Undifferentiated Embryonal Sarcoma of the Liver: A Case Report and Review of the Literature
Pineda-Garcés Catalina1*, Romero-Moreno Katherine2, Muñoz-Rayo Luis3, Fox-Quintana Javier4, Gutiérrez-Montoya Jorge5
1Physician, specialist in General and Hepatobiliary Surgery, Hospital Universitario San Vicente Fundación, Medellín, Colombia
2Physician, resident in General Surgery, Universidad de Antioquia, Medellin, Colombia
3Physician, resident of Pathology, Universidad de Antioquia, Medellin, Colombia
4Physician, specialist in Pediatric Oncology, Hospital Universitario San Vicente Fundación, Medellín, Colombia
5Physician, specialist in General Surgery and Transplant Surgery, Hospital Universitario San Vicente Fundación, Medellín, Colombia
Submission:July 15, 2023; Published:July 28, 2023
*Corresponding author: Catalina Pineda-Garcés, Physician, specialist in General and Hepatobiliary Surgery, Hospital Universitario San Vicente Fundación, Medellín, Street 64 # 51D-154, Medellin, Colombia, Email: diana.pineda@sanvicentefundacion.com
How to cite this article: Pineda-Garcés C, Romero-Moreno K, Muñoz-Rayo L, Fox-Quintana J, Gutiérrez-Montoya J. Undifferentiated Embryonal Sarcoma of the Liver: A Case Report and Review of the Literature. Adv Res Gastroentero Hepatol, 2023; 19(5): 556024. DOI: 10.19080/ARGH.2023.19.556024.
Abstract
Sarcomas represent less than 1% of all malignant tumors. Undifferentiated Embryonal Sarcoma (UES) of the liver is the third most common pediatric liver cancer. The main differential diagnoses are mesenchymal hamartoma, hepatoblastoma, and biliary embryonal rhabdomyosarcoma. Definitive diagnosis is confirmed by histopathology and immunohistochemical. 4-year-old male patient with fever, abdominal pain and palpable hepatomegaly was found. Magnetic Resonance Imaging (MRI) with an unifocal cystic hepatic mass, with compression and displacement of vascular structures, but without invasion; hamartoma was suspected. The management was a right hepatectomy. Immunohistochemistry studies were positive for UES. Adjuvant chemotherapy was started with a good response.
Keywords: Liver neoplasms; Sarcoma; Hamartoma; Surgical oncology; Pediatric
Abbreviations: UES: Undifferentiated Embryonal Sarcoma; MRI: Magnetic Resonance Imaging; ALT: Alanine Aminotransferase; AST: Aspartate Aminotransferase; US: Ultrasound; CT: Computed Tomography
Introduction
Sarcomas are malignant tumors of skeletal and extraskeletal connective tissue that can arise from mesenchymal tissue at anybody site. In the United States, represent less than 1% of all newly diagnosed malignant tumors [1]. Was first described as a mesenchymoma by Donovan and Santulli in 1946 and was subsequently termed malignant mesenchymoma by Stout in 1948 before being first recognized as a distinct form of sarcoma by Stocker and Ishak in 1978 [2].
Undifferentiated Embryonal Sarcoma (UES) of the liver is a very rare sarcoma, and is considered the malignant counterpart of the hamartoma, share the same cytogenetic abnormality, and they are often considered to be the entities of the same spectrum of diseases [3]. That occurs mainly in children between 5 and 12 years old, with equal gender distribution [4-6]. After hepatoblastoma and hepatocellular carcinoma, UES is the third most common pediatric liver cancer, accounting for approximately 9 to 13 percent of all cases. There are no known risk factors associated [7,8]. Extrahepatic disease has a prevalence of approximately 20% [16], has been observed in organs such as the lung (8.3%), diaphragm (5.8%), heart (3.3%) and peritoneum (2.5%) [9].
Commonly arises from the right lobe of liver (62.7%) and is presented as solitary lesions (90.5%); as a result, patients can present with an abdominal mass, with or without abdominal pain [9]. Other symptoms include fever, weight loss, anorexia, vomiting, fatigue, constipation and respiratory distress [1,4,6]. There are reports of spontaneous tumor rupture as a result of rapid growth [8]. Liver function tests are usually normal, although slightly elevated alanine aminotransferase (ALT) or aspartate aminotransferase (AST) levels may be seen. Rarely, increased levels of alpha-fetoprotein and CA-125 have been documented [6].
Imaging studies such as ultrasound (US), computed tomography (CT) and magnetic resonance imaging (MRI) of abdomen can provide useful information about UES. US shows a heterogeneous solid tumor that is predominantly hyperechoic [6]. In CT the tumor is seen as a large, well-circumscribed, lobulated mass with notches and peripheral solid and central cystic areas [8]. MRI is the study of choice; in T2 images, the cystic components are very hyperintense, while in T1 images, the tumor appears as a hypointense mass, with hyperintense spots suggestive of intratumoral hemorrhage [8,10].
Macroscopically, masses are typically large (diameter between 14-21cm), of rapid growth, heterogeneous aspect due to the development of central necrosis and cystic degeneration [5,8] and well circumscribed by a pseudocapsule resulting from compressed hepatic tissue [4,10]. Microscopic evaluation shows clusters of hepatocytes in cords within the pseudocapsule and at the peripheral margin of the tumor. Solid component consists of spindle or stellate cells with inconspicuous nucleoli and poorly defined cell borders. Among the sarcomatoid cells, multinucleated cells with irregular morphology and hyperchromatic nuclei are usually observed. Eosinophilic globules are present in the cytoplasm of the tumor cells and in the extracellular matrix [4,10]. The resemblance to mesenchymal hamartoma suggests that UES is its malignant counterpart [11]. In immunohistochemistry, there is no specific immunophenotype; but vimentin, α1 antitrypsin and α-antichymotrypsin have been the most consistent markers [11].
The differential diagnosis of UES is not easy. The main differential diagnoses are mesenchymal hamartoma, hepatoblastoma, and biliary embryonal rhabdomyosarcoma [6]. Definitive diagnosis is confirmed by histopathology with hematoxylin-eosin staining and immunohistochemical analysis positive for CD56, CD68, vimentin and desmin.
Clinical behavior of this tumor is aggressive. In initial reports of the disease, most children affected died within 12 months of diagnosis from tumor progression or local recurrence, abdomen and/or pulmonary and peritoneal metastases [12]. In a review of patients treated between 1950 and 1988, it was noted that only 37% of patients survived [8]. The combination of surgery and chemotherapy has improved the results, increasing five-year survival from 40% in the 1980s to 70% today [6,13], and it has become the treatment of choice [6].
Case Report
A 4-year-old male patient, previously healthy and with no significant family history. He was admitted to a primary care hospital for two weeks of fever and abdominal pain. In the evaluation with finding of hepatomegaly 5 cm below the right costal margin without other alterations. US with report of enlarged liver due to heterogeneous mass in segment V and VI, so he was referred to a hospital of higher complexity. Laboratory studies revealed no signs of cholestasis, and the serum AFP level was negative. MRI (Figure 1) was performed with evidence of predominantly cystic unifocal hepatic mass and posterior wall enhancement with contrast administration, involving the segments V and VIII, generating compression and displacement of the vascular structures (hepatic venous and portal system), but without invasion. Also, slight compression and displacement of the gallbladder and the bile duct without dilation. No extrahepatic disease, free fluid, or lymphadenopathy. A hamartoma is considered the first diagnostic possibility.

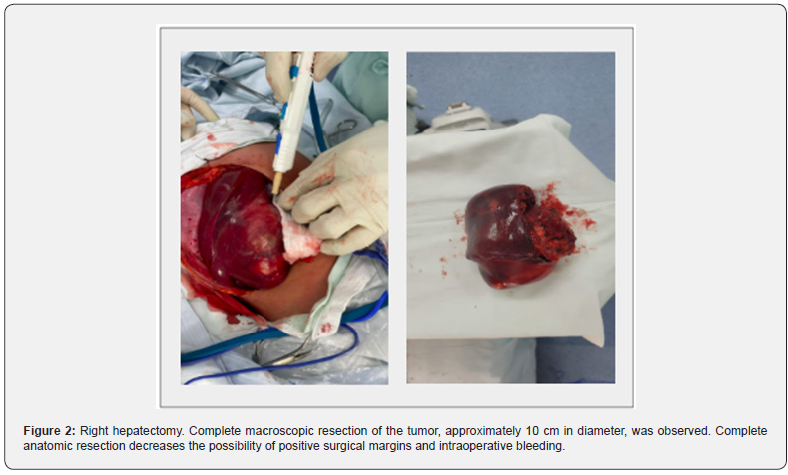
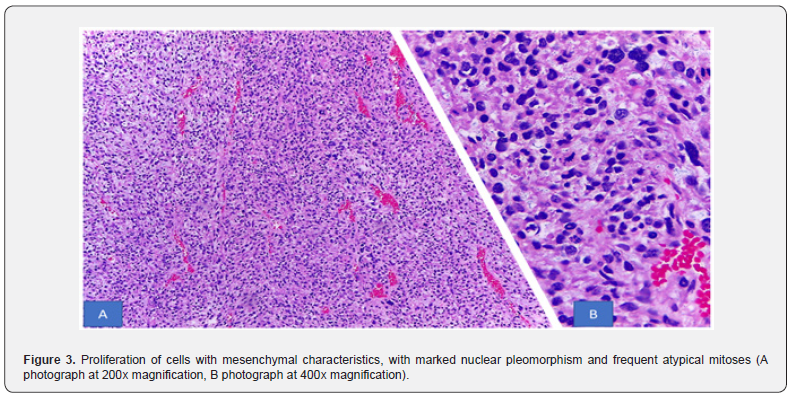
Due to the size of the lesion, the case was discussed in an interdisciplinary meeting, where surgical management was defined. A right hepatectomy was performed (Figure 2), without complications and with adequate postoperative recovery. In the anatomopathological study (Figure 3) heterogeneous tumor was found of 12 x 11.5 x 7.8 cm, with soft consistency, cystic areas, solid and hemorrhagic content. On microscopic evaluation with evidence of myxoid stroma with cells with clear basophilic cytoplasm, irregular hyperchromatic nuclei and frequent atypical mitoses. There was no involvement of the tumor resection margins or lymphovascular invasion. Immunohistochemical studies showed positivity for synaptophysin, chromogranin, CD56, NSE, and Glypican-3; and negativity for the markers cytokeratin cocktail, myogenin, WT1, arginase and CD99.
Adjuvant chemotherapy with vincristine, actinomycin-D, and cyclophosphamide was started. In the follow-up carried out (six months) there were no signs of recurrence.
Discussion
UES of the liver is a rare tumor, predominantly of the pediatric age. Patients often present with very large tumors or tumors adjacent to critical vascular structures that are unresectable. It has an aggressive clinical behavior and maybe fatal be fatal due to extensive enlargement of the upper abdomen with secondary involvement of the other organs [8], however is potentially treatable with multimodality therapy including chemotherapy, surgery, radiation, and in select cases, orthotopic liver transplantation [14].
Negative resection margin, tumor size less than 15 cm, and combination therapy (surgery and chemotherapy) are independent prognostic factors [6]. If R0 resection does not seem possible, neoadjuvant chemotherapy can be started with regimens based on non-rhabdomyosarcoma soft tissue sarcoma-type protocols. An initial prospective series of the Italian and German Soft Tissue Sarcoma Cooperative Groups (1979-1996) reported results with a protocol consisting of surgery or biopsy followed by induction chemotherapy for four cycles. This was followed by revision surgery in an attempt to resect residual tumor, and further chemotherapy. In this series, 12 of 17 patients survived with complete remission [8].
Liver transplantation may be an alternative for technically unresectable disease after neoadjuvant chemotherapy, or if there is recurrence [6,16]. The treatment approach is dependent on the patient’s eligibility for surgical resection, and they should undergo multidisciplinary evaluation at a sarcoma center of excellence.
Conclusion
UES is a very rare tumor and difficult to correctly diagnose preoperatively. Prompt management with surgical resection and adjuvant chemotherapy in cases of resectable tumor or neoadjuvant chemotherapy in cases of unresectable or locally recurrent is of paramount importance to achieve long-term overall survival.
Ethical Considerations
The authors declare that data protection was reserved, the right to privacy was respected, and informed consent was signed. It was not necessary to obtain authorization from the institution’s ethics committee, since at no time did, they breach or violate the patient’s anonymity norms, although the subject was exposed to experimentation.
References
- Siegel RL, Miller KD, Fuchs HE, Jemal A (2022) Cancer statistics, 2022. CA Cancer J Clin 72(1): 7-33.
- Shu B, Gong Lei, Huang X, Cao L, Yan Z, Yang S (2020) Undifferentiated embryonal sarcoma of the liver in adults: Retrospective analysis of a case series and systematic review. Oncology Letters 20: 102.
- Zhang C, Jia CJ, Xu C, Sheng QJ, Dou XG, Ding Y (2020) Undifferentiated embryonal sarcoma of the liver: Clinical characteristics and outcomes. World J Clin Cases 8(20): 4763-4772.
- Putra J, Ornvold K (2015) Undifferentiated embryonal sarcoma of the liver: a concise review. Arch Pathol Lab Med 139(2): 269-273.
- Matsui O, Kobayashi S, Gabata T, Ueda K (2011) Hígado: masas hepáticas focales. TC y RM. Diagnóstico por imagen del cuerpo humano. España, Elsevier Health Sciences Spain, pp. 1501-1566.
- Andrews WA, Kane B, Hendrickson RJ (2021) Lesiones del hí Holcomb y Ashcraft. Cirugía pediátrica (séptima edición). España, Elsevier, pp. 1031-1065.
- Walther A, Geller J, Coots A, Towbin A, Nathan J, et al. (2014) Multimodal therapy including liver transplantation for hepatic undifferentiated embryonal sarcoma. Liver Transpl 20(2): 191-199.
- O`Hara SM (2017) The Pediatric Liver and Spleen. Diagnostic Ultrasound (5th Edition). Elsevier Health Sciences, Philadelphia, USA, pp. 1730-1774.
- Wu Z, Wei Y, Cai Z and Zhou Y (2020) Long-term survival outcomes of undifferentiated embryonal sarcoma of the liver: a pooled analysis of 308 patients. ANZ J Surg 90(9): 1615-1620.
- Fletcher, Christopher DM (2021) Diagnostic histopathology of tumors (5th Edn). Elsevier, pp. 2310.
- Leuschner I, Schmidt D, Harms D (1990) Undifferentiated sarcoma of the liver in childhood: morphology, flow cytometry, and literature review. Hum Pathol 21(1): 68-76.
- Stocker JT, Ishak KG (1978) Undifferentiated (embryonal) sarcoma of the liver: report of 31 cases. Cancer 42(1): 336-348.
- Martins-Filho SN, Putra J (2020) Hepatic mesenchymal hamartoma and undifferentiated embryonal sarcoma of the liver: a pathologic review. Hepat Oncol 7(2): HEP19.
- Babu BI, Bigam DL, Gilmour SM, Dajani KZ, Shapiro AMJ, et al. (2020) Liver Transplantation in Locally Unresectable, Undifferentiated Embryonal Cell Sarcoma. Transplant Direct 7(2): e654.
- He M, Cai JB, Lai C, Mao JQ, Xiong JN, et al. (2022) Neoadjuvant transcatheter arterial chemoembolization and systemic chemotherapy for the treatment of undifferentiated embryonal sarcoma of the liver in children. World J Clin Cases 10(19): 6437-6445.
- Bahador A, Forooghi M, Shahriarirad R, Geramizadeh B, Ataollahi M, et al. (2022) A largue undifferentiated sarcoma of the liver in a 13-year-old girl treated with anatomical resection: a case report and review of the literature. BMC Gastroenterol 22(1): 2.
- May LT, Wang M, Albano E, Garrington T, Dishop M, et al. (2012) Undifferentiated sarcoma of the liver: a single institution experience using a uniform treatment approach. J Pediatr Hematol Oncol 34(3): e114-116.
- Techavichit P, Masand PM, Himes RW, Abbas R, Goss JA, et al. (2016) Undifferentiated Embryonal Sarcoma of the Liver (UESL): A Single-Center Experience and Review of Literature. J Pediatr Hematol Oncol 38(4): 261-268.






























