Clinically, Radiologically and Biochemically Metastatic Cancer Prostate: could be treated without Biopsy? A Clinical Case Study
Bader A Abdelmaksoud1,2*, Fayez G Alruwaily3, Zaki Alalem4 and Ahmad A Dafaallah5
1Clinical oncology, Oncologist, King Abdulaziz Specialist Hospital, Aljouf, KSA
2Lecturer of clinical oncology, Faculty of medicine, Zagazig university, Egypt
3Consultant family medicine and palliative care physician, King Abdulaziz Specialist Hospital, Aljouf, KSA
4Consultant radiologist, King Abdulaziz Specialist Hospital, Aljouf, KSA
5Urologist, King Abdulaziz Specialist Hospital, Aljouf, KSA
Submission: May 17, 2019; Published: May 24, 2019
*Corresponding Address:Bader A Abdelmaksoud, Clinical oncology, Oncologist, King Abdulaziz Specialist Hospital, Aljouf, KSA, Lecturer of clinical oncology, Faculty of medicine, Zagazig university, Egypt
How to cite this article:Bader A A, Fayez G A, Zaki A, Ahmad A D. Clinically, Radiologically and Biochemically Metastatic Cancer Prostate: could be treated without Biopsy? A Clinical Case Study. Canc Therapy & Oncol Int J. 2019; 13(5): 555873. DOI:10.19080/CTOIJ.2019.13.555873
Abstract
Diagnosis of prostate cancer is suspected if there are abnormalities during digital rectal examination (DRE) and/or steady rising in levels of prostate specific antigen (PSA) and the confirmative diagnosis is established by histopathological confirmation of malignancy by biopsy from the prostate. In this report, 87 years old male diagnosed clinically (DRE), radiologically and biochemically (markedly elevated PSA level) as a case of advanced prostate cancer and started treatment without biopsy. After one month of treatment and then after, the quality of life of the patient was significantly improved, and within 7 months patient showed radiologically and biochemically complete response, so, treatment of advanced prostate cancer might be started without biopsy if there is high probabilities malignancy in exceptional cases.
Keywords:Prostate cancer; Androgen deprivation therapy; Biopsy
Introduction
Worldwide, Prostate cancer (PCa) is one of the most common cancers in old men (≥ 70 years of age) and one of the major health concerns in both developed and developing countries [1]. The risk factors for PCa development still not be well understood, but old age, heredity and ethnic predisposition might be encountered in its development [2]. Also, there are exogenous factors that might affect the development of PCa as certain types of foods, pattern and type of sexual activities, consumption of alcohol, ultraviolet ray exposure, occupational exposure and less frequently chronic prostatitis [3]. Patients with advanced PCa usually symptomless or presented with nonspecific symptoms and the diagnosis usually reached by routine investigations such as laboratory tests and radiological scans for symptoms such as back pain or other bony aches, generalized fatigue or unexplained weight loss [4]. PCa diagnosis is suspected if there are abnormalities during digital rectal examination (DRE) and/or steady rising in levels of prostate-specific antigen (PSA) andthe confirmative diagnosis is established by histopathological confirmation of malignancy in core biopsy or specimens from the prostate. PSA is a serum biomarker that has important role in PCa detection [5]. PSA is organ specific but cancer nonspecific, so, its rising not only indicate PCa but also may be present in other benign prostatic conditions as hypertrophy, prostatic inflammation but fortunately, it is considered an independent easy, cheep, feasible indicator for PCa prediction than transrectal ultrasound (TRUS) or DRE [6].
Biopsy of the prostate usually needed for suspected cases with elevated level of PSA or abnormalities by DRE, but age of the patient, other co-morbidities, and subsequent therapeutic options should be taken in mind before going to perform it [7]. By any way, ultrasound guided prostatic biopsy either transrectal or perineal approach is considered the standard of care to obtain biopsy from the prostate [8,9]. Expected or reported complications that may be occurred after biopsy includehaematuria, haematospermia, rectal bleeding, prostatitis, epididymitis, urinary retention and few other complications [10]. When diagnosis of PCa is established, the treatment will be based on the stage of the disease, in very early cases with localized disease, treatment of PCa usually with watchful waiting, active surveillance or both specially for men with multiple comorbidities or limited life expectancy, in more advanced cases but still localized PCa, local radiotherapy or radical prostatectomy will be alternative options according patient and tumor conditions [11,12]. For more advanced and metastatic disease, the primary standard of care is androgen deprivation therapy (ADT). ADT could be achieved either by testicular androgen suppression or inhibition of circulating androgens receptors by anti-androgens or both methods to achieve what could complete androgen blockade (CAB) [13]. This study will report a case of advanced PCa diagnosed clinically, radiologically and biochemically (markedly elevated PSA level) and treated without biopsy.
Case study
History
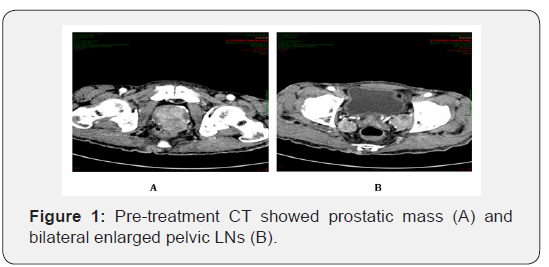
87 years old male not diabetic nor hypertensive or other co-morbidities, family history was unremarkable. He was well apart from mild low back pain associated with mild irritative urinary symptoms, but in last few months, patient cannot carry on ordinary day activities. Patient went to urology clinic due his urinary symptoms, by examination, patient looked markedly ill, unable to walk without support of his relatives, appeared to be underweight, Wt: 35kg Height: 150.5 cm , systematic review revealed no remarkable abnormalities apart from loss of subcutaneous fat in abdominal wall, both thighs and arms, DRE revealed markedly significant indurations of the prostate mainly on the posterior part of the left lobe, PSA and computed tomography (CT) chest, abdomen and pelvis were asked. CT showed that, the prostate was heterogeneously enlarged in size measured 56 x 50 x 47 mm with loss of the pre rectal fat plan and showed inhomogeneous exophytic mass in its posterior aspect measures about 42 x 31 mm associated with multiple bilateral significantly enlarged pelvic LNs and multiple sclerotic bony lesions mainly at lumbosacral region of vertebral body (Figure 1). PSA was very high, ≥700ng/L.
So, based on these clinical, radiological and biochemical findings, this case was diagnosed provisionally as a case ofadvanced prostate cancer. The next step after these findings was to go for prostatic biopsy, but unfortunately biopsy maneuvers either by TRUS or other methods were not feasible at our Centre at that time, so patient was ordered to be referred to another higher Centre in other region for further evaluation and management, but due to some social and cultural issues patient was reluctant to accept this decision and did not go to complete his work up and start treatment, this condition continued for three to four months during which the general conditions of the patient worsened and the patient became nearly chair holder most of time, so there was no way to start treatment without biopsy. Explanation of all aspects of benefits and risks with patient and his family was counseled, finally they agreed and informed written consent was taken, and treatment was started.
Treatment
Treatment was started as a front-line ADT by anti-androgen (biclutamide 150 mg) per-oral once daily for two weeks then combination of LHRH agonist (gosrolin 3.6mg) monthly with biclutamide 50mg once daily to achieve CAB. Other symptomatic and supportive maneuvers as analgesics, bone targeted therapy (denusomab), Vit D and calcium supplementation also offered. Patient was followed every other week by history, physical examinations. First radiological and biochemical (PSA, testosterone) assessment were ordered after three months from the start of the treatment then PSA monthly continuously
Results
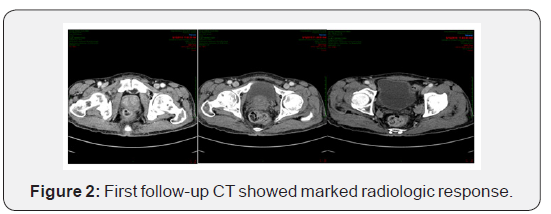
After one month of treatment and then after, general conditions of the patient started to be significantly improved, the patient could do ordinary daily life activities with out or with minimal help, can walk alone by stick support, anorexia disappeared, skin wrinkles due loss of subcutaneous fat decreased markedly, this was noted during subcutaneous injection, regarding the pain, the patient was analgesic free from the 4th month after the treatment, generally the quality of life of the patient was markedly improved. Radiologically, the first follow-up CT showed considerable decrease of the mass size with partial restore of the pre rectal fat plan, together with remarkable regression of the pelvic lymph nodal size (Figure 2).
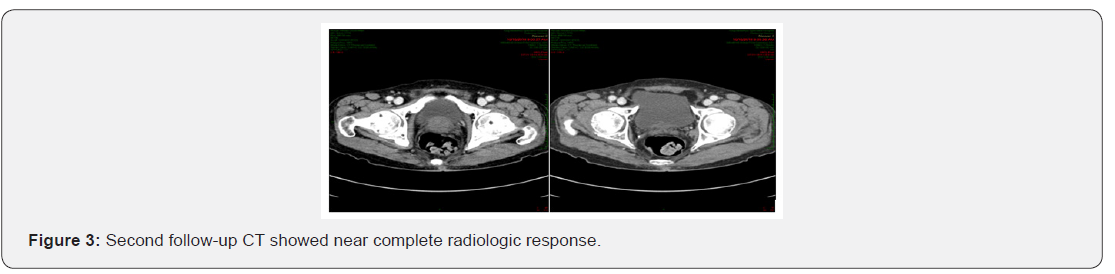
Second follow-up CT scan within four months interval showed total non-visualization of the previous prostatic mass, with marked decrease of the lymph nodal size (Figure 3). Biochemically, after three months of treatment, PSA level decreased markedly, dropped from ≥700ng/mL to 6.867 ng/mL, and then continued to decrease in subsequent monthly evaluations (Table 1). Serum testosterone level was tested 1,3,6months after starting of the treatment to be sure that we reached the castrate level, the last level at 6 months was 0.31nml/L.

Discussion
The term advanced prostate cancer refers to cases with locally advanced tumor either invading (bladder, rectum or pelvic wall) with or without regional lymph-nodes involvement or metastatic disease with non-regional lymph-nodes involvement or metastasis to other body sites, commonly bone [14]. In patients suspected to have PCa by either clinical examination or imaging studies, the high level PSA is a highly indicative of advanced prostate cancer, it is believed that PSA level more than 20ng/ml is strongly suggestive of advanced disease, and a level >50ng/ ml is a substantially diagnostic of tumor metastasis [15,16]. The current practice guidelines require biopsy before treatment to confirm histological evidence of PCa, despite this procedure has risks of some complications [17]. So, some practice guidelines recommended that no need for biopsy for advanced cases if it is highly suspected clinically and radiologically [18], this option not mentioned clearly in most of cancer practice guidelines. Surprise, Keller and Kua treated two cases of early prostate cancer by radical prostatectomy without biopsy based on clinical, radiological and biochemical diagnosis [19]. For current case the diagnosis also based on clinical examination (DRE), radiological findings (CT) and biochemical tests( markedly elevated PSA) and the treatment started after patient and family counseling for high probabilities of PCa and they were satisfied that diagnosis was correct and they were informed about small risk of treatment even the response not good as expected, but the response to the treatment was very good, clinically and biochemically and the patient achieve marked response and regained his fully good quality of life not more than 7 months of treatment
Conclusion and Recommendation
Based on the findings of this study supported with recent recommendations of NICE guidelines and some reported case series, if there is high probabilities for PCs by DRE, imaging studies and significant rising in PSA level, treatment should be started without prostatic biopsy in exceptional cases due toany reason make the biopsy not feasible. the findings in this clinical case study should be added to previous case reports and series and encourage future reports to established new recommendations to forgo the biopsy and start treatment in some circumstances of PCa.
References
- Gronberg H (2003) Prostate cancer epidemiology. Lancet 361: 859- 864.
- Hemminki K (2012) Familial risk and familial survival in prostate cancer. World J Urol 30(2): 143-148.
- Leitzmann MF, Rohrmann S (2012) Risk factors for the onset of prostatic cancer: age, location, and behavioral correlates. Clin Epidemiol 4: 1-11.
- Cancer Council Australia (2009) Advanced prostate cancer: A guide for men and their family. ISBN: 978-0-9807421-0-7.
- Stamey TA, Yang N, Hay AR, McNeal JE, Freiha FS, et al. Prostate-specific antigen as a serum marker for adenocarcinoma of the prostate. N Engl J Med 317(15): 909-916.
- Catalona WJ, Richie JP, Ahmann FR, Hudson MA, Scardino PT et al. (1994) Comparison of digital rectal examination and serum prostate specific antigen in the early detection of prostate cancer: results of a multicenter clinical trial of 6,630 men. J Urol 151(1): 1283-1290
- Roobol MJ, Steyerberg EW, Kranse R, Wolters T, van den Bergh RC, et al. (2010) A risk-based strategy improves prostate-specific antigendriven detection of prostate cancer. Eur Urol 57(1): 79-85.
- Hara R, Jo Y, Fujii T, Kondo N, Yokoyoma T, et al. (2008) Optimal approach for prostate cancer detection as initial biopsy: prospective randomized study comparing transperineal versus transrectal systematic 12-core biopsy. Urology 71(2): 191-195.
- Takenaka A, Hara R, Ishimura T, Fujii T, Jo Y, et al. (2008) A prospective randomized comparison of diagnostic efficiency between transperineal and transrectal 12-core prostate biopsy. Prostate Cancer Prostatic Dis 11: 134-138.
- NCCN Clinical Practice Guidelines in Oncology TM (2012) Prostate Cancer Early Detection 2: 15.
- Hayes JH, Ollendorf DA, Pearson SD, Barry MJ, Kantoff PW, et al. (2013) Observation versus initial treatment for men with localized, low-risk prostate cancer: a cost-effectiveness analysis. Ann Intern Med 158: 853-860.
- Godtman RA, Holmberg E, Khatami A, Stranne J, Hugosson J, et al. (2013) Outcome following active surveillance of men with screendetected prostate cancer. Results from the Göteborg randomised population-based prostatecancer screening trial. Eur Urol 63(1): 101- 107.
- Pagliarulo V, Bracarda S, Eisenberger MA, Mottet N, Schröder FH, et al. (2012) Contemporary role of androgen deprivation therapy for prostate cancer. Eur Urol 61(1): 11-25.
- kaliks R, Giglio A (2008) Management of advanced prostate cancer. Rev Assoc Med Bras 54: 178-182.
- Di Blasio CJ, Rhee AC, Cho D, Scardino PT, Kattan MW, et al. (2003) Predicting clinical end points: treatment nomograms in prostate cancer. Semin Oncol 30(5): 567-586.
- Partin AW, Mangold LA, Lamm DM, Walsh PC, Epstein JI, et al. (2001) Contemporary update of prostate cancer nomograms (Partin tables) for the new millennium. Urology 58(8): 843-848.
- Lange D, Zappavigna C, Hamidizadeh R, Goldenberg SL, Paterson RF, et al. (2009) Bacterial sepsis after prostate biopsy--a new perspective. Urology 74(6): 1200–1205.
- National collaborating Centre for cancer (2014) Prostate cancer: diagnosis and treatment. NICE clinical practice guidelines.
- Keller A, Kua B (2015) Case Report: Radical prostatectomy without prostate biopsy in PI-RADS 5 lesions on 3Tmulti-parametric MRI of the prostate gland. F1000Research 4: 54-62.






























