A Prospective Study to Compare Concomitant Boost Radiotherapy and Conventional Radiotherapy in Oral Cavity Cancer
Yadav Raj kumar*, Prasad SN, Kumar Nitin, Singh Sharad and Verma sanjay kumar
Department of Radiation Oncology, JK Cancer Institute, Kanpur, India
Submission: April 01, 2019; Published: May 08, 2019
*Corresponding Address:Yadav Raj Kumar, Department of Radiation Oncology, JK cancer Institute, Rawatpur main road, Kanpur, Uttar Pradesh, India
How to cite this article:Yadav Raj k, Prasad S, K Nitin, S Sharad, V sanjay k. A Prospective Study to Compare Five Fractions Versus Six Fractions of Radiotherapy Per week for the Treatment of Carcinoma Larynx. Canc Therapy & Oncol Int J. 2019; 13(4): 555866. DOI:10.19080/CTOIJ.2019.13.555866
Abstract
Background: Concurrent chemo radiation is currently considered to be the standard of care in the treatment of head and neck cancer. In developing countries like ours, a good number of patients cannot tolerate chemo radiation because of the poor general condition and financial constraints. Those patients are treated with radiation alone. The optimum radiotherapy (RT) schedule for best local control and acceptable toxicity is not yet clear. We aimed to find out whether shortening of treatment time using six instead of five RT fractions per week improves the loco regional control in squamous cell carcinoma of larynx. Cases of non metastatic squamous cell carcinoma of larynx reporting to JKCI Kanpur between September 2016 to September 2018 were randomised to receive Radical dose of 70 Gy. Study group (19 patients) received accelerated RT with 6 fractions per week, Control group (15 patients) received conventional RT with 5 fractions per week. Tumour control, acute and late toxicities were compared. Partial response was seen in 4 patients (31%) in conventional arm and 4(21%) patients in study arm. The benefit of shortening was higher for advanced disease control though it was not statistically significant Grade 3 mucositis and grade 3 skin reaction were significantly higher in accelerated radiotherapy arm
Conclusion: Radiotherapy of six fractions per week promising with a trend of better response rate and manageable side effect
Keywords: Pure accelerated fractionation; Carcinoma; Larynx
Introduction
Squamous cell carcinoma of the larynx is predominantly a locoregional disease and the primary treatment methods are surgery and radio therapy with RT being the favoured treatment if organ preservation is required [1]. The optimum Radio therapy schedule for best local control and acceptable toxicity is not yet clear. When treating squamous cell carcinoma of head and neck by RT, there is a need to optimize the irradiated volume, total dose, dose/fraction, and overall treatment time. Whether the conventional system of fractionation (i.e., 60–70 Gy in 2 Gy/ fractious, 5 times a week) is the optimal way of delivering RT in all circumstances is highly debatable. One of the most important biological factors related to the outcome of RT in squamous cell carcinoma of the head and neck is the proliferation of tumour stem cells during treatment. A cause of resistance with conventional fractionation RT could be radiation-induced accelerated proliferation of clonogenic tumour cells. A reduction in the chance of tumour control through the lengthening of treatment times has been clinically and biologically documented [2]. Furthermore, in a substantial number of clinical reports, reduction in the total treatment time has improved tumourcontrol [3,4,5]. A shorter treatment time can be accomplished by applying a higher dose per fraction, but this change will disproportionately increase the rate of late complications. Accelerated treatment is therefore only possible if the weekly number of fractions is increased without increasing the dose per fraction. This shortening of overall treatment time should limit the extent of accelerated repopulation and therefore one may expect an increase in the probability of tumour control for given total dose [6]. Since treatment time is thought to have little or no influence on the response of late reacting normal tissue, a reduction in overall treatment time would not be expected to affect the incidence and severity of late normal tissue injury. At the same time, reducing overall treatment time will increase the turnover on machine, thus will reduce the waiting list also, especially in a busy department like ours with limited resources. Keeping above facts in mind, we planned a randomized clinical trial to test the efficacy of shortening the overall treatment time from 7 weeks to 6 weeks by delivering six fractions per week instead of five fractions per week in the treatment of head and neck cancers in our institution with the aim to find out whethershortening of overall treatment time by use of this regimen is tolerable and improves the tumour response.
Methods and Materials
The case material for the study were selected from the cross section of patients registered at the J. K. cancer institute, G. S. V. M Medical College, Kanpur, between September 2016 to September 2018. eligible patients were randomized in to two arms with the help of single blind randomization in to study arm (6# per week) & control arm (5# per week) both arms received 2Gy per fraction. each patient was evaluated with Complete history, general physical examination, complete systemic examination., Body surface area (BSA). The assessment of general condition was done by using Karnofsky Performance Status. Haematological assessment was done by complete haemogram including haemoglobin, total leukocyte count (TLC), differential leukocyte count (DLC) and platelet count. Biochemical assessment to assess the kidney and liver functions were done by the estimation of blood urea, serum creatinine, SGOT and SGPT levels
Radiological assessment including chest X-ray & contrast enhancing CT scan of neck region were done in all patients and USG whole abdomen will be done in all patients. The patients were staged according to AJCC (American Joint Committee on Cancer) 8 staging system. For inclusion in the study patients needed to full fill the inclusion criteria, based on: Histologically proven cases of Carcinoma larynx, Karnofsky Performance Status > 70, Complete hemogram with HB>10gm%; TLC>4000/ cubic mm, Platelet count >100,000/cubic mm. Renal function tests with Blood urea < 40mg/DL and Serum creatinine< 1.5mg/ DL. Liver function tests with SGOT < 35 IU/L and SGPT < 40 IU/L. Patients who sign the informed consent and were ready to be on follow up as required. Patients who had metastatic disease, Prior radiation, surgery or chemotherapy for the disease, poor general condition with Karnofsky Performance Status of<70, Pregnant / lactating patients. Associated medical condition such as renal disease, liver disease or heart disease were excluded from study. Arm A constituted conventional 70 Gy with 2 Gy/ fraction for 5 days/week. While Arm B Accelerated arm 70 Gy with 2 Gy/fraction for 6 days/week. In both arms’ spine sparing after 46GY/23#. RT schedule in both arms by using CO60. Radiotherapy technique: 2 D technique, Supine position, Patients underwent a pre-treatment simulation to Work out the field borders to cover the primary tumour, disease extension, and neck nodes. B/L field were treated every day. Assessment during treatment: From the commencement of treatment, all the patients included in the study were carefully and regularly assessed weekly (Friday) during treatment. Detailed clinical evaluation of the patient for local disease status and acute toxic side effects of radiation was done by thorough local examination. Radiation reactions were assessed by Radiation Therapy Oncology Group (RTOG) criteria.
Radiation Therapy Oncology Group (RTOG) acute morbidity scoring criteria are relevant from day 1, the commencement ofradiation, through day 90 and thereafter, the RTOG criteria for late effects were applied. Tumour response (both primary and nodal response) were assessed by RECIST response criteria, 2 months after completion of Radiotherapy. The major study endpoints were tumour response, acute and late toxicities. Assessment after completion of treatment: All the patients were assessed on completion of treatment and r two months after the completion of treatment, to detect acute complications like mucositis, skin reaction. Treatment related acute toxicity graded by using common terminology criteria for adverse events (RTOG) and late toxicity by RTOG criteria. Patients were followed-up two monthly after completion of radiotherapy. Late toxicities were assessed after 6 months of completion of Radiotherapy. The tumour response was assessed by using the RECIST 1.1 criteria.
Follow up
All the patients were followed up regularly on OPD basis for a period of at least 6 months, once every month after completion of the treatment. At every visit, each patient was clinically evaluated for local control of disease and treatment related complications. The patients were assessed for any evidence of distant metastasis during each follow up. To evaluate the local disease control, local examination using inspection, palpation was done at each follow up and response was assessed. On the suspicion of any local recurrence, biopsy was taken for histopathology and correlated clinically. In case of suspicion, relevant investigations were done to rule out the presence of distant metastasis. Statistical analysis: The data thus obtained was assessed, analysed and compared to find out difference in all the groups in terms of tumour response and toxicity by comparing two parameters by fisher Z test for testing the significance between two groups. P value <005 was considered significant.
Observation
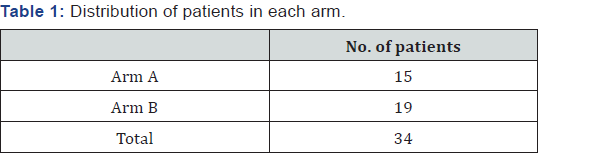
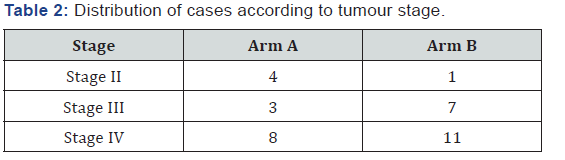
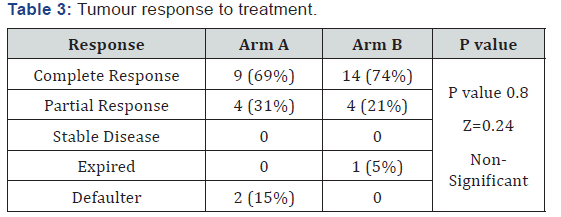
Distribution of patients in each arm (Table 1). Distribution of cases according to tumour stage. Most patient are in stage III and IV comparable in both the Arms (Table 2). Response assessment (Table 3). Tumour Response to treatment was assessed 8 weeks after completion of radiotherapy using RECIST1.1 criteria. The complete response in arm B when compared to Arm A (74% VS 69%) was found to be non-significant with a P value of 0.8
Intervention in the form of tracheostomy / Ryle’s tube insertion during treatment (Table 4).

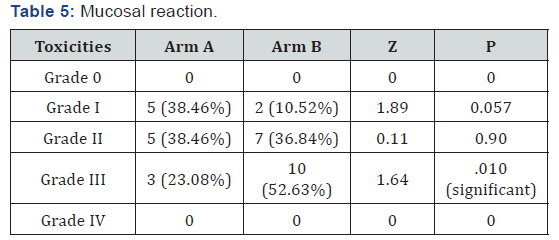
Acute toxicities at completion of treatment and the 8-week post treatment and thereafter Mucosal reaction grade III is significantly more in arm B. Acute toxicities were recorded weekly during treatment and the 8-week post treatment and thereafter
Skin Reaction (Table 6)

Skin toxicities grade 3 more in Arm B as compared to Arm A, but the difference was not statistically significant p value= 0.26.
Late Toxicities (Table 7)
We have observed late skin toxicities in the form of subcutaneous fibrosis. Subcutaneous fibrosis was present in 10 patients (in the accelerated arm and 17 patients in conventional RT arm. This difference was statistically not significant (P = 0.465). There was no significant difference in late salivary toxicities between the accelerated and conventional RT arms.

Results
At a median follow-up of 12 months, 14 patients (74%) in the 6 fractions group and 9.0 patients (69%) in the 5 fractions group were disease-free. Partial response was seen in 4 patients (31%) in conventional arm and 4(21%) patients in study arm. The benefit of shortening was higher for advanced disease control though it was not statistically significant Grade 3 mucositis and grade 3 skin reaction were significantly higher in accelerated radiotherapy arm. These were managed conservatively. There was no drop out because of reaction. There was no difference in late toxicities between the two arms
Discussion
we observed better local control both at primary and nodal site in accelerated RT arm as compared to conventional RT arm. On first follow-up, 74% had CR at primary site in accelerated arm and 69% in conventional arm respectively. Though the difference in loco regional control was not statistically significant but this study clearly indicates a trend toward improved outcome. In Danish Head and Neck Cancer Study Group (DAHANCA) study, [7] loco regional tumour control improved significantly in the accelerated fractionation group compared with that in the conventional RT group (70% vs. 60% 5 years actuarial rate, P = 0.0005). There was 10% statistically significant improvement in loco regional disease control in accelerated arm. In International Atomic Energy Agency (IAEA)-ACC study by Overgaard et al. [8] the 5-year actual locoregional control was 42% in the accelerated versus 30% in the conventional group (P = 0.004).
In our study, the statistical significance could not have reached because of the smaller sample size and shorter followup. But our study is certainly in accordance with DAHANCA trial and IAEA-ACC study. On subset analysis, the trend of better response with accelerated fractionation was seen preferably in larynx thought it was not statistically significant. Like DAHANCA and IAEA-ACC study, the benefit of acceleration in this study was slightly higher for controlling advanced disease, but there was no difference in terms of control at early stage between the two schedules. Almost all treatment failures were due to insufficient loco regional tumor control. Therefore, disease-specific survival was strongly related to insufficient loco regional control and was therefore significantly better in patients receiving six fractions per week than for those who received five fractions per week [9].
We observed that acute complications were considerably more severe in the accelerated RT arm than those of conventional fractionation arm. Grade 3 mucositis were significantly higher in the accelerated arm as compared to conventional arm (52.6% vs.23.08%; P = 0.1004). Moreover, the mucositis persisted longer in the accelerated fractionation arm, but all healed 3 months within the start of treatment. Similarly, Grade 3 skin toxicities were seen in significantly higher number of patients in the accelerated RT arm (42%) as compared to conventional arm (23%). In our study, higher severe acute reactions seen in the accelerated RT arm were expected due to accumulated dose per week (AD) of 12 GY in accelerated arm as compared to accumulated dose per week (AD) of 10 GY in conventional arm, as acute toxicity is directly dependent on accumulated dose per week.
All toxicities were effectively managed. Regarding acute radiation related morbidity and time taken for healing of acute reaction, our findings are comparable with DAHANCA trial, where acute radiation related morbidity was significantly higher in the accelerated RT group with a 53% frequency of a confluent mucositis compared with 33% in the conventional treatment group (P < 0.0001). Regarding late toxicities in our study, we observed radiation induced late morbidity in the form of xerostomia and subcutaneous fibrosis at anterior aspect of neck, which did not differ significantly in both groups. Comparable late toxicities in two groups were expected as late morbidity depends upon dose per fraction, which was not different in two treatment arms, that is, 200CGy per fraction. In the DAHANCA trial and IAEA-ACC study too, the probability of developing a severe late radiation related complication mainly in the form of late subcutaneous fibrosis
The six fractions per week schedule, resulting in a 1-week reduction in treatment time relative to conventional treatment, seems to give a good balance between improved tumor control and avoidance of excess late morbidity. Based on our study (though it is small), DAHANCA trial and IAEA-ACC study, we feel that six fractions per week treatment is a better option as compared to five fractions per week, especially in countries where working days are 6 in a week. The conventional schedule has been evolved in West based on their working convenience rather than based on any radiobiological or scientific evidence, as they work 5 days a week. Moreover, shortening of overall treatment time will increase the turnover on treatment machine which will help to treat a greater number of patients in 1-year and will reduce the waiting. Hence, shortening of overall treatment time from 7 weeks to 6 weeks by use of 6 fractions perweek instead of 5 fractions per week is feasible, tolerable, and results in better outcome in the patients of head and neck cancer.
Conclusion
Radiotherapy of six fractions per week is reasonable alternative to the conventional five fractions per week, offers advantages of decreased overall treatment time, decreased hospital stay with comparable response rate and toxicity profile
Conflict of Interest
None.
References
- Overgaard J, Hansen HS, Jørgensen K, Hjelm Hansen M (1986) Primary radiotherapy of larynx and pharynx carcinoma – An analysis of some factors influencing local control and survival. Int J Radiat Oncol Biol Phys 12: 515–521.
- Withers HR, Taylor JM, Maciejewski B (1988) The hazard of accelerated tumor clonogen repopulation during radiotherapy. Acta Oncol 27(2): 131–146.
- Nguyen LN, Ang KK (2002) Radiotherapy for cancer of the head and neck: Altered fractionation regimens. Lancet Oncol 3(11): 693-701.
- Bernier J, Bentzen SM (2003) Altered fractionation and combined radio-chemotherapy approaches: Pioneering new opportunities in head and neck oncology. Eur J Cancer 39(5): 560–571.
- Fu KK, Pajak TF, Trotti A, Jones CU, Spencer SA, et al. (2013) A Radiation Therapy Oncology Group (RTOG) phase III randomized study to compare hyperfractionation and two variants of accelerated fractionation to standard fractionation radiotherapy for head and neck squamous cell carcinomas: First report of RTOG 9003. Int J Radiat Oncol Biol Phys 48(1): 7-16.
- ICMR (2013) Sites of cancer associated with use of tobacco in: Threeyear Report of Population based cancer registries 2009-2011. Ch. 3. Bangalore: national cancer registry programme ICMR 23-6.
- Hansen O, Overgaard J, Hansen HS, Overgaard M, Höyer M, et al. (1997) Importance of overall treatment time for the outcome of radiotherapy of advanced head and neck carcinoma: Dependency on tumor differentiation. Radiother Oncol 43(1): 47–51.
- Lyhne NM, Primdahl H, Kristensen CA, Andersen E, Johansen J, et al. (2015) The DAHANCA 6 randomized trial: effect of 6 vs 5 weekly fractions of radiotherapy in patients with glottic squamous cell carcinoma. Radiother Oncol 117(1): 91–98.
- Overgaard J, Mohanti BK, Begum N, Ali R, Agarwal JP, et al. (2010) Five versus six fractions of radiotherapy per week for squamous cell carcinoma of head and neck (IAEA-ACC study): A randomised, multicentre trial. lancet Oncol 11(6): 553-560.






























