Research Article
Spectrum of Etiological Factors for Hoarseness: A Retrospective Study in a Teaching Hospital
Ramesh Parajuli*
Department of Otorhinolaryngology, Chitwan Medical College Teaching Hospital, Nepal
7The Ottawa Hospital and Ottawa Research Institute, Canada
Submission: March 17, 2016; Published: May 11, 2016
*Corresponding author: Ramesh Parajuli, Department of Otorhinolaryngology, Chitwan Medical College Teaching Hospital, P.O.Box:42, Chitwan, Nepal, Tel: +977-56-532933; Fax: +977-56-532937; Email: drrameshparajuli@gmail.com
How to cite this article: Ramesh P. Spectrum of Etiological Factors for Hoarseness: A Retrospective Study in a Teaching Hospital. Glob J Oto. 2016; 1(3): 555561. DOI: 10.19080/GJO.2016.01.555561
Abstract
Introduction: Hoarseness is a common complaint encountered by Otorhinolaryngologist in daily practice. It can result from various causes ranging from minor infection to a more sinister pathology like malignancy. Thorough history and physical examination along with fibreoptic laryngoscopy and other special investigations may have to be performed to diagnose the cause of hoarseness.
Objective: To evaluate the etiological factors of hoarseness.
Materials and methods: This is a retrospective study carried out among the patients presenting with hoarseness in a study period from August 2014 to July 2015 in a teaching hospital. Routine as well as special investigations were performed when necessary to reach the diagnosis.
Results: There were a total of 76 patients; 46 being the males and 30 were females. The most common cause of hoarseness was vocal nodule accounting for 34.21% of cases; followed by 15.78% of patients each of functional voice disorder and laryngeal carcinoma; and inflammatory cause was responsible in13.15% cases of hoarseness. Neurological etiology was the least common cause of hoarseness (4; 5.26%).
Conclusion: The spectrum of etiological factors for hoarseness varies from minor functional voice disorders to a major pathological condition such as malignancy. Habitual dyshponia resulting from vocal abuse and misuse was responsible for the hoarseness in majority of our patients.
Keywords: Hoarseness; Dysphonia; Vocal Nodule; Laryngitis; Laryngeal Carcinoma
Abbreviations: MLS: Micro Laryngoscopic Surgery; ENT: Ear, Nose and Throat; NPL: Naso Pharyngo Laryngoscopy; CT: Computed Tomography; HPE: Histo Pathological Examination; COPD: Chronic Obstructive Pulmonary Disease
Introduction
Hoarseness is defined as a change in the quality of voice which is caused by abnormal vocal cord movement [1]. Hoarseness is a vague complaint that encompasses various terms such as dysphonia, aphonia, dipophonia, dysresonance, voice breaks, odynophonia and vocal fatigue [2]. Hoarseness is a common reason for a visit to Otolaryngologists as it hampers the quality of life of an affected person. It is a symptom rather than a disease entity. So, the underlying cause has to be searched for.
Hoarseness is more common in certain professions such as teachers, singers, salesmen, preachers and leaders who have excessive use and misuse of voice. Young children who have habit of excessive talking or screaming are frequently suffered from this problem. Teachers have been found to have a higher incidence of dysphonia [3]. The etiology of hoarseness varies from upper respiratory tract infection to malignancies. Based on the onset of symptom hoarseness can be divided into acute and chronic [4]. Acute onset hoarseness is commonly seen which is usually associated with upper respiratory infection such as laryngitis, and the other causes include vocal abuse, smoking, laryngeal trauma and thyroid surgery [5]. Chronic or persistent hoarseness can be caused by vocal nodule, vocal cord polyp, vocal abuse, functional dysphonia, laryngeal neoplasms, respiratory papilloma, laryngo pharyngeal reflux disease, post nasal drip, neoplasm of thyroid, esophagus and lung; granulomatous diseases like tuberculosis; and systemic diseases such as hypothyroidism and diabetes mellitus [6-9]. Most cases of acute onset hoarseness improve with conservative therapy such as vocal hygiene, voice rest, medications and voice therapy. All of these patients may not require laryngoscopic examination as these cases usually do not progress. However, hoarseness that lasts for longer than 3 weeks should be evaluated thoroughly [10]. Benign tumors like papiloma, haemangioma; or tumors like masses such as vocal nodule, vocal polyp and cyst causing hoarseness that do not respond to conservative therapy often need microlaryngoscopic surgery (MLS) of the lesions which has both diagnostic and therapeutic value. The delay in diagnosis of serious underlying disease such as malignancy; will have adverse effect on the prognosis. The main aim of this study is to evaluate the etiological factors responsible for hoarseness in patients presenting to a tertiary care hospital.
Materials and Methods
It is a retrospective study conducted among consecutive patients presenting with hoarseness or change in quality of the voice to the Otorhinolaryngology department of Chitwan Medical College Teaching Hospital, Nepal. The study period was from August 2014 to July 2015. The detailed history, thorough clinical (ENT and systemic) examination and the nasopharyngolaryngoscopy (NPL) were carried out in all of the patients. Routine and other investigations like chest x-ray, X-ray of soft tissue neck as well as special investigations such as direct laryngoscopy, computed tomography (CT) scan and histopathological examination (HPE) of laryngeal mass lesions were performed to find out the etiological diagnosis of hoarseness when necessary. The ENT examination of such patients included the examination of oral cavity, oropharynx, nose and nasopharynx, lower cranial nerves, cervical lymph nodes, laryngeal crepitus. Visual inspection of the larynx and hypopharynx was tried in almost all cases with indirect laryngoscopy as it is a simple and cost effective method. Fiberoptic laryngoscopy was also performed in all the cases for the diagnosis and exclusion of laryngeal causes of hoarseness. The data thus obtained from hospital record books was analyzed using SPSS 16 software.
Results
There were a total of 76 patients included in this study. Among these patients 42 (55.26%) were males and 34 (44.73%) were females with the male to female ratio of 1.23:1. The age range of the patients was 9 years to 89 years. The majority of patients presenting with change in voice belonged to the age group 31-40 years (20; 26.31%). The causes of hoarseness are shown in the Table 1.
Table 1: Etiological distribution of patients with hoarseness (n=76).
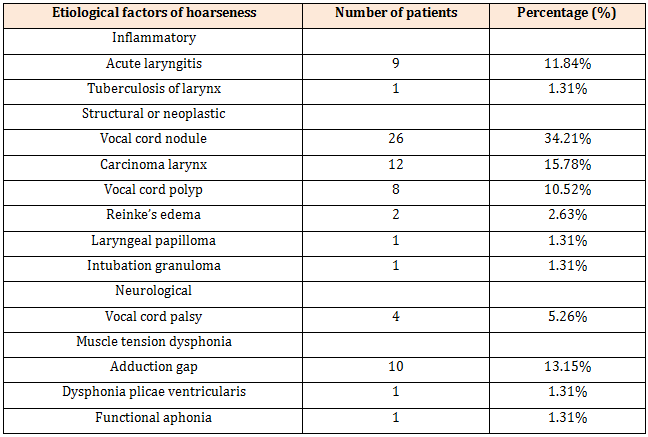
Discussion
Hoarseness is a term commonly used to describe any change in the quality of voice. However, some surgeons prefer to use the terms aphonia and dysphonia. The term ‘aphonia’ is used when there is no voice or a mere whisper; and ‘dysphonia’ is used to describe any alteration in quality of the voice. Hoarseness is a common reason for the patients seeking Otolaryngologist consultation in daily practice as it hampers the patient’s quality of life. Patients who use professional voice usually present early to an Otorhinolaryngologist when there is any change in voice. It may also be easily misdiagnosed and neglected in people who do not use professional voice especially in developing country like ours. We performed flexible NPL examination in all of our patients. Although video stroboscopic examination has been found to be a valuable tool in the early detection and diagnosis of various causes of dyshponia, it is not available in our hospital.Hoarseness can affect people of all ages which are reflected in this study as the age range was 9-89 years. Present study showed a male preponderance with a male to female ratio of 1.23:1 that is similar to the results of Nwaorgu et al. [11] and Pal et al. [12] but the result is in contrast to many other studies which reported hoarseness to be more common in women [10,13,14]. In this study, the most common age group affected by change in voice was age group of 31-40 years, similar to the results of Batra et al. [15]. Although hoarseness can be a complaint of an underlying disease or condition in any age group ranging from young children to elderly people; overall the people of younger ages have been found to be more commonly involved as seen in some other studies [15,16]. People of younger age belongs to the productive group who are mostly involved in the vocal abuse and are concerned with the change in their voice which probably be the reason for majority of our patients belonged to younger age group. In spite of having the primary symptom of change in voice the other associated symptoms that were present in our patients included various symptoms such as sore throat, fever, cough, repeated desire of clearing throat, foreign body sensation in throat, vocal fatigue, dysphagia, odynophagia, dyspnea and neck swellings. The causes of hoarseness range from trivial viral infection to a serious pathology like malignancy. Similar etiological spectrum was also found in this study. Disorders of the voice are often multifactorial in aetiology. Frequently there is more than one condition to cause voice disorder for example muscle tension imbalance along with extra-esophageal (laryngopharyngeal) reflux. The causes of voice disorders can be classified to 4 main groups such as inflammatory, structural or neoplastic, neuromuscular and muscle tension imbalance [17].
In this study the most common cause for hoarseness of voice was found to be vocal nodule (34.21%). However, Baitha et al. [16] reported vocal nodules in only 12.72% of their patients. Koufman and Isaacson [2] have developed a classification system for professionals based on their level of voice use. Level I (Elite vocal performers): Voice users such as singers and actors, for whom even a mild vocal problem causes serious consequences to their careers. Level II (Professional voice users): Voice users for whom a moderate vocal difficulty would hamper adequate job performance; which includes the following professionals like clergymen, lecturers, politicians, public speakers, and telephone operators. Level III (Non-vocal professionals): Professionals in this group can perform their jobs with slight or moderate voice problems; only severe dysphonia endangers adequate job performance. This group includes teachers, doctors and lawyers. Level IV (Non-vocal/non-professionals): These are the people who are not impeded from doing their work when they experience any kind of dysphonia. People belonging to this group are labourers, farmers, homemakers and clerks. According to this classification, in the present study we found most of our patients presenting to us with change in quality of the voice were the teachers of primary and middle schools who belongs to the level III professionals. Other structural or neoplastic causes of hoarseness in this study were vocal cord polyp (10.52%); Reinke’s edema (2.63%), papilloma of vocal cord (1.31%) and intubation granuloma (1.31%).
Carcinoma of larynx and hypopharynx was found to be present in 12 (15.78%) patients. It was the second most common cause of hoarseness in our patients. Similar incidence i.e. 14.54% of patients having laryngeal carcinoma has been reported by Batra et al. [15] in their study. Some of our patients who were from remote villages were misdiagnosed at primary health centre (PHC) as having chronic obstructive lung disease (COPD) and; were on bronchodilators and other medications such salbutamol and steroid inhalers. Malignancy has to be ruled out in patient with persistent hoarseness of more than 3 weeks especially in chronic smoker who is above 45 years of age.
Both muscle tension dysphonia; and carcinoma of larynx and hypopharynx were responsible for the hoarseness in equal percentage of our patients i.e. 15.78% in each group. Frequency of adduction gap, dysphonia plicae ventricularis and functional aphonia that were responsible for muscle tension dysphonia is shown in the Table 1. Voice therapy is the mainstay of treatment for the muscle tension dysphonia. In our study, the frequency of acute laryngitis was 11.84% which was much lower than the study performed by Baitha et al. [16] that is 23.63%. Tubercular laryngitis was reported in a single patient (1.31%) in this study similar to the finding of Batra et al. [15] which is in contrast to the findings of Baitha et al. [16] who reported 5.45% frequency of tubercular laryngitis. Vocal cord palsy was responsible for hoarseness in 5.26% of our patients which is lower than the findings of Baitha et al. [16] (10; 9.09%). Vocal cord paralysis following hemithyroidectomy was responsible for a case of hoarseness which was temporary in nature that subsided later. Two were the cases of carcinoma of lung; however in a single patient the cause of vocal cord paralysis could not be identified and was labeled as ‘idiopathic’.
Regarding the treatment options, first of all such patients with change in voice should be assessed in a voice clinic in presence of speech and language pathologist where a treatment plan can be made. The type of treatment is based on the etiology of hoarseness. However, it usually consists of vocal hygiene, lifestyle and dietary advice, voice therapy, voice rest, medical treatment, MLS or phonosurgery. If the cause is malignancy then that follows a different treatment regimen based on the stage of tumor and patient’s desire to preserve or not the larynx.
In developing countries like Nepal lower socioeconomic status, poor nutrition and health condition, smoking and drinking habits and vocal habit are probably the major predisposing factors for the various causes of hoarseness. Improving the health status and awareness in general population in our society may help decrease the incidence of hoarseness.
Conclusion
The spectrum of etiological factors for hoarseness encompasses infections, minor functional voice disorders to a major pathological condition such as malignancy. Habitual dyshponia resulting from vocal abuse and misuse was responsible for the hoarseness in majority of our patients.
Author’s contributions
RP: Carried out acquisition of data and its analysis and interpretation; and drafting of manuscript.
Acknowledgement
I would like to thank Dr. Tilak raj limbu, the head of the department of Otorhinolaryngology for critically reviewing the manuscript.
References
- Loyns BM (1994) Doctor, my voice seems husky. Aust Fam Physician 23(11): 2111-2119.
- Koufman JA, Isaacson G (1991) The spectrum of vocal dysfunction. The Otolaryngologic clinics of North America: Voice disorders. Philadelphia WB Saunders, USA 24(5): 985-988.
- Roy N, Merrill RM, Thibeault S, Parsa RA, Gray SD, et al. (2004) Prevalence of voice disorders in teachers and the general population. J Speech Lang Hear Res 47(2): 281-293.
- Dettelbach M, Eibling DE, Johnson JT (1994) Hoarseness from viral laryngitis to glottic cancer. Postgrad Med 95(5): 143-146.
- Chagnon FP, Moulder DS (1996) Laryngotracheal trauma. Chest surg din north Am 6: 73 -78.
- Smit CE, Van Leeuwen JA, Mathus-Vliegen LM, Devriese PP, Semen A, et al. (2000) Gastropharyngeal and gastroesophageal reflux in globus and hoarseness. Arch Otolaryngol Head Neck Surg 126(7): 827-830.
- Woodson GE, Blitzer A (2005) Neurologic evaluation of the larynx and pharynx. In: Cummings Otolaryngology Head and Neck Surgery, 4th (edn), St. Lous Mosby, 61-17.
- Ramazan HH, Tarazi ARE, Baroudy FM (1993) Laryngeal tuberculosis presentation of 16 cases and review of literature. J Otolaryngol 22(1): 39-41.
- Acharya VK, Sahoo R, Sreedharan S, Anand R, Pathak R (2008) Rare causes of voice hoarseness: A case report. Nepal Med Coll J 10(2): 141- 143.
- Cohen SM, Kim J, Roy N, Courey M (2014) Factors influencing referral of patients with voice disorders from primary care to otolaryngology. Laryngoscope 124(1): 214-220.
- RNwaorgu OG, Onakoya PA, Ibekwe TS, Bakari A (2004) Hoarseness in adult Nigerians: A University College Hospital Ibadan experience. Niger J Med 13(2): 152-155.
- Pal KS, Kaushal AK, Nagpure PS, Agarwal G (2014) Etiopathological Study of 100 Patients of Hoarseness of Voice: In a Rural Based Hospital. Indian J Otolaryngol Head Neck Surg 66(1): 40-45.
- Roy N, Merill RM, Gray SD, Smith EM (2005) Voice disorders in the general population prevalence, risk factors, and occupational impact. Laryngoscope 115: 1988-1995.
- Smith E, Kirchner HL, Taylor M, Hoffman H, Lemke JH (1998) Voice problems among teachers: Differences by gender and teaching characteristics. J Voice 12(3): 328-334.
- Batra K, Motwani G, Sagar PC (2004) Functional voice disorders and their occurrence in 100 patients of hoarseness as seen on fibreoptic laryngoscopy. Indian J Otolaryngol Head Neck Surg 56(2): 91-95.
- Baitha S, Raizada RM, Singh AK, Puttewar MP, Chaturvedi VN (2002) Clinical profile of hoarseness of voice. Indian J of Otolaryngol Head Neck Surg 54(1): 14-18.
- McGlashan J (2008) Disorders of the voice. In: Scott-Brown’s Otorhinolaryngology, Head and Neck Surgery, 7th (edn), Edward Arnold, London, UK, 2192-2210.





























