Quality of Postoperative Handover as Perceived by Nurses in Saudi Arabia: A Cross-Sectional Study
Somayah Mohsen Mohammed Al-Qarni1, Dalyal Al Osaimi1,2 and Hala Mohamed Mohamed Bayoumy2,3*
1 College of Nursing, King Saud University, Riyadh, KSA, Saudi Arabia
2 College of Nursing and Dentistry, Vision Colleges, Riyadh, KSA, Saudi Arabia
3 Nursing Department, College of Nursing, Cairo University, Cairo, Egypt, Saudi Arabia
Submission: June 11, 2023; Published: June 20, 2023
*Corresponding author: Hala Mohamed Mohamed Bayoumy, College of Nursing and Dentistry, Vision Colleges, Nursing Department, College of Nursing, Cairo University, Cairo, Egypt, Saudi Arabia. Email: hamr77@hotmail.com
How to cite this article: Somayah Mohsen Mohammed Al-Q, Dalyal Al O, Hala Mohamed Mohamed B. Quality of Postoperative Handover as Perceived 002 by Nurses in Saudi Arabia: A Cross-Sectional Study. Ann Rev Resear. 2023; 9(3): 555762. DOI: 10.19080/ARR.2023.08.555762
Abstract
Background: Handover is considered a basic nursing practice in which a patient's care information is moved to another nurse. Handover of patients after surgery is critical due to number of care transitions, presence of a surgical procedure, and the influence of anesthesia. High-quality postoperative handover is essential to safe patient care. Few studies have been conducted to evaluate the quality of current postoperative handover practices and the factors contributing to quality of such process, especially in Saudi Arabia.
Aim: The present research aimed at evaluating nurses' perceptions of postoperative handover quality and assessing factors impacting this process. Research Methodology: Design: A non-experimental, cross-sectional design was utilized. Sample: The target population were registered nurses with at least 1 year of professional experience with conduction of postoperative handovers across various hospital departments. A total sample of 143 nurses were selected via a convenient sampling technique. Study instruments included Handover Quality Rating Form, patient status, and nurses’ background characteristics tools.
Results: Overall, postoperative handover quality was perceived high by handing over and receiving nurses. Handover was conducted under acceptable circumstances. Ratings of receiving nurses were much higher than transferring nurses. Factors affecting postoperative handover quality included involved departments, nurses’ background characteristics (experience, age), and patients’ status factors.
Conclusion: Postoperative handover quality was highly perceived by nurses. Several nurse and patient related factors were found to impact the handover process. This current research may serve as a guide to developing strategies to improve postoperative handover practice.
Keywords: Postoperative; Handover; Quality; Nursing
Abbreviations: NICE:National Institute of Health and Care Excellence; WHO: World Health Organization; KKUH: King Khalid University Hospital; HQRF: Handover Quality Rating Form; SPSS: Statistical Package for Social Science; PACU: Post Anesthesia Care Unit; DSU: Day Surgery Unit; OR: Operating Room
Relevance to clinical practice
To improve nurses' competency in providing high quality handover services that minimize errors associated with patient’s transfer, factors related to nurses’ handover practices must be addressed. Gaining knowledge of the postoperative handover practices and its influencing factors is important for nursing administration and policymakers to continually plan and implement appropriate interventions.
What does this paper contribute to the wider global clinical community?
a) Understanding the perceptions of nurses concerning the quality of handover procedures and practices is paramount if nursing practice is to be enhanced.
b) Examining the influence of patient and nurse related factors on postoperative handover quality is essential for redirecting required improvements in future nursing handover practices as well as ensuring positive patient’s health outcomes.
Introduction
Nursing handover is a process of transferring patients among different hospital departments which requires comprehensive communication of the needed information to ensure the continuity of patients’ care [1]. According to the National Institute of Health and Care Excellence (NICE, 2018) [2] nursing handover is a system by which the responsibility of continued and urgent patient care is shared across various departments of the healthcare organization. The World Health Organization (WHO, 2020)[3], also identified nursing handover as the communication process by which information specific to the health of a patient are shared between a team of caregivers or between caregivers and patient or family members, to comply with standards of care continuity and safety practices. Such definitions not only demonstrate how common or essential is the practice of handover in the nursing profession but also demonstrate the importance of ensuring that a patient receives high-quality care [4]. A clinical handover that is comprehensive and safe is also essential for optimum patient care and prevention of clinical errors [5]. Caution has to be taken to ensure that there lies consistency and patient-centeredness in communicating the interventions, diagnostic needs and changing health status of the patients during their time of stay in the healthcare organization [6]. Such consistency is necessary to ensure that patient care is not compromised irrespective of changes in individuals and environments providing the needed care [7]. Differences in handover communication components can exist in the form of incorrect or incomplete information, wrong diagnosis, incomplete medical history or intolerance, lack of information on the history of care, limited or incorrect information on the surgical procedures, and diagnostic tests or medication administration factors (dosage, time, type) [8,9].
In fact, the practice of handover transfer and reception can further be prone to differences in quality standards pertaining to documentation of critical patient health status, treatment needs, and medical history variables [10]. Postoperative handover occurs between hospital surgical departments that involve nurses with different experiences, expectations, perceptions, and patients with different conditions. Additionally postoperative handover, being a complex process with multitasks such as vital signs monitoring and patient transferring, raises the chances of error.5 The loss of quality and ineffectiveness of clinical handovers were found to be the reason for the most significant adverse events, health care errors, and poor health outcomes among patients according to the reviewed root cause analyses and sentinel events [11-13,5]. In Saudi Arabia, out of 433 reported sentinel incidents between 2012 and 2015, 35% of them were due to failure in communication [14]. Identifying the potential risks associated with handover practices is likely to improve timely correction, resulting in improved handover and patient care quality [15,16,9]. Health care organizations should ensure that all handovers comply with a ‘minimum data set’ irrespective of departmental differences. The minimal amount of information required to provide patient needs, health status, and risks should be communicated sufficiently during interdepartmental transfer. Horwitz [17] have discovered five factors that govern the quality of a handover, including the acquaintance with the patient, the number of handovers to be conducted, a sense of duty and responsibility, the presence of a leader, and a documented handover sheet.17 Healthcare organizations thus have been advised to follow a standard structured format of handover communication while transferring patients from one department to another [18,2].
The structured and standardized handover should include all content and information necessary for the continuity of care to patients. Several studies therefore focused on the importance of using a standardized handover process after surgery and indicated the positive impact of such standardization [11,19]. NICE (2018)2 emphasized that following a structured handover tool or format is one of the most effective ways to prevent errors associated with the subjective nature of interpreting written or verbal handover information. Care transition processes primarily occur during the transference of handovers, primarily between practitioners possessing diverse skills, training, competencies, knowledge, expectations, and perspectives of care. These demonstrate the importance of communication and cooperation in enabling an effective handover process. According to the Joint Commission (2009) [20], problems in handover communication were responsible for about 70% of the reported sentinel events. Additionally, of all sentinel incidents which occurred during the transition of patient care in the hospital’s environment, 80% were due to poor communication among healthcare professionals [21,22]. Weinger et al. [23] postulated that effective communication processes are of utmost importance for maintaining patient safety.
However, there is evidence of many variations in the way nurses share, transfer and receive communication about postoperative patient handovers, resulting in various styles and tools used for the process [24]. A systematic review conducted by Smeulers, Lucas, and Vermeulen, identified several different handover styles. These comprised of: verbal handovers where nurses share patient information by reading out clinical notes of the patient, the combined practice of verbal communication as well as reading aloud and taking down clinical notes, or the practice of handover communication at the patient’s bedside to ensure patient participation during the same. Reine reported some of the key factors which were found to be associated with a poor quality of nursing handover. These included: uncertainty of clinical situation, high frequency of situations with time constraints, and pressures and the complexity of health problems experienced by the patients. Moreover, Mohammad [25] in his analysis of 80 nursing interactions conducted across seven diverse wards in two hospitals of Saudi Arabia, revealed that linguistic differences influenced nursing interactions during the handover process.
Several other barriers to effective handover processes were also communicated in the narrative literature review by Suganandam [26]. Such barriers include the resistance shown in response to changes such as the practice of standard tools for handover communication, limited time by nurses, limited resources to evaluate the existing quality of handover processes, inadequate levels of knowledge held by staff, bad ratio of staffing between patients and nurses, lack of leadership, the prevalence of cultural differences between nurses and an absence of technology used to share patient information between one department to another. Several factors therefore can cause transferring a weak or incomprehensive handover between departments. Hence, nurses need to be aware of the various factors affecting handover quality and take appropriate actions to improve the process [27].
To sum up, differences in the quality of a handover are thus likely to raise the risk of clinical errors, especially in a postoperative patient who is characterized by the vulnerability to develop complications due to the surgical procedure and the effect of the anaesthesia and the multiple transitions between hospital departments [11]. Thus, it is important to understand the perceptions held by nurses concerning the quality of handover procedures and practices to identify the areas that can be further enhanced for future nursing practice. However, according to the best of the researchers’ knowledge, no studies were previously conducted to assess the quality of the postoperative handover nursing practice in Saudi Arabia. Hence, in this respect, the present study was undertaken to evaluate the postoperative patient handover quality among both the transferring and receiving nurses. Likewise, there was a shortage of existing literature exploring the impact of nurses’ socio-demographic characteristics in yielding differences underlying perceptions of handover quality in hospitals. Thus, to address these limitations, not only this research explored a multitude of factors such as patient health status and nurses’ socio-demographic variables in nurses’ perceptual differences for handover quality, but this research also provided findings that could direct future improvements in nursing handover practice to ensure high-quality patient care as well as positive health outcomes across the population residing in Saudi Arabia.
Research Aim
The present research aimed at assessing perceptions of the quality of postoperative handover practice among receiving and transferring nurses in a Tertiary Hospital in Saudi Arabia. Moreover, factors impacting the handover quality were investigated, including: involved departments, nurses’ demographic and background variables, and finally patient status.
Material and Methods
Research Design
A quantitative cross-sectional, descriptive, and non-experimental research design was carried out. Since this research aimed to understand how consideration of factors like nurses’ role, the status of patients, and nurses’ background variables influence perceptions concerning the quality of the nursing handover, a cross-sectional descriptive form of research was the most appropriate. Furthermore, a descriptive form of research was primarily conducted to obtain in-depth knowledge and understanding concerning an issue or phenomenon [28].
Research Setting and Population
The research was carried out at King Khalid University Hospital (KKUH), being one of the largest tertiary healthcare organization situated in Riyadh, Saudi Arabia, with a capacity of 850 beds. The population frame based on which sample of the present research drawn was the registered nurses who are handing over or receiving postoperative patients between surgical departments of the selected hospital. Therefore, the total population for the present study was 281 registered nurses. A convenience sampling strategy was implemented. An overall sample size of 143 registered nurses was calculated using the sample calculator of Raosoft with a 95% confidence level and 5% margin of error. The researchers ensured that the sample met the following inclusion criteria: registered nurses with at least 1 year of professional experience, and being employed in departments including the Operating Room, Post Anesthesia Care Unit, Surgical Intensive Care Unit, Day Surgery Unit or Surgical Inpatient Wards. Exclusion criteria were nurses who were receiving or transferring postoperative pediatric, neonate or maternity patients. As data collection was carried out during COVID 19 pandemic and there was absolutely limited access specially to those wards that contained the high risk group of patients and the staff working there.
Data Collection Instruments
Self-reported questionnaire comprised of three sections was utilized for data collection. The first section included questions related to the patient’s age and medical status with respect to the following variables: blood circulation and respiration (impaired, medium, good), level of patient’s consciousness (unconscious, semiconscious, awake), feelings or experiences of the patient concerning wellness or nausea (no or yes), pain perceptions in patients (strong pain, moderate, slight, no pain), surgical procedures used, anesthetic techniques. Additionally, information was collected concerning physical status classification of the patient as per the American Society of Anesthesiology. The second section contained information regarding the nurse participants’ background characteristics including: the total years of professional experience in practicing nursing, nurse’s age, professional experience in the concerned department, educational level, and current nursing role. This section of the questionnaire further involved collecting data pertaining to handover areas and nurses' role (whether being transferring nurse or receiving nurse). The last section of the questionnaire involved the Handover Quality Rating Form (HQRF), formulated by Manser [29]. The HQRF included 21 items focused on evaluating the overall handover quality. These items were divided into four dimensions that included circumstances of handover (4 items), the conduct of handover (8 items), teamwork (4 items), and handover quality (5 items). Individual items for each dimension can be found in results section (Table 1-4). Each item was rated on a four-point rating scale ranging from agreeing (4), partially agreeing (3), partially disagreeing (2), and disagreeing (1). For each dimension, a mean score was calculated using its related sub-items scores. This mean score was further utilized to calculate percentage agreement/disagreement for that construct using the four-point rating reference.
Pilot Study
It is worth denoting that the Handover Quality Rating Form (HQRF) was developed and validated by Manser [29], from whom the researchers had obtained permission via mail. A pilot study was carried out, using 20 registered nurses, to verify the validity and reliability of this instrument and to identify necessary modifications. The pilot study sample was excluded from the main study. The validity was evaluated using Pearson's Correlation Coefficient. The statistical analysis indicated a statistically significant correlation at the level of α = 0.05 between the scores of each item and the total score of the dimension to which it belongs. Circumstances of the handover item correlations ranged between 0.769 to 0.851, item correlation for conduct of the handover ranged between 0.520 to 0.735 and item correlation for teamwork range was 0.598 to 0.866 and finally the item correlation for handover quality was between 0.467 and 0.783. Moreover, to verify the reliability of the Handover Quality Rating Form (HQRF), the Cronbach's alpha was calculated. The values of stability on the dimensions of the tool showed scores ranged between 0.702 to 0.814, which indicated a high degree of stability.
Data Collection Process
The researchers ensured that the design and methods are ethically compliant and respectful of the recruited participants' dignity, expectations, safety, and possibility of risk. Ethical approval was obtained from the Institutional Review Board of King Saud University, a notable ethics community of the university, as well as ethical approval was provided by King Khalid University Hospital from where participants for the study were recruited) [30,31]. To ensure that this research is respectful of the autonomy of the participants, the researchers ensured that informed consents were obtained and that participants were informed that their recruitments were voluntary and free of coercion [32]. The researcher ensured that each participant was well informed concerning the present research purpose and procedures. Furthermore, participants were assured that they have the freedom to withdraw from the study and that participation will not cause any risk or harms to their health care whatsoever [33]. All nurses that met the inclusion criteria were invited to participate in the study. Upon securing the necessary approval for participation, eligible participants were requested to complete the handover quality questionnaire. Data collection was carried out between February 2021 and March 2021 using electronic devices (iPad) due to the COVID 19 precautions. To maintain privacy and confidentiality, participants’ sociodemographic characteristics and patient’s status information were kept anonymous without any identification as well as data were secured in a safe database with a password and limited access to only researchers and authorized stakeholders from IRB [34].
Data Analysis
This study utilized the IBM Statistical Package for Social Science (SPSS) version 23.0 for statistically analyzing the collected data. To assess for statistically significant differences in the perception of postoperative handover quality regarding patient and socio-demographic variables and between receiving and transferring nurses, Chi-square, goodness of fit test, Independent Sample T-test and One-way ANOVA test were conducted. Posthoc analyses were carried out using Bonferroni test for analyses that had omnibus (i.e., initial ANOVA) significant differences. In this study, the significant level (P-value) was set at < 0.05.
Results
Demographic Profile of Study Subjects
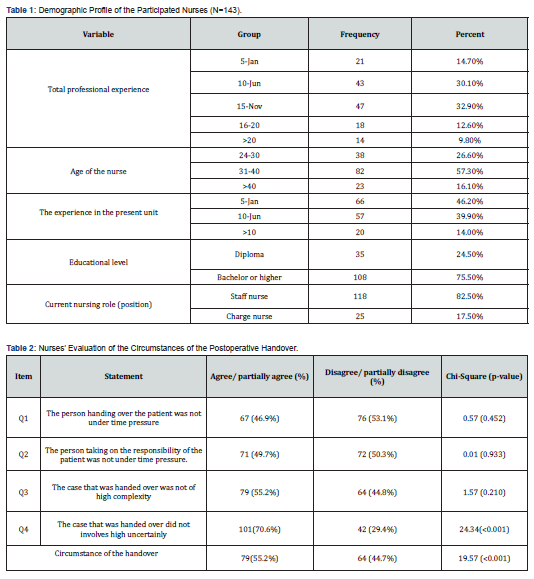
A total of 143 nurses voluntarily representing 87.7% of the total sample, participated in the present study. From Table 5, most respondents (63%, n= 90) had six to fifteen years of nursing experience. Majority of the respondents (57.3%; n=82) had an age range between 21-40 years. The majority of respondents (75.5%, n=108) had a bachelor or higher degree, while 35 nurses (24.5%) had a diploma. More than half of the nurse participants (82.5%, n=118) were staff nurses, and (17.5%, n=25) were charge nurses. Eighty-four percent of the conducted surgical procedures were elective, while only 16% were done as emergency surgery. 64.34% of the patients were younger than fifty years old, while 35.66% were older than fifty years old. Furthermore, 47.79% of the procedures were general surgeries, and 24.26% were Orthopedic surgeries.
Overall postoperative nursing handover practice quality
Table 2 shows the responses of nurses on each statement related to the circumstances of the handover. The majority of the respondents (101, 70.6%) agreed that the case handed over did not involve high uncertainty versus (42, 29.4%) who agreed (Chi-Square = 24.34, p˂0.001). The rest of the items did not show any significant statistical differences. Generally, 55.2% of nurses agree on the different items supporting the positive circumstance for handover, while 44.7% disagree on the circumstance of handover (p˂0.001), indicating that the circumstances of postoperative handover were satisfactory and almost perceived well. Table 3 illustrates the response of participants to the conduct of handover. More than three-quarters of nurses agreed with the 8 items as shown. In short, the results reflected satisfactory performance of postoperative handover. There was 92.3% agreement on all statements compared to only 7.69% disagreement (Chi-Square=99.807, p˂0.001).
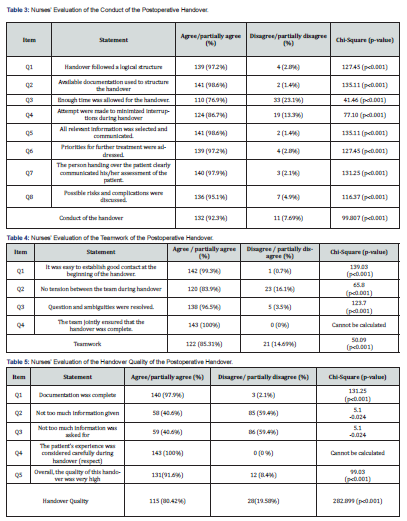
Majority of nurses agreed that handover followed a logical sequence (Q1:139, 97.2%), the person handing over continuously used the available documentation (Q2:141, 98.6%), attempts were made to minimize the interruptions during handover (Q4:124,86.7%), all relevant information were communicated (Q5:141, 98.6%), priorities for further treatment were addressed (Q6;139,97.2%), the patient assessment data were properly communicated (Q6;140,97.9%), and that possible risks and complications were discussed (Q8;136,95.1%). Table 4 displays the four assessment items related to teamwork during postoperative handover. Almost all participating nurses agreed on items (Q1 and Q4). Only one respondent (0.7%) disagreed about easiness to establish satisfactory contact at the beginning of the handover. The majority of nurses (n=120, 83.9%) agreed that there was no tension between the teams during the handover, and one hundred thirty-eight respondents (96.5%) agreed that questions and ambiguities were resolved. Significant statistical differences were observed between agreement and disagreement on items (Q1, Q2, and Q3) as well as on teamwork as a whole (p˂0.001).
Table 5 shows the five indicators for overall Handover Quality. Significant statistical differences were observed between agreement and disagreement on four items (Q1, Q2, Q3, and Q5) as well as on the handover quality as a whole (P<0.001). Regarding documentation, 97.9% of respondents reported agreement that the documentation was complete. More than half of the experienced nurses (59.4%) agreed that too much information was given and asked for during handover (i.e., they disagreed with the statements in Q2 and Q3). Interestingly, one hundred thirty-one (115) respondents, representing 80.42% of the total sample, rated the postoperative handover as of high quality. In summary, the postoperative handover was conducted well under ideal circumstances, with satisfactory teamwork and high rated quality.
Nurses’ perception of postoperative handover quality based on involved departments:
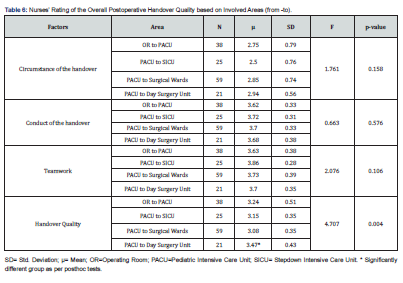
For testing groups differences, mean score for each item was calculated using the nurse participants’ ratings. Moreover, Handover Quality Rating Form (HQRF) dimensions mean score were calculated by summing up the sub-items means scores and dividing the resultant by number of items under each dimension. These two calculated scores were utilized in carrying out the comparison of means using the t-test and the ANOVA tests. ANOVA Test was used to determine the differences in nurses’ perception of the postoperative handover quality as per postoperative involved departments. Results in Table 6 revealed no significant statistical difference in the agreement on the circumstance of handover (p>0.05), the conduct of handover (p=0.576) or teamwork (p=0.106) based on the involved postoperative handover departments. Data however showed a significant statistical difference (p=0.004) concerning the handover quality according to the involved postoperative handover departments (from-to). Posthoc analyses were therefore carried out using Bonferroni test. PACU to Day surgery unit handover showed highly significant statistical handover quality mean difference compared to the rest of the unit’s transfer. The rest of the ward’s handover process had similar perception for the quality of handover (Table 6).
Nurses’ perception regarding the quality of postoperative nurse to nurse handover practice based on selected demographic variables
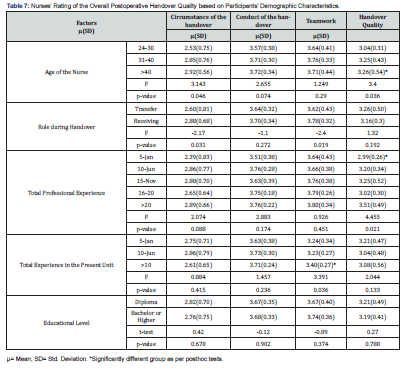
As shown in Table 7, there was a significant statistical difference for the agreement on the handover quality as well as (p=0.036) circumstance of postoperative handover (p=0.046) based on respondents’ age. Nurses’ perception of conduct and teamwork of postoperative handover did not differ based on age group. Moreover, significant statistical differences were found for the circumstance of handover (p=0.031); as well as teamwork (p=0.019) between the receiving and handing respondents; nurses’ receiving ratings were higher than the ratings of handing nurses. Concerning total professional experience, a significant statistical difference was observed in the handover quality items based on the respondents' experience. Finally, ratings for circumstances, conduct, teamwork, and handover quality did not differ based on respondents’ educational level or current nursing role. Posthoc analyses were therefore carried out using Bonferroni test for analyses that had omnibus (i.e., initial ANOVA) significant differences. As shown, nurses above 40 years of age had the highest rating for circumstances as well as handover quality compared to the rest of the other age groups. People who have five years of professional experience or less rated their quality of handover practice the less compared to other groups. Finally, nurse who had more than ten years of unit experience had highest team work ratings.
Nurses’ perception regarding the quality of postoperative nurse to nurse handover practice based on patient status
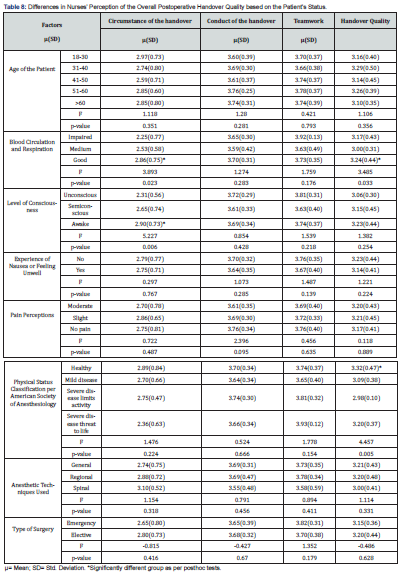
As shown in Table 8, ANOVA Test revealed no significant statistical differences in the nurses’ perception of the overall postoperative handover quality (p>0.05) as per patients’ age group. Concerning patient’s blood circulation and respiration, the perception of the circumstance of postoperative handover and handover quality was significantly different according to patients’ circulation and respiratory status (p=0.023, p=0.033; respectively). Furthermore, there was a significant statistical difference (p=0.006) in the agreement of the postoperative handover circumstances based on the patient’s level of consciousness. Neither patient’s experience of nausea or feeling unwell; feeling pain; anesthetic techniques used; nor the type of surgery affected nurses’ perception of the overall postoperative handover quality (p>0.05). Regarding patients’ physical status classification, only handover quality significantly differed (p=0.005) based on the physical status classification of the patients as per the American Society of Anesthesiology. Posthoc analyses, further revealed that nurses’ perception for circumstances as well as handover quality were the best where patient blood circulation and respiration were classified as satisfactory. patients who were awake as per level of consciousness assessment perceived handover circumstances higher than when patient had impaired consciousness. Finally, health rating for patient physical classification as healthy affected nurses high rating for quality of the handover compared to the rest of categories of physical states.
Discussion
The purpose of this research is to assess the quality of postoperative handover practice among nurses; specifically, circumstances, teamwork, conduct of handover as well as their overall perceived quality. Overall, the results of the present study, as compared to previous similar research, have emphasized the significant role of effective handover practices in the nursing profession. The study found a significant agreement regarding the circumstances of postoperative handover which were well perceived by both the receiving and the transferring nurses. This finding is in line with previous findings by Mamalelala . It is essential to recognize that the overall nurses’ perception of the circumstances of the postoperative handover could significantly contribute to handover quality. The study showed that factors associated with poor perception of postoperative handover circumstances included time pressure and complexity of patient’s health. Reine stated that time strain during postoperative handover is considered a threat to the handover quality. On the same vein, Schramm’s circular model of communication emphasized that the communication process is influenced by environmental factors such as workload, which causes time pressure [35]. Similarly, the important role of having enough time for a quality handover was reported by the majority of nurses as being one of the most important criteria for evaluating the conduct of the handover process. This result ties nicely with previous studies wherein 88% of nurses agreed on the need for securing enough time to ensure that a satisfactory handover was provided.
The present study further revealed that the conduct of postoperative handover was perceived well among majority of study participants. Logical sequencing of the postoperative handover in addition to the vital role of available documentation in structuring the handover were significantly agreed upon by nurses. The importance of utilizing structured and logical handover process has also been emphasized in the literature not only for the quality of such a process but also for patient’s safety. Leonardsen [36] & Rikos [37] stated that implementing a structured tool of communication that is based on a logical workable process with some standard interdepartmental communication mechanisms is significant for improving the safety and quality of handover and ensuring the consistency and continuity of patient care. Nurses further emphasized the important role of minimizing interruptions during the handover process as a mean of improving the quality. Murray [38] stated that among the key barriers that could hinder the handover transition process by nurses is the prevalence of interruptions in the environment during the transition of patient care process. The present study further confirmed that the high-quality communication and discussion between the involved nurses in the postoperative handover must accurately include: all critical information of the patient condition, patient’s assessment, any suspected risk or complications and possible further treatment or interventions. A similar pattern of results was obtained in studies conducted by Manser [29] & Manser [39]. Additionally, Jones [13] emphasized that transferring practitioner must communicate the essential factors about the patient condition and ongoing treatment interventions to the healthcare worker receiving the same [40,41].
Concerning teamwork, the majority of study participants positively perceived team process and the members involved in the postoperative handover. Thomson [42] contended that excellent teamwork between receiving and handing over nurses could enhance participants’ perception of handover quality. Almost all participating nurses had agreed on both the easiness of establishing satisfactory contact at the beginning of the handover and the completion of the handover jointly by all team members. In accordance with the present results, a previous study conducted by Streeter [40] demonstrated that interaction between transferring and receiving nurses during handover should ensure a satisfactory contact to exchange information, ask and answer questions, and achieve optimal communication. Additionally, participating nurses agreed upon the vitality of having no tension between the teams, and having questions and ambiguities adequately resolved. These results are in line with those of a previous study by Kerr [41] & Nagpal [11], stated that achieving teamwork during handover correlated with decreasing the missed information and lowering the chance of error which consequently could led to high-quality handover. Furthermore, the study evaluated postoperative handover quality; the fourth construct of the Handover Quality Rating Form (HQRF), which focus on documentation [43], shared information, patient’s experience, and self-rating of the handover quality. Percentage of nurses who agreed on the high quality perception for the handover was high. Similarly, overall handover quality, as measured using nurses’ general satisfaction item on the said construct, showed consistent results among 91.6% of respondents. Additionally, this was similarly shown by both handing over and receiving nurses. Similar results were reported by Reine et al. (2019)5. While, satisfaction rate reported in Nepal by Koirala [44] were lower than the present study. Koirala [44] reported that only 50.9% of nurses were satisfied with their current handover quality.
Study results further revealed that complete documentation as well as careful consideration of patient’s experience showed highest agreement for handover quality among study participants. This was consistent with the findings of Manser [39] & Reine [5]. Manser [39] reported that 92% of the participating nurses agreed on necessity to respect patient’s experience during handover. Moreover, according to Manser [39] and Segall [43] complete and precise patient’s documents are very important to give clear picture about the patient to receiving team which ensure continuity of care and patient’s safety. On line with that, the results of this study also indicated that more than half of the participated nurses agreed that not too much information was given and asked for during the handover. In fact, providing the most relevant and important patient’s information is very detrimental in facilitating the communication process. A high-quality handover should therefore be characterized by the exchange and share of information between two parties in which they are able to ask and answer the questions needed for securing continuity of quality patient care. [40] Such results support the idea that a focused handover that eliminates irrelevant and unnecessary information is more likely to result in best patient care. The study further explored the differences in perceptions of practice quality based on involved departments, nurses’ handover role, nurse participant’s demographics and patients’ status variables. Nurses’ perception of handover quality revealed a statistically significant difference based on the departments involved, specifically the self-rating of handover quality. This result is in line with the study conducted by Koirala [44] who showed that nursing perception of handover quality depended significantly upon the type of nursing unit. Similarly, reported that the difference in the nature of nurses’ clinical practice throughout hospital areas is playing an important role in the variation of nursing perceptions of handover quality. The study further showed that nurses conducting handover between Post Anesthesia Care Unit (PACU) and Day Surgery Unit were more likely to agree with the handover quality item than other postoperative handover areas. A possible explanation for this might be the difference in duty hours, workload, patients’ census, duration of hospital stays and severity of conditions between Day Surgery Unit (DSU) and other surgical departments.
Transferring and Receiving Nurses’ Assessment of the Postoperative Handover Practice
Concerning nurses’ handover role, the study revealed a significant difference between the receiving and the handing over nurses' rating of the postoperative circumstances as well as postoperative team work perception. The ratings of receiving nurses for the postoperative handover were higher than the transferring nurses. In the current study, the transferring nurses are either Operating Room (OR) staff or Post Anesthesia Care Unit (PACU) staff. Hence, the current study's findings do not support previous studies in which the transferring team were more satisfied with the postoperative handover than those who were receiving the patient's responsibility [5,19].
The reason behind transferring nurses’ lower perception of the postoperative circumstances and teamwork is that they do handover different cases with various surgical procedures to different hospital departments which might make it difficult for them to figure out the different expectations of the receiving staff that have various backgrounds and views as well. Furthermore, Petrovic [19] cited that the PACU accepts different conditions and communicates to transfer their responsibilities to more than one department in the hospital which might be responsible for their flexibility, predetermined expectations and consequently easily achieved satisfaction compared to the transferring nurses. On the other hand, nurses’ handover role revealed no significant effect on perception of handover conduct or the quality. These findings could be attributed to the fact that King Khaled University Hospital is implementing a standardized handover process which control nurses’ practice roles variations. Mohammad [25] reported that utilizing standardized handover tools is a way to overcome the difference in quality perception between nurses. A standard handover process makes it easy for nurses to conduct the handover consistently and have similar views of the handover quality [45-47,38].
Quality of Postoperative Handover Practice Based on Selected Demographic Variables
The present study findings revealed that nurses' total professional experience, total experience in the present unit, and nurses’ age effect the overall handover quality assessment. This was inconsistent with Koirala [44] & Nagammal [24]. Furthermore, the study results indicated that the total years of nursing experience did not affect the perception of nurses' postoperative handover circumstances or their teamwork. This finding contradicts the findings of Reine [5]. Moreover, Redley [48] reported that the ability of nurses to manage and deal with teamwork and relationships during postoperative handover is correlated with their length of experience. Moreover, the current study found, however not statistically significant, nurses with six to ten as well as those having sixteen to twenty or more years of nursing experience had a better perception of handover conduct compared to those with five years or less of nursing experience. In fact, more experienced nurses are better familiar with the handover process between different hospital units than inexperienced nurses who might miss some of the important information during handover due to their unfamiliarity.
Additionally, the nurses’ total professional experience enhanced their perception of the quality of postoperative handover, including evaluation of documentation, shared information, patient’s experience, and self- rating of the handover quality. Nurses with professional experience of more than twenty years reported the highest quality of postoperative handover. This result may be explained in light of the cumulative experiences and information gained by expert nurses in addition to their critical thinking skills which are used in widening their knowledge about patients, through asking and answering questions during handover. This explanation is supported by Mcfetridge [49] study who found that junior nurses were not asking any questions during handover because they did not recognize that there was missing information.
In line with previous results, the study showed that as the nurses' experience in the assigned unit increased, the perception of the self-rating of handover teamwork increased. Consistent with the present study findings, Schramm's Circular Model of communication emphasized that during the postoperative handover communication, the transfer, receipt and understanding of the information are affected by the common field of experience, which includes the experience duration in the specialty unit of nurses [35]. Hilligoss & Cohen [50] stated in their study that nurses have an excellent chance to learn from each handover process they are involved in and that the experience is the best source to get lessons about the handover process. Concerning participants’ age, nurses older than forty years old had higher perception for postoperative handover circumstances compared to younger nurses. In the same vein, the study found that as nurses’ age increases, the perception of quality of postoperative handover increases through the evaluation of documentation, shared information, patient’s experience, and the self-rating of handover quality. This finding, however, is contrary to previous studies [42,24,44].
Quality of Postoperative Handover Practice Based on Patients’ Status Variables
The present study revealed three characteristics related to the patients’ condition that had significant impact on nurses’ assessment of the overall handover quality including: patient’s blood circulation and respiration, level of consciousness, and physical status classification as per the American Society of Anesthesiology. This finding is supported by Reine [5] & Streeter [40] who showed that patient’s status affects the postoperative handover quality and that nurses must therefore recognize and understand the patients’ needs and conditions. A significant difference was obtained in postoperative handover circumstance items as well as handover quality based on patient’s blood circulation and respiration (good, medium, impaired). The study showed that nurses tend to agree with the handover circumstances and the quality construct when patient has good blood circulation and respiration than when patient had medium or impaired status. These results might be attributed to the fact that the impaired circulation and respiration reflect the high complexity of the case which do take the greatest focus and highest attention from the nurses during the handover process. Nurses also tend to work under pressure and stress when handing over patients with impaired circulation and/or respiration. Reine [5] emphasized the significant effect of the patient’s condition on the quality of the handover process and revealed that handing over or receiving patients with complex problems is correlated with lower handover quality. Concerning the patient’s level of consciousness, a significant difference in the agreement of circumstance items was found. It was illustrated that nurses who received or transferred awake postoperative patients tend to agree on the handover circumstance items as they relate to quality handover than those who received or transferred unconscious patients.
In fact, patients with impaired consciousness require the highest concern from nurses as well as priority monitoring to prevent patient’s harm by themselves removing tubes, their unwanted movement, or deficient handover information. Patients’ safety upon handover process is considered a high priority for nurses and earlier studies therefore emphasized on the adaptation of handover process based on the current patient’s status and handover circumstances to ensure quality and safe care [5,51,52]. Finally, physical status classification of the patient as per the American Society of Anesthesiology significantly influenced the agreement on handover quality construct. According to Manser [39] information about a patient’s medical history and chronic illness is significant for an obvious picture of the patient. This study revealed that postoperative nurses who received or transferred healthy postoperative patients were more likely to agree on the handover quality items than those who received or transferred patients with mild systematic disease and severe systematic disease that limits normal activity. This finding is consistent with previous studies, which showed that the handover process tends to be effective and easy if the patient was in good health.
Conclusion
The purpose of this research was to investigate the nurses' perception of the overall postoperative handover quality based on the nurses’ handover role; handover involved departments, selected participant's demographic variables and patients' status. This study revealed high postoperative handover quality as perceived by handing over and receiving nurses. The postoperative handover was conducted well under satisfactory and acceptable circumstances, with ideal teamwork and high rated quality. The participated nurses were satisfied with the current postoperative handover practice. Involved departments (from-to) impact the nurses' perception of the overall postoperative handover quality through their assessment of the handover quality items. This study found three nurses' characteristics that impact their overall handover quality assessment: total professional experience, total experience in the present study and nurses’ age. Additionally, there were three characteristics related to the patient's condition impact the nurses’ assessment of the overall handover quality, which were; patient's blood circulation and respiration, the patient's level of consciousness, and the physical status classification of the patient as per the American Society of Anesthesiology. This study strongly emphasized the need to understand nurses' perceptions and satisfaction about the current postoperative handover practice by leaders and policymakers in the healthcare system.
Recommendations
Based on the study findings, the researchers recommended that nursing administration and policymakers have to continually evaluate the postoperative handover practice and understand the factors affecting the quality of the postoperative handover to decide and implement the appropriate interventions. It is also recommended to develop guidelines for postoperative handover to benefit from implementing the standardized handover process and the structured handover tool and enhancing nurses’ compliance. Planning and implementing postoperative handover training programs and workshops to enhance nurses’ communication and teamwork skills is necessary. Nurses should be attentive to the factors that could impact the quality of the postoperative handover to decide how to deal with them. Workload and time pressure were found to contribute to poor postoperative handover quality. Thus, nurses should incorporate time and workload management strategies into their practice. Although the postoperative handover quality is perceived high, repeating the study using qualitative research design, observation, and video or audio records with a large sample will be needed to gain in-depth data about postoperative handover quality and find other possible affecting variables. Replication of the current study in other institutions, hospitals, and regions of Saudi Arabia to get a wide perspective about the postoperative handover and enhance the study findings generalization. Finally, future studies are needed to investigate and bring out the relationship between postoperative handover quality and patient outcome.
Limitations
The present study has the following limitations. They first conducted this study in only one tertiary hospital in Riyadh due to the COVID-19 crisis and strict precautions. This is in turn, limits the generalization of the current study findings. Secondly, although the participating nurses provided the survey questionnaire after they have completed the handover process. However, assessing a process in which nurses are active stakeholders and using the self-report questionnaire may not represent the reality of postoperative handover practice. Finally, using a sample size which considers relatively small and using convenience sampling limits the generalization of the findings.
References
- Mamalelala TT (2017) Quality of handover assessment by registered nurses on transfer of patients from emergency departments to intensive care units. Doctoral dissertation. University of the Witwatersrand. Electronic Theses and Dissertations.
- Structured patient handovers
- Communication during Patient Hand-Overs. Who.int.
- Beuken JA, Verstegen DM, Dolmans DH, Van Kersbergen L, Losfeld X, et al. (2020) Going the extra mile-cross-border patient handover in a European border region: Qualitative study of healthcare professionals’ perspectives. BMJ Quality & Safety.
- Reine E, Ræder J, Manser T, Småstuen MC, Rustoen T (2019) Quality in postoperative patient handover: different perceptions of quality between transferring and receiving nurses. J Nurs Care Qual 34(1): E1-E7.
- Randmaa M, Engström M, Swenne CL, Mårtensson G (2017) The postoperative handover: a focus group interview study with nurse anesthetists, anesthesiologists and PACU nurses. BMJ open 7(8): e015038.
- Vander WI, Poot EP, Nanayakkara PWB, Loer SA, Wagner C (2019) Handover Structure and Quality in the Acute Medical Assessment Unit: A Prospective Observational Study. J Patient Saf 15(3): 224-229.
- Puzio TJ, Murphy PB, Virtanen P, Harvin JA, Hartwell JL (2020) Handover Practices in Trauma and Acute Care Surgery: A Multicenter Survey Study. J Surg Res 254: 191-196.
- Smeulers M, Lucas C, Vermeulen H (2014) Effectiveness of different nursing handover styles for ensuring continuity of information in hospitalized patients. Cochrane Database Syst Rev 2014(6): CD009979.
- Yegane SAF, Shahrami A, Hatamabadi HR, Hosseini-Zijoud SM (2017) Clinical Information Transfer between EMS Staff and Emergency Medicine Assistants during Handover of Trauma Patients. Prehosp Disaster Med 32(5): 541-547.
- Nagpal K, Abboudi M, Manchanda C, Vats A, Sevdalis N (2013) Improving postoperative handover: a prospective observational study. Am J Surg 206(4): 494-501.
- Singh H, Thomas EJ, Petersen LA, Studdert DM (2007) Medical errors involving trainees: a study of closed malpractice claims from 5 insurers. Arch Intern Med 167(19): 2030-2036.
- Jones PM, Cherry RA, Allen BN (2018) Association Between Handover of Anesthesia Care and Adverse Postoperative Outcomes Among Patients Undergoing Major Surgery. JAMA 319(2): 143-153.
- Al Wahabi S, Farahat F, Bahlou AY (2017) Prevalence and preventability of sentinel events in Saudi Arabia: analysis of reports from 2012 to 2015. East Mediterr Health J 23(7): 492-492.
- Spooner AJ, Aitken LM, Corley A, Chaboyer W (2018) Developing a minimum dataset for nursing team leader handover in the intensive care unit: A focus group study. Aust Crit Care 31(1): 47-52.
- Kitney P, Tam R, Bennett P, Buttigieg D, Bramley D (2016) Handover between anaesthetists and post-anaesthetic care unit nursing staff using ISBAR principles: A quality improvement study. ACORN: The Journal of Perioperative Nursing in Australia 29(1): 30-35.
- Horwitz LI, Dombroski J, Murphy TE, Farnan JM, Johnson JK (2013) Validation of a handoff assessment tool: the Handoff CEX. J Clin Nurs 22(9-10): 1477-1486.
- Clarke S, Clark-Burg K, Pavlos E (2018) Clinical handover of immediate post-operative patients: A literature review. Journal of Perioperative Nursing 31(2): 29-35.
- Petrovic MA, Aboumatar H, Scholl AT, Gill RS, Krenzischek DA (2015) The perioperative handoff protocol: evaluating impacts on handoff defects and provider satisfaction in adult perianesthesia care units. J Clin Anesth 27(2): 111-119.
- Joint Commission (2009) Sentinel event statistics
- (2012a) Joint Commission Center for Transforming Healthcare releases targeted solutions tool for hand-off communications. Joint Commission Perspectives 32(8): 1-3.
- Joint Commission. Transition of care: The need for a more effective approach to continuing patient care.
- Weinger MB, Slagle JM, Kuntz AH (2015) A Multimodal Intervention Improves Postanesthesia Care Unit Handovers. Anesth Analg 121(4): 957-971.
- Nagammal S, Nashwan AJ, Nair SL, Susmitha A (2016) Nurses perceptions regarding using the SBAR tool for handoff communication in a tertiary cancer center in Qatar. J Nurs Educ Pract 7(4): 103-110.
- Mohammad A (2017) A Discourse Analysis of Nursing Handoffs: Exploring Nurse-to-nurse Interactions in Two Hospitals in Saudi Arabia. [Doctoral thesis]. South Florida, USA. University of South Florida.
- Suganandam DK (2018) Handoff communication: Hallmark of nurses. Indian Journal of Continuing Nursing Education 19(1): 12-20.
- Seada AM, Bayoumy SA (2017) Effectiveness of handoff educational program on nurses’ interns’ knowledge, and communication competence. American Journal of Nursing Science 6(6): 467.
- Park J, Park M (2016) Qualitative versus quantitative research methods: Discovery or justification? Journal of Marketing Thought 3(1): 1-7.
- Manser T, Foster S, Gisin S, Jaeckel D, Ummenhofer W (2010) Assessing the quality of patient handoffs at care transitions. Qual Saf Health Care 19(6): e44.
- Asman O, Melnikov S, Barnoy S, Tabak N (2019) Experiences, behaviors, and perceptions of registered nurses regarding research ethics and misconduct. Nurs Ethics 26(3): 859-869.
- Petillion W, Melrose S, Moore SL, Nuttgens S (2017) Graduate students experiences with research ethics in conducting health research. Research Ethics 13(3-4): 139-154.
- Miracle VA (2016) The Belmont Report: The Triple Crown of Research Ethics. Dimens Crit Care Nurs 35(4): 223-228.
- Sellman D (2016) The practice of nursing research: getting ready for ethics and the matter of character. Nurs Inq 23(1): 24-31.
- Obeidat RF, Al-Delaimy W (2020) Applying the ethical principle of social benefits in nursing research in developing countries: The case of Jordan. Journal of Academic Ethics 20: 39-50.
- Arnold EC, Boggs KU (2019) Interpersonal Relationships E-Book: Professional Communication Skills for Nurses. Elsevier Health Sciences.
- Leonardsen AC, Moen EK, Karlsøen G, Hovland T (2019) A quantitative study on personnels experiences with patient handovers between the operating room and the postoperative anesthesia care unit before and after the implementation of a structured communication tool. Nursing Reports 9(1).
- Rikos N, Linardakis M, Merkouris A, Rovithis M, Philalithis A (2019) Exploration of the experiences, opinions and attitudes of nurses on inter-shift handover procedures. Archives of Hellenic Medicine/Arheia Ellenikes Iatrikes 36(4).
- Murray JS, McGrath J, Smith MF (2013) Understanding the clinical handoff perspective of pediatric emergency nurses. Pediatr Nurs 39(5): 243-248.
- Manser T, Foster S, Flin R, Patey R (2013) Team communication during patient handover from the operating room: more than facts and figures. Hum Factors 55(1): 138-156.
- Streeter AR, Harrington NG, Lane DR (2015) Communication behaviors associated with the competent nursing handoff. Journal of Applied Communication Research 43(3): 294-314.
- Kerr MP (2002) A qualitative study of shift handover practice and function from a socio-technical perspective. J Adv Nurs. 37(2): 125-134.
- Thomson H, Tourangeau A, Jeffs L, Puts M (2018) Factors affecting quality of nurse shift handover in the emergency department. J Adv Nurs 74(4): 876-886.
- Segall N, Bonifacio AS, Schroeder RA (2012) Can we make postoperative patient handovers safer? A systematic review of the literature. Anesth Analg 115(1): 102-115.
- Koirala S, Mehta RK, Acharya S, Gauro P (2019) Critical Care Nurses' Views on Handover in Chitwan, Nepal. CONNECT: The World of Critical Care Nursing 13(1): 36-45.
- Randmaa M, Mårtensson G, Swenne CL, Engström M (2016) An observational study of postoperative handover in anesthetic clinics; the content of verbal information and factors influencing receiver memory. J Perianesth Nurs 30(2): 105-115.
- Naour MG (2018) Transition of care: The evaluation of hand-off communication between emergency department and Medical/Surgical nursing units. Doctoral dissertation. ProQuest Dissertations & Theses Global.
- Kilic SP, Nimet Ovayolu RN, Ozlem Ovayolu RN, Ozturk MH (2017) The approaches and attitudes of nurses on clinical handover. International Journal of Caring Sciences 10(1): 136-145.
- Redley B, Bucknall TK, Evans S, Botti M (2016) Inter-professional clinical handover in post-anaesthetic care units: tools to improve quality and safety. International Journal for Quality in Health Care 28(5): 573-579.
- McFetridge B, Gillespie M, Goode D, Melby V (2007) An exploration of the handover process of critically ill patients between nursing staff from the emergency department and the intensive care unit. Nurs Crit Care 12(6): 261-269.
- Hilligoss B, Cohen MD (2011) Hospital handoffs as multifunctional situated routines: implications for researchers and administrators. Adv Health Care Manag 11: 91-132.
- Gu X, Liu HC, Itoh K (2019) Inter-department patient handoff quality and its contributing factors in Chinese hospitals. Cognition, Technology & Work 21(1): 133-143.
- Wiig S, Fahlbruch B (2019) Exploring Resilience: A Scientific Journey from Practice to Theory.






























