Dysphagia in Forestier Syndrome
Cristina Otilia Laza* and Mostafa Sarv
ENT Clinic SCJU, SFAPOSTOL ANDREI ", Constanta, Romania
Submission: April 06, 2017; Published: April 17, 2017
*Corresponding author: Cristina. Otilia Laza, Professor associate PhD -ENT -head and neck surgery, ENT/OMF Clinic, SCJU SF "APOSTOL ANDREI " Constanta, B-dul Tomis, 145,8700, Constanta, Romania, Email: cristinaotilia@gmail.com
How to cite this article: Cristina O L, Mostafa S. Dysphagia in Forestier Syndrome. Glob J Oto 2017; 6(4): 555695. DOI: 10.19080/GJO.2017.06.555695
Abstract
Dysphagia is a frequent complaint in elderly patients. At this age, neurological and tumoral causes predominates. Diffuse idiopathic skeletal hyperostosis (DISH), also known as Forestier disease , first described in1950 by J. Forestier, is a rare cause of dysphagia ,caused by large calcification along the anterior and lateral sides of the vertebral bodies, produces the appearance of candle wax dripping down the spine. Most patients are free of symptoms, so that DISH is usually discovered fortuitously upon plain radiographs of the spine obtained for another reason. A few patients experience spinal pain, spinal stiffness, or dysphagia. We report a case in which the diagnosis was made upon evaluation for dysphagia in an old patient. The diagnosis requires imaging but also other causes especially tumors must be excluded.
Keywords: Dysphagia; Retropharyngeal; Prevertebral space; Diffuse idiopathic skeletal hyperostosis (DISH); Forestier syndrome
Case Report
A 69-year-old man with was referred to our otorhinolaryngology clinic for difficulties in swallowing solid food, with significant weight loss in 3 month, at presentation he was capable to swallow very soft pureed foods or liquids. Dysphagia had worsened gradually over the last 3 months. With difficulties in initiating swallowing and a feeling of obstruction as if food has become stuck in the throat. There were no sign nasal regurgitation. He had no history of smoking or alcohol abuse, and he take Digoxin, Aspenter, Indapamid, Betabioptal, Syofor [1-5]. His general diseases are: Diabetes type II, Glaucoma, Atrial fibrillation, Arterial hypertension, Dyslipidemia. He had no respiratory symptoms or dysphonia, or couching on deglutition- sign of aspiration. Also he denied cervical pain or odynophagia. He had no changing in bowel habits-like diarrhea or blood in the stool.
Clinical Examination
On examination was pale and cachectic, he weight just 49 kilo with low muscle tone.
Inspection: The cervical area was normal without masses like adenopaties or cysts with laryngeal cracment present but with rigid cervical spine non painful. The oral cavity and bucopharynx were normal to physical examination -good dentures, no sign of infection or tumors at bucopharyngoscopy. In the hipopharynx a posterior mass located on the posterior wall, covered with normal mucosa was discovered at the laryngoscopy, compressing the cricoids [6].
Laboratory Tests
His full blood count showed a normocytic anaemia (9.32 g/ dl) with a normal ferritin level. Erythrocyte sedimentation rate and thyroid stimulating hormone were normal .Liver function was normal apart from a low albumin level of 28g/l. Neurological examination -normal for his age. Endoscopy of the pharynx and larynx showed a posterior bulge consistent with extrinsic compression with the aspect of a retropharyngeal tumor, but it can be dangerous -0risc of perforation. We use a small flexible endoscop for children [7,8].
Imaging
An pharyngoesophageal barium x-Ray revealed an extrinsic compression on the pharynx. A profile X-ray of the cervical spine demonstrate the ostheophytic nature of compression -showing calcification along the anterior aspect of five vertebras, from C3 to C7. The calcification pressed on the posterior wall of the hypopharynx, without causing stasis or blockage of the contrast medium [7,8]. Computer tomography-scan (CT) (confirmed the anterior ossification extending from C3 to C7 and impinging on the hypo pharynx and esophagus. A space was clearly visible between the ossification and the spine, establishing that the lesion was due to ossification of the anterior longitudinal ligament (ALL), as opposed to osteophytosis. Also visible on the CT images were ossification of the ALL along the thoracic spine and calcifications on the posterior side of a vertebral body indicating involvement of the posterior longitudinal ligament (PLL) [9]. The sacroiliac joints were normal by plain radiography. MRI confirm the lesions and the absence of mechanical compression on the nerves or spinal cord. This finding, together with the appearance of the spinal lesions, led to a diagnosis of DISH-diffuse idiopathic skeletal hyperostosis.
Treatment
The treatment was medical, with non steroids antiinflammatory drugs, myorelaxant, and antianemics, vitamins. The nutrition was improved first parenteral with IV solution containing glucoses, animoacids and lipids like Aminoven, Nutriflex. Than a nasogastric tube was inserted to feed the patient with hipercaloric hyperproteic shakes [5,7]. The patient was referred to the rheumatology department for evaluation and treatment because of his poor general status and cardiovascular disorders.
General Information
In 1950 Forestier and Rotes-Querol described an ankylosing disease of the spine developing in elderly people. This entity was known as Forestier's disease. In the 1970s, Resnick termed this condition Diffuse Idiopathic Skeletal Hyperostosis. DISH or diffuse idiopathic skeletal hyperostosis is an ankylosing hyperostosis of the spine characterized by ossification of tendons and, ligaments at their sites of attachment to bone, with appearance of large, osteophytic spurs or bony proliferation in the form of anterior osseous bridges with an thickening of the corresponding vertebral cortex. The anterior longitudinal ligament and periferal part of the disc are also calcified also concomitent ossification of posterior longitudinal. ligment and flavus are present. Although its origin remains unknown, the considered causes are: abnormal vitamin A metabolism or insulin- induced growth hormone stimulation have been suggested association with diabetes mellitus type II, hypercholesterolemia and gout and obesity association with fluorosis, hypocalcemia, hypophosphatemic hypoparathypoidism hypocalcemia, hypophosphatemia association with Dupuytrens contracture,HLA-B72 antigen.
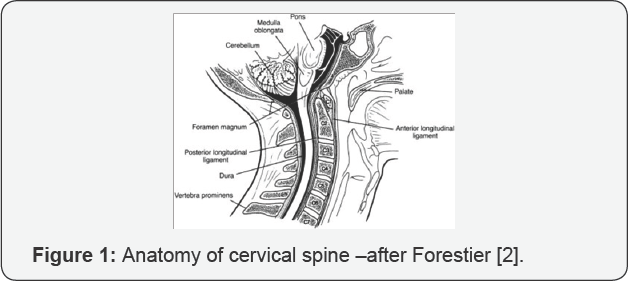
DISH is common, with a prevalence of 5 to 15% among individuals older than 60 or 70 years especially obese It is characterised by new bone formation into axial and peripheral region. Men are affected predominantly in a ratio of 3/1 (Figure 1). DISH most commonly affects the thoracic and lumbar spine although cervical involvement is found in 76% of those affected .However the thoracic region is the most immobile segment of the spine and the most common site for ossification of the anterior longitudinal ligament in DISH .This argues against mobility being the only catalyst for ossification. The most frequent level of involvement related to dysphagia is C 5-6 followed by C 4-5, C 2-3 being the least common level affected. Extras pinal lesions may develop, the main sites of involvement the pelvis, calcaneus, olecranon and patella
Histophatology
Ossified tissues in (DISH) are composed of normal-appearing haversian bone as opposed to the wormian or disorganized structure of bone seen in patients with hypervitaminosis A.
Symptoms and Signs
DISH is usually asymptomatic. The main initial symptoms are moderate spinal pain and mild dorsal kyphosis and decrease in lumbar lordosis stiffness, and restriction on movements, but these do not always prompt a physician visit. The picture is completed by findings of outgrowths in the knee, shoulder, hip, pubian symphysis. Large osteophytes have also been reported to compress or obstruct a number of structures, including: bronchus, IVC, esophagus, increased incidence of calcification in surgical scars is associated with, hyperostosis frontalis interna [3]. The proportion of cases revealed by dysphagia has ranged across studies from 0.1% to 28% . The dysphagia is usually marked, present for solid foods, improved by anterior flexion of the neck, and worsened by extension of the neck. Dysphagia, or swallowing disorder, is a general term used to describe the inability to move food from the mouth to the stomach.
Aspiration is a term referring to the passive entry of any food item into the trachea (e.g, during inhalation), although the word often is used to denote any entry of a bolus into the trachea in any manner. Penetration refers to the active entry of any food item into the trachea (eg, during swallowing), although the term often is used to denote the entry of any bolus into the laryngeal vestibule. Dysphagia can be secondary to defects in any of the 3 phases of swallowing. These phases are as follows:
- oral faze-mastication, bolus formation,
- pharyngeal faze,
- esophageal faze
I. Concomitant symptoms
a) foreign body sensation,
b) odynophagia,
c) reffered otalgia,
d) salivary stasis,
e) dysphonia,
f) sleep apnea,
g) aspiration,
h) dyspnoeea,
II. Dysphagia caused by DISH may be due to several factors
a) direct mechanical compression of the oesophagus or pharynx by large anterior osteophytes;
b) smaller osteophytes located at sites of hypopharingeal fixation such as at the level of the cricoid cartilage;
c) inflammation of the peri-oesophageal, peripharyngeal soft tissue in contact with overlying osteophytes;
d) oesophageal spasm caused by painful osteophytes.
Odynophagia may result also from hypopharyngeal ulceration at a point of pressure between the posterior cricoid cartilage and a protruding osteophyte. Dysphonia or airway obstruction may result from laryngeal edema, arytenoids ankylosis, or vocal cord paralysis caused by an osteophyte at the cricoids level. Obstructive sleep apnea and stridor may result of impingement of the osteophyte on the laryngeal vestibule. Although DISH causes a mass syndrome in the retropharyngeal space, the epicenter is in the prevertebral space .In addition to ossification, inflammation develops, causing mucosal thickening or laryngeal immobility and producing tumor-like formations.
III. Neurological complications
a) spinal cord or nerve root compression,
b) peripheral nerve entrapment,
c) Recurrent laryngeal nerve palsy
Spinal cord or nerve root compressions are caused by ossification of the PLL or ligamentum flavum, probably in combination with congenital spinal stenos is. Because the clinical symptoms lack specificity, the diagnosis rests on imaging studies, X-ray-with barium, CT-scan, MRI.
IV. Radiologic criteria for diagnosis developed by Resnick
a) calcifications and ossifications along the anterolateral aspect of at least four contiguous vertebral bodies,
b) normal disk space height in the affected segments, absence of facet joint fusion,
c) Absence of clinical or radiological evidence of sacroiliitis. Although plain radiography remains the reference investigation (Figures 2-7).
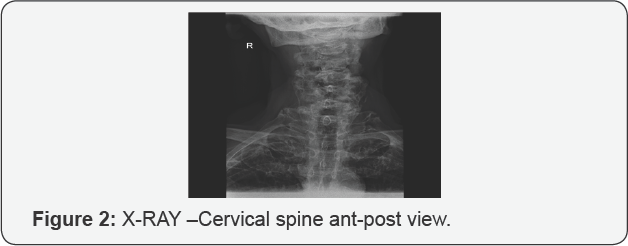
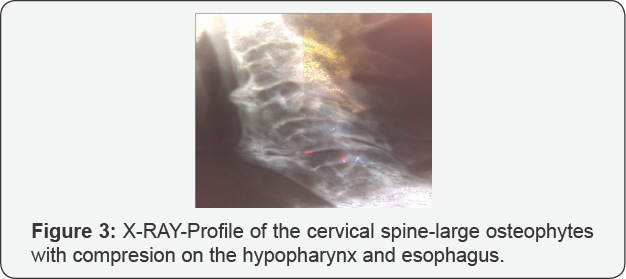
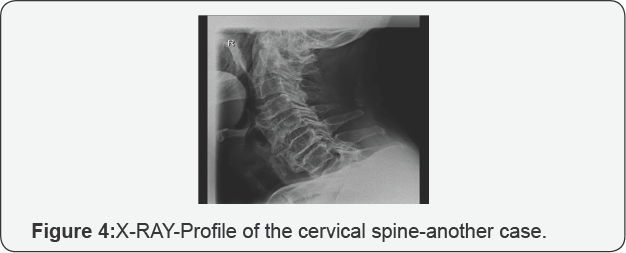
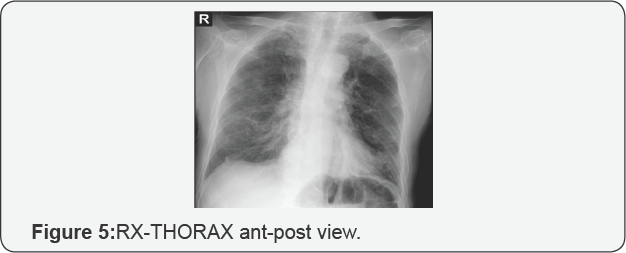
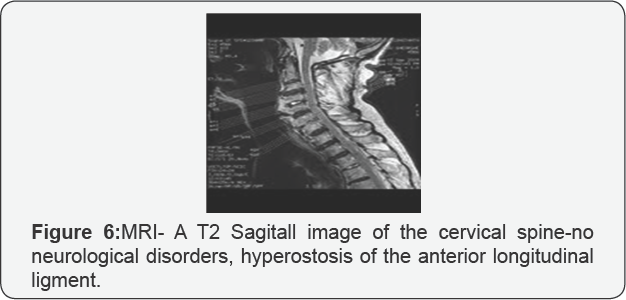

V. CT-scan visualizes
a) the cleavage plane,
b) ossifications in the PLL,
c) ligamentum flavum, morever, it allows measurement of the antero-posterior diameter of the spinal canal
Magnetic resonance imaging (MRI) is indicated in patients with neurological manifestations of spinal cord compression and concomitant myelopathy (Figures 8 &9).
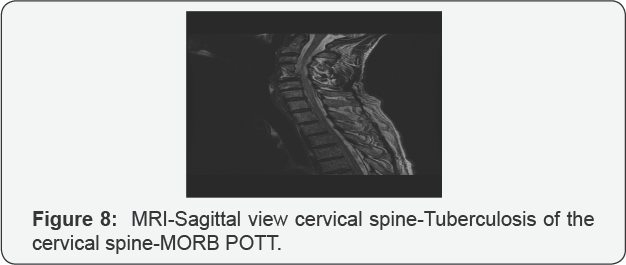
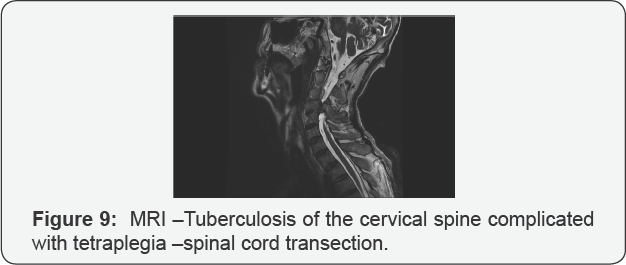
VI. Differential Diagnosis of Cervical Mass
a) Osteoarthritis when the lesions simulate osteophytes,
b) Spondyloarthropathy when they suggest syndesmophytes,
c) Retropharyngeal calcification tendinitis- Ossified posterior longitudinal ligament (OPLL).
d) Discitis, Spondylosis deformans, Pachydermoperiostosis
e) Spondylosis deformans,
f) Fluorosis,Osteomalacia,Hypophosphatemia , Hypervitaminosis A, Retinoids
g) Acromegaly
I. Also Other Causes Of Dysphagia Must Be Excluded
A. Central nervous system disorders
a) Neuropathic disorders,
b) Endocrine disorders,
c) Vitamin B-12 deficiency
B. Oropharyngeal /hypo pharyngeal dysphagia
a) MORB POTT-tuberculosis of the cervical spine
b) Foreign bodies complication -ex a bone inserted in the retropharyngeal space
c) Retropharyngeal abscess,
d) Retropharyngeal mass-chordoma, osteoma, sarcomas
e) Benign and malignant tumors like-pleomorphic adenoma, papilloma, lymphomas, plasmocytoma, sarcomas or vegetant, carcinomas, hypertrophied lingual tonsil, lingual thyroid, base of the tongue tumors -large cyst, lymphomas, sarcomas etc.
C. Medications
D. Surgeries- in neurosurgery or ENT
E. Psychogenic dysphagia: Psyhiatric disorders with intact speech and pharyngoesophageal and neurologic function Associated psychiatric conditions include anxiety, depression, somatoform disorders, hypochondriasis, conversion disorders, and eating disorders.
F. Esophageal disorders
a) Motility disorders
b) Structural disorders
Treatment
No treatment capable of preventing the progression of vertebral hyperostosis in DISH patients is available today. Physical therapy may improve range of motion in patients with spinal stiffness. Medical therapy nonsteroidal anti-inflammatory agents or glucocorticoid bolus therapy in combination with a muscle relaxant can be used to improve the symptoms. Spinal pain may require analgesic therapy. Surgical treatment osteophytotomy transorally or using a cervicotomy aproach.
A. Dietary precautions: Typical therapy programs involve the following components:
a) Oral feeding with consistency modifications,
b) Thickened liquids increase oropharyngeal control, while a diet of chopped or pureed foods decreases difficulties with mastication.
c) Minimizing gastroesophageal reflex are in order in patients with dysphagia,
B. Nonoral feeding:
a) Parenteral alimentation and intravenous (IV) fluid replacement should be prescribed, also. hyperproteic, hypercaloric cocktails.
b) Nasogastric (NG) tubes are convenient for the short term, but their use is limited by complications, including regurgitation, irritation, bleeding, and discomfort. H2- blocker or proton-pump inhibitors should be given as prophylaxis to prevent some of the above complications.
c) Gastrostomy can be placed by percutaneous endoscopic means, allowing for continuous or bolus feedings. vertical position, H2 blockers to decrease gastric pH, chlorpromazine to facilitate gastric emptying, and proton-pump inhibitor to decrease gastroesophageal reflux.
d) Tracheostomy is needed to prevent aspiration pneumonia in patients with severe dysphagia related to a marked prominent ossification.
Conclusion
a) DISH, a common after 60 years of age, may be revealed by dysphagia.
b) In an elderly patient with dysphagia and no otorhinolaryngological lesions, an upper gastrointestinal series should be obtained.
c) Plain radiographies ensure the diagnosis, although CT provides additional information. When reading CT sections of the pharynx, the bony structures should be examined carefully.
d) The familiarity with the signs of DISH is essential to ensure the diagnosis of this disease that can cause major morbidity related to swallowing dysfunction and to aspiration.
e) Because DISH is extremely common, it should not be accepted as the cause of dysphagia until other lesions, most notably tumors, have been convincingly ruled out by a thorough otorhinolaryngological examination.
f) Swallowing disorders are becoming a major source of disability. However, improvements have been made in the ways these disorders can be treated, especially with regard to dysphagia-related malnutrition, and with the available tests and management options for swallowing disorders, the prognosis for patients with dysphagia has improved
g) An understanding of the anatomy and physiology of the areas of the body affected by dysphagia is of paramount importance in the diagnosis and management of swallowing disorders.
h) Early involvement of other specialists, including ENT surgeons, nutritionists, gastroenterologists, neurosurgeons, and speech-language therapists, offers a good prognosis for the management of swallowing disorders.
References
- Matan AJ, Hsu J, Fredrickson BA (2002) Management of respiratory compromise caused by cervical osteophytes: a case report and review of the literature. Spine J 2(6): 456-459.
- Forestier J, Rotes-Querol J (1950) Senile ankylosing hyperostosis of the spine. Ann Rheum 9(4): 321-330.
- Resnick D, Shapiro RF, Wiesner KB, Niwayama G, Utsinger PD, et al. (2005) Diffuse idiophatic skeletal hyperostosis (DISH). Semin Arthritis Rheum 7: 153-187.
- Arlet J, Abiteboul M, Mazieres B, Laffont F, Dedieu - Snapir G, et al. (1983) Vitamine A et hyperostose vertebrale ankylosante. Rev Rhum Mal Osteoartic 50: 63-65.
- Ehara S, Shimamu ra T, Nakamu ra R, Yamazaki K (1998) Paravertebral ligamentous ossification : DISH, OPLL and OLF. Eur J Radiol 27: 196205.
- Kiss C, Szilagyi M, Pasky A, Poor G (2002) Risk factors for diffuse idiopathic skeletal hyperostosis:a case-control study. Rheumatology 41: 27-30.
- Littlejohn GO, Hall S, Brand CA, Davidson A (1986) New bone formation in acromegaly: pathogenic implications for diffuse idiopathic skeletal hyperostosis. Clin Exp Rheumatol 4: 99-104.
- Resnick D, Niwayama G (1976) Radiographic and pathologic features of spinal involvement in diffuse idiopathic skeletal hyperostosis. Radiology 119: 559-568.
- Julkunen H, Heinonen OP, Knekt P, Maatela J (1975) The epidemiology of hyperostosis of the spine together with its symptoms and related mortality in a general population. Scand J Rheumatol 4: 23-27.





























