QT Interval Prolongation in Patients with Liver Cirrhosis
Karki N*, K.C S, Thapa P, Sah M and Hamal AB
Department of Medicine, Liver Unit, Bir Hospital, Nepal
Submission:May 30, 2023; Published:June 16, 2023
*Corresponding author: Niyanta Karki DM (HEPATOLOGY), Department of Medicine, Liver Unit, Bir Hospital, Kathmandu, Nepal, Email: niyakb@gmail.com
How to cite this article: Karki N, K.C S, Thapa P, Sah M, Hamal AB. QT Interval Prolongation in Patients with Liver Cirrhosis. Adv Res Gastroentero Hepatol, 2023; 19(5): 556021. DOI: 10.19080/ARGH.2023.19.556021.
Abstract
Introduction: Cirrhotic cardiomyopathy which involves the loss of stress-related contractile reaction and/or delayed-type diastolic dysfunction along with electrophysiological abnormalities such as QT interval prolongation. QT interval prolongation is common, with a prevalence exceeding 60% in patients with advanced stage of cirrhosis. A prolonged Q-T interval in chronic liver disease could lead to ventricular arrhythmias and sudden death. In these cases, beta blockers and antiarrhythmics should be avoided or used with caution.
Objectives: To discern QT interval and its correlation with liver dysfunction assessed by Child Pugh and MELD scores in patients with liver cirrhosis.
Methods: It is a cross sectional study of diagnosed cirrhotic patients who came to Liver unit between May 2015 to May 2016. 105 consecutive patients fulfilling the inclusion criteria were enrolled. Resting pulse and B.P was recorded with calculation of MAP. Electrocardiography was done on every patient. Cardiac dysfunction was evaluated by 2D-echocardiography in all patients. QT interval was measured and corrected by applying Bazzet’s formula. Correlation of QT interval was done with severity of liver dysfunction as assessed by CTP and MELD scores.
Results: Of total patients, male to female ratio is 2.3:1 with mean age of 48.29 and 54.3% fell in the age group between 40-60 years. Prolonged QTc of >0.44 secs was noted in 79% of total patients mainly in Child Pugh C and MELD score >10.
Conclusion: QT interval prolongation is seen in more than half of the patients with liver cirrhosis and is directly correlated with liver dysfunction assessed by Child Pugh and MELD scores.
Keywords: Chronic liver disease; Cardiac dysfunction; MELD score; QTc; MAP; Cirrhotic cardiomyopathy
Introduction
Electrophysiologic changes reported in patients with cirrhosis irrespective of its etiology which may be due to dysfunctional transmembrane sodium and potassium channels. Moreover, a direct relationship between plasma noradrenalin levels and the corrected QT interval was also reported suggesting that enhanced adrenergic stimulation of myocardial cells may play a significant role in abnormal repolarization [1]. QT interval prolongation is common, with a prevalence exceeding 60% in patients with advanced stage of cirrhosis. Prolongation of the QT-interval (>0.44 s) is seen even with mild increments in portal pressure in subjects with cirrhosis and in noncirrhotic patients with portal hypertension, whereas a further increase has been described after TIPS insertion [2]. A prolonged Q-T interval in chronic liver disease could lead to ventricular arrhythmias and sudden death. In these cases, beta blockers and antiarrhythmics should be avoided or used with caution [1].
More than 50 years ago, it was noted that persons with alcohol-related cirrhosis had increased cardiac output, and it was attributed to either impaired thiamine utilization or the presence of an endogenous vasodilator [3]. Cardiac hypertrophy and cardiomyocyte edema in the absence of coronary artery disease, hypertension, or valvular heart disease were next described in an autopsy series of subjects with cirrhosis. [4]. The hyperdynamic circulation in cirrhosis is characterized by increased cardiac output and heart rate and decreased systemic vascular resistance (SVR) with low arterial blood pressure arises as a complication of portal hypertension [5]. In 2005, a working party of expert hepatologists and cardiologists met at the World Congress of Gastroenterology and proposed a working definition of cirrhotic cardiomyopathy which proposed that “cirrhotic cardiomyopathy is a form of chronic cardiac dysfunction in patients with cirrhosis, characterized by blunted contractile responsiveness to stress, and/or altered diastolic relaxation with electrophysiological abnormalities in the absence of other known cardiac disease” [6].
Diastolic dysfunction is the first manifestation of Cirrhotic cardiomyopathy and reflects the increased stiffness of the myocardial wall owing to myocardial hypertrophy, fibrosis, and subendothelial edema. The prevalence of diastolic dysfunction has been reported to range from 45% to 56% [7]. Suggesting that some element of diastolic dysfunction is present in most of the patients with cirrhosis, whereas systolic dysfunction present later and only manifests as a blunted increase in cardiac output and decrease contractility with exercise or pharmacological stress and may have an impact on the development of ascites and hepatorenal syndrome.
One of the most common electrophysiologic changes reported in patients with cirrhosis irrespective of its etiology is a QT interval prolongation detected by electrocardiography which may be due to dysfunctional transmembrane sodium and potassium channels. Moreover, a direct relationship between plasma noradrenalin levels and the corrected QT interval was also reported suggesting that enhanced adrenergic stimulation of myocardial cells may play a significant role in abnormal repolarization [8]. Prolongation of the QT-interval (>0.44 s) is seen even with mild increments in portal pressure in subjects with cirrhosis and in noncirrhotic patients with portal hypertension, whereas a further increase has been described after TIPS insertion [9]. QT prolongation correlates directly with the severity of the liver disease, as defined by the Child-Pugh score and MELD score.
Methods
A Hospital based cross sectional study was conducted from May 2015 to May 2016 for 1year period. Diagnosis of cirrhosis was based on clinical grounds i.e stigmata of Chronic liver disease, impaired liver function tests, presence of Esophageal/ Gastric/Ectopic varices on Upper Gastro endoscopy. Evidence of coarse parenchyma with features of portal hypertension on ultrasound abdomen and biopsy whenever required. Sample size was calculated by using N= (Za2) (P) (Q)/d2, Where N=required sample size, Za=Variate corresponding to desired reliability level (1.96 for 95% reliability), P=Estimated proportion in the population, Q=100-P (if P is in % i.e., 40%), d=Maximum tolerable error=10% of P. Thus, the minimum sample size of this study was 92.196.
Inclusion criteria
Cirrhotic patients with or without ascites.
Exclusion criteria
a) Evidence of cardiovascular disease (IHD, Rheumatic heart disease, congenital heart disease, arrhythmias), pulmonary disease like bronchial asthma, COPD,
b) Hypertension, Diabetes Mellitus, Thyroid disorder, Severe anemia (<6gm/dl),
c) Peripheral vascular disease,
d) Liver cirrhosis with Pregnancy,
e) Taking drugs (betablockers, amiodarone, nitrates and Anti/hypertension within 4weeks),
f) Any substance abuse, mental illness or conditions which would make it difficult for the potential participant to participate in the intervention.
Consecutive Cirrhotic patients after assessing the exclusion criteria were recruited for the study. Routine blood investigations were done to assess the liver dysfunction by Child Pugh and MELD scores. Cardiac dysfunction was evaluated by measuring resting pulse and blood pressure with calculation of mean arterial pressure, by electrocardiography and echocardiography. QT was measured and corrected by applying Bazzet’s formula and QT interval of more than 0.44 secs was considered to be prolonged and was correlated with type of cardiac dysfunction and severity of liver dysfunction.
ECHO was done (by Cardiologist with experience of doing echocardiography > 10 years) in all subjects despite of normal ECG to assess for systolic or diastolic dysfunction. EF < 50% was considered as systolic dysfunction and normal EF with E/A ratio < 1 was considered as diastolic dysfunction. Chi square test and student T-test was used to compare the results of various numerical parameters among the studied patients. ANOVA test was used to see the association of parameters with child Pugh scoring and MELD score. Logistic regression analysis (Pearson correlation coefficient) was performed for determining the degree of association between different parameters. All values was expressed as mean ±SD, a 95% confidence interval was taken and P values of <0.05 was considered to be statistically significant.
Results
The age of the patient enrolled in this study was from 24 years - 82 years with mean age being 48.29%. Maximum 54.3% fell in age group 40-60 years. 74(70.5%) cases were male, and 31(29.5%) cases were female at the ratio of 2.38:1. Predominant cause of cirrhosis was found to be alcohol (72.4%) followed by chronic hepatitis B, Chronic hepatitis B with alcohol, cryptogenic being 6.7% each, Chronic Hepatitis C with alcohol, Chronic Budd Chiari syndrome being 1.9% each and Chronic Hepatitis C, choledochal cyst being 1% each.
Correlation of Type of Cirrhosis with Pulse and MAP
Resting pulse in alcoholic cirrhosis group ranged from 60- 128 beats per minute (BPM) with mean 83.90 BPM whereas resting pulse in nonalcoholic cirrhosis group ranged from 68- 88BPM with mean 78BPM. Mean MAP in Alcoholic cirrhosis group was 86.32mmHg and in Non-Alcoholic cirrhosis group, it was 81.25mmHg. Both resting pulse and MAP were higher in alcoholic cirrhosis group (Table 1).

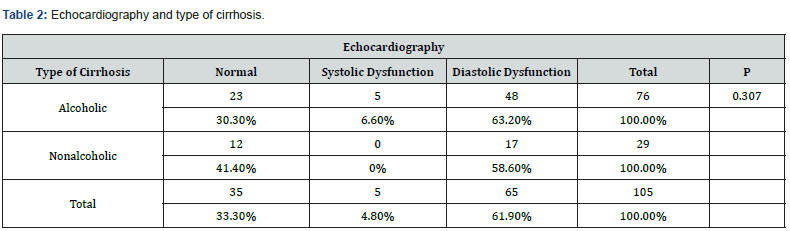
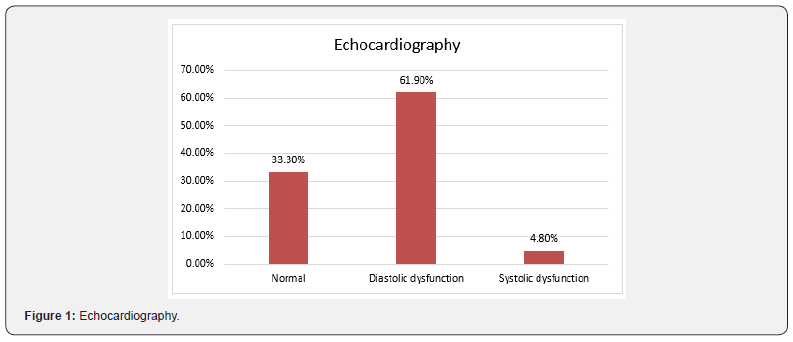
Echocardiography:
Diastolic dysfunction was seen in 61.9% of cases, systolic dysfunction in 4.8% of patients and normal echocardiography in 33.3% of cases (Figure 1). 6.6% of Systolic dysfunction and 63.2% of diastolic dysfunction was seen in total alcoholic patients whereas 58.6% of diastolic dysfunction and not a single case of systolic dysfunction was noted in nonalcoholic group (Table 2).
Cirrhotic Cardiomyopathy:
Among 105 enrolled patients, 51.4% had cirrhotic cardiomyopathy according to the criteria (proposed by WCGE in 2005) and 44.8% had cardiac findings other than cirrhotic cardiomyopathy and 3.8% had dilated cardiomyopathy (Figure 2).
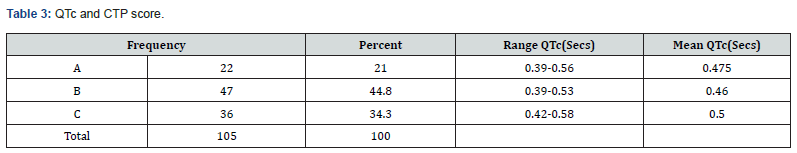
Among the total patients 44.8% fell in Child Pugh B group followed by 34.3% in C and 21% in A group. Prolonged QTc with mean of 0.5 seen in Child Pugh C group which was greater than seen in Child Pugh A (0.475) and Child Pugh B (0.46) (Figure 3 & Table 3).
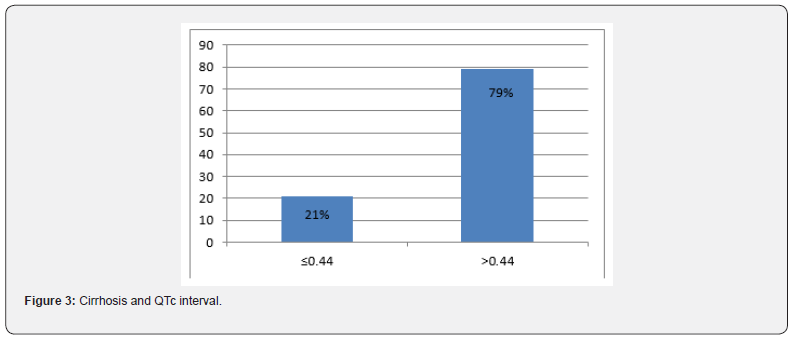
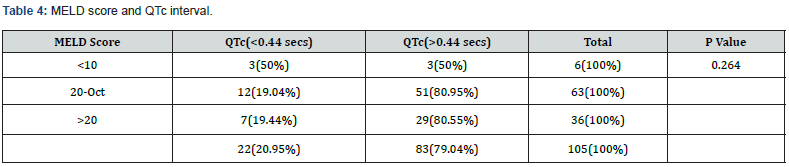
QTc was prolonged in79.04% of total cases. QTc was prolonged mostly in patients with MELD score >10, in group 10-20 about 80.95% 0f total 63 patients and in group >20, about 80.55% of 36 patients. So, the higher the MELD score, more chance of QTc to be prolonged (Table 4).

Discussion
Cirrhosis is more common in male group with male to female ratio of 2.38:1 with predominant cause being alcohol. This is in tune with high rate of alcoholism among males worldwide. Prolonged QTc of >0.44 secs was noted in 79% of total patients. Undefined factors related to the severity of cirrhosis, sympathoadrenergic hyperactivity may play a pathogenetic role [10] in the prolongation of QTc. Q-Tc was longer (>0.44 secs) in patients with cirrhosis with Child Pugh C and B or MELD >10 than in Child Pugh A regardless of the etiology of cirrhosis. So, QTc directly correlates with the severity of the liver dysfunction and may have an important prognostic meaning similarly shown in another study by Mimidis K et al. [11] that the QTc interval prolongation in cirrhotic patients refers to Child-Pugh B and C but is independent from the etiology of cirrhosis.
Acquired prolongation of the QTc interval has been documented in cirrhosis and it might be an important sign helpful to identify patients at risk of cirrhotic cardiomyopathy. Bhatti AB et al. [12] in their study also showed that the QTc interval was prolonged in 24.7% of cirrhotic patients with significant increase in frequency with worsening of Child Pugh Grade, thereby indicating an association between QTc prolongation and the severity of cirrhosis. There is limited data regarding the actual prevalence of cirrhotic cardiomyopathy due to the fact that the disease usually remains silent with near normal cardiac function unless the patients are exposed to stress [13].
The prevalence of cirrhotic cardiomyopathy is 50.4% in our study which is similar to the study done by Zardi EM et al. [14]. A study done by Dadhich S et al showed that cirrhotic patients with or without ascites has both morphological and functional cardiac dysfunction. Left ventricular diastolic dysfunction was present in 70% of cirrhotic patient with or without ascites which is similar to our study showing 61.9% of total cases irrespective with the presence of ascites and systolic dysfunction was seen in 4.6% of cases especially in alcoholic group with refractory ascites [15] and HRS similarly to study done by Dadhich et al. [16] where they showed that systolic dysfunction in cirrhotic patients is preserved in the absence of renal failure and refractory ascites. Systolic dysfunction, however, is mostly latent. Hyperdynamic unloaded heart failure is the main feature and cardiac output proves to be normal or increased at rest in most cases. Reduction in myocardial function becomes overt under conditions of pharmacological or physical stress.
Accordingly, clinical symptoms of systolic heart failure may evolve after liver transplantation or a Trans jugular Intrahepatic Portosystemic Shunt (TIPS) placement. Incidence of left ventricular diastolic dysfunction in medical-ward patients with no prior history of cardiovascular disease to that of the patients with hepatic cirrhosis caused by alcohol abuse was carried out by Brotanek J et al. [17]. which showed that the incidence of left ventricular diastolic dysfunction in patients with alcoholrelated liver cirrhosis, classified as Child-Pugh grade A and B, was significantly higher than in the controls without any prior liver disease which is also similar to our study.
Conclusion
QTc prolongation was the prominent feature seen in cirrhotic patients, especially in alcoholic groups. Resting pulse and MAP, the indicators of hyperdynamic circulation were slightly higher in alcoholic cirrhotic group than in other etiology. QTc prolongation correlated with liver dysfunction and was more prevalent in CTP-C and MELD score >10. QTc prolongation might be an early indicator of cardiac dysfunction especially cirrhotic cardiomyopathy in patients with liver cirrhosis and can play an important role to assess the severity of liver dysfunction.
References
- Aytemir K, Aksoyek S, Gurlek A, Oto A (1998) QT dispersion and autonomic nervous system function in patients with type 1 diabetes. Int J Cardiol 65(1): 45-50.
- Bernardi M, Calandra S, Colantoni A, Trevisani F, Raimondoet M L, et al. (1998) QT prolongation in cirrhosis: Prevalence, relationship with severity and etiology of the disease and possible pathogenetic factors. Hepatology 27(1): 28-34.
- Shorr E, Zweifach BW, Furchgott RF, Baez S (1951) Hepatorenal factors in circulating homeostasis. Circulation 3(1): 42-79.
- Gould L, Shariff M, Zahir M, Di Lieto M (1969) Cardiac haemodynamics in alcoholic patients with chronic liver disease and presystolic gallop. J clin Invest 48(5): 860-868.
- Samuel SL, Baik SK (2012)Complications of Cirrhosis. In: Boyer TD, Manns MP, Sanyal AJ, (Ets.), Textbook of Hepatology (6th), (Chapter 22), pp. 369-370.
- Møller S, Henriksen JH (2008) Cardiovascular complications of cirrhosis. Gut 5(2): 268-278.
- Pozzi M, Carugo S, Bolla GB, Pecci S de Ceglia V, Maggiolini S, et al. (1997) Evidence of functional andstructural cardiac abnormalities in cirrhotic patients with or without ascites. Hepatology 26(5): 1131-1137.
- Aytemir K, Aksoyek S, Gurlek A, Oto A (1998) QT dispersion and autonomic nervous system function in patients with type 1 diabetes. Int J Cardiol 65(1): 45-50.
- Bernardi M, Calandra S, Colantoni A, Trevisani F, Raimondo M L, et al. (1998) QT prolongation in cirrhosis: Prevalence, relationship with severity and etiology of the disease and possible pathogenetic factors. Hepatology 27(1): 28-34.
- Bernardi M, Calandra S, Colantoni A (1998) Q-T interval prolongation in cirrhosis: prevalence, relationship with severity, and etiology of the disease and possible pathogenetic factors. Hepatology 27(1): 28-34.
- Mimidis, Papadopoulos V, Thomopoulos K (2003) Prolongation of the QTc interval in patients with cirrhosis. Annals of Gastroenterology 6(2).
- Bhatti AB, Ali F, Satti SA (2014) Prolonged QTc Interval Is an Electrophysiological Hallmark of Cirrhotic Cardiomyopathy. Open Journal of Internal Medicine 4: 33-39.
- Rahman S, Mallett SV (2015) Cirrhotic cardiomyopathy: Implications for the perioperative management of liver transplant patients. World J Hepatol 7(3): 507-520.
- Zardi EM, Abbate A, Zardi DM (2010) Cirrhotic cardiomyopathy. J Am Coll Cardiol 56(7): 539-549.
- Dadhich S, Goswami A, Jain VK, Ankur Gahlot, Ganaraj Kulamarva, et al. (2014) Cardiac dysfunction in cirrhotic portal hypertension with or without ascites. Ann Gastroenterol 27(3): 244-249.
- Myers RP, Lee SS (2000) Cirrhotic cardiomyopathy and liver transplantation. Liver Transpl (4 Suppl 1): 44-52.
- Brotanek J, Ort M, Kubanek M, Stiborova M (2013) Alcoholic liver cirrhosis increases the risk of left ventricular diastolic dysfunction. Neuro Endocrinol Lett 34: 64-70.






























