Duodenal Ulcer a Rare Peptic Ulcer Disease in Children: Two case Reports in a Tertiary Care Hospital of Bangladesh
Afsana Yasmin1*, Rokshana Haque2, Qausar Alam JMH3, Natasha Tarannum4 and Mashfiqur Rahman Khan5
1MD (Pediatric Gastroenterology), MCPS, MRCPCH (Pediatrics), Consultant, Department of Pediatrics and Pediatric gastroenterology, KPJ specialized Hospital Dhaka, Bangladesh
2DCH, MRCPCH (Pediatric), Consultant and Head, Department of Pediatrics, Department of Pediatrics, KPJ specialized Hospital Dhaka, Bangladesh
3MRCS, FRCS, Consultant, General surgery, KPJ specialized Hospital Dhaka, Bangladesh
4MD (Hepatology), Hepatologist, KPJ specialized Hospital Dhaka, Bangladesh
5FCPS, MCPS, DA (Anesthesiology), Anesthesiologist, KPJ specialized Hospital Dhaka, Bangladesh
Submission:March 17, 2026;Published:March 25, 2026
*Corresponding author:Afsana Yasmin, MD, MRCPCH, MCPS, Consultant Pediatrician and Pediatric gastroenterologist, Department of Pediatrics, KPJ specialized Hospital Dhaka, Bangladesh
How to cite this article:Afsana Y, Rokshana H, Qausar Alam JMH, Natasha T, Mashfiqur Rahman K. Duodenal Ulcer a Rare Peptic Ulcer Disease in Children: Two case Reports in a Tertiary Care Hospital of Bangladesh. Adv Res Gastroentero Hepatol, 2026; 22(3): 556087.DOI: 10.19080/ARGH.2026.22.556087.
Abstract
Peptic ulcer disease uncommon in children, among PUD, Duodenal ulcer rarer than gastric ulcer. Therefore, physicians are less suspicious of DU in pediatric patients. It was diagnosed when already in advanced stage presented with GI bleeding. We report two cases who presented at OPD with active hematemesis by case 1 a 9-year boy and other case 2 a 13-year boy with iron deficiency anemia and later with vomiting and abdominal pain. There were no medical problems, and no drugs, such as corticosteroids or non-steroidal anti-inflammatory drugs. In case 1 we tried to control bleeding with octreotide and omeprazole infusion followed by endoscopic haemoclip application and 2nd case we gave PPI infusion. Both cases discharged with oral antibiotics 14 days and PPI 6 weeks. They recovered well without any complications. However, case 2 develop recurrence after 2 months and 2nd time anti-H. pylori treatment was needed.
Keywords:Duodenal ulcer; PUD; Children; Hematemesis; Anemia
Abbreviations:PUD: Peptic ulcer disease; GI: gastrointestinal; DU: duodenal ulcer; HP: Helicobacter pylori; ZES: Zollinger-Ellison syndrome; NSAID: Non-Steroidal Anti-Inflammatory Drugs; CD: Crohn’s disease; EGD: esophagogastroduodenoscopy
Introduction
Peptic ulcer disease (PUD) refers to a mucosal defect deeper than the muscularis mucosa involving the duodenal wall is duodenal ulcer (DU). The presentations of DU range from asymptomatic, dyspepsia, abdominal pain, upper gastrointestinal (GI) bleeding to perforation [1]. The etiologies of DU are The hemoglobin (Hb) was 8.6 g/dL despite getting iron supplementation which was 6 gm/dl 3 months back, MCV-65, MCHC 17. His CRP, LDH, USG whole abdomen liver function test barium enema was normal. Upper GI endoscopy has done which showed a large duodenal (Hp) infection, Non-Steroidal Anti-Inflammatory Drugs (NSAIDs), other potential factors include acid hypersecretion (Zollinger-Ellison syndrome (ZES)), eosinophilic gastroenteropathy, non-Hp infections, malignancy, Ischemic event, medications (corticosteroids, anti-cancer drugs, iron chelators, etc.), Crohn’s disease (CD), and other infiltrative diseases. Among them incidence of Hp infection in pediat ric DU increasing for availability of lab facilities [1-7]. We reported two cases of DU in children presenting with acute bleeding in one and epigastric pain with refractory anemia in other cases. Another study suggested that patients with Hp-related PUD had higher mean age and rate of family history, but they enrolled patients with “PUD” instead of exclusive DU.
Case 1
A 9-year- 3-month-old boy got admitted through OPD with complaints of abdominal pain since last night, hematemesis for 5 times since morning. On query, he had Headache and stuffy nose. His perinatal history uneventful, no history of jaundice, no previous bleeding manifestations, no offending drug history. On admission baby was alert, ill looking, pale, HR; 101 bpm, RR: 22 bpm, SpO2: 95% in room air, temp: 98.2f, BP 100/70 mm hg, anthropometrically normal, abdomen: soft, epigastric tenderness present. Other systems revealed no abnormality. The hemoglobin (Hb) was 6.3 g/dL, platelet normal, PBF, Liver function test, PT, APTT normal and transfusion started. Infusion octreotide loading dose followed by maintenance started and also standard dose of infusion omeprazole started loading followed by maintenance. After stabilization upper GI endoscopy have done which showed large duodenal ulcer in 1st part of duodenum Forest classification IIC and haemoclip placed. Tissue biopsy taken, RUT was positive and histopathology revealed features of gastritis and duodenitis. After bleeding his hemoglobin increased to 9 gm/dl. Patients were discharged with amoxicillin and clarithromycin 14 days PPI for 6 weeks. On follow up he was stable with no recurrent symptoms.
Case 2
A 13-year-old boy visited the OPD with complaints of vomiting for few days and vomitus containing raw fleshy few pieces. On query he had history of upper abdominal pain became severe at night, aggravated after meal. He visited to medicine OPD with complaints of loss of appetite, vertigo pallor and diagnosed as IDA after blood tests 3 months back and treated conservatively with iron supplementation. He had no history of hematemesis melena, haematochezia and loss weight. There were no previous hospitalizations or medical problems, his immunization status was up-todate, and no drugs had been prescribed or administered recently (especially NSAIDs). Physical examination revealed pallor present, not icteric, anthropometrically normal, vitally stable, blood pressure 110/60 mmHg; pulse rate 110 beats/minute (bpm); respiration rate 20 breaths/min; temperature 98 F., per abdominal examination revealed epigastric tenderness with no organomegaly. Chest examination revealed regular heart beats without murmurs and clear breath sounds. Bowel sounds were hyperactive without localized tenderness or rebound tenderness.
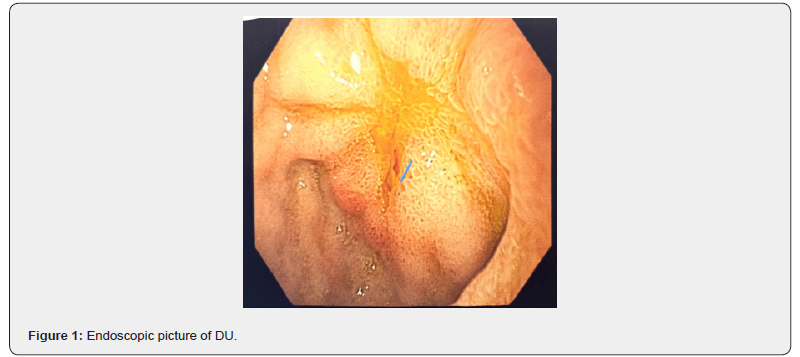
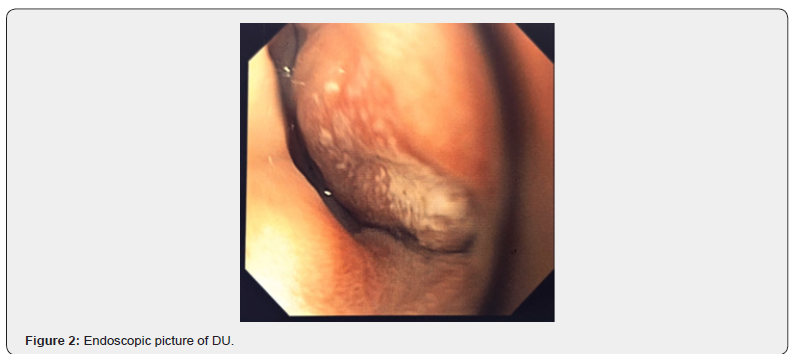
The hemoglobin (Hb) was 8.6 g/dL despite getting iron supplementation which was 6 gm/dl 3 months back, MCV-65, MCHC 17. His CRP, LDH, USG whole abdomen liver function test barium enema was normal. Upper GI endoscopy has done which showed a large duodenal ulcer in 1st part of duodenum Forest classification 2C. RUT positive and histopathology report showed the lamina propria reveals increased number of chronic inflammatory cells including eosinophils. Small amount of granulation tissue is also present. No evidence of malignancy is found. Features suggestive of chronic duodenitis with nonspecific ulcer. The patient was treated with Amoxicillin and clarithromycin for 14 days and esomeprazole for 6 weeks with iron supplementation. The patient fully recovered. Follow up endoscopy after 10 weeks showed –duodenal ulcer still present but better than previous with RUT positive, therefore H. pylori eradication treatment again started with PPI and sucralfate. Now patients are symptoms free (Figure 1 & Figure 2).
Discussion
DU is an important etiology of GI bleeding or acute abdomen in children. We reported two cases of DU who presented with acute massive GI bleeding and abdominal pain with refractory anemia. The prevalence of DU in children ranges at around 1.6–13.7%(cases/ EGDs), depending on the country, study year (2001–2018), and test indications reported by previous cohort of studies [8-18]. The annual incidences were around 3–5%(cases/EGDs) reported by a recent large cohort study in Taiwan [19]. Though common etiology of DU in children is NSAIDS, corticosteroids, H-pylori infection, eosinophilic gastroenteropathy, underlying secondary cause like IBD, portal hypertension, HSP but younger age group specially in neonate, the risk factors for ulcer are prematurity, hypovolemia, stress, coagulopathy [19]. In both of our cases we found H. Pylori infection is the cause of DU. The most prevalent symptoms were abdominal pain, vomiting, melena, hematemesis, and dizziness (and weakness), nocturnal pain [12]. If left untreated may develop shock perforation and death. The cases in this study also presented with hematemesis and anemia with abdominal pain. The Hp-positive group was prone to “hemorrhagic” features (melena, syncope, anemia) that we found in our cases. Male children, hematemesis and melena, decreased hemoglobin levels and high uric acid levels are clinically predicting factors of DUs due to H. Pylori infection and the children should be promptly referred to a facility with pediatric endoscopic capabilities for further diagnosis and treatment [20].
Diagnosis of duodenal ulcer was done by direct visualization with esophagogastroduodenoscopy (EGD). Contrast barium swallows imaging also can help in diagnosis where EGD facilities are not available. H. pylori infection can be diagnosed with rapid urease test. Besides that, microscopic evidence of H. pylori infection, culture sensitivity and PCR of tissue specimen can be done specially in refractory or recurrence H. pylori infection. The cure of H. pylori after treatment can be assessed using the 13C-urea breath test (UBT) or stool antigen test at least 4 weeks after therapy [21,22]. In the presented cases H. pylori was found by positive RUT and microscopic evidence of H. pylori. Histopathology showed features of chronic inflammatory cells without any malignant cells. However, culture sensitivity test had not done. Treatment of DU is treatment of acute condition, complications and underlying pathology H. pylori eradication. If presented with acute bleeding or perforation may need control of bleeding by endoscopic or surgical intervention. For anemia blood products or hematinic supplementations [19]. In this case series who presented with active bleeding need endoscopic haemoclip application. For H. pylori infection, 1st line therapy in children triple drug therapy PPI with amoxicillin with clarithromycin or metronidazole for 14 days according to NASPGHAN & ESPGHAN [23]. Other treatments of H. pylori eradication are sequential therapy for 10 days, concomitant therapy or bismuth based quadruple therapy, adjuvant therapy with probiotics [22]. In our patients we had given conventional triple drug therapy. Second, older patient was refractory to treatment, and second line therapy was given. A recent study PJ et al showed there were four independent parameters were associated after multivariable logistic regression analysis for refractory or recurrence of DU. Male sex, lower Hb level, and perforation were risk factors for refractory or recurrence, while hematemes is showed a possible reverse effect need at 1 follow up EGD [19]. Our 2nd patient was male and had low hb, follow EGD showed still ulcer was present and 2nd line therapy was given.
Conclusion
DU though rare in children should be excluded if children are presented with hematemesis melena and unexplained anemia. Early intervention can prevent complications and case fatality.
References
- Ocasio Quinones GA, Woolf A (2022) Duodenal ulcer. StatPearls. Treasure Island (FL): StatPearls Publishing LLC.
- Kubo K, Kimura N, Mabe K, Matsuda S, Tsuda M (2020) Eosinophilic gastroenteritis-associated duodenal ulcer successfully treated with crushed budesonide. Intern Med 59: 2249-2254.
- Riggle KM, Wahbeh G, Williams EM, Riehle KJ (2015) Perforated duodenal ulcer: an unusual manifestation of allergic eosinophilic gastroenteritis. World J Gastroenterol 21: 12709-12712.
- Annibale B, De Magistris L, Corleto V, D’Ambra G, Marignani M (1994) Zollinger-Ellison syndrome and antral G-cell hyperfunction in patients with resistant duodenal ulcer disease. Aliment Pharmacol Ther 8: 87-93.
- Blecker U, Gold BD (1999) Gastritis and peptic ulcer disease in childhood. Eur J Pediatr 158: 541-546.
- Bernard R, Aljomah G, Klepper E, McDonough E (2017) Cytomegalovirus-associated duodenal ulcer and duodenitis in a malnourished pediatric patient. Case Rep Pediatr 2017: 2412930.
- Zahra A, Ragab A, Al-Abboh H, Ismaiel A, Adekile AD (2021) Perforated duodenal ulcer associated with deferasirox in a child with β-thalassemia major. Hemoglobin 45: 335-337.
- Elitsur Y, Lawrence Z (2001) Non-Helicobacter pylori-related duodenal ulcer disease in children. Helicobacter 6: 239-243.
- Demir H, Gürakan F, Ozen H, Saltik IN, Yüce A (2002) Peptic ulcer disease in children without Helicobacter pylori infection. Helicobacter 7: 111.
- El Mouzan MI, Abdullah AM (2004) Peptic ulcer disease in children and adolescents. J Trop Pediatr 50: 328-330.
- Kato S, Nishino Y, Ozawa K, Konno M, Maisawa S (2004) The prevalence of Helicobacter pylori in Japanese children with gastritis or peptic ulcer disease. J Gastroenterol 39: 734-738.
- Kawakami E, Machado RS, Fonseca JA, Patrício FR (2004) Clinical and histological features of duodenal ulcer in children and adolescents. J Pediatr 80: 321-325.
- Egbaria R, Levine A, Tamir A, Shaoul R (2008) Peptic ulcers and erosions are common in Israeli children undergoing upper endoscopy. Helicobacter 13: 62-68.
- Houben CH, Chiu PW, Lau JY, Lee KH, Ng EK (2008) Duodenal ulcers dominate acute upper gastrointestinal tract bleeding in childhood: a 10-year experience from Hong Kong. J Dig Dis 9: 199-203.
- Bontems P, Kalach N, Vanderpas J, Iwanczak B, Casswall T (2013) Helicobacter pylori infection in European children with gastro-duodenal ulcers and erosions. Pediatr Infect Dis J p: 32.
- Huang SC, Sheu BS, Lee SC, Yang HB, Yang YJ (2010) Etiology and treatment of childhood peptic ulcer disease in Taiwan: a single-center 9-year experience. J Formos Med Assoc 109: 75-81.
- Hernández C, Serrano C, Einisman H, Villagrán A, Peña A (2014) Peptic ulcer disease in Helicobacter pylori-infected children: clinical findings and mucosal immune response. J Pediatr Gastroenterol Nutr 59: 773-778.
- Boyanova L, Hadzhiyski P, Markovska R, Yaneva P, Yordanov D (2019) Prevalence of Helicobacter pylori is still high among symptomatic Bulgarian children. Acta Microbiol Immunol Hung 66: 255-260.
- Yeh PJ, Chen CC, Chao HC, Lai JY, Ming YC (2024) The trends of pediatric duodenal ulcer and predictors of recurrence. Journal of the Formosan Medical Association 123(10): 1070-1077.
- Zheng S, Zheng C, Cai S, Ge Xiaoyu, Chen Y (2025) Prediction of duodenal ulcers in children with Helicobacter pylori infection. Translational Pediatrics 14(11): 2968-2980.
- Perri F, Pastore M, Clemente R, Festa V, Quitadamo M (1998) Helicobacter pylori infection may undergo spontaneous eradication in children: A 2-year follow-up study. J. Pediatr. Gastroenterol. Nutr 27: 181-183.
- Vanzanten SV (2021) Knowledge Translation Action is Needed to Address Problems in Adherence to Pediatric Helicobacter Consensus Guidelines in Clinical Practice. J. Pediatr. Gastroenterol. Nutr 73: 138-139.
- Lai HH, Lai MW (2022) Treatment of Pediatric Helicobacter pylori Infection. Antibiotics 11: 757.






























