Diagnostic Criteria for IgG4-Related Autoimmune Pancreatitis: HISORt
Marta Á lvarez-García1*, María Luque-Cabal2, Rocío Condori Bustillos1, María Rebeca de la Fuente-Olmos1 and Teresa Guerra-Garijo1*
1Rio Hortega University Hospital, Spain
2Vital Alvarez Buylla Hospital, Spain
Submission:May 5, 2023; Published:May 17, 2023
*Corresponding author: Marta Á Alvarez-García, 2nd Dulzaina St. Postal Code: 47012, Valladolid, Spain, Email: martaal94.ma@gmail.com
How to cite this article: Marta Á lvarez-G, María Luque-C, Rocío Condori B, María Rebeca de la Fuente-O, Teresa Guerra-G. Diagnostic Criteria for IgG4- Related Autoimmune Pancreatitis: HISORt. Adv Res Gastroentero Hepatol, 2023; 19(4): 556017. DOI: 10.19080/ARGH.2023.19.556017.
Abstract
Immunoglobulin G4 (IgG4) constitutes the least frequent immunoglobulin G (IgG) subclass. IgG4-related diseases (IgG4-rD) are considered a multisystemic pathology, characterized by tissue infiltration of IgG4+ plasma cells and lymphocytes. Pathophysiology is not well known, and its diagnosis is difficult, so it is underdiagnosed. Moreover, it can be confused with tumoral processes. Pancreas is the most frequently affected organ, constituting IgG4-related autoimmune pancreatitis (IgG4-rAIP). Specific criteria have been developed for its diagnosis, known as HISORt. Knowledge of this entity is important. Its first-line treatment is based on the use of corticosteroids, avoiding unnecessary surgical therapies.
Keywords: Immunoglobulin G4-related disease; Autoimmune pancreatitis; Diagnosis
Abbreviations: AIP: Autoimmune Pancreatitis; CT: Computed Tomography; IgG4-rAIP: IgG4-related Autoimmune Pancreatitis; IgG4-rD: IgG4-Related Disease; IgG: Immunoglobulin G; IgG4: Immunoglobulin G4; MRI: Magnetic Resonance Imaging
Introduction
Immunoglobulin G (IgG) is subdivided into four subclasses: G1, G2, G3 and G4. Immunoglobulin G4 (IgG4) constitutes 5% of healthy people. It is the least abundant and maintains stable serum levels in each person, but
has a high interindividual variability. Levels of 1-135 mg/dl are considered normal [1]. IgG4-related diseases (IgG4-rD) used to be considered as individual entities. Now they are known to conform a group of immune-mediated diseases, with similar clinical, serological and pathological features [2]. IgG4-related autoimmune pancreatitis [2]. It has received different names over time (IgG4-related sclerosing diseases, systemic IgG4 disease, IgG4-related autoimmune disease, systemic IgG4 plasmacytic syndrome…). A Japanese study group simplified and unified these terms into “IgG4-related diseases” [3]. The common feature is tissue infiltration of IgG4+ plasma cells and lymphocytes. Fibrosis could be associated and one or more organs may be involved. The most frequently affected organ is the pancreas. Therefore, pancreas is where this disease was described first. In 2001, Hamano et al. [4] described an elevated serum IgG4 concentration in patients with type 1 sclerosing pancreatitis. They also described pancreatic infiltration by IgG4+ plasma cells. However, not all patients have elevated plasma IgG4 levels [5].
Since its knowledge, multiple organ involvement has been described, including head and neck involvement (IgG4-related orbitopathy and dacryoadenitis, thyroiditis...), thoracic (pneumopathy, mediastinitis, mastitis...) and abdominal (sclerosing cholangitis, nephropathy, sclerosing mesenteritis...). Extrapancreatic manifestations can precede, coexist or appear later than autoimmune pancreatitis, so pancreatic involvement is not a necessary
criterion for diagnosis [5]. Pathophysiology is not completely known. Two main theories have been proposed: the autoimmune theory and the allergic theory. The autoimmune theory assumes that some individuals with certain HLA have a predisposition to over-activate IgG4 [6]. The allergic theory implicates Th2 and Treg lymphocytes in IgG4 activation. However, these theories still have unresolved questions [7]. Definitive diagnosis can be difficult, especially at the beginning of the disease. Due to its clinical and radiological features, it can be confused with other diseases, especially tumoral processes.
Histology may not provide the correct diagnosis in the absence of suspicion, as it requires specific tests [8]. IgG4-rD are often underdiagnosed and can be confused with other diseases (such as tumors, infections or other autoimmune diseases) [9]. Only a few cases have been associated with the development of malignant tumors: lymphomas and pancreatic cancer. However, the potential malignization of these entities is not completely determined [10] In the following review, we will focus on developing, within IgG4- rD, IgG4-related autoimmune pancreatitis (IgG4-rAIP), with the most recent updates on suspicion and diagnosis of this entity.
Discussion
IgG4-related autoimmune pancreatitis (IgG4-rAIP)
IgG4-rAIP is chronic pancreatitis and, as its name suggests, its etiology is autoimmune. The most recent studies differentiate between two main types of AIP [11]:
a) Type 1 or lymphoplasmacytic sclerosing pancreatitis: it is part of the IgG4-rD spectrum. It is more frequent in older Asian males. Abdominal pain is rare. IgG and IgG4 are elevated in serum and autoantibodies are positive. It is associated with other IgG4- rD.
b) Type 2 or idiopathic duct-centric chronic pancreatitis: it isn’t an entity of IgG4-rD. Its clinical and histologic profiles are different. There is no elevation of IgG4 concentration in serum or positive autoantibodies. With in chronic pancreatitis, IgG4-rAIP prevalence is between 2-8%. It usually occurs in middle-aged and older men (95% of patients are over 45 years old) [12].
Diagnosis
For IgG4-rD diagnosis, several criteria have been developed by different study groups (Table 1). Specifically for IgG4-rAIP, Mayo Clinic criteria, known as HISORt criteria, have been generalized. These criteria combine histological (H = Histology), radiological (I = Imaging) and serological findings (S = Serology) with other organ involvement (O) and response to treatment (Rt) [8].
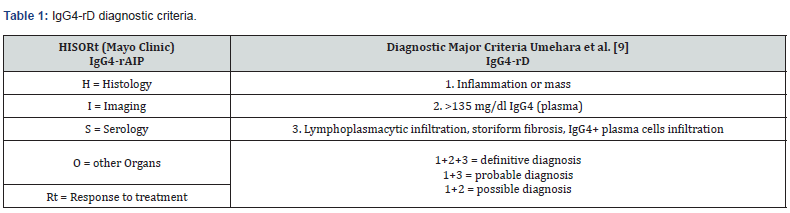
IgG4-rAIP: IgG4-Related Autoimmune Pancreatitis; IgG4-rD: IgG4-Related Disease; IgG4: Immunoglobulin G4
IgG4-related autoimmune pancreatitis [3]
Umehara et al. [9] have proposed three major criteria for the general IgG4-rD diagnosis:
a. Inflammation or mass in one or more organs, with focal or diffuse involvement.
b. Elevation of IgG4 concentration in plasma ≥135mg/dl.
c. Lymphoplasmacytic infiltration, fibrosis with storiform pattern (i.e., irregular, “cartwheel” pattern) and organ infiltration by IgG4+ plasma cells.
If all three criteria are present, the definitive diagnosis is done. If the first and last criteria are present, the diagnosis is probable. If only the first and second criteria are present, the diagnosis is possible. As it can be deduced, according to these criteria, the presence of inflammation or mass is a prerequisite [9]. Because of the clinical variability and ubiquity of this disease, the criteria cannot be applied to all patients. They may guide physicians in their diagnosis or, at least, their suspicion [12].
To make this review more didactic, we will develop the clinical features of IgG4-rAIP and following the different sections of HISORt criteria.
Clinical diagnosis
In general terms, IgG4-rD symptoms are mild. There is no fever or plasmatic elevation of acute phase reactants. It is usually diagnosed incidentally when inflammation of an organ is detected by imaging tests. Excellent response to steroid treatment is one of its main characteristics; although some patients may be refractory, needing more aggressive therapies [3]. IgG4-rAIP does not have typical symptomatology. Patients may remain asymptomatic for long periods of time. When symptoms occur, they may manifest as abdominal pain, obstructive jaundice, weight loss or new-onset diabetes mellitus. Unlike other pancreatic pathologies, symptoms are usually neither acute nor severe and acute pancreatitis is not a frequent manifestation. When associated with involvement of other organs, extra pancreatic symptoms may appear, which vary depending on the affected system [13].
Therefore, at the beginning, they can simulate a malignant pancreatic tumor. It has been shown that there are no differences between pancreatic adenocarcinoma and IgG4-rAIP symptoms [14]. Diagnosis is difficult due to overlapping findings with pancreatic adenocarcinoma. Between 3-5% of patients who undergo pancreatic resection for suspected pancreatic adenocarcinoma, IgG4-rAIP is demonstrated on definitive histological diagnosis [15].
Histological diagnosis
Histological findings are very characteristic, but they alone are not enough for definitive diagnosis. IgG4 immunohistochemical tests are needed. The presence of IgG4+ plasma cells must be demonstrated. They are not pathognomonic (they can be found in other inflammatory processes), but they are very specific. A high rate of infiltration by IgG4+ plasma cells increase the specificity for IgG4-rD (considering the cut-off point of 10-50
IgG4+ cells per high magnification field). It is useful the ratio of IgG4+ plasma cells/IgG+ plasma cells: if it is >40%, it is highly indicative of IgG4-rD6. IgG4-rAIP is histologically characterized by periductal infiltration of IgG4+ plasma cells. In advanced stages, periductal fibrosis is observed. Immunohistochemical studies show that most of the lymphocytes involved in the pathogenesis of this disease are of T lineage (CD4+ and CD8+) [16].
Radiological diagnosis
Those situations in which clinical and serological findings are not enough for a correct clinical suspicion, imaging tests play an essential diagnostic role [12].
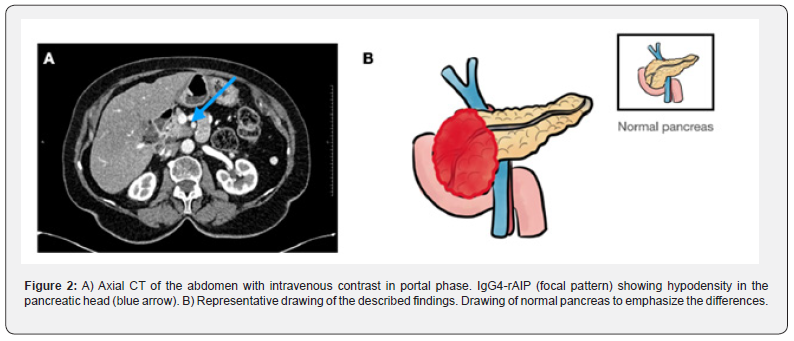
Two types of involvement have been described (Figures 1 & 2) [17]:
i. Diffuse: it is the most frequent. It is characterized by a uniform enlargement of the pancreas. The edges of the gland are smooth, losing lobulation and pancreatic clefts, giving a “sausage” appearance.
ii. IgG4-related autoimmune pancreatitis [4]
iii. Focal: pancreatic head is the most common localization, giving a pseudotumoral appearance. Its frequency varies between 33-41% of cases. This is the real diagnostic challenge.
iv. Main imaging tests that can be used are [12]:
v. Ultrasound, the affected pancreatic area appears hypoechoic.
vi. Computed tomography (CT), in which the affected area is hypodense.
vii. Magnetic resonance imaging (MRI), with a slight signal increase in T2-weighted sequences and low signal in T1-weighted sequences.
viii. Intravenous contrast studies may show delayed enhancement due to the presence of fibrosis [18].
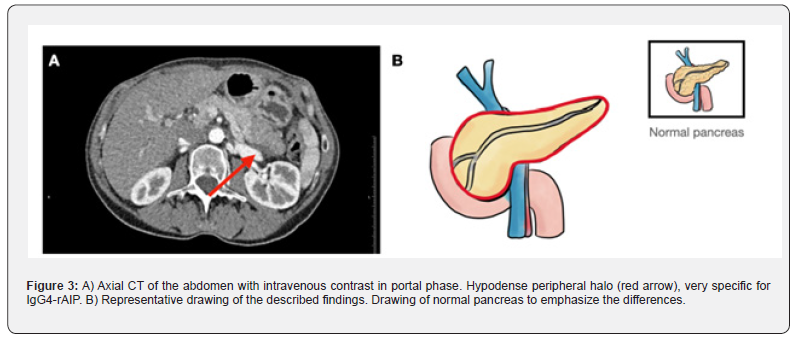
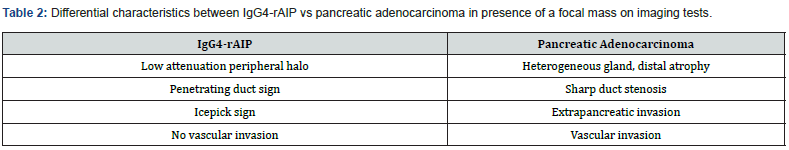
ix. The imaging findings that are indicative of IgG4-rAIP are (Table 2 & Figure 3) [19-21]:
x. Homogeneous pancreatic parenchyma enhancement. In long evolution cases, there may be associated volume loss secondary to atrophy and fibrosis.
xi. Peripancreatic low attenuation halo: described as one of the most specific findings.
xii. Alteration of the pancreatic ducts. Penetrating duct sign refers to the maintenance of the duct caliber when crossing the mass. The icepick sign refers to progressive duct narrowing distal to the lesion.
xiii. Absence of vascular invasion is a finding more suggestive of an inflammatory process, instead of a tumoral one.

IgG4-rAIP: IgG4-Related Autoimmune Pancreatitis
Cases of patients with concomitant IgG4-rAIP and pancreatic adenocarcinoma have been published, although
there is no scientific evidence to support a higher tumor risk in patients with IgG4-rD [22].
Serological diagnosis
Elevation of IgG4 in plasma is very common, but it is not a necessary criterion. It can be normal in 20-40% of individuals with histological IgG4-rAIP confirmation [10]. Relationship between elevated serum IgG4 levels and disease activity has been found. So, it can be used for onitoring, considering a cut-off point of 135 mg/ dl5. No significant differences have been demonstrated between the levels of tumor markers of pancreatic adenocarcinoma and IgG4-rAIP, such as carcinoembryonic antigen and CA19.9, because any pancreatic disease may increase them [14].

Modified from Á lvarez-García M et al. [12].
Involvement of other organs
As mentioned at the beginning of this review, IgG4-rD can affect different organs. These diseases can lead us to
suspect a concomitant pathology at other parts of the organism [2].
Head and neck involvement:
I. Salivary gland involvement (known as Mikulicz disease and Kü ttner’s tumor).
II. IgG4-related orbitopathy (dacryoadenitis and orbital pseudotumors).
III. IgG4-related thyroiditis (including Riedel thyroiditis and fibrous variant of Hashimoto thyroiditis).
IV. IgG4-related meningitis.
V. IgG4 pituitary involvement.
VI. Thoracic involvement:
VII. IgG4-related pulmonary and pleural involvement.
VIII. IgG4-related mediastinitis.
IX. IgG4-related cardiovascular involvement (including thoracic aorta and coronary arteries).
X. IgG4-related mastitis.
Abdominal involvement:
a. IgG4-related sclerosing cholangitis.
b. IgG4-related nephropathy (this is one of the main indicators of IgG4-rAIP: the presence of renal lesions in apatient with suspected autoimmune pancreatitis is highly indicative of IgG4-rAIP and not a pancreatic neoplasm).
c. IgG4-related retroperitoneal fibrosis.
d. IgG4-related sclerosing mesenteritis.
e. IgG4-related gastrointestinal involvement.
IgG4-related autoimmune pancreatitis [5]
a. IgG4-related prostatitis.
b. IgG4-related testicular pseudotumors.
c. Affection of the female genital system secondary to IgG4.
Other:
I. IgG4-related lymphadenopathy (very frequent in mediastinal, cervical and intra-abdominal regions). In 2019, the American College of Rheumatology (ACR) and the European Alliance of Associations for Rheumatology (EULAR) developed a set of inclusion and exclusion criteria for IgG4-rD. The primary criterion is based on typical organ involvement, including lacrimal glands, major salivary glands, orbits, lungs, paravertebral tissue, pancreas, bile ducts, kidneys, retroperitoneum, aorta, meninges and thyroid gland [23].
Response to Treatment
The treatment of IgG4-rAIP is based on oral corticosteroids, similar to the treatment of the rest of IgG4-rD. Although, the tendency is to relapse, because its etiology is autoimmune, the origin is not well-known and the
evolution tends to be chronic [1]. Prednisolone 30mg orally for 2-4 weeks is usually used as initial therapy. Repeat imaging is recommended 2 weeks after the beginning of therapy. In cases of absence of response, the diagnosis should be reconsidered, being very careful of a possible underlying cancer. In cases of relapse or resistance to corticosteroids, immunomodulators such as azathioprine or methotrexate can be associated [24]. Rituximab (an anti-CD20 monoclonal antibody) has shown good results in this pathology, but its use is not yet
approved. It can be employed in patients at high risk of relapse, those with multisystem involvement, in the first
relapse or in cases of failure of previous therapies [25].
Conclusion
IgG4-rAIP is one of the entities of the IgG4-rD spectrum, which are characterized by similar clinical, serology and pathological features. The pancreas is the main affected organ, although it is not the only one. Due to the difficulty in diagnosis, a series of criteria have been developed. For IgG4-rAIP, specific criteria have been published by Mayo Clinic, known as the HISORt criteria: histology, imaging, serology, involvement of other organs and response to treatment. The presence of inflammatory cells and fibrosis in the histological study makes differential diagnosis with other inflammatory and neoplastic processes necessary. It is important to recognize these diseases, since they usually respond to corticosteroid treatment, avoiding unnecessary therapeutic actions.
References
- Wallace ZS, Naden RP, Chari S, Choi HK, della-Torre E, et al. (2020) The 2019 American College of Rheumatology/European League Against Rheumatism classification criteria for IgG4-related disease. Ann Rheum Dis 72(1): 77-87.
- Martínez-de-Alegría A, Baleato-Gonzá lez S, García-Figueiras R, Bermú dez-Naveira A, Abdulkader-Nallib I, et al. (2015) IgG4-related disease from head to toe. Radiographics 35(7): 2007-2025.
- Hegade VS, Sheridan MB, Huggett MT (2019) Diagnosis and management of IgG4-related disease. Frontline Gastroenterol 10: 275-283.
- Hamano H, Kawa S, Horiuchi A, Unno H, Furuya N, et al. (2001) High serum IgG4 concentrations in patients with sclerosing pancreatitis. N Engl J Med 344: 732-738.
- Stone JH, Khosroshahi A, Deshpande V, Chan JK, Heathcote JG, Aalberse R, et al. (2012) Recommendations for the nomenclature of IgG4-related disease and its individual organ system manifestations. Arthritis Rheum 64(10): 3061-3067.
- Aalberse RC, Stapel SO, Schuurman J, Rispens T (2009) Immunoglobulin G4: An odd antibody. Clin Exp Allergy 39(4): 469-477.
- Cheuk W, Chan JK (2010) IgG4-related sclerosing disease: A critical appraisal of an evolving clinicopathologic entity. Adv Anat Pathol 17(5): 303-332.
- Hubers L, Maillette de Buy L, Doorenspleet M, Klarenbeek P, Verheji J, et al. (2015) IgG4-associated cholangitis: A comprehensive review. Clin Rev Allergy Immunol 48(2-3): 198-206.
- Umehara H, Okazaki K, Masaki Y, Kawano M, Yamamoto M, et al. (2012) Comprehensive diagnostic criteria for IgG4-related disease (IgG4-RD). Mod Rheumatol 22(1): 21-30.
- Sánchez-Oro R, Alonso-Muñoz EM, Martí Romero L (2019) Review of IgG4-related disease. Gastroenterol Hepatol 42(10): 638-647.
- Nagpal SJS, Sharma A, Chari ST (2018) Autoimmune pancreatitis. Am J Gastroenterol 113(9): 1301.
- Á lvarez-García M, Á lvarez Torices JC, Díez Lié bana MJ, de la Fuente Olmos MR (2023) Manifestaciones toracoabdominales de las enfermedades relacionadas con la inmunoglobulina G4. Radiología 65(2): 165-175.
- Madhani K, Farrell JJ (2016) Autoimmune pancreatitis: An update on diagnosis and management. Gastroenterol Clin North Am 45(1): 29-43.
- Zen Y (2016) The pathology of IgG4-related disease in the bile duct and pancreas. Semin Liver Dis 36(3): 242-256.
- Khandelwal A, Inoue D, Takahashi N (2023) Autoimmune pancreatitis: An update. Abdom Radiol (NY) 45: 1359-1370.
- Gupta R, Neyaz A, Chougule A, Akita M, Zen Y, et al. (2019) Autoimmune pancreatitis type 2: Diagnostic utility of PD-L1 immunohistochemistry. Am J Surg Pathol 43(7): 898-906.
- Zhao YX, Lü H (2016) Autoimmune pancreatitis: Typing, diagnosis, and treatment. Zhongguo Yi Xue Ke Xue Yuan Xue Bao 38: 731-734.
- Suzuki K, Itoh S, Nagasaka T, Ogawa H, Ota T, Naganawa S (2010) CT findings in autoimmune pancreatitis: Assessment using multiphase contrast-enhanced multisection CT. Clin Radiol 65(9): 735-743.
- Wolske KM, Ponnatapura J, Kolokythas O, Burke LMB, Tappouni R, et al. (2019) Chronic pancreatitis or pancreatic tumor? A problem-solving approach. Radiographics 39: 1965-1982.
- Okazaki K, Uchida K (2018) Current perspectives on autoimmune pancreatitis, IgG4-related disease. Proc Jpn Acad Ser B Phys Biol Sci 94: 412-427.
- Dickerson LD, Farooq A, Bano F, Kleeff J, Baron R, Raraty M, et al. (2019) Differentiation of autoimmune pancreatitis from pancreatic cancer remains challenging. World J Surg 43: 1604-1611.
- Witkiewicz AK, Kennedy EP, Kennyon L, Yeo CJ, Hruban RH (2008) Synchronous autoimmune pancreatitis and infiltrating pancreatic ductal adenocarcinoma: Case report and review of the literature. Hum Pathol 39(10): 1548-1551.
- Katz G, Stone JH (2022) Clinical Perspectives on IgG4-Related Disease and Its Classification. Annu Rev Med 73: 545-562.
- Uchida K, Okazaki K (2022) Current status of type 1 (IgG4-related) autoimmune pancreatitis. J Gastroenterol 57(10): 695-708.
- Nista EC, De Lucia SS, Manilla V, Schepis T, Pellegrino A, et al. (2022) Autoimmune Pancreatitis: From Pathogenesis to Treatment. Int J Mol Sci 23(20): 12667.






























