A Case Report on Prevalence of Polycystic Ovarian Syndrome in an Adolescent Female from Bangalore Urban
Soumya V Menon1*, Surajit Sasmal2 and Nirmalya Bhattacharya2
1Department of Chemistry and Biochemistry, School of Sciences, Jain (Deemed to be University), Karnataka, India
2Department of Biochemistry, Indian Academy Degree College Autonomous, Hennur Cross, Kalyanagar, Karnataka, India
Submission: July 16, 2022; Published: July 25, 2022
*Corresponding author: Soumya V Menon, Department of Chemistry and Biochemistry, School of Sciences, Jain (Deemed to be University), Karnataka, India
How to cite this article: Soumya V M, Surajit S, Nirmalya B. A Case Report on Prevalence of Polycystic Ovarian Syndrome in an Adolescent Female from Bangalore Urban. Ann Rev Resear. 2022; 7(4): 555718. DOI: 10.19080/ARR.2022.07.555718
Abstract
PCOS is a multifactorial disorder in which diagnosis, treatment and management is very difficult as its causes and symptoms vary from one woman to another of reproductive age. The major characteristics include irregular and painful periods, obesity, diabetes, infertility, mental stress due to late diagnosis or improper diagnosis of PCOS. Hyperinsulinemia, hypercholesterolemia, dyslipidemia, cardiovascular disease are other co-morbidities. As the ovaries are affected majorly, ovarian cancer occurrence also is prevalent in PCOS women. It is a hyperandrogenic disorder with an approximate prevalence of 15% to 20%; despite being a common disease in women, an estimated 68% of the total cases remain undiagnosed. In this report we present a case study of a 20-year-old female diagnosed with PCOS at an early age. The elevated random blood sugar and total cholesterol levels indicated its relationship with insulin resistance and dyslipidemia. The comparison of results is made with respect to the control samples. Based on the results it is concluded that one major factor in the PCOS is overproduction of insulin which leads to insulin tolerance and obesity development in female population. Overall changes in the healthy lifestyle also may result in some complications in this disorder. Proper management and personalized medical treatments are the effective method and mainly psychological distress of the patient also needs to be addressed appropriately.
Keywords: Blood glucose; Cholesterol; Insulin resistance; Polycystic ovarian syndrome
Abbreviations: BMI: Body Mass Index, PCOS: Polycystic ovary syndrome; RBS: Random blood sugar; FAI: Free androgen index; IR: Insulin resistance
Introduction
Polycystic ovary syndrome (PCOS) is a multifactorial disorder with various genetic, metabolic, endocrine and environmental abnormalities. The general characteristics of PCOS are oligo/anovulatory cycles, hirsutism and polycystic ovaries, together with a considerable prevalance of insulin resistance. Although the aetiology of the syndrome is not completely understood yet, PCOS is considered a multifactorial disorder. Moreover, PCOS patients have a higher risk of metabolic and cardiovascular diseases and their related mobidity, if compared to the general population Menon & Golgeri [1]. It is a leading cause of female infertility. The prevalence of PCOS among reproductive-age women has been estimated at 4%-12%. Multiple biochemical pathways have been implicated in the pathogenesis of PCOS.
Women with PCOS show high prevalence of glucose intolerance. Research found that women with glucose normal glucose intolerance even after adjusting for age, BMI, waist hypertension, fasting insulin, testosterone and family history of diabetes. Results suggested that androgen excess indicated by high FAI (Free androgen index) levels might serve as indicator of glucose intolerance, as it might promote insulin resistance and β-cell dysfunction in women with PCOS Zhang et al. [2]. Other reasons include irregular food habits, lifestyle, obesity etc.
The worst condition about PCOS is that due to the longer process of diagnosis, various hormonal tests and other tests, doctor visits etc. which creates stress in some women. Because much is still unknown about PCOS, these women may not get the adequate answers that they were looking for. Furthermore, many women have stated that they are not much aware of this disorder, its prevalence, diet to be followed etc. which is a major lacuna in the studies done in PCOS.
Case Study
The study focused mainly on the identification of genetic changes in the PCOD patients and based on their biochemical profile, BMI index and other physiological changes. The consent was taken from all the four PCOD patients before conducting the study. All the patients aged between 20-30 years of age. The samples were collected from urban area of Bangalore and Dharwad, Karnataka during the period of February-March, 2019 and 2020. Here in this case study, we report the PCOD condition, biochemical observations of the woman aged 20 years residing in urban region of Bangalore, Karnataka.
Case History
Woman aged 20 years, had irregular periods, but no severity index of acne. There was a slight variation in the BMI index of the woman. After diagnosing with PCOD, there was a sudden increase in her body weight over the period of time may be due to the medications. Biochemical examination of her blood glucose showed very high levels of sugar than the normal level of random blood sugar level (RBS). With regard to the drug treatment and dosages and its medical complications were not revealed by the diagnostic centre/clinic nor the doctors due to ethical concerns. The written consent was taken from the patient as well as the control women.
Results & Discussion
The random blood sugar levels and total cholesterol were estimated and compared with control samples. The results are depicted in Table 1. From the results obtained, the woman with PCOS had a very high level of sugar compared with the control samples and this could be mainly due to the insulin resistance (IR) mechanism. There are numerous studies which highlights the relation between PCOS and diabetis mellitus. This syndrome is mainly seen to be involved with insulin defects causing IR. Moreover, these, IR is subjected with glucose intolerance in patients suffering type II diabetes along with obesity Book & Dunaif [3]. Studies suggests that pancreas of women with PCOS when compared to women of their age; tend to release high amount of insulin to counter act on high glucose levels.
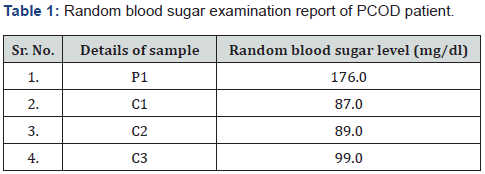
P1: Patient with PCOS; C1, C2, C3: Controls
In PCOS, basal insulin secretion is specified by global IR and resistance to insulin-induced increased, but insulin responses to glucose are suppression of lipolysis that was independent of inappropriately low. There is a relationship between adiposity and 17-OHP levels. Therefore, genetic insulin secretion and glucose tolerance known as predisposition to PCOS may be related with early IR and disposition index and under normal circumstances, the adipocyte dysfunction Menon & Golgeri [1]. Insulin resistance is also associated with hyperandrogenemia more than to irregular menus in women with PCOS (Table 2).
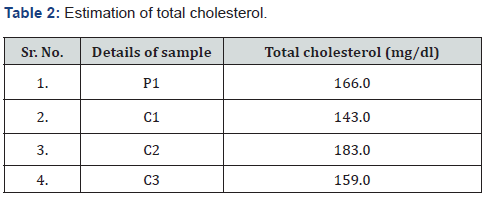
P1: Patient with PCOS; C1, C2, C3: Controls
The total cholesterol levels were high in P1 and C2 samples, other control samples reported lower amount of cholesterol in comparison with woman with PCOS. The abnormal levels of cholesterol can be related to obesity in PCOD woman, contributing to cardiovascular diseases. Lipid abnormalities, especially dyslipidemia, hypercholesterolemia etc. One of the animal studies by Patel & Shah [4] found that the implementation of a high-fat diet in prepubertal rats induced metabolic and ovarian changes which were present commonly in PCOS suggesting a potential impact of hyperlipidemia on the hormonal profile. It has also been observed that there is a significant increase in the levels of fatty acids and cholesterol in the follicular fluid of PCOS woman compared with normal woman Zhang [5].
References
- Menon SV, Golgeri DB (2021) A Review on Polycystic Ovarian Syndrome in Relation to Insulin Resistance Pathogenesis. Advances in Biological Research 15: 24-31.
- Zhang B, Wang B, Shen S, Liu J, Sun J, et al. (2018) Association of androgen excess with glucose intolerance in women with polycystic ovary syndrome, Biomed Res Int 8: 6869705.
- Book CB, Dunaif A (1999) Selective insulin resistance in the polycystic ovary syndrome. J Clin Endocrinol Metab 84(9): 3110-3116.
- Patel R, Shah G (2018) High-fat diet exposure from pre-pubertal age induces polycystic ovary syndrome (PCOS) in rats. Reproduction 155(2): 141-151.
- Zhang Yan, Liu L, Yin T Yang J, Xiong CL (2017) Follicular metabolic changes and effects on oocyte quality in polycystic ovary syndrome patients Oncotarget 8(46): 80472-80480.






























