmography (ENG) and led to the development of tests of rotation (rotary chair test) and standing balance / posture (computerized dynamic posturegraphy). This has broadened the audiologists's ability to assess not only the vestibular system, but also aspects of the visual and somatosensory systems. In some instances the clinical application has lagged behind the technical advances, which has made it somewhat difficult to detail the clinical usefulness of certain tests.
- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
Vestibular-Ocular Reflex (VOR)
- Causes eyes to move in the opposite direction to head movement
- Speed of the eye movement equals that of the head movement
- Allows objects to remain in focus during head movements
- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
Compensatory Eye Movements
VOR, Optokinetic reflex, Smooth pursuit reflex, Neck reflexes combine to stabilize object on the same area of the retina=visual stability. The VOR is mediated by a three-neuron arc.
For the horizontal VOR, these neurons include:
- the eighth cranial nerve (neuron 1),
- an interneuron that arises from the vestibular nucleus & terminates in abducens nucleus (neuron 2),
- The motor neuron to the eye muscles (neuron 3).
- A VOR followed by a rapid eye movement back to midline is vestibular nystagmus (Figures 1 & 2).
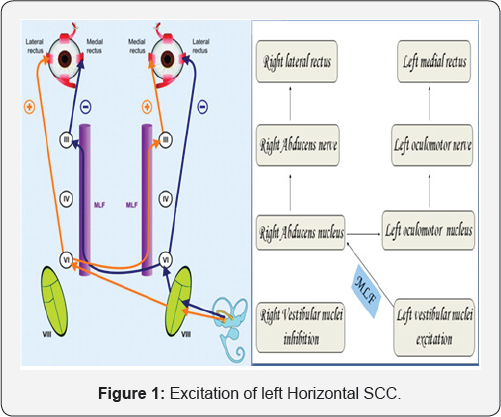
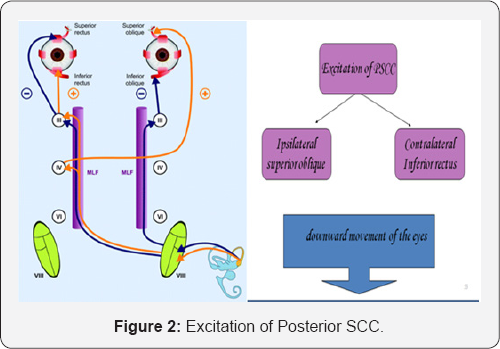
Activated by pitching the head upward and attempting straight ahead fixation (Figure 3) excited by pitching the head down, that is chin to the chest & attempting straight ahead fixation.

- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
Vestibulospinal Reflex (VSR)
- Generates compensatory body movement to maintain head and postural stability, thereby preventing fall
- VSR helps to maintain & regain postural stability during movement.
- It is an assemblage of several reflexes named according to the timing (dynamic vs. static or tonic) and sensory input (canal, otolith or both).
- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
Nystagmus
Nystagmus is a condition of involuntary eye movement, acquired in infancy or later in life, that may result in reduced or limited vision. There are two key forms of Nystagmus: pathological and physiological, with variations within each type. Nystagmus may be caused by congenital disorders, acquired or central nervous system disorders, toxicity, pharmaceutical drugs or alcohol. Previously considered untreatable, in recent years several pharmaceutical drugs have been identified for treatment of Nystagmus.
Diagnosis
Nystagmus is very noticeable but little recognized. Nystagmus can be clinically investigated by using a number of non-invasive standard tests. The simplest one is Caloric reflex test, in which one external auditory meatus is irrigated with warm or cold water or air. The temperature gradient provokes the stimulation of the horizontal semicircular canal and the consequent nystagmus. The resulting movement of the eyes may be recorded and quantified by special devices called electro nystagmograph (ENG), a form of electrooculography (an electrical method of measuring eye movements using external electrodes), or even less invasive devices called video nystagmograph (VNG), a form of video-oculography (VOG) (a video-based method of measuring eye movements using external small cameras built into head masks) by an audiologist. Special swinging chairs with electrical controls can be used to induce rotatory nystagmus.
Over the past forty years objective eye movement recording techniques have been applied to the study of nystagmus, and the results have led to a greater accuracy and understanding of the condition. Orthoptists may also use an optokinetic drum, or Electro oculography to assess their eye movements. Nystagmus can be caused by subsequent foveation of moving objects, pathology, sustained rotation or substance use. Nystagmus is not to be confused with other superficially similar-appearing disorders of eye movements (saccadic oscillations) such as opsoclonus or ocular flutter that are composed purely of fast-phase (saccadic) eye movements, while nystagmus is characterised by the combination of a smooth pursuit, which usually acts to take the eye off the point of regard, interspersed with the saccadic movement that serves to bring the eye back on target. Without the use of objective recording techniques, it may be very difficult to distinguish between these conditions. In medicine, the presence of nystagmus can be benign, or it can indicate an underlying visual or neurological problem.
Pathologic nystagmus
Pathologic nystagmus is characterized by a biphasic ocular oscillation alternating a slow eye movement, or smooth pursuit, in one direction and a fast eye movement, or saccadic movement, in the other direction. The velocity of the slow phase eye movement (SPEV) and the fast phase eyes velocity (FPEV) are related to each other and can be considered as a measurement of the efficiency of the system stimulus/response. When nystagmus occurs without fulfilling its normal function, it is pathologic (deviating from the healthy or normal condition). Pathological nystagmus is the result of damage to one or more components of the vestibular system, including the semicircular canals, otolith organs, and the vestibulocerebellum. Pathological nystagmus generally causes a degree of vision impairment, although the
severity of such impairment varies widely. Also, many blind people have nystagmus, which is one reason that some wear dark glasses.
Variations
Central nystagmus: It occurs as a result of either normal or abnormal processes not related to the vestibular organ. For example, lesions of the midbrain or cerebellum can result in up- and down-beat nystagmus.
Peripheral nystagmus: It occurs as a result of either normal or diseased functional states of the vestibular system and may combine a rotational component with vertical or horizontal eye movements and may be spontaneous, positional, or evoked.
Gaze Induced nystagmus: Itoccurs or is exacerbated as a result of changing one's gaze toward or away from a particular side which has an affected vestibular apparatus.
Positional nystagmus: It occurs when a person's head is in a specific position. An example of disease state in which this occurs is Benign paroxysmal positional vertigo (BPPV).
Post rotational nystagmus: It occurs after an imbalance is created between a normal side and a diseased side by stimulation of the vestibular system by rapid shaking or rotation of the head.
Spontaneous nystagmus: It is nystagmus that occurs randomly, regardless of the position of the patient's head.
Physiologic nystagmus
Physiologic nystagmus is a form of involuntary eye movement that is part of the vestibulo-ocular reflex (VOR), characterized by alternating smooth pursuit in one direction and saccadic movement in the other direction.
Variations
The direction of nystagmus is defined by the direction of its quick phase (e.g. a right-beating nystagmus is characterized by a rightward-moving quick phase, and a left-beating nystagmus by a leftward-moving quick phase). The oscillations may occur in the vertical, horizontal or torsional planes, or in any combination. The resulting nystagmus is often named as a gross description of the movement, e.g. downbeat nystagmus, upbeat nystagmus, seesaw nystagmus, periodic alternating nystagmus. These descriptive names can be misleading however, as many were assigned historically, solely on the basis of subjective clinical examination, which is not sufficient to determine the eyes’ true trajectory.
Opticokinetic nystagmus: A nystagmus induced by looking at moving visual stimuli, such as moving horizontal or vertical lines, and/or stripes. For example, if one fixates on a stripe of a rotating drum with alternating black and white, the gaze retreats to fixate on a new stripe as the drum moves. This is first a rotation with the same angular velocity, then returns in a saccade in the opposite direction. The process proceeds indefinitely. This is optokinetic nystagmus, and is a source for understanding the fixation reflex.
Postrotatory nystagmus: If one spins in a chair continuously and stops suddenly, the fast phase of nystagmus is in the opposite direction of rotation, known as the «post-rotatory nystagmus,» while slow phase is in the direction of rotation.
Nystagmus and Alcohol
In police work, testing for horizontal gaze nystagmus is one of a battery of field sobriety tests used by officers to determine whether a suspect is driving under the influence of alcohol. The test involves observation of the suspect's pupil as it follows a moving object, noting
- lack of smooth pursuit,
- distinct and sustained nystagmus at maximum deviation, and
- the onset of nystagmus prior to 45 degrees.
The field sobriety test studies published by the National Highway Traffic Safety Administration have never been peer reviewed and attempts to duplicate the study results have been unsuccessful. The horizontal gaze nystagmus test has been highly criticized and major errors in the testing methodology and analysis found. However, the validity of the horizontal gaze nystagmus test for use as a field sobriety test for persons with a blood alcohol level between 0.04-0.08 is supported by peer reviewed studies and has been found to be a more accurate indication of BAC than other standard field sobriety tests.
- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
Electronystagmography
Electronystagmography (ENG) is the diagnostic test used most commonly to assess patients with complains of dizziness or vertigo. It also is used for the detection and measurement of several eye movement aberrations such as visual fixation and suppression abnormalities, eye movement accuracy, velocity and latency deficits, breakup in the smoothness of visual pursuit, disconjugate eye movement, limitations in the range of ocular motion, and various forms of nystagmus.
The purpose of the ENG test is used- To detect the presence or absence of organic pathologic conditions within at least a portion of the vestibular system,
- To monitor change in vestibular function,
- To identify a general site of lesion limited to the peripheral or central vestibuloocular pathways, to include the ocular motor system.
- The ENG is used to detect disorders of the peripheral vestibular system (the parts of the inner ear that interpret balance and spatial orientation) or the nerves that connect the vestibular system to the brain and the muscles of the eye.
- The test may be performed if an individual is experiencing unexplained dizziness, vertigo, or hearing loss.
- Additional conditions in which ENG may be performed are acoustic neuroma, labyrinthitis, Usher syndrome, and Meniere's disease. If a known lesion exists this test can identify the actual site.
- The ENG is also useful in diagnosis of BPPV and bilateral vestibular loss.
- Inform patients that ENG may cause dizziness, nausea, or both.
- Patients should be advised to limit food intake prior to examination and arrange for transportation after the examination, which usually takes 1-1.5 hours.
The ENG procedure includes a battery of neurologic and otologic tests that have been used by physicians for many years [2] . The addition of ENG to these bedside tests provides objective documentation of the examination on a strip-chart recorder and allows for a more precise measurement of the response. The sensitivity and specificity of the various ENG subtests have been enhanced even further by the more recent computer-based ENG systems. In addition, the ENG procedure permits the clinician to record eye movements behind closed eyelids, thus enhancing the eye movement response by eliminating the effects of visual suppression.
The recording technique is rather straightforward. Surface electrodes are taped on the forehead, at the outer and inner canthi for horizontal recordings, and above and below one eye for vertical recordings. The electrodes should be positioned so that a straight line can be drawn through the electrodes to intersect at the center of each pupil. When the eyes move from the center of the socket to the right, the positive pole (cornea) of each eye moves closer to the electrode positioned at the right outer canthus and further from the electrode at the left outer canthus. Since the negatively charged retina also moves in a direction opposite that of the cornea, the difference in electrical activity is detected by the various electrodes. The resultant change in polarity is transmitted through the electrodes, where it is amplified by a recording device.
The clinical usefulness of ENG depends on several factors. For example, the ENG test procedure deals primarily with only one of the major vestibular tracts, namely, the vestibuloocular reflex (VOR). The overall ENG procedure fails to address the vestibulospinal tracts, which play an important role in the maintenance of balance and posture. In addition, stimulation of the vestibular end-organs, either by temperature change (caloric test) or by head/body acceleration (rotary chair test), is limited to the horizontal semicircular canals and superior branch of the vestibular nerves. The remaining semicircular canals (superior and posterior), otolith organs (utricle and saccule), and the inferior branch of the vestibular nerves are not stimulated directly with routine VOR test techniques. As a result, data generated from the various ENG subtests relate to only a portion of the peripheral vestibular system and do not address the vestibular system in its entirety. These limitations, accompanied by considerable variability in test administration and interpretation between clinics, have limited the overall effectiveness and general acceptance of ENG until recently, when more accurate and sensitive computer-based systems were introduced.
Although the information from the ENG battery is important, it must be evaluated in conjunction with the patient's history, symptoms, and other pertinent tests. The purpose of the ENG battery is not to diagnose or identify specific pathologic processes such as Meniere’s disease, acoustic neuroma, or multiple sclerosis. Rather, the test is used:
- To detect the presence or absence of organic pathologic conditions within at least a portion of the vestibular system,
- To monitor change in vestibular function, and
- To identify a general site of lesion limited to the peripheral or central vestibuloocular pathways, to include the ocular motor system.
The standard ENG test battery consists of a number of subtests. They include:
Gaze (fixation) test: The gaze, or visual fixation system, functions to stabilize visual fixation of an object on the fovea during fixed, visual gaze. The fovea is the retinal area of most distinct vision. The purpose of the gaze test is to identify the presence of random or spontaneous eye motion, primarily nystagmus, which interferes with the ability of the eyes to maintain visual fixation. Persons with normal gaze control ability can maintain ocular fixation indefinitely when looking at a fixed target in their visual field. Patients with abnormal gaze stability cannot. In conducting the gaze test, the patient is asked to fixate visually on stationary targets placed directly in front, 20 or 30 degrees to either side of center gaze, and 20 or 30 degrees above and below the central fixation point. If the patient's gaze fixation ability is compromised, either by an acute, unilateral, peripheral vestibular lesion or by a lesion in the brain stem or cerebellum, a spontaneous eye movement often results.
This eye movement usually takes the form of nystagmus, although other ocular movements also may be seen. When nystagmus is detected, its direction always is determined by the fast phase of the nystagmus «beat», (for example, the nystagmus is said to be right beating when the fast phase of the nystagmus is to the patient’s right). If a gaze nystagmus is present and its direction changes when the patient changes direction of gaze (for example, right-beating nystagmus with right-lateral gaze, left-beating nystagmus with left-lateral gaze, up-beating nystagmus with upward gaze), the lesion is likely to be isolated in the central nervous system (CNS), usually within the brain stem or cerebellum, and not in the peripheral vestibular system. This type of nystagmus is referred to as a direction-changing gaze nystagmus, where the gaze nystagmus «beats» in the same direction as the patient's gaze.
Conversely, if the gaze nystagmus beats in only one horizontal direction (right beating or left beating), irrespective of the patient’s direction of gaze, the nystagmus is probably caused by an acute, unilateral peripheral vestibular lesion. This is referred to as a direction-fixed gaze nystagmus and results from weaker neural output from one vestibular system compared with that of the opposite side. The asymmetry between the left and right vestibular systems creates a neural imbalance in the VOR that causes the eyes to be pulled (slow phase of the nystagmus) toward the weaker ear, followed by a rapid saccade (fast phase of the nystagmus) directed toward the stronger ear. As a result, a peripherally based vestibular nystagmus will beat horizontally, away from the weaker ear in most cases, and will not change direction even when the patient changes direction of gaze (Table 1).
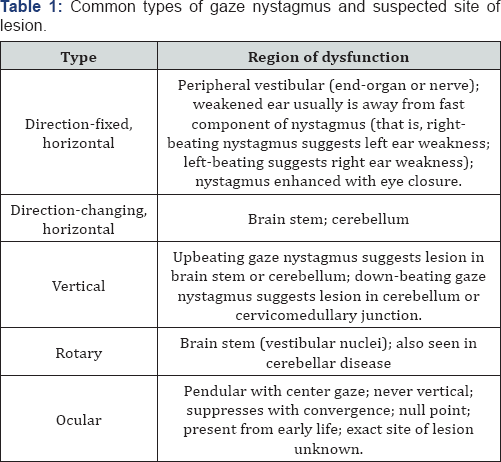
Saccade test: The saccadic eye movement system has at least two distinct functions. The first is to redirect the eyes from one target to another in the shortest possible time. This may be involuntary, as in the case of the fast phase of a nystagmus beat, or voluntary, from the desire to look to either side. The second function is refixation, when saccades correct the retinal position error by bringing the object to the fovea as quickly as possible.
In the saccade test the patient is asked to look between targets (dots on the wall or lights mounted on a light bar) on either side, as well as above and below the center gaze position. The targets are usually spaced 10 degrees from center gaze although this can vary depending on the purpose of the test. The patient looks rapidly between the targets, and the examiner inspects for eye movement accuracy. Inaccurate eye movements, where the eyes either undershoot or overshoot the target, is referred to as ocular dysmetria. Consistent undershoot (hypometric saccades) are abnormal and are seen frequently in patients with cerebellar dysfunction [3]. In certain instances, hypometric saccades may be seen in normal subjects [4] although a consistent finding of hypometric or hypermetric saccadic eye movement deserves further consideration. In addition to noting saccadic dysmetria on the recording device, hypometric and hypermetric saccadic eye movements also can be detected earily by watching the patient's eyes (Table 2).
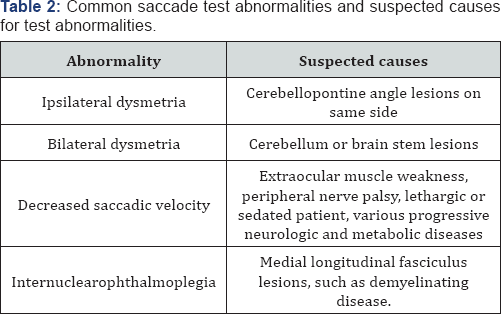
Ocular pursuit test: Ocular pursuit is one of the more important ocular motor systems. Its function is to stabilize a slowly moving object on the fovea by matching the angular acceleration of the eye with that of the moving object. During the pursuit test the patient is asked to watch a target that moves in a slow, sinusoidal fashion. As in the case with all ocular motor tests, the examiner should watch the patient’s eyes during this test in addition to recording the eye motion, and the patient should be tested under a condition of best corrected vision.
When a patient's visual pursuit system is impaired, rapid corrective eye movements replace the smooth pursuit movement so the eye can «catch up» with the moving target. When the catch-up movements form a «stair-step» pattern consisting of small saccadic movements, the defect is referred to as saccadic pursuit. Saccadic pursuit is seen frequently in patients with cerebellar disease.
Visual pursuit abnormalities are usually caused by lesions in the brain stem, cerebellum, or cerebral cortex. However, acute peripheral vestibular lesions that cause a spontaneous nystagmus also may affect the smooth pursuit test unilaterally and must be considered. In this situation a unilateral pursuit tracing abnormality may be secondary to a peripheral lesion when there is no actual deficit within the pursuit per se. It is important to note that breakup of the pursuit smoothness may result from visual clutter or distraction behind the pursuit target. Therefore a clear, clutter-free background should be present to eliminate any extraneous visual cues. Despite these test artifacts, ocular pursuit provides useful information for detection of ocular motor or central vestibular lesions and is one of the more sensitive tests for CNS dysfunction within the ENG battery (Table 3).
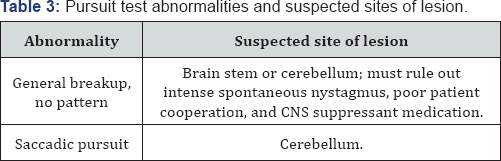

Optokinetic test: The purpose of the optokinetic test (OKN) system is to maintain visual fixation when the head is in motion. The OKN system complements the vestibular system in this regard but functions primarily at frequencies lower than those of the vestibular system. It also functions during more sustained head movements whereas the vestibular system, through the VOR, functions during the quick, short-lived head movements. The OKN test is performed by having the patient fixate visually on horizontal and vertical moving stripes or objects, usually from an OKN drum or a light bar. This task creates a nystagmus similar to that obtained during head rotation or following caloric irrigation. OKN abnormalities may include an asymmetric nystagmus response, a low amplitude response, or poor nystagmus wave-form morphology.
OKN abnormalities are noted in lesions affecting the ocular motor pathways of the brain stem and cerebral cortex. Although most OKN abnormalities are secondary to slow phase (pursuit) deficits, they can also be caused by fast-phase (saccade system) pathologic conditions. Isolated OKN abnormalities are thought to reflect cerebral cortex disease, and when they appear in conjunction with a direction-changing gaze nystagmus, they are thought to represent brain stem or cerebellar dysfunction [2]. When the lesion is in the brain stem, an abnormal OKN response is more commonly asymmetric not because of dysfunction within the OKN system, but because of the presence of the gaze nystagmus. Similarly, a spontaneous nystagmus generated from an acute, unilateral peripheral vestibular lesion also can cause an OKN asymmetry that is dominant in the direction of the fast phase of the spontaneous nystagmus.
Static positional test: The purpose of static positional testing is to determine if changes in head position create nystagmus or modify already existing nystagmus. The test is conducted with the patient's head and body placed in several positions and with eyes closed. Eye closure is necessary to eliminate the effects of visual suppression on potential nystagmus. Nystagmus that is present with eyes closed during static head positions (sitting, supine, supine-head right, supine-head left, and supine-head hanging) indicates organic disease although the site of lesion could be central or peripheral. In other words, persistent nystagmus that is present behind closed eyes in any or all head positions is considered «nonlocalizing» with reference to site of lesion.
When a nystagmus direction remains unchanged, even when the patient’s head position changes, this is referred to as direction-fixed positional nystagmus. When the nystagmus direction changes as the patient's head position changes, this is referred to as direction-changing positional nystagmus. Both types are non-localizing although static positional nystagmus in general is seen more commonly in peripheral vestibular disease than in central vestibular disease.
If a nystagmus is present behind closed eyes only in the sitting position, it is referred to as a spontaneous nystagmus. If the spontaneous nystagmus changes (intensifies or changes direction) when the head is moved into other positions, the patient is said to have a spontaneous and positional nystagmus. If the nystagmus is present only in head positions other than sitting, the patient is said to have a positional nystagmus alone. When a spontaneous nystagmus is present, the direction of the fast phase and the intensity of the slow phase should be noted. This allows the clinician to monitor changes over time. Nystagmus that beats toward the undermost ear is called geotropic, and nystagmus that beats toward the uppermost ear is referred to as ageotropic. It has been suggested that ageotropic nystagmus is seen more commonly in central vestibular disease, and geotropic is seen more commonly in peripheral vestibular disease. In reality, both types are caused by peripheral vestibular disease more often than central disease.
Dynamic positioning test: The most common type of true vertigo in adult patients is probably benign paroxysmal positional vertigo (BPPV). After the history, the test used to diagnose this condition is a dynamic positioning maneuver, the Dix-Hallpike test. This test should always be performed as part of the ENG test battery, especially when patients complain of motion-related vertigo. Although head position is important, this subtest is considered to be a positioningtest rather than a positional test. The final position of the head is important; however, it is the maneuver that places the patient’s head into the position that creates the response.
The phenomenon of BPPV was first described by [5] and popularized years later by Dix and Hallpike. These investigators discovered that by moving certain patients rapidly from a sitting to a head-hanging lateral position, they observed a burst of nystagmus accompanied by vertigo following a brief latency period after the final head position was reached. Repeat positioning maneuvers lessened the response until there was no response after several repetitions. When the investigators noted a positive response, the patient was said to have benign paroxysmal vertigo provided certain criteria were met.
The criteria used today for a «classic» Dix-Hallpike response include
- Subjective vertigo,
- A transient nystagmus burst,
- A gradual lessening in the severity of the nystagmus and vertigo when the maneuver was repeated (fatigue), and
- The response begins following a latency period of 1 to 10 seconds once the head reaches the final position.
If the response is determined to be classic, a benign peripheral vestibular lesion (BPPV) in the undermost ear is suspected. If the response is «nonclassic» (one or more of the above criteria are absent), the lesion is nonspecific as to site. The lesion can be either peripheral or central in this case. Although the pathophysiology remains in question, one common theory suggests that loose otoconia become dislodged and fall from the utricle into the ampulla of the posterior semicircular canal. This action creates a mechanical stimulation of the posterior semicircular canal cupula when the patient performs a specific head movement such as rolling over in bed, looking upward, or bending down. As noted above, this vertigo is arguably the most common type observed in patients from 40 to 70 years old. The hallmark of a classic Hallpike response is a rotary nystagmus without horizontal or vertical components. Keeping in mind the fact that a true rotary nystagmus cannot be detected on a strip- chart recorder, even with electrodes surrounding the eyes, the clinician should visually monitor the patient's eyes during the Dix-Hallpike maneuver [6] (Table 4).
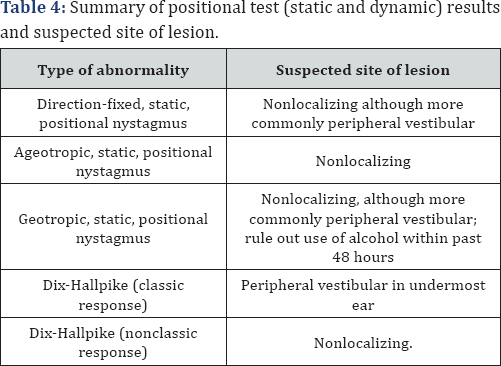
Caloric test: The bithermal caloric test is the oldest and most specific test within the ENG battery. The caloric test is a nonphysiologic procedure used to induce endolymph flow in the semicircular canals (primarily the horizontal canal) by creating a temperature gradient from the lateral to the medial part of the canal. The standard procedure stimulates only one labyrinth at a time, and the test results can be compared only within the same patient (one ear compared to the other). Several types of caloric stimulation are used clinically, including water (the most common), air, and closed low (water within a closed silicon balloon).
The test consists of having the patient lie on a table with the head anteroflexed 30 degrees. This position places the horizontal semicircular canals in a vertical plane. A thermal stimulus, usually water, flows into the external ear canal. Water temperatures of 30oC and 44oC are used with approximately 250 mL delivered over a 30-second period. When cold water is used, the temperature is transmitted to the wall of the horizontal canal, cooling the endolymph and causing the fluid to become denser as it falls in the vertically positioned canal. This sets up a fluid motion in the canal that deflects the cupula away from the utricle. The deflected cupula causes the resting neural discharge to drop relative to the opposite ear, creating a neural imbalance and resulting in a nystagmus with the slow phase toward the side of irrigation and the fast phase away from the irrigated side. The opposite occurs when warm water is used, causing the nystagmus to beat toward rather than away from the irrigated ear.
The period of maximum nystagmus activity is identified (usually occurring approximately 60 to 90 seconds after the irrigation begins) and measured. The right ear warm and right ear cool responses are summed and compared to the left ear warm plus left ear cool responses to determine if a unilateral weakness (UW) exists. Right-beating (right warm + left cool) responses are compared to left-beating (left warm + right cool) responses to determine if a directional preponderance (DP) is present. Inter ear differences of 20% and greater are considered abnormal for UW, and differences of 30% or greater are considered abnormal for DP.
Caloric abnormalities (unilateral or bilateral weakness) usually reflect peripheral lesions. In a small number of patients, a caloric abnormality may also reflect a brain stem lesion, although this is rare. DP is considered a nonspecific finding. In fact, most cases of DP simply represent either a spontaneous nystagmus or a positional nystagmus that is present in the caloric head position.
Failure of fixation suppression: During the caloric test, normal patients and those with peripheral vestibular disease should be able to suppress caloric-induced nystagmus by opening the eyes and fixating visually on a target. Patients with CNS pathologic conditions show little difference in the velocity of caloric-induced nystagmus whether their eyes are open or closed.
After the peak portion of the caloric-induced nystagmus is reached, the patient is instructed to open the eyes and fixate on a target. After the patient’s eyes are opened and fixed, the nystagmic amplitude drops significantly although the slow- phase nystagmic velocity remains at approximately 12 degrees/ sec. A reduction in the nystagmus velocity of at least 40% should be achieved when the patient’s eyes are open and fixed before fixation suppression is considered normal. Failure of fixation suppression (FFS) is a strong indication of CNS disease, usually within the cerebellum. Patients with FFS frequently have pursuit system deficits as well, most often showing saccadic pursuit.
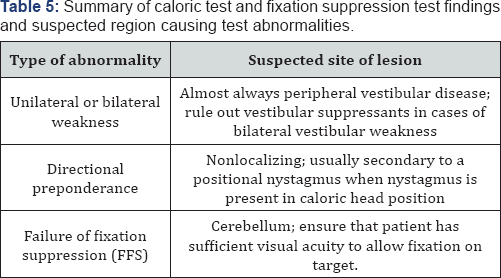
The clinician must ensure that the patient has sufficient visual acuity to clearly visualize the fixation target, so that each patient should be tested under best corrected vision with sufficient light available when the fixation target appears (Table 5).
- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
Risks of the ENG Procedure
- ENG is associated with minimal risks. Some people may experience dizziness or nausea during the test.
- ENG should not be used in individuals with pacemakers because the equipment may interfere with pacemaker function.
- Back or neck problems may be aggravated by rapid changes in position required for the test.
- The water caloric test may produce mild discomfort. Patients who have previously been diagnosed with a perforated tympanic membrane should not undergo the water caloric portion of the ENG test.
- Certain factors or conditions may interfere with ENG. These include:
- Earwax
- Impaired vision
- Frequent blinking
- Certain medications, such as sedatives, tranquilizers, and antivertigo medications.
- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
Rotational Tests
In addition to stimulation of the vestibular system by temperature change within the inner ear fluid (caloric test), a similar nystagmic response can be elicited by rotation of the head. In 1907 Barany described a manually driven rotary chair that produced observable nystagmic eye movements. Barany turned the patient, seated in the chair, from side to side and observed the patient's eye movements after the rotation stopped (post-rotary nystagmus).
Renewed interest appeared in the 1970s [7] based in part on the emergence of microprocessors and improved hardware. The torque-driven motors used to control the rotary chair improved dramatically as did the computer software that controlled the stimulus and measured the per-rotary nystagmus, a more sensitive parameter than the postrotary nystagmus used earlier. Because the acceleration and deceleration of a chair could be controlled more accurately, the subsequent compensatory eye movements could be measured more effectively.
The rotational chair system has several advantages over the standard caloric test:
- The rotational stimulus is less bothersome to the patient because it does not create the vertigo and nausea often associated with the caloric test.
- The mechanical artifacts associated with delivering the caloric stimulus to the inner ear (size and shape of the external ear canal, scarring, thickness, and cross-sectional area of the tympanic membrane; aeration of the mastoid; thermal transmission through bone and soft tissue; small but significant temperature changes in the caloric stimulus; and operator experience and skill) are not factors with the rotation stimulus. As a result, a more accurate stimulus response relationship is possible.
- The rotational stimulus is more natural than caloric irrigation because it attempts to simulate natural environmental motion. In addition, the nystagmus can be measured at various acceleration levels, enabling the vestibular system to be tested over a wider portion of its operating range.
- Multiple gradations of the stimulus can be presented in a short time period.
- Because the rotational stimulus is controlled more accurately and the response measured irrespective of the external ear canal and middle ear geometry, small changes within the VOR can be monitored more effectively.
The primary disadvantage of the rotary chair test is that it stimulates both labyrinths (horizontal semicircular canals and superior vestibular nerves) simultaneously. To determine the relative strength of the right and left horizontal semicircular canals, respectively, a caloric test must be performed. Three test parameters (phase, gain, and symmetry) are considered on most commercially available rotary chair systems. Phase of the rotation-induced compensatory eye movement is the temporal relationship between the velocity of the head (chair) and that of the slow-phase component of the rotation-induced nystagmus. At high frequencies of head movement, the eyes move in a precise compensatory manner, although 180 degrees out of phase.
At lower acceleration frequencies, the eye movement velocity leads or lags in reference to the chair velocity. Phase leads are inversely related to rotational frequency. As the acceleration frequency decreases, the phase lead increases. A low-frequency phase lead is exaggerated in many patients with central or peripheral vestibular pathologic conditions, and this phase lead will likely remain, even following compensation of unilateral vestibular lesions [7]. Phase is probably the most stable and repeatable parameter measured during the low-frequency rotary chair test provided gain is adequate, although its clinical significance is still somewhat obscure. With rotation to the right, a leftward compensatory eye movement occurs. A rightward eye movement occurs when the chair turns to the left.
The symmetry parameter of the rotary chair test reflects the peak slow-phase eye velocity when the patient turns to the right, versus the peak slow-phase velocity when the patient turns to the left. This parameter is usually expressed as a percentage although it may be expressed in degrees. It must be stressed that the symmetry measure is not a definite indication of laterality (side of the lesion); rather, it is similar to directional preponderance on the caloric test. In both cases the cause is often secondary to a spontaneous or positional nystagmus and, as a result, is nonlocalizing. In acute, unilateral peripheral vestibular disease, the fast phase of the spontaneous nystagmus usually beats away from the weaker ear. In this situation the rotary chair symmetry will indicate accurately a weakened response on the impaired side. In unilateral peripheral vestibular lesions where the spontaneous nystagmus beats toward the side of the disease (so-called irritative lesions), the rotary chair symmetry measure mistakenly will indicate that the normal ear is the involved side.
Lesions such as early Meniere's disease, serous labyrinthitis, labyrinthine fistulas, and occasionally, acoustic neuromas can cause irritative spontaneous nystagmus. Because the symmetry parameter seems to reflect central compensation to some degree, it is often normal in compensated, unilateral peripheral vestibular lesions. This observation is based on clinical evidence that shows the degree of asymmetry decreases as central compensation occurs. The improvement in symmetry in these cases likely reflects a decrease in the intensity of the spontaneous nystagmus, resulting in a decreased directional preponderance, another possible indication of central physiologic compensation following unilateral peripheral vestibular disease.
The gain parameter of the rotary chair test is the amplitude of maximum slow-phase velocity of the nystagmus compared with the amplitude of the maximum velocity of the rotating chair. In other words, the gain response is a ratio between the maximum eye velocity and the maximum chair velocity. At «natural» head movement frequencies (1 to 5 Hz), a gain of «1» indicates that the compensatory slow-phase eye movement velocity is equal and opposite the chair/head movement velocity. At lower chair/head velocities, the compensatory eye movement gain is generally less than the chair/head movement velocity. In other words, slow-phase eye movement velocity (in darkness) decreases when the head velocity decreases. Because gain is a performance parameter, abnormally low gain may indicate a pathologic condition. Of all the parameters measured during the low-frequency rotary chair test, however, gain appears to be the most unstable since it is related closely to the patient’s state of mental alertness. Because adequate gain is needed for the analysis algorithm used to calculate phase and symmetry, every effort must be made to keep the patient mentally alert.
In patients with acute, unilateral peripheral vestibular lesions, gain is likely to be depressed. This finding has been noted following disease and labyrinthectomy. Following central compensation, gain appears to recover somewhat, provided appropriate mental alertness is maintained. In bilateral peripheral vestibular lesions secondary to ototoxicity, gain decreases as the drug-induced damage increases, although changes in phase may be a more sensitive parameter than gain for monitoring purposes [1].
- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
Clinical Utility
Attempts have been made to identify the location of vestibular lesions based on patterns of phase, symmetry, and gain relationships. Although certain trends may appear, low frequency phase leads, asymmetries, and depressed gain can be seen both in peripheral and central vestibular lesions [2]. As a result, it is difficult to determine the exact site of lesion on a consistent basis from the parameter pattern generated during the low frequency rotary chair test.
The primary strength of the computerized rotary chair test appears to be its sensitivity to monitor change within the vestibular system, particularly in the early detection of bilateral peripheral vestibular disease [1]. Although disagreement continues about the low-frequency rotary chair test's ability to monitor physiologic compensation following a sudden, unilateral vestibular insult, some points are worth reviewing. For example, in an acute, unilateral vestibular weakness, an asymmetry will usually be present in the direction of the spontaneous nystagmus. In addition, gain may be depressed (primarily in the low frequencies) and a large phase lead should be seen. As central compensation occurs, the degree of asymmetry will usually decrease or resolve completely, and gain may improve to a degree as well. In contrast, the low-frequency phase lead appears to persist in most but not all patients [4,5]. Recall that abnormalities in the symmetry parameter are affected by spontaneous nystagmus and the gain parameter can be affected by patient alertnes and other extra vestibular factors during low-frequency acceleration [3]. For these reasons the clinical significance of gain and symmetry (as well as phase) during low frequency rotation remains somewhat unclear.
Another effective application of the rotary chair test is its use with special populations, especially infants and young children in whom caloric testing cannot be completed effectively [1]. The test is easy to administer and takes a minimal amount of time, and the gentle rocking motion is usually enjoyable to infants and young children. Even though the low-frequency rotary chair test has specific limitations (for example, inability to consistently identify site of lesion or side of involvement), it has demonstrated a significant clinical usefulness. Stockwell reported a 15% improvement in the detection of vestibular abnormalities using the rotary chair when compared to ENG. It must be stressed, however, that the rotary chair results should be treated with a degree of caution. Our knowledge of the visual/ vestibular system is limited to date, and the low-frequency rotary chair test monitors only a fraction of the VOR. We must take into account other factors such as the otolith organs (that may influence the response), the remaining semicircular canals, the brain stem integration of the response, and the cognitive processes, such as prediction, that may also affect the test results. As is appropriate with all clinical assessments, the rotary chair results, as well as those obtained with the standard ENG, should always be interpreted in conjunction with patient history, symptoms, and other test findings.
- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
Posturography
Up to this point, we have discussed objective measures of vestibule ocular and ocular motor function alone. These VOR tests permit us to examine only a portion of the mechanism used for the maintenance of posture and both static (standing) and dynamic (walking) balance. In addition, although the VOR tests provide the clinician with diagnostic information related to the physiologic status of the vestibule ocular system, they do not provide a complete indication ofthe functional impact a vestibular lesion may have on a patient's sense of equilibrium. That is, one patient with a profound, bilateral peripheral vestibular weakness may have much greater difficulty ambulating when compared to a second patient with a similar condition. Circumstances such as age, visual acuity, overall strength, interactive or suppressive medications, and status of the patient’s somato sensory system represent but a few of the reasons for this difference. It would seem logical to conclude that a functional measure of a patient's balance is important if the audiologists is to obtain knowledge into the effects of various vestibular system lesions, and, at the same time, to provide the vestibular- or balance-disordered patient the most effective care and treatment possible.
Although many of the patients referred for «dizziness» have straight forward vestibular disease, others have multi-system lesions. Standard vestibular tests such as electronystagmography (ENG) and computerized rotation may be insufficient for these patients since these tests deal almost exclusively with the vestibuloocular reflex (VOR). The effects of vision and proprioception are not effectively considered with VOR tests.
Over the years, several attempts have been made to evaluate the somato sensory and visual influences on posture and equilibrium, commonly using some type of force platform that measures body sway with and without visual awareness (often referred to as static post urography or stabilometry). Because the effects of sensory input referable to balance usually are measured through a motor reaction, the patient’s coordinated muscle response also must be considered. That is, the brain must not only receive and integrate the input from the sensory systems subserving balance, but also generate an appropriate motor response. Therefore both sensory and motor components of balance should be evaluated when assessing postural stability. Normal motor responses imply normal function of both sensory and motor arcs, but abnormal motor responses can reflect abnormalities in the sensory or motor arcs or both.
Recently computerized force vector analysis has been added to improve the precision of platform posturography. Nashner [6] has carried this evaluation a step further. This system (Equitest), known generically as computerized dynamic posturography (CDP), attempts to ferret out the effects of various sensory inputs to the brain and relate them to overall on-feet balance and stability. CDP employs a computer-controlled, menu-driven moveable platform and a moveable background that surrounds the patient almost completely and fills the patient's visual field. The background, attached to a moveable surround, contains colored patterns simulating an abstract landscape and provides the surface for visual orientation and fixation. Both the platform and background are «sway referenced». That is, the platform and background move to track the anteroposterior (AP) sway of thepatient, who is asked to stand on the platform surface with feet shoulder width apart.
The patient’s body sway is monitored by pressure-sensitive gauges located in each quadrant of the platform. As the patient sways around his or her center of balance, the platform and background tracj the patient's motion, providing an objective measure of actual AP sway. The surface platform is able to operate independently of the background. The test is conducted with eyes open or closed, which eliminates all visual cues, and because of sway referencing, can provide conditions of visual distortion and somatosensory distortion. In addition, the platform can be jerked suddenly front-to-back and back-to-front to measure the patient’s motor response to sudden loss of balance. The platform also performs a «toes-up» and «toes-down» movement. These latter computer-induced platform movements evaluate motor responses that include the strength (force), symmetry, and latency of muscle response. In addition, movement adaptation is evaluated with repeat platform rotations. A safety harness is attached to the patient to prevent injury should a fall occur.
The standard, clinical CDP test battery includes an assessment of automatic postural responses to platform perturbations, the so-called motor control (MC) test, and the sensory organization (SO) test. The sensory organization portion of the test battery manipulates visual and proprioceptive inputs while determining the effects on a patient's standing balance.
- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
Clinical Uses of Computerized Dynamic Posturography
CDP is suggested for
- Patients with histories of imbalance and on- feet unsteadiness, as opposed to patients with rather straightforward vertigo for which ENG would likely be given first thought;
- Children with delayed motor development or «clumsiness» in order to evaluate body alignment and disorganization of sensory inputs to the brain;
- Neurologically impaired patients to evaluate weight and strength symmetry, long motor loop reaction time between left and right legs, and adaptation ability;
- Patients with suspected organic vestibular system disease where the standard VOR tests are noncontributory [1]; and
- Patients who need a determination of the functional impact a lesion (or feigned lesion in the case of a malingerer) has on a patient's standing balance and posture.
The test results can assist in planning remediation strategies for balance-disordered patients, and the effects of various therapies (medical, surgical, and physical) can be monitored in patients with known or suspected vestibular disease by repeating the test at specific intervals. The primary value of this test appears to lie in its ability to describe the functional impact various lesions have on static and dynamic balance. Although certain patterns of dysfunction have been noted and are illustrated in the preceding figures, this test does not yet possess the diagnostic usefulness of the ENG battery, at least as far as vestibular lesions are concerned. This is not meant to criticize the test procedure. In fact, we believe CDP can add significantly to the evaluation of patients with dizziness and various forms of disequilibrium and imbalance. The test is easy to administer, requires very little time (approximately 15 to 20 minutes), and does not create discomfort. The test results appear to be repeatable, when conducted properly, and improvement in on-feet stability can be monitored over time with considerable reliability. Because of the repeatability of testing, the effect of physical therapy and improvement noted following medical or surgical intervention can be quantified. On the negative side, the dynamic posturography equipment is expensive, and at this time, reimbursement by third parties is poor, which may restrict placement of CDP to larger clinical settings.
- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
Videonystagmography (VNG)
Videonystagmography (VNG) is a series of tests used to determine the causes of a patient’s dizziness or balance disorders. If dizziness is not caused by the vestibular portion of the inner ear, it might be caused by the brain, by medical disorders such as low blood pressure, or by psychological problems such as anxiety. VNG is a test used to determine whether or not dizziness may be due to inner ear disease.
How does VNG Work?
VNG is a complete diagnostic system for recording, analyzing and reporting involuntary eye movements, called nystagmus, using video imaging technology. Hi-tech video goggles with infrared cameras are worn while you look or lie in different positions.
There are four main parts to the VNG. The saccade test evaluates rapid eye movements. The tracking test evaluates movement of the eyes as they follow a visual target. The positional test measures dizziness associated with positions of the head. The caloric test measures responses to warm and cold water circulated through a small, soft tube in the ear canal. The cameras record the eye movements and display then on a video/ computer screen. This allows the examiner to see how the eyes move which is very helpful in assessing balance system health.
There are 4 main parts to a VNG test:
Occular Mobility
- Patient will be asked to have his eyes follow objects that jump from place to place, stand still, or move smoothly.
- The clinician will be looking for any slowness or inaccuracies in their ability to follow visual targets.
- This may indicate a central or neurological problem, or possibly a problem in the pathway connecting the vestibular system to the brain.
Optokinetic Nystagmus
- Patient will be asked to view a large, continuously moving visual image to see if his eyes can appropriately track these movements.
- Like the occular mobility tests, the clinician will be looking for any slowness or inaccuracies in his ability to follow visual targets.
- This may indicate a central or neurological problem, or possibly a problem in the pathway connecting the vestibular system to the brain.
Positional Nystagmus
- The clinician will move patient head and body into various positions to make sure that there are no inappropriate eye movements (nystagmus), when his head is in different positions.
- This test is looks at inner ear system and the condition of the endolymph fluid in your semi-circular canals.
- The technician is verifying that small calcium carbonate particles called otoconia are not suspended in the fluid and causing a disturbance to the flow of the fluid.
Caloric Testing
- The clinician will stimulate both of your inner ears (one at a time) with warm and then cold air.
- They will be monitoring the movements of your eyes using goggles to make sure that both of your ears can sense this stimulation.
- This test will confirm that your vestibular system for each ear is working and responding to stimulation. This test in the only test available that can decipher between a unilateral and bilateral loss.
The cameras record the eye movements and display them on a video/computer screen. This allows the examiner to see how the eyes move which is very helpful in assessing balance system health.
Instructions for the VNG test
- Do not eat two hours prior to testing. (NOTE: if you are diabetic or hypoglycemic pleasemaintain your regular eating schedule.)
- Please wear only minimal makeup or facial moisturizers - NO mascara or eyeliner.
- Do not consume alcohol at least 48 hours prior to testing.
- Please let the audiologist know if you have any history of neck or back surgery problems.
- Do not drink coffee, tea, cola, or any other beverage containing caffeine within 24 hours of the test.
- Do not eat or smoke for 3 hours before the test.
- Medications- Some medications may interfere with test results.
- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Alcohol in any Quantity: Including bear, wine, and cough medicines containing alcohol.
- Anti - Nausea Medicine: Dramamine, Compazine, Bonine, Marezine, Phenergan, Thorazine etc.,
- Anti - Vertigo Medicine: Antivert, Meclizine, Scopolamine, Flunarizine
- Antihistamines: Chlortrimeton, Dimetane, Disophrol, Benadryl, Actified, Teldrin, Triaminic any over the counter cold remedies etc.,
- Aspirin
- Marijuana
- Marcotics AND Phenobarbital, Codeine, Demerol, Benadryl
- Barbiturates: Actified, Teldrin, Triaminic, any over the counter cold remedies etc.,
- Quinine
- Sedatives: Membutal, Seconal, Dalmane, Doriden, Placidyl, Qualude, Butisol. Chloral hyrate or any other sleeping pills.
- Stimulants: Amphetamines
- Tranquilizers: Benzodiazepines, Ativan, Xanax, Valium, Librium, Atarax, Vistril, Equanil, Miltown, Serax, Etrafon etc.,
- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
Interpretation
Look for:
- Spontaneous Nystagmus
- Severity of the Nystagmus
- Directions of the Nystagmus
- Duration, No. of Beats, Culmination fy
- Canal/Unilateral Peresis/Weakness
- Directional preponderance
- Visual Fixation Index
- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
Advantages
- Eye movements are captured on video and can be viewed by the clinician during and after testing.
- Clinician is able to visually assess for torsional eye movement by observing the striations of the iris. This is especially important for the diagnosis of benign paroxysmal positional vertigo.
Tests to assess vestibular disorders have proved to be ideal to understand the vestibular system in a better way. These tests allow the clinician to comprehend the cause of dizziness and provide suitable rehabilitation to their clients. They also help Otolaryngologists and neurologists to provide medical intervention timely and effectively.
- Research Article
- Introduction
- Vestibular-Ocular Reflex (VOR)
- Compensatory Eye Movements
- Vestibulospinal Reflex (VSR)
- Nystagmus
- Electronystagmography
- Risks of the ENG Procedure
- Rotational Tests
- Clinical Utility
- Posturography
- Clinical Uses of Computerized Dynamic Posturography
- Videonystagmography (VNG)
- The Following Medications Must Not Be Taken For At Least 2 Days (48 Hours) Before The Test
- Interpretation
- Advantages
- References
References
- Hillier SL, Hollohan V (2007) Vestibular rehabilitation for unilateral peripheral vestibular dysfunction. Cochrane Database of Systematic Reviews 4.
- Hilton M, Pinder D (2004) The Epley (canalith repositioning) manoeuvre for benign paroxysmal positional vertigo. Cochrane Database of Systematic Reviews 2.
- Herdman SJ (2007) Vestibular Rehabilitation. (3rd edn). F.A. Davis Co, Philadelphia, USA.
- Nall R (2012) Vestibular Therapy Exercises.
- National Institute of Health (1989) A Report of the Task Force on the National Strategic Research Plan. Bethesda 12.
- Vestibular Rehabilitation Therapy (2012).





























