Ectopic Lingual Thyroid: Imaging Features
M Krishna Kumar* and L Rupa kumar
Associate Professor of Radiodiagnosis, Tamilnadu, India
Submission: October 12, 2017; Published: October 26, 2017
*Corresponding author: M Krishna Kumar, Associate Professor of Radiodiagnosis, Velammal Medical College & Research Institute, Tamilnadu, India.
How to cite this article: M Krishna K, L Rupa k. Ectopic Lingual Thyroid: Imaging Features. Curr Trends Clin Med Imaging. 2017; 2(2): 555582. DOI: 10.19080/CTCMI.2017.02.555582
Abstract
Ectopic Lingual thyroid (ELT) is a rare developmental anomaly, caused due to aberrant embryogenesis during the descent of thyroid gland from base of tongue to the neck. Lingual thyroid is the most common presentation of ectopic thyroid tissue. Lingual thyroid (LT) may present with symptoms like dysphagia, dysphonia, upper airway obstruction or even hemorrhage at any time from infancy through adulthood. We report a case of a 27 year old female.
Who had ELT, presented with dysphagia and foreign body sensation in the throat since 3months. The diagnosis was reached with clinical examination, computed tomography and ultrasound scan. There are different types of surgical approaches for the treatment of this condition.
Keywords: Dysphagia; Ectopic lingual thyroid; Ectopic thyroid tissue; Lingual thyroid; midline neck swelling.
Introduction
Ectopic thyroid is an uncommon embryological abnormality characterized by the presence of thyroid tissue in a site other than its usual pretracheal location [1,2]. ELT is the most common type accounting for 90% of cases, while sublingual types are less frequently encountered. The sublingual types may be suprahyoid, infrahyoid or at the level of the hyoid bone [3].
Prevalence rates of ELT vary from 1 in 100,000 to 1 in 300,000, with females to male ratio ranging from 4:1 to 7:1[4]. The reported age at diagnosis of lingual thyroid has ranged from birth to 83 yr of age, with the mean of 40.5 yr. In 70–75% of patients with lingual thyroid, there is no eutopic thyroid tissue present in the pretracheal position [5].
Clinical presentation is varying from mild dysphagia to severe upper airway obstruction. Diagnosis depends on finding thyroid tissue at the base of the tongue with the absence of normally located gland. Imaging studies such as ultrasound scan, CT scan and Technetium (Tc99m) thyroid scan would be of great value in establishing the diagnosis [6].
Fine needle aspiration cytology (FNAC) is required for confirmation of diagnosis and helps to distinguish benign from malignant lesion. We report a case of ELT presenting with dysphagia and foreign body sensation in the throat, which was diagnosed on Imaging & confirmed with FNAC.
Case Report
A 27 year old female patient presented with dysphagia and foreign body sensation in the throat since 3 months. She had no history of either past or present thyroid disease.
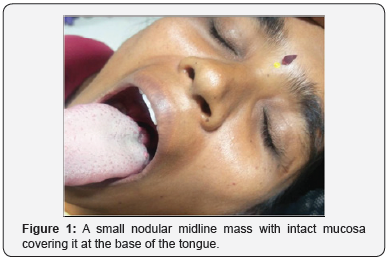
The past medical history of the patient was insignificant, and she was not currently taking any medication. Neck examination revealed neither palpable thyroid gland, cervical lymphadenopathy nor any other palpable masses. Thyroid function tests (TFT) demonstrated euthyroid levels. Other laboratory tests were within normal limits. Throat examination revealed nodular masses at the base of the tongue with congested vessels on the surface Figure 1. Laryngoscopy was performed and showed the presence of a mass at the base of the tongue, covered with intact mucosa and displacement of the uvula.
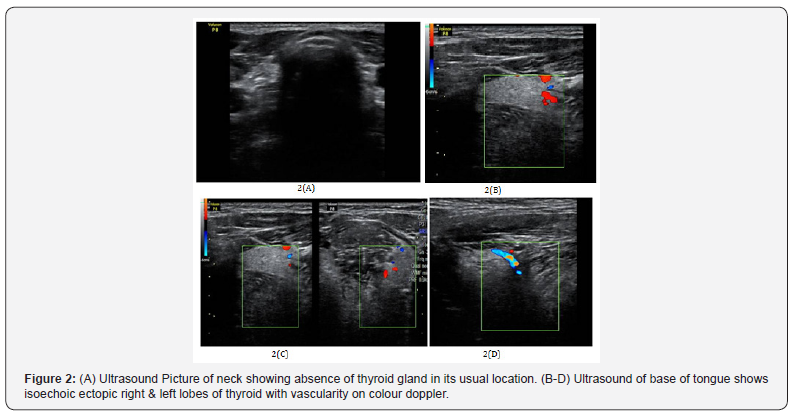
Ultrasound scan (US) of neck revealed the absence of thyroid gland in its usual location Figure 2A. US of the base of tongue showed bilobed isoechoic mass with vascularity Figure 2(B-D).
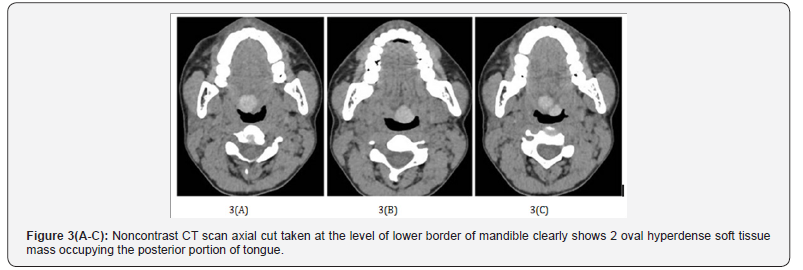
Non-contrast CT of neck done confirmed bilobed oval hyper dense mass in the base of tongue suggestive of ELT Figure 3(A-C).
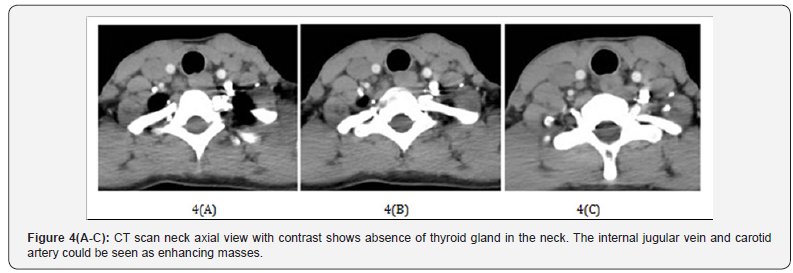
CT scan neck axial view with contrast shows absence of thyroid gland in the neck. The internal jugular vein and carotid artery could be seen as enhancing masses Figure 4(A-C).
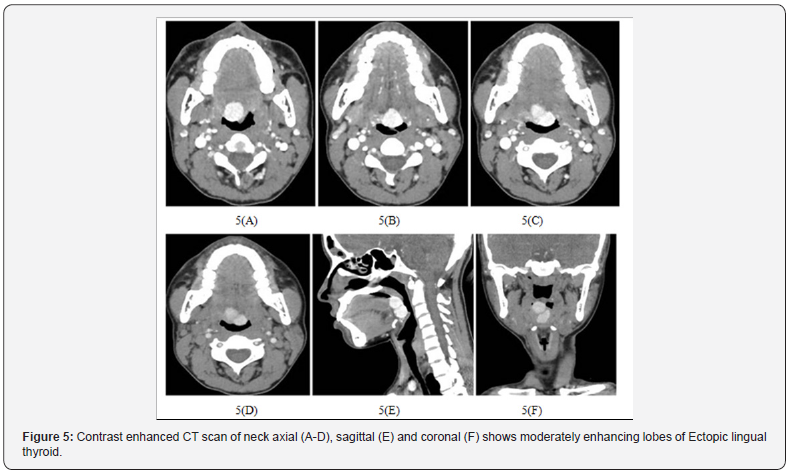
Contrast enhanced CT of neck shows moderate enhancement of both lobes of ELT Figure 5(A-F).
Discussion
Ectopic Lingual thyroid (ELT) is defined as the presence of thyroid tissue in the midline anywhere between the circumvallate papillae of tongue and the epiglottis. Hickmann recorded the first case of lingual thyroid (LT) in 1869. Montgomery stressed that for a condition to be branded as LT, thyroid follicles should be demonstrated histopathologically in tissues sampled from the lesion [7].
Early in embryogenesis, thyroid gland appears as proliferation of endodermal tissue in the floor of the pharynx between tuberculum impar and hypobranchial eminence (this area is the later foramen caecum) [3].
ELT arises from the embryonic failure of normal thyroid tissue to descend from the foramen cecum area of the tongue base through the lower neck by 7th weak of gestation and presents as a lobular midline mass in the mucosal surface of the tongue base. The exact pathogenesis of this ELT is not known [8]. The surface of the lesion is usually smooth and vascularity can be seen.
Other locations in the head and neck regions where ectopic thyroid tissue may be found include the trachea, sub-mandibular, lateral cervical regions, axilla, palatine tonsils, carotid bifurcation, iris of the eye, and pituitary gland. Furthermore, the presence of ectopic thyroid tissue in other places distant from the neck region include the heart, ascending aorta, thymus, oesophagus, duodenum, gallbladder, stomach bed, pancreas, mesentry of the small intestine , Porta Hepatis, adrenal gland, ovary, fallopian tube, uterus and vagina [9].
Ectopic thyroid is the most common cause of congenital hypothyroidism in infants [10]. 70% of patients with ELT without a co-existing eutopic thyroid tissue will develop sub-clinical hypothyroidism. This often progresses to become clinically manifest during periods of physiological stress [11].
The clinical presentation of ELT could be classified into two groups according to the appearance of the symptoms: infants and young children whose LT is detected via routine screening may suffer from failure to thrive and mental retardation, or even severe respiratory distress, resulting in a medical emergency [8,12]. Other cases may present with onset of slowly progressing dysphagia and symptoms of oropharyngeal obstruction before or during puberty. This occurs as a response to the increased demand for thyroid hormone in these hypermetabolic states. Similar response is also encountered during other metabolic stress conditions like pregnancy, infections, trauma, menopause, etc [13]. In addition, malignant transformation of the LT has been reported, albeit rarely [14]. Frequency of carcinoma in lingual thyroid is estimated to be approximately one in 100 cases with a female to male ratio ranging from 3:1 to 8: 1. The majority of these tumours are described as being of the follicular type, while papillary forms comprise 23% [15].
Palpation of the neck is extremely essential, in order to check the presence or the absence of the thyroid gland in its normal position.
High resolution ultrasound scanning (US) is generally favoured in the initial assessment of thyroid gland. The sensitivity of detection of an ectopic thyroid is enhanced by the use of colour Doppler technique by demonstrating peripheral or internal colour flow signals that are reflective of hypervascularity [16].
Computed Tomography (CT) scan and Magnetic Resonance Imaging (MRI) are valuable imaging tools in the investigation of patients with ectopic thyroid. They are especially useful when a eutopic thyroid gland is not identified by ultrasound. Ectopic thyroid tissue has a characteristic uniform high attenuation on non-contrast CT, while on MRI it shows an elevated signal on T1- and T2-weighted images compared with the surrounding musculature [17].
Radionuclide thyroid imaging employing technetium 99m pertechnetate, iodine 131 or iodine 123 is useful in the evaluation for ectopic thyroid. Thyroid tissue takes up the radioisotope and this helps in localizing the ectopic thyroid and at the same time in determining the presence of a eutopic thyroid gland [10]. The radionuclide scanning provides an approximate estimation of the size, and the degree of activity
Angiography has been used in the past to determine patterns of vascularization of LT and this can help in planning surgical intervention. It can also allow the use of embolization preoperatively to decrease the risk of intraoperative haemorrhage or serve as the primary treatment modality in patients who are treated non-operatively [18].
The main differential diagnoses are: hemangioma, thyroglossal duct cyst, dermoid cyst, midline branchial cysts, epidermal and sebaceous cysts, cystic hygroma, minor salivary gland tumours, adenoma, fibroma, lipoma and carcinoma.
Fine needle aspiration cytology (FNAC) confirms the diagnosis of ectopic thyroid and differentiates between benign and malignant lesion. Histopathology of ELT reveals a nonencapsulated collection of embryonic or mature thyroid follicles that may extend between muscle bundles [19].
Treatment depends on the size, the presence or absence of symptoms and complications like ulceration, hemorrhage, malignancy or obstruction of the upper airway.
Regular follow- up is recommended for cases completely asymptomatic and euthyroid in order to detect mass complications [20]. Levothyroxine therapy corrects hypothyroidism and also induces shrinkage of gland [16]. When symptoms of bleeding or obstruction appear, therapy by means of surgery or radioiodine ablation is warranted. There are different types of surgical approaches for the treatment of this condition. The ectopic gland may be the only functional thyroid and complete excision is followed by lifelong hormone replacement. In patients lacking thyroid tissue in the neck, the lingual thyroid can be excised and auto-transplanted to the muscles of the neck [21].
In our patient, once the diagnosis of Lingual thyroid was established, she was put on Levothyroxine therapy. She has been on regular follow up and has shown significant improvement symptomatically and some regression of the midline mass.
Conclusion
ELT is rare developmental entity which may present as dysphagia or dysphonia. It should be included in differential diagnosis of tongue masses especially in children and adolescence. Physical examination, thyroid function tests, Ultrasound scan, CT / MRI and radionuclide scanning are essential for making diagnosis. FNAC is important in to confirm ELT & exclude rare possibility of malignancy. Treatment depends on the size, the presence or absence of symptoms and complications like ulceration, hemorrhage, malignancy or obstruction of the upper airway.
References
- Yang YS, Hong KH (2008) “Case of thyroid hemiagenesis and ectopic lingual thyroid presenting as goitre”. Journal of J Laryngol Otol 122(8): e17.
- Dolezal J, Vizda J, Horacek J, Spitalnikova S (2013) “Lingual thyroid: diagnosis using a hybrid of single photon emission computed tomography and standard computed tomography”. J Laryngol Otol 127(4): 432-434.
- Batsakis JG, El-Naggar AK, Luna MA (1996) Thyroid gland ectopias. Ann Otol Rhinol Laryngol 105(12): 996-1000.
- Marina Dj, Saji´c S (2007) Lingual thyroid. Srp Arh Celok Lek 135(3–4): 201-203.
- Neinas FW, Gorman CA, Devine KD, Woolner LB (1973) Lingual thyroid: Clinical characteristics of 15 cases. Ann Intern Med 79(2): 205–210.
- Ramzisham AR, Somasundaram S, Nasir ZM (2004) Lingual thyroid - a lesson to learn. Med J Malaysia 59(4): 533-534.
- Burkart CM, Brinkman JA, Willging JP, Elluru RG (2005) Lingual cyst lined by squamous epithelium. Int J Pediatr Otorhinolaryngol 69(12): 1649-1653.
- Williams JD, Sclafani AP, Slupchinskij O, Douge C (1996) Evaluation and management of the lingual thyroid gland. Ann Otol Rhinol Laryngol 105(4): 312-316.
- Ibrahim NA, Fadeyibi IO (2011) Ectopic thyroid: etiology, pathology and management. Hormones (Athens) 10(4): 261-269.
- Yoon JS, Won KC, Cho IH, Lee JT, Lee HW (2007) Clinical characteristics of ectopic thyroid in Korea. Thyroid 17(11): 1117-1121.
- Larochelle D, Arcand P, Belzile M, Gagnon NB (1979) Ectopic thyroid tissue-a review of the literature. J Otolaryngol 8(6): 523-530.
- Rocha-Ruiz A, Beltrán C, Harris PR, Orellana P, García C, et al. (2008) Disphagia caused by a lingual thyroid: report of one case. Rev Med Chil 136(1): 83-87.
- Stoppa-Vaucher S, Lapointe A, Turpin S, Rydlewski C, Vassart G, et al. (2010) Ectopic thyroid gland causing dysphonia: imaging and molecular studies. J Clin Endocrinol Metab 95(10): 4509-4510.
- T Bao, H Wang, D Wei, Di Yu (2012) “Transposition of a lingual thyroid to the submandibular space using a modified technique” Journal of Laryngology and Otology 126(12): 1287-1291.
- Hari CK, Kumar M, Abo-Khatwa MM, Adams-Williams J, Zeitoun H (2009) Follicular variant of papillary carcinoma arising from lingual thyroid. Ear Nose Throat J 88(6): E7
- Kansal P, Sakati N, Rifai A, Woodhouse N (1987) Lingual thyroid- Diagnosis and treatment. Arch Intern Med 147(11): 2046-2048.
- Wong RJ, Cunningham MJ, Curtin HD (1998) Cervical ectopic thyroid. Am J Otolaryngol 19: 397-400.
- Rahbar R, Yoon MJ, Connolly LP, Robson CD, Vargas SO, et al (2008) Lingual Thyroid in Children: A Rare Clinical Entity. Laryngoscope 118(7): 1174-1179.
- Baughman RA (1972) Lingual thyroid and lingual thyroglossal tract remnants -A clinical and histopathologic study with review of the literature. Oral surg Oral Med Oral Pathol 34(5): 781-799.
- Rovena B, Medi A, Etmond C, Myzafer K, Rudin D, et al. (2015) Lingual Thyroid Gland: A Case Report. IOSR J Den Med Sci 14(8): 73-77.
- Jones P (1961) Auto transplantation in lingual ectopia of the thyroid gland: review of the literature and report of a successful case. Arch Dis Child 36: 164-170.






























