A Case of Primary Tuberculosis of Tonsil: A Rare Entity- Case Report
Sushna Maharjan1*, Ramesh Parajuli 2 and Puja Neopane3
1Department of Pathology, Chitwan Medical College Teaching Hospital, Nepal
2Department of Department of Otorhinolaryngology, Chitwan Medical College Teaching Hospital, Nepal
3Department of Oral Medicine and Pathology, School of Dentistry, Health Sciences University of Hokkaido, Japan
Submission:February 10, 2017; Published: February 22, 2017
*Corresponding author: Sushna Maharjan, Department of Pathology, Chitwan Medical College Teaching Hospital (CMC-TH), P.O. Box 42, Bharatpur, Chitwan, Nepal, Email:sushnamaharjan74@gmail.com
How to cite this article: Sushna M, Ramesh P, Puja N. A Case of Primary Tuberculosis of Tonsil: A Rare Entity- Case Report. Glob J Oto 2017; 4(1): 555629. DOI: 10.19080/GJO.2017.04.555629
Key Clinical MessageTuberculosis of tonsil should be in differential diagnosis if a patient presents with sore throat, cervical lymphadenopathy and unilateral tonsillar enlargement. Histopathological examination should be sent for confirmation and rule out malignancy. Chest X-ray and HIV-screening is always recommended since there is increased incidence of extrapulmonary tuberculosis in AIDS patients.
Abstract
Primary tuberculosis of tonsils is rare. We reported a case of primary tonsillar tuberculosis in a 55-year-old female who presented with sore throat and enlargement of right tonsil. Histopathology revealed tuberculoisis. Complete resolution was found after antitubercular therapy. Tonsillar tuberculosis should be considered if patient is not responding to antibiotics.
Keywords:Antitubercular therapy; Primary tuberculosis of tonsil; Sore throat
Introduction
Tuberculosis (TB) is one of the most serious and life threatening infectious diseases in the world [1]. Upper respiratory tract involvement is encountered in approximately 2% of patients with active pulmonary TB [2]. It affects all organs and tissues but tonsil is one of the uncommon sites for tuberculosis. Primary TB of tonsils is even rarer and thus it usually occurs as secondary involvement to pulmonary infection [3]. The advent of antitubercular drugs has overall diminished the incidence of TB and the occurrence of TB of tonsils is further reduced after widespread use of pasteurized milk [4]. It is surprising for not infecting tonsils although tonsils are placed at the site of frequent contact with infected sputum by tubercle bacilli and it is postulated that cleaning and antiseptic effects of saliva protect tonsils [5]. The presence of saprophytes and thick protecting epithelial layer covering the tonsils might be further resisting them to tubercle bacilli [6,7]. A few research articles and case reports of extrapulmonary TB are available from Nepal. Thus, the rare involvement of tonsils with tuberculous infection encouraged us to report a case of primary foci of tonsillar TB.
Case History
A 55-year-old female presented with history of sore throat, difficulty and pain in swallowing of solid food for 2 months in Department of Otorhinolaryngology in our hospital. There was no history of cough, fever, hoarseness of voice, vomiting and regurgitation of food. On examination of oropharyngeal cavity, there was congestion and slight enlargement of right tonsil. Left tonsil was normal. She had past history of recurrent sore throat. Clinical diagnosis of chronic tonsillitis was made. She was given Ciprofloxacin (500 mg) twice daily and Paracetamol (500mg) twice daily for five days. The patient re-visited with the same complaints after 5 days since symptoms did not subside. On examination, enlargement of right tonsil about 9x9 mm in dimension with an ulcer and slough was found.
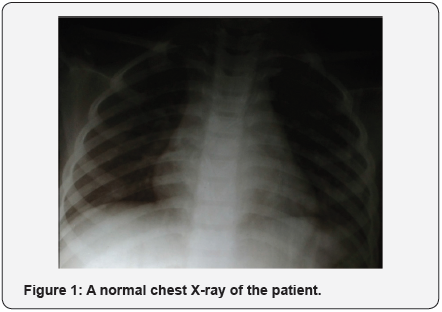
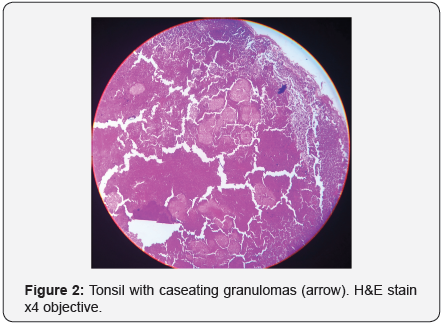
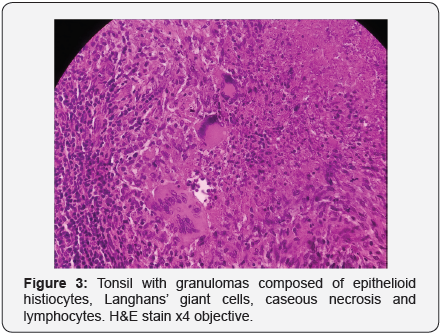
Rest of the oral cavity was normal. Right cervical lymphadenopathy was also noted. Systemic examination revealed no abnormality. Chest X-ray and sputum for acid fast bacilli were suggested to rule out primary foci in lungs. Chest X-ray was normal (Figure 1) and sputum for acid fast bacilli was also negative. Routine investigations of blood, urine and biochemical tests were normal except for ESR-55mm at 1hour. The patient was HIV seronegative. Mantoux test was positive with indurations of 20× 18 mm. The differential diagnosis of TB and malignancy was made. Hence, histopathological examination was recommended. Punch biopsy was taken from the ulcerative lesion on right tonsil and sent to Department of Histopathology. The histopathological examination of the tonsillar biopsy revealed epithelioid cell granulomas, caseous necrosis, Langhans’ giant cells and lymphocytes (Figures 2 & 3). Ziehl Neelsen stain was negative for acid-fast bacilli. Antitubercular therapy was started. Patient was kept under regular follow up. The symptoms of sore throat, difficulty and pain in swallowing were absent, and there was a complete resolution of lesion on right tonsil on his recent follow up.
Discussion
The burden of extrapulmonary TB represents approximately 25 % of overall tubercular morbidity [8]. TB of the oral cavity is uncommon and tonsillar involvement is even rare [9]. The cause of TB of tonsils is either infection with Mycobacterium bovis due to ingestion of unpasteurized cow’s milk as primary form, or it may be as secondary form associated with contact of infected sputum expectorated from TB of lungs. The secondary form is common in the present day as pasteurization of milk almost eliminate the primary TB of tonsils [10]. The route of spread of bacilli may be hematogenous or inhalation of tubercle bacilli which harbour in the Waldeyer’s ring. Although TB of tonsil is not frequent, tonsillar granulomata are commonly observed in patients with poor host reaction due to alcoholism, HIV infection, and so on [11]. Poor dental hygiene, dental extraction, periodontitis, and leukoplakia are some of the predisposing factors for primary oral TB [12,13].
Patients usually present clinically with enlargement of tonsils, painful ulceration, white patches, cervical lymphadenopathy, productive cough, sore throat, dysphagia, odynophagia, with or without constitutional symptoms and signs of TB [14-16]. The most common presentation is sore throat [15]. Few features are typically suggestive of tonsillar TB, such as asymmetric enlargement of tonsil, tonsillar enlargement without exudate, obliteration of crypts, painful deglutition, and the presence of enlarged mobile jugulo-digastric lymph nodes [14]. However, its presentation usually simulates tonsillar malignancies which are more common in elderly patient. Thus, it is very difficult to differentiate them only on clinical ground, and histopathological examination is mandatory to remove the confusion. Hence, diagnosis of tonsillar TB is based on histopathological findings and the identification of tubercle bacilli [16-18].
Jana et al. [5] reported a unique case of tonsillar TB in a young adult male, prior to involvement of lungs. There was a late appearance of cough and infiltration in chest X-ray. This case is quite unique as it suggested primary involvement of tonsils with secondary spread of hilar lymph node and lungs which is very rare. The clinician should keep in mind about the possibility of TB especially in older patients and in developing countries like India [19], and Nepal [20] where the incidence of TB still remains high. Antitubercular therapy is the choice of treatment but requirement of tonsillectomy depends on condition of tonsil and duration of illness. Miller et al. [21] had provided guideline that tonsillectomy is performed in recent infection under coverage of antitubercular therapy, and avoidance of removal of tonsil in old calcified and fibrotic tonsil.
Conclusion
It is difficult to differentiate tonsillar tuberculosis from a malignant tumor as both conditions may have similar presentations and common abnormal tonsillar findings. Thus, histopathological examination is mandatory. Tonsillar TB should be suspected if the patient is not responding to antibiotics, especially in our country where TB is still a prevalent disease.
Acknowledgement
We would like to thank Mr. Anil Shah, the staff of histopathology department for his technical assistance.
Author Contributions
Author 1: Conceived the idea, collected relevant information of the patient, reviewed literature, drafted manuscript of the case, read and approved the final manuscript.
Author 2: Reviewed literature, helped in drafting manuscript, read the manuscript and critically reviwed it; and approved the final manuscript.
Author 3: Collected clinical information of the patient, helped in drafting manuscript, read the manuscript and critically reviewed it; and approved the final manuscript.
References
- Sutbeyaz Y, Ucuncu H, Murat karasen R, Gundogdu C (2000) The association of secondary tonsillar and laryngeal tuberculosis: a case report and literature review. Auris Nasus larynx 27(4): 371-374.
- Rohwedder JJ (1974) Upper respiratory tract tuberculosis: Sixteen cases in a general hospital. Ann Intern Med 80(6): 708-713.
- Weidman WN, Campbell HB (1939) Laryngeal tuberculosis. The American Review of Tuberculosis 40: 85-98.
- Anim JT, Dawlatly EE (1991) Tuberculosis of the tonsil revisited. West African Journal of Medicine 10(2): 194-197.
- Janna U, Mukherjee S (2003) Tuberculosis of tonsil-a rare involvement. Indian journal of otolaryngology and head and neck surgery 55(2): 119-120.
- Verma A, Mann SBS, Randotra B (1989) Primary tuberculosis of the tongue. Ear Nose Throat J. 68(9): 719-720.
- Rauch DM, Freidman E (1978) Systemic Tuberculosis initially seen asan oral ulceration: report of a case. J Oral Surg 36: 384-389.
- Farer LS, Lowell AM, Meader MP (1979) Extrapulmonary tuberculosis in the United States. Am J Epidemiol 109(2): 205-217.
- Ricciardiello F, Martufi S, Cardone M, Cavaliere M, D’Errico P, et al. (2006) Otorhinolaryngology-related tuberculosis. Acta Otorhinolaryngol Ital 26(1): 38-42.
- Selimoğlu E, Sütbeyaz Y, Ciftçioğlu MA, Parlak M, Esrefoğlu M, et al. (1995) Primary tonsillar tuberculosis: A case report. J Laryngol Otol 109(9): 880-882.
- Sunderam G, McDonald RJ, Maniatis T, Oleske J, Kapila R, et al. (1986) Tuberculosis as a manifestation of the acquired immunodeficiency syndrome (AIDS). JAMA 256(3): 362-366.
- Das A, Das SK, Pandit S, Basuthakur S (2015) Tonsillar Tuberculosis: A Forgotten Clinical Entity. J Family Med Prim Care 4(1): 124-126.
- Prasad P, Bhardwaj M (2012) Primary Tuberculosis of Tonsils: A Case Report. Case Reports in Medicine 2012(2012): 3.
- Balasubramanian T, Geetha R, Venkatesan U (2012) Secondary tuberculosis of tonsil case report and literature review. Online J Otolaryngol 2(1): 59-67.
- Srirompotong S, Yimtae K, Srirompotong S (2002) Clinical aspects of tonsillar tuberculosis. Southeast Asian J Trop Med Public Health 33(1): 147-150.
- Gupta KB, Tandon S, Jaswal TS, Singh S (2001) Tuberculosis of tonsil with unusual presentation. The Indian Journal of Tuberculosis 48(4): 223-224.
- Chumakov FI, Gerasimenko NV (2000) Isolated tuberculosis of pharyngeal and palatine tonsil in child. Vestn Otorinolaringol 2: 58.
- Hajioff D, Snow MH, Thaker H, Wilson JA (1999) Primary tuberculosis of the posterior oropharyngeal wall. J Laryngol Otol 113(11): 1029- 1030.
- Kant S, Verma SK, Sanjay (2008) Isolated tonsil tuberculosis. Lung India 25(4): 163-164.
- Ministry of Health & Population. National Strategic Plan - Nepal National Tuberculosis Programme 2010-2015.
- Miller JFW, Seal RME, Taylor MD (1963) Tuberculosis in children. JA





























