Retroperitoneal Secretant Paraganglioma
Ines Azri1, Haifa Ben Romdhane1, Fedi Saoudi1, Welid Zakhama2, Ali Majdoub1*
1 Department of Anesthesia and Intensive Care, Mahdia hospital, Tunisia
2 Department of Urology, Mahdia hospital, Tunisia
Submission: April 10, 2018; Published: April 20, 2018
*Corresponding author: Ali Majdoub, Intensive care unit of tahar safr mahdia Hospital, Tunisia.
How to cite this article: Ines A, Haifa B R, Fedi S, Welid Z, Ali Majdoub, Retroperitoneal Secretant Paraganglioma. Curr Trends Clin Med Imaging. 2018; 2(3): 555589. DOI: 10.19080/CTCMI.2018.02.555589
Keywords: Retroperitoneal; Secretant; Paraganglioma; Kidney; Ultrasonography; Abdominal; Echocardiography;
Observation
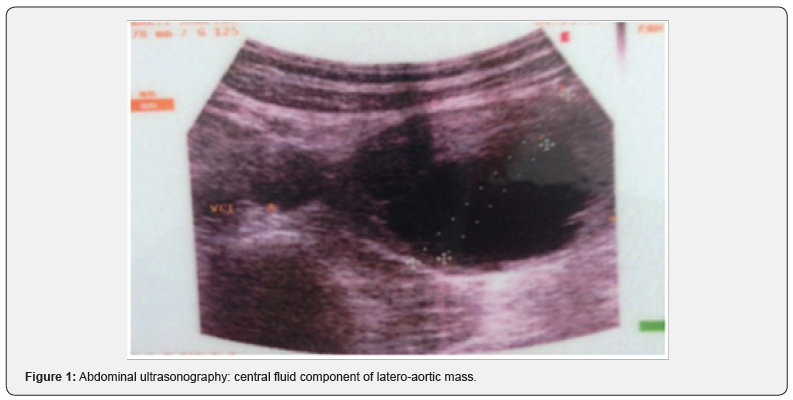
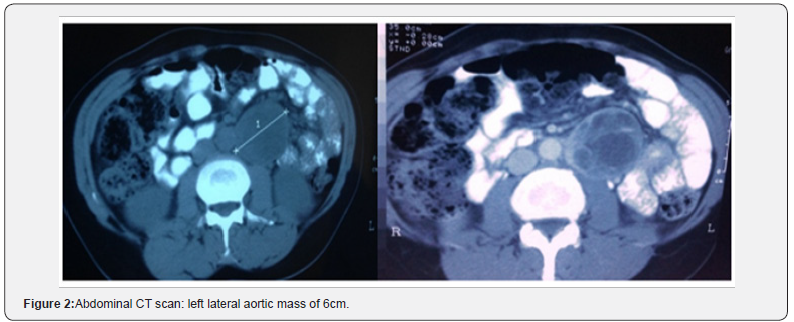
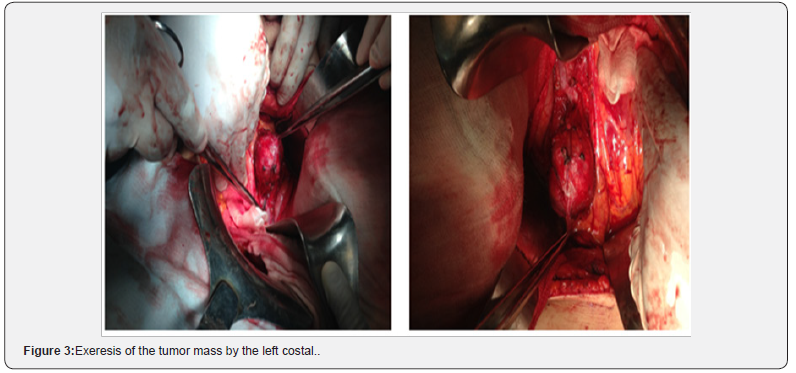
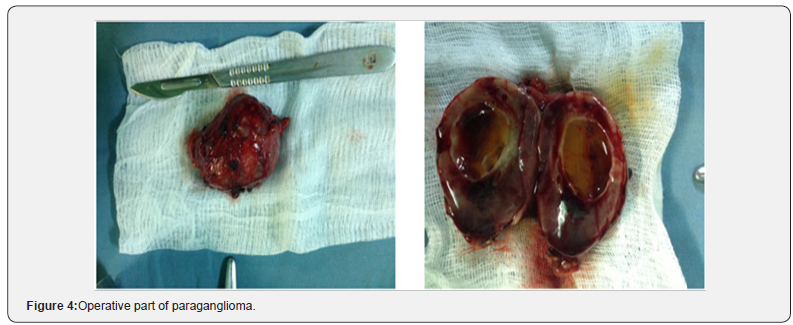
ObservationWe report a complete iconography from ultrasound to the operative specimen of a 42-year-old patient who had been treated for hypertension about 6months by a calcium channel blocker. Hospitalized for a thrust of severe hypertension. Diagnosis of pheochromocytoma was evoked and confirmed by the determination of urinary metanephrines. Abdominal ultrasonography revealed a well-defined 58x55x50mm mass with a central fluid component and a non-vascular Doppler peripheral echogenic part. Localized latero-aortic at the level of the inferior pole of the left kidney (Figure 1). Abdominal computed tomography showed a left lateral aortic mass of 6cm long axis with cystic component very probably corresponding to a paraganglioma (Figure 2). A MIBG scintigraphy shows an intense fixation of this mass suggestive aspect of para-aortic paraganglioma. Surgical treatment was then decided. Surgical excision by left costal approach was performed in Figure 3. The pathological examination concluded that it was compatible with a paraganglioma, 6cm long, with complete excision, no microscopic sign of malignancy, and no endovascular tumor extension. Control echocardiography was normal and blood pressure had become normal without treatment (Figure 4).
Comment
Retroperitoneal paragangliomas are tumors developed at the expense of neuroectodermal cells of the autonomic nervous system [1]. They are secretive in 60% of the cases and they can reach important dimensions. The frequency of the malignant forms is estimated between 20 and 50% [2] the treatment of these tumors is surgical, it consists of complete excision. All the times of the surgical procedure are at risk, the mobilization of the tumor remaining the most critical moment with a risk of hypertensive peak of up to 100%. The perioperative mortality of patients with paragangliomas has increased from 40-60% to 0-6% over the last 50years due to the improvement of the multidisciplinary management of these patients between surgeons, anesthetists, endocrinologists and cardiologists [3].
References
- Barfield R, Hill DA, Hoffer FA, Tekautz T, Spunt SL (2002) Retroperitoneal paraganglioma. Med Pediatr Oncol 39(2): 120-124.
- Arthoua TPF, Platel JP, Meusnier F, Pourrière M, Thouard H (1997) Paragangliome rétropéritonéal sécrétant. À propos d’un cas. J Chir 134: 248 -251.
- Kinney MA, Narr BJ, Warner MA (2002) Perioperative management of pheochromocytoma. J Cardiothorac Vasc Anesth 16(3): 359-369.






























