Surgical Experience of Togo Level 2 Hospital During Peacekeeping Mission in Northern Mali
Akloa Kolima1, Assogba Komi2, Mossi K Edem3, Agbao A Komlan1, Bouassalo K Mawabah4, Lamboni Damessane5, Sama D Hamzah6 and Abalo Anani1
1Department of Orthopaedic and traumatology Surgery, Sylvanus Olympio University Teaching Hospital, Togo
2Department of Neurology, Teaching University Hospital of campus,Togo
3Departemet of Internal Medicine, Sylvanus Olympio University Teaching Hospital, Togo
4Department of Dental surgery, Dapaong regional hospital, Togo
5Department of Thoracic Surgery, Sylvanus Olympio University Teaching Hospital, Togo
6Department of Anaesthesiology, Sylvanus Olympio University Teaching Hospital, Togo
Submission: September 25, 2018;Published: October 29, 2018
*Corresponding author: Akloa Komlavi E. Kolima, Department of Orthopaedic and traumatology Surgery Teaching University Hospital Sylvanus Olympio Lomé-Togo, Togo, PO Box 57.
How to cite this article: Akloa K, Assogba K, Mossi K E, Agbao A K, Bouassalo K M, et al. Surgical Experience of Togo Level 2 Hospital During Peacekeeping Mission in Northern Mali. Ann Rev Resear. 2018; 4(2): 555635. DOI: 10.19080/ARR.2018.04.555635
Abstract
Introduction: The Level 2 hospital of Togo has been deployed in the northern sector of Mali to provide emergency medical and surgical care to patients in this sector. The purpose of this work was to report our surgical experience in the care of the wounded.
Materials and Methods: This was a cross sectional study conducted from September 2014 to March 2015. The parameters studied were the age, sex, time of admission, seat and nature of the lesions and the surgical procedure performed.
Results: Ninety-seven wounded including 92 men and 5 women were identified. Sixty-two (63.9%) wounded were admitted within hours of the attacks. We recorded 212 injuries of which 173 (81.6%) concerned the limbs, 18 (8.4%) seated on the thoraco-abdominal area and 9 (4.2%) were cranio-cerebral lesions. The radio-clinical assessment allowed us to diagnose 69 cases (32.5%) of musculo-cutaneous decay and 20 cases (9.4%) of opened fractures. The thoracoabdominal lesions were penetrating in seven cases. Severe wounded received resuscitation and six were operated on urgently. We evacuated 10 (10, 3%) patients to a level 3 hospital in Bamako for further care.
Conclusion: The experience obtained in caring of the wounded during these attacks allowed us to improve our strength in the management of the wounded in the war field and save life.
Keywords: Surgical Experience; Medical support; Mission; Trauma injury; North Mali
Introduction
In 2013 the United Nations Council adopted Resolution 2100 (2013) establishing the United Nations Multidimensional Integrated Mission for the Stabilization of Mali (MINUSMA) [1]. The view was to pacify the conflict that had started since 2012. This mission constituted of military and police officers of many nationalities. Several types of both conventional and unconventional weapons were regularly used to attack the forces of this mission resulting in several casualties and deaths [2-4]. According to the International Committee of the Red Cross (ICRC), gunshot injuries account for 65-78.25% of injuries in conflict [5-7]. When these lesions were not deadly on the battlefield, the soldiers died secondarily by lack of proper care [8].
The United Nations health care system has been therefore organized into several steps with increasingly facilities care from battlefields to rehabilitation centers to keep the life-threatening of a maximum number of wounded and maintain them functional [9]. It was in that context, that the Togolese level 2 (TGLV2) hospital was deployed in the northern sector of Mali to provide emergency medical and surgical care to soldiers in this sector. These soldiers were often attacked while performing their duties.
This hospital was based in Kidal and was the referral facility for the entire northern sector. The purpose of this work was to describe the capabilities of TGLV2 hospital and report our surgical experience in the care of the wounded during two attacks against MINUSMA’s Kidal camp.
Materials and Methods
Framework of study
Togo Level 2’s hospital is a referral health facility in the northern part of Mali. Its main was to provide emergency medical and surgical care to soldiers engaged in the mission and to civilian staff of MINUSMA. Secondly, it provides medical assistance to local civilian population of this sector through some health actions to strengthen the links between members of the mission and the civilian population.
The capacities and resources of the hospital
Hospital equipment
Togo Level 2 Hospital is a front-end care facility. It has 20 beds hospital. It was able to provide resuscitation and emergency surgical care to causalities before there evacuation to a higherlevel hospital. For this purpose, the hospital had a resuscitation unit (Figure 1), an intensive care unit, an operating room, a radiology unit, a laboratory, and an aeromedical evacuation team (AMET).

It had also a dental unit and a pharmacy. The hospital is refueled every month and has an operational autonomy of 2 months.
a) The operating room (Figure 2) had two operating tables that can be used simultaneously when needed. The sterilization equipment was constituted of two autoclaves and two dolls.

b) The radiological unit had a fixed standard X-ray machine, a mobile X-ray, and two mobile ultrasounds.
c) The dental office had a dental chair, and a dental X-ray machine.

d) The AMET has two ambulances equipped for emergency care and several emergency kits (Figures 3).
Composition of the medical staff
The medical staff consisted of 15 doctors and 22 nurses. The doctors were distributed as follows: a chief medical officer, a deputy chief physician, two surgeons, a resuscitation doctor, an internist doctor, a dental surgeon, a public health doctor, a general practitioner, five doctors in charge of aeromedical evacuations and a pharmacist.
The surgical team was composed of a general surgeon, an orthopedic surgeon, a resuscitation doctor and six nurses (two anesthesiologists, two operating room nurses, two emergency nurses). The paramedical personal were distributed in to the different units of the hospital. Four nurses were assigned for evacuations, three for the reception of patients, three for hospitalizations, two at the dental office, two at the pharmacy and two at the laboratory.
The activities of the hospital
In addition to situation of massive influx of wounded, the hospital performs daily consultations, dental care and following of hospitalized patients. Some common surgical pathologies were programmed and operated. The resources of the hospital allow to perform:
a) 40 patient consultations / day,
b) 5-10 consultations and dental care / day,
c) 10-20 hospitalizations for 7 days,
d) 3-5 surgeries / day.
Radiological and biological examinations were also performed daily.
In an attack context, the wounded were evacuated from level 1 structures to the level 2 hospital by the medical team of each contingents. When the patient needed resuscitation during transport, our evacuation team was asked to pick up the casualties from the field and evacuate them to the Level 2 hospital.
Patient medical data was stored in medical records and archived. These data were used for the realization of some scientific works. Some training exercises, refresher and upgrading courses are given regularly to our personnel and to the personnel of the other contingents of the sector in order to maintain the operational capacity of the camp.
Type of study and period
This was a cross-sectional study focus on management of wounded during two attacks against MINUSMA’s Kidal camp. The first occurred on November 28th, 2015 made of mortar and rocket fire and the second occurred on February 12th, 2016 made of mortar fire followed by the explosion of a kamikaze car.
After each attack, all the victims were received in triage room where they were categorized according to their hemodynamic status and named as alpha (A), bravo (B) and Charli (C).
a) The alpha wounded regrouped those whom hemodynamic state was unstable and needed, in addition to resuscitation, an emergency surgery for their stabilization.
b) The wounded bravo was consisted of patients with an unstable hemodynamic state and stabilized by resuscitation. The surgical procedure can be performed after stabilization of the hemodynamic state.
c) The wounded Charli regrouped patients with stable hemodynamic status and benign lesions.
The interrogation of the wounded or their entourage allowed to collect the identity, the age, the sex, and the time of admission, the mode of admission. The site of the lesions was established after a clinical examination. The unstable wounded were admitted to operating room for emergency treatment. After stabilization of the hemodynamic state, some patients were to transfer to a higher level, and others were followed in our hospital according to the lesions of the patient and our resources.
Results
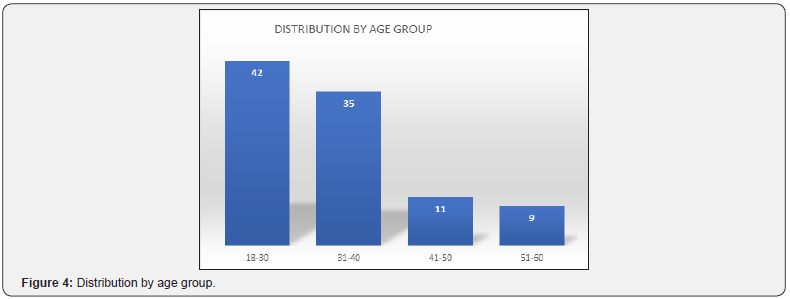
Ninety-seven wounded were identified during these two attacks, 37 wounded in the first attack and 60 wounded in the second attack. There were 92 men and 5 women. The most affected age group was 18 to 30 (Figure 4).
The wounded were admitted immediately after the attacks. Sixty-two (63.9%) wounded were admitted in the hour following the attack, 23 patients (23.7%) were admitted between the second and sixth hours, and 12 other patients (30%) were admitted beyond the 6th hour. The wounded were transported to TGLV2 hospital with ambulances available in each unit of Kidal camp.
The admission of causalities of the attack at the same time into TGLV2 hospital created an influx of wounded. The sorting and categorization of the wounded allowed to manage these massive influxes of wounded.
A clinical examination allowed us to assess the hemodynamic state and consciousness of the wounded. So, we found 11 (11.4%) alpha, 32 (32.9%) bravo and 34 (55.7%) Charli wounded.
We recorded a total of 212 injuries, 85 after the first attack and 127 after the second attack. We found 173 (81.6%) limb lesions, 18 (8.4%) thoracoabdominal lesions, 9 (4.2%) cranio-cerebral lesions, and 12 (5.6%) of ENT lesions (Table 1). More than half (60.8%) of the wounded had an associated injury. Thirty-eight (39.2%) wounded had one lesion.

Injuries concerned lower limbs in 95 (54.9%) cases and upper limbs in 78 (45.1%) cases. We noted a predominance of the leg lesions (18.5%) and thigh (14.1%) lesions on the lower limb. In the upper limb this predominance concerned the shoulder (13.1%) and the hand (12.7%).
The thoracoabdominal lesions concerned the thorax in 7 cases and the abdomen in 11 cases.
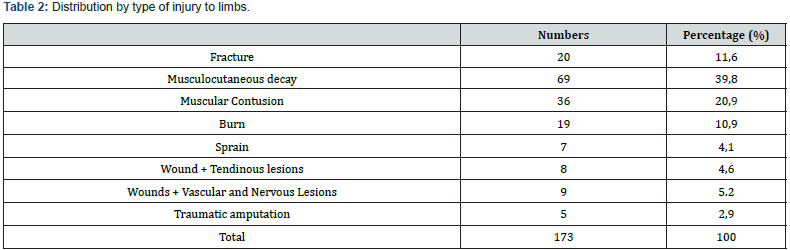
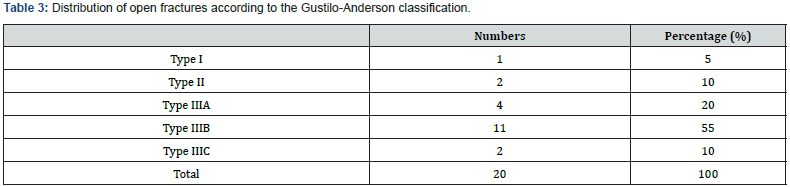
The radio-clinical assessment revealed 69 cases (32.5%) of musculo-cutaneous decay, 20 cases (9.4%) of fractures that were all open (Table 2). The classification of these open fractures according to Gustilo-Anderson noted a predominance of type IIIb lesions (Table 3). The thoracoabdominal lesions were penetrating wounds in seven cases. The remaining 11 lesions were parietal contusions and superficial wounds of the thoracoabdominal wall. The examination of the ENT sphere found 7 cases of tympanic rupture and 5 cases of burns of the upper airways.

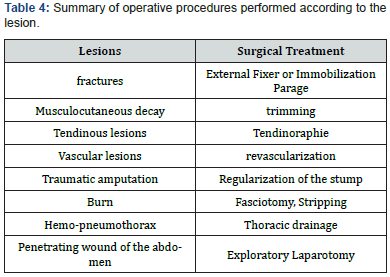
Six alpha wounded were operated emergently. The other injured alpha and bravo had been resuscitated as soon as they were admitted (Figure 5). They were operated once their hemodynamic state was stabilized. The procedure performed depended on the preoperative diagnosis and the lesions observed during the procedure (Table 4).
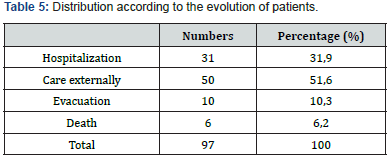
We evacuated 10 (10, 3%) patients to a higher-level hospital at Bamako for further care. The other wounded were followed in our hospital until their wounds were healed (Table 5). Nether sequels bad been noted on patient we had followed in our hospital. We recorded 6 (6, 18%) deaths during these two attacks.
Patients in our hospital and those who were externally followed received psychological support. In group therapy sessions were organized for all soldiers who were on the site during the attack.
Discussion
Ninety-seven patients were identified. The most affected age group was 18-30. This low average age reflects the relatively youngness of soldiers deployed in this peacekeeping operation. Most of them were on their first peacekeeping mission and faced these attacks for the first time. Psychological support must be provided to these causalities to avoid post-traumatic stress [10].
We counted 92 men for 5 women. The clear predominance of male casualties is related to the fact that very few women are deployed in the conflict area. This low female representation in conflict theaters was noted during deployments in Iraq and Afghanistan [11,12].
The injuries depend on the type of explosive and the distance between the casualties and the center of the explosion. Explosive detonation causes five types of injury [13].
More than half of the wounded were admitted to the hospital within one hour of the attack. TGLV2 hospital is located in the camp, the transfer of wounded was done quickly and within less than 6 hours for most of the wounded. The organization of the system of care in different levels allowed refer of the wounded requiring the surgical care to the appropriate level and to preserve their prognosis vital.
Limbs injuries constituted 81, 6% in our study. War lesions are particularly violent and affect the limbs in 70% of the cases, are often opened and contaminated [14]. When lesions were caused by kamikaze explosion, the wounds of the causalities can be contaminated by the kamikaze’s tissues and his blood. Viral and sometimes bacterial infections of the kamikaze can be transmitted to the causalities during this exposure [15,16]. We did not find traces of foreign body tissue on our patients, but we cannot attest that some of them were not infected by the blood of the kamikaze.
We had 81.6% of limb injuries in our study, of which 54.9% were in the lower limbs.
Excision and debridement were the most surgical procedures performed in our study. The first step in the management of these lesions is washing and cleaning wounds with serum and antiseptics after antibiotic administration. Correct debridement is the best way to avoid infection and gangrene of limbs [17-19].
The treatment of musculocutaneous decay consists of a wide excision of all necrotic tissues or doubtful vitality. Ablation of all foreign bodies accessible during trimming must be done. The use of a tourniquet allowed to avoid blood loss. It also allows a better tissue appreciation [20]. The wounds are left open and their closure is realized only secondarily after elimination of all infection signs [21]. Fasciotomies are performed for compartmental syndromes during this debridement [17].
Fractures are treated according to Orthopedic Damage Control principles. It consists of a temporary stabilization, in order to control the bleeding, to vascularize the limb and to excise the necrotic tissue while ensuring a resuscitation of the patient. The objective is to preserve the patient’s vital prognosis and then evacuate to a more equipped center where a final stabilization by external or internal fixation can be performed according to the cutaneous state [22-24]. The principles of treatment of closed fractures do not differ from those used in routine traumatology. After administration of analgesic, fractures are reduced and temporarily immobilized by a splint. Final care is provided in a specialized facility outside the conflict zone [25].
We recorded 10, 9% of burn lesions. The management of burn injuries is difficult and long, especially when associated with other serious lesions [8]. The patient once admitted is washed correctly with an antiseptic solution and then examined to determine the degree and surface area burned. When the burn affects more than 2/3 of the circumference of a limb segment, a discharge incision is made.Burning of the face and neck can lead to considerable edema, sometimes impeding the permeability of the airways. A tracheostomy can be performed if needed.
The phlyctenes are flattened and a sterile dressing with antiseptic gel is carried out [26-28]. The hemorrhage from vascular lesions are responsible for 90% of deaths on battle theaters [29]. Pre-hospital care involves the use of tourniquet and hemostatic dressings. These techniques are taught to all soldiers. Vascular ligations for hemostasis are contraindicated and usually lead to amputations. Vascular repair performed in the context of damage control should be done within 2 hours of the trauma. The saphenous vein may serve as an autologous graft for loss of substances [30,31].
The traumatic amputations secondary to the explosions are accompanied by an important destruction and a contamination of the soft parts. The level of healthy tissue does not correspond to the seat of traumatic amputation [11, 32,]. Three levels of amputation had been descripted after an explosion [33].
Zone I represent the area closest to the seat of the explosion [11,13]. It is characterized by traumatic amputation of the limb, with extensive damage and extensive destruction of the skin, tendons, vessels, muscles and bones. Soft tissue lesions in this area are associated with significant soil contamination and explosive fragments under tension.
Surgical amputations performed in Zone I were considered unsustainable
a) In zone II of the injured limb, there are focal areas of muscle micro-laceration, associated with lacerations of small and large blood vessels.
b) The main features of the wounds in Zone III are avulsion of small arterioles, impaired venous return, and reactive changes in peripheral nerve axons.
c) The optimal level of surgical amputation which is recommended is the limit of zones II and III [32].
d) Tendon and nerve damage are not repair in emergency in the context of damage control. It is recommended to locate the ends of the tendons or nerves sectioned and then fix them temporarily in the soft parts to avoid their retraction. Their repair will be secondarily performed once the wounded stabilized [34].
e) We evacuated 10, 3% of wounded to a higher-level structure for further care. The primary mission of a Level 2 hospital is to provide emergency medical and surgical care. Once the patient has been hemodynamically stabilized and the emergency surgery is completed, the casualty must be referred to a Level 3 hospital where treatment is continued [16]. The patient is usually evacuated within 24 hours of arriving at the Level 2 Hospital. Our patients were evacuated to Bamako and to Dakar for some.
f) The mortality rate recorded during these attacks is low compared to that of the literature [35,36]. Emergency management and the rapid evacuation of the wounded to higher level structures may explain the low mortality rate recorded during these attacks.
Conclusion
The Level 2 hospital in Togo is the referral facility in northern Mali. Its capabilities in equipment and human resources allow to effectively support the wounded in the northern sector of Mali. This first experience as a Level 2 hospital in a peacekeeping mission allowed us to note a predominance of limb injuries during attacks. The most lethal lesions concern the head, the neck, the thorax and the abdomen. The emergency management of the lesions must be done according to the principle of damage control followed by the rapid evacuation of the wounded to higher level hospitals. Many injured had been saved by using this therapeutic strategy. The experience obtained in caring for the wounded during these attacks allowed us to improve our results in the management of the wounded of war.
References
- United Nations (2013) Security Council Distr General. Resolution 2100. pp. 12.
- Coupland RM, Samnegaard HO (1999) Effect of type and transfer of conventional weapons oncivilian injuries: retrospective analysis of prospective datafrom Red Cross hospitals. BMJ 319(7207): 410-412.
- Hakimoglou S, Karcioglu M, Tuzcu K, Davarcı I, Koyuncu O, et al. (2015) Assessment of the peroperative period in civilians injuried in Syrian civil war. Rev Bras Anestesiol 65(6): 445-449.
- Ramasamy A, Harrisson SE, Clasper JC, Stewart MP (2008) Injuries from roadside improvised explosive devices. J Trauma 65(4): 910-914.
- Meddings RD (1997) Weapons injuries during and after periods of conflict: retrospective analysis. BMJ 315(7120): 1417-1420.
- Coupland RM, Korver A (1991) Injuries from antipersonnel mines: the experience of the International Committee of the Red Cross. BMJ 303(6816): 1509-1512.
- Murray CK, Obremskey WT, Hsu JR, Andersen RC, Calhoun JH, et al. (2011) Prevention of infections associated with combat-related extremity injuries. J Trauma 71(2 Suppl 2): S235-S257.
- Colin N, Mifsud M, Borg JN, Mizzi C (2015) The Libyan civil conflict: selected case series of orthopaedic trauma managed in Malta in 2014. Scand J Trauma Resusc Emerg Med 23: 103.
- Malin AS, Brannan PS (2013) The deployed military Orthopaedic Surgeon: experiences of a recent Iowa graduate in Afghanistan. Iowa Orthop J 32: 231-235
- Hoge CW, Castro CA, Messer SC, McGurk D, Cotting DI, et al. (2004) Combat Duty in Iraq and Afghanistan, Mental Health Problems, and Barriers to Care. N Engl J Med 351(1): 13-22.
- Ramasamy A, Harrisson SE, Stewart MPM, Midwinter M (2009) Penetrating missile injuries during the Iraqi insurgency. Ann R Coll Surg Engl 91(7): 551-558.
- Ziemba R (2012) Types of injuries among Polish soldiers and civilian staff in the 7th, 8th, 9th and 10th rotation of the Afghan stabilization mission. Med Sci Monit 18(3): 9-15.
- FrankeA, Bieler D, Friemert B, Schwab R, Kollig E, et al. (2017) The First Aid and Hospital Treatment of Gunshot and Blast Injuries. Dtsch Arztebl Int 114(14): 237-243.
- Sheean AJ, Tintle SM, Rhee PC (2015) Soft tissue and wound management of blast injuries. Curr Rev Musculoskelet Med 8(3): 265- 271.
- Patel HD, Dryden S, Gupta A, Stewart N (2012) Human body projectiles implantation in victims of suicide bombings and implications for health and emergency care providers: the 7/7 experience. Ann R Coll Surg Engl 94(5): 313-317.
- Braverman I, Wexler D, Oren M (2002) A novel mode of infection with hepatitis B: penetrating bone fragments due to the explosion of a suicide bomber. Isr MedAssoc J 4(7): 528-529.
- Bakhach J, Abou Ghanem O, Bakhach D, Zgheib E (2017) Early free flap reconstruction of blast injuries with thermal component. Ann Burn Fir Dist 30(4): 303-308.
- Bowyer GW (1996) Management of small fragment wounds: experience from the Afghan border. J Trauma 40(3 Suppl): 170-172.
- Taylor CJ, Hettiaratchy S, Jeffery SL, Evriviades D, Kay AR (2009) Contemporary approaches to definitive extremity reconstruction of military wounds. J Roy Army Med Corps 155(4): 302-307.
- Coupland RM (1991) The role of reconstructive surgery in the management of war wounds. Ann R Coll Surg Engl 73(1): 21-25.
- Evriviades D, Jeffery S, Cubison T, Lawton G, Gill M, Mortiboy D (2011) Shaping the military wound: issues surrounding the reconstruction of injured servicemen at the Royal Centre for Defence Medicine. Philos Trans R Soc Lond B Biol Sci 366(1562): 219-230.
- Mathieu L, Ouattara N, Poichotte A, Saint-Macari E, Barbier OF, et al. (2014) Temporary and definitive external fixation of war injuries: use of a French dedicated fixator. Int Orthop 38(8): 1569-1576.
- Possley DR, Burns TC, Stinner DJ, Murray CK, Wenke JC, et al. (2010) The Skeletal Trauma Research Consortium Temporary external fixation is safe in a combat environment. J Trauma 69 Suppl 1: S135-S139.
- Lerner A, Fodor L, Soudry M (2006) Is staged external fixation a valuable strategy for war injuries to the limbs? Clin Orthop Relat Res 448: 217-224.
- Barbiera O, Malgrasb B, Versiera G, Ponsc F, Rigald S, et al. (2014) French surgical experience in role 3 medical treatment facility of Kaia (Kabul International Airport, Afghanistan): The place of orthopedic surgery. Orthop Traumatol Surg Res 100(6): 681-685.
- Vinsonneau C, Benyamina M (2009) Management of major thermal burns. Réanimation 18: 679-686.
- Cuttle L, Pearn J, McMillan JR, Kimble RM (2009) A review of first aid treatments for burn injuries. Burns 35(6): 768-775.
- Brusselaers N, Hoste EAJ, Monstrey S, Colpaert KE, De Waele JJ, et al. (2005) Outcome and changes over time in survival following severe burns from 1985 to 2004. Intensive Care Med 31(12): 1648-1653.
- Van Oostendorp SS, Tan EC, Geeraedts LM (2016) Prehospital control of life-threatening truncal and junctional haemorrhage is the ultimate challenge in optimizing trauma care; a review of treatment options and their applicability in the civilian trauma setting. Scand J oTrauma Resusc and Emerg Med 24(1): 1-13.
- Tien HC, Spencer F, Tremblay LN, Rizoli SB, Brenneman FD (2007) Preventable deaths from hemorrhage at a level I Canadian trauma center. J Trauma 62(1): 142-146.
- Hinck D, Gatzka F, Debus ES (2011) Surgical combat treatment of vascular injuries to the extremities. American experiences from Iraq and Afghanistan. Gefässchirurgie 16: 93-99.
- Hull JB, Bowyer GW, Cooper GJ, Crane J (1994) Pattern of injury in those dying from traumatic amputation caused by bomb blast. Br J Surg 81(8): 1132-1135.
- Clasper J, Ramasamy A (2013) Traumatic amputations. Br J Pain 7(2): 67-73.
- Bennett PM, Stevenson T, Sargeant ID, Mountain A, Penn-Barwell JG (2018) Outcomes following limb salvage after combat hindfoot injury are inferior to delayed amputation at five years. Bone Joint Res 7(2): 131-138.
- Arora MM, Bhatia JK, Rana K (2009) Pattern of Fatal Injuries in Counter Terrorist Operations: An Innovative Analysis through Embalming Services. Med J Armed Forces India 65(2): 103-107.
- Singleton JA, Gibb IE, Hunt NC, Bull AM, Clasper JC (2013) Identifying future unexpected survivors: a retrospective cohort studyof fatal injury patterns in victims of improvised explosive devices. BMJ Open 3(8): e003130.






























