Giant Cell Reparative Granulomapresenting as Cheek Swelling: Case Series of Four Patients
Neelam Sood1 and Minakshi Gulia*2
1Consultant and Head of Department of Pathology and Lab Medicines, Deen Dayal Upadhyay Hospital, India
2Senior Resident Pathology, Deen Dayal Upadhyay Hospital, India
Submission: November 12, 2016; Published: December 02, 2016
*Corresponding author: Minakshi Gulia, Consultant and Head of Department of Pathology and Lab Medicines, Deen Dayal Upadhyay Hospital, 361, Sector 21, Gurgaon, Haryana- 122001, India, Tel:9582110284; Email:mint.ucms@gmail.com
How to cite this article: Dusan P. Posterior Semicircular Canal Dehiscence Presenting with Recurrent Positional Vertigo. Glob J Otolaryngol. 2016; 2(3): 555588. DOI: 10.19080/GJO.2016.02.555588
Abstract
Giant cell reparative granuloma is a clinically distinctive intraosseous proliferation most commonly arising in mandible and maxilla. It is classified under fibroinflammatory reactive-reparative lesion. Histopathological features comprise of irregularly distributed multinucleated osteoclast like giant cells in a supporting fibrous stroma along with peripheral osteoid formation and stromal hemorrhage. All the four patients in this study had a characteristic clinicopathological presentation and immunohistochemistry. Differential diagnosis from other giant cell lesions of the bone, especially Giant cell tumor, was pivotal since GCT has a tendency for recurrence and a rare ability to undergo sarcomatous transformation or metastasis. Postoperative follow up of all the patients was unremarkable and there was no recurrence.
Keywords: Giant cell reparative granuloma; Giant cell tumor; Vimentin CD68; Immunohistochemistry
Abbreviations: GCRG: Giant Cell Reparative Granuloma; GCT: Giant Cell Tumor; IHC: Immunohistochemistry
Introduction
Giant cell reparative granuloma, a pseudotumoral lesion, is a benign reactive intraosseous process most commonly arising in craniofacial skeleton and in small bones of the hand and feet, and affects children and young adults [1]. Its origin could be triggered by trauma or inflammation. Histopathological examination shows giant cells are arranged around hemorrhagic areas, stromal cells in storiform pattern and osteoid formation at the periphery [2]. In the present case reports Giant cell reparative granuloma in four patients is described focusing on the cytopathological and histopathological findings.
Case Report
First patient, a thirteen year old girl presented with pain and swelling in the right maxillary region since four months, on examination there was an ill-defined right cheek and nasolabial region swelling. Contrast Enhanced CT scan of the paranasal sinuses revealed relatively well defined homogenously enhancing cystic lesion on Right side in nasolabial region, suggestive of Nasolabial cyst (Figure 1). Second patient, 35 years old female presented with a fleshy mass in the Right maxillary antrum for past one year. The mass was gradually progressive and pushed the nasal bone medially (Figure 2). Another patient, 30 years old male, presented with a fleshy mass protruding from the alveolar ridge and it was gradually progressive (Figure 3). The fourth patient, 35 years old female had left maxillary swelling (Figure 4). The serum levels of calcium, phosphorous and alkaline phosphatase were normal in all four cases, with adequate renal function. Fine needle aspiration cytology was done.
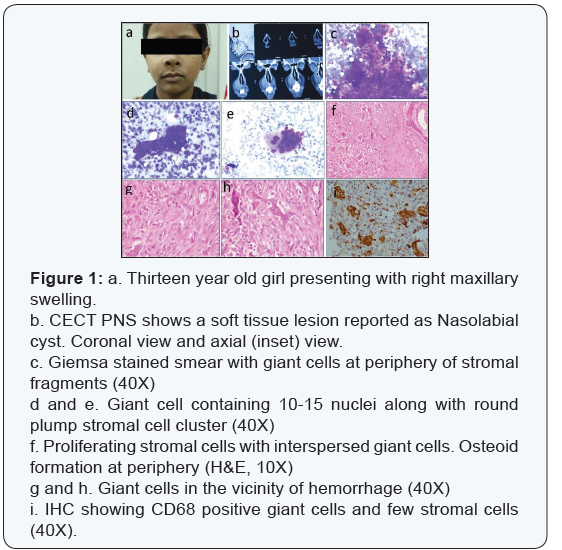
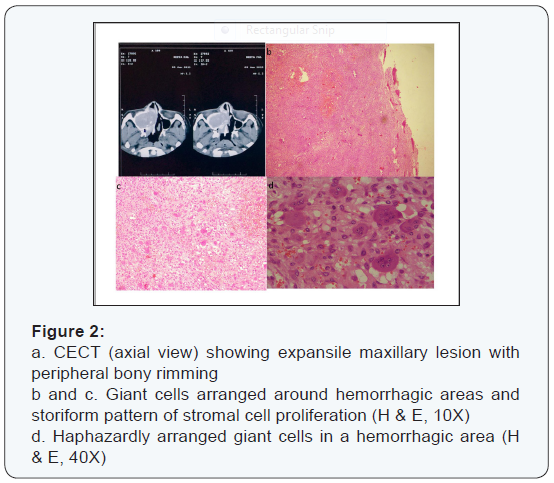
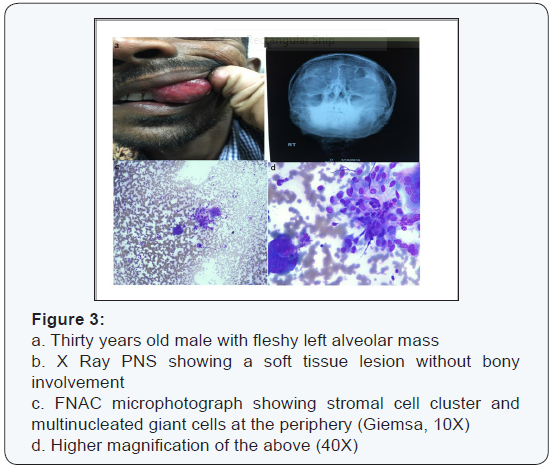
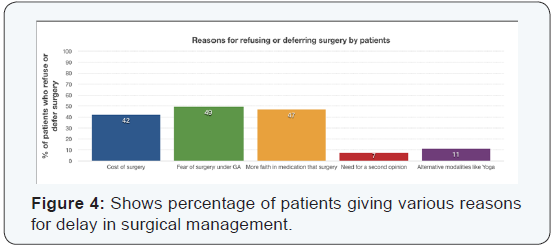
HandE and Giemsa stained FNA smears showed numerous giant cells (5-20 nuclei) having bland nuclear chromatin in a background of hemorrhage. Giant cells are located at the periphery of the stromal fragments. No mitotic activity was seen. FNAC was suggestive of a Giant cell lesion and possibility of Giant Cell Reparative Granuloma was considered. Excision was advised. Histopathological examination of the excised specimens (through Caldwell Luc’s procedure) showed giant cells arranged around hemorrhagic areas, stromal cells in storiform pattern and osteoid formation at the periphery. IHC showed the stromal to be fibroblastic (or myofibroblastic) in origin and the Giant cells were positive for Vimentin and CD68. Features were suggestive of Giant Cell Reparative Granuloma in all of the four patients. The alveolar mass was classified as Peripheral giant cell reparative granuloma and the rest three were Central giant cell reparative granulomas [2-4]. Postoperative follow up of the fourth patient has been unremarkable for 20 years now. Five year follow up of the other patients too has been unremarkable.
Discussion
Giant cell reparative granuloma is a rare, benign reactive intraosseous lesion which represents a reactive process to intraosseous hemorrhage although a history of trauma is infrequent [1]. It was introduced into medical literature by Jaffe in 1953 and accounts for 1-7% of all benign lesions of the jaw and arises most often in the mandible and maxilla [3-10]. Cases have been reported in small bones of the hand and feet, sinuses, temporal bone, skull, spine, clavicle, tibia, humerus, ribs and femur. Children and young adults, predominantly females, are affected in the second and third decades of life. GCRG are further classified into two distinct clinical forms-the peripheral type, involving the gingival and alveolar mucosa; and the central type which causes lytic destruction at the intraosseous level [4]. Although GCRG is described as a lytic lesion, the cortex usually remains intact. In the more aggressive type, cortical erosion and soft tissue expansion has been described.
Radiologically it presents as a solitary radiolucent expansive lesion with sharp margination. FNAC is suggestive of a giant cell rich lesion and histopathological examination of the excised specimen shows giant cells arranged around hemorrhagic areas with stromal cells in storiform pattern and periphery showing osteoid formation [5,6]. IHC findings suggest that the giant cells exhibit both osteoclastic and fibroblastic (or myofibroblastic) phenotype since they are positive for Vimentin as well as CD68. The mononuclear cells, however, are the major proliferative elements in the reparative granuloma and a subpopulation of these cells may represent precursors of the multinucleated giant cells [9]. Other Giant cell lesions of the bone should be considered in the differential diagnosis: Giant cell tumor (GCT), fibrous dysplasia, aneurysmal bone cyst, lesions of primary and secondary hyperparathyroidism (Brown tumor) and Cherubism [7].
Conclusion
The most important differential diagnosis for GCRG is that of GCT. GCT is distinctly unusual in the jaw and has a characteristic epiphyseal involvement in long bones. The giant cells are more regularly and uniformly distributed in GCT with a more uniformly ovoid stromal cell population, in which the nuclei are similar to those of the giant cells. Fibrous dysplasia has a characteristic presence of Chinese figure like trabeculae of immature or woven bone within a proliferating fibroblastic stroma. Aneurysmal bone cyst shows large spaces filled by blood and is hence excluded. Brown tumor of Hyperparathyroidism is identical to GCRG but is ruled out on the basis of normal serum levels of calcium, phosphorous, alkaline phosphatase and adequate renal function. Cherubism, which is hereditary intraosseous fibrous swelling of the jaw, usually has bilateral presentation in a young individual with a hereditary autosomal dominant mode [7]. The accurate diagnosis of GCRG has considerable importance since it has relatively better prognosis and a surgery ranging from simple curettage to resection is usually curative. However, in cases of aggressive and extensive lesion, it must be completely excised because of high rate of recurrence after incomplete removal [8].
References
- Olvi, Liliana G, Maria L. Gonzalez, Eduardo Santini-Araujo (2015) Giant Cell Reparative Granuloma. Tumors and Tumor-like lesions of Bone, Springer, London, UK, pp. 793-800.
- Whitaker SB, Waldron CA (1993) Central giant cell lesions of the jaws, a clinical, radiologic and histopathologic study. Oral Surg Oral Med Oral Pathol 75(2): 199-208.
- KA Jeevan Kumar, S Humayun, B Pavan Kumar, J Brahmaji Rao (2011) Reparative giant cell granuloma of the maxilla. Ann Maxillofac Surg 1(2): 181-186.
- Rodrigo Gadelha Vasconcelos, Marcelo Gadelha Vasconcelos, Lélia Maria Guedes Queiroz (2013) Peripheral and central giant cell lesions: Etiology, origin of giant cells, diagnosis and treatment. J Bras Patol Med Lab 49(6): 446-452.
- De Corso E, Politi M, Marchese MR, Pirronti T, Ricci R (2006) Advanced giant cell reparative granuloma of the mandible: Radiological features and surgical treatment. Acta Otorhinolaryngol Ital 26(3): 168-172.
- Morris JM, Lane JI, Witte RJ, Thompson DM (2004) Giant cell reparative granuloma of the nasal cavity. AJNR Am J Neuroradiol (25): 1263-1265.
- Pogrel AM (2012) The diagnosis and management of giant cell lesions of the jaws. Ann Maxillofac Surg 2(2): 102-106.
- Seo ST, Kwon KR, Rha KS, Kim SH, Kim YM (2015) Pediatric aggressive giant cell granuloma of nasal cavity. Int J Surg Case Rep 16: 67-70.
- Tian XF, Li TJ, Yu SF (2003) Giant cell granuloma of the temporal bone: a case report with immunohistochemical, enzyme histochemical, and in vitro studies. Arch Pathol Lab Med 127(9): 1217-1220.
- Schlorf RA, Koop SH (1977) Maxillary Giant cell reparative granuloma. Laryngoscope 87(1): 10-17.





























