Analysis of the Importance of Comorbidities with RNAGraft Survival in Liver Transplantation: Analysis of the Importance of Comorbidities with ANN
Begona Zalba Etayo1,4,5, Lucia Marin Araiz5, Sara Lorente Perez2,4,5, Pilar Palacios Gasos3,4,6, Ana Pascual Bielsa1,4,7, Nuria Sanchez Donoso1,7, Trinidad Serrano Howl1,4,5 and Juan José Araiz Burdio1,4,5,7*
1Intensive Care Unit, University Hospital Lozano Blesa, Spain
2Department of Gastroenterology, University Hospital Lozano Blesa, Spain
3Department of Surgery, University Hospital Lozano Blesa, Spain
4Health Research Institute of Aragon (IIS Aragon), Spain
5Department of Medicine, University of Zaragoza, Spain
6Department of Surgery, University of Zaragoza, Spain
7Transplant Procurement Management, University Hospital Lozano Blesa, Spain
Submission:June 16, 2022; Published:January 23, 2023
*Corresponding author:Juan José Araiz Burdio, Intensive Care Unit University Hospital Lozano Blesa Zaragoza, Spain
How to cite this article:Begona Zalba E, Lucia Marin A, Sara Lorente P, Pilar Palacios G, Ana Pascual B, et al. Analysis of the Importance of Comorbidities with RNA Graft Survival in Liver Transplantation: Analysis of the Importance of Comorbidities with ANN. Adv Res Gastroentero Hepatol, 2023; 19(2): 556008. DOI: 10.19080/ARGH.2023.19.556008.
Keywords: Liver transplantation; Age; Disease status; Comorbidities; Coronary heart disease; Pathologies; Portal vein thrombosis; HIV; Morbid obesity
Abbreviations: BDA: Big Data Analysis; ML: Machine Learning; ANN: Artificial Neural Networks; MLP: Multilayer Perceptron
Introduction
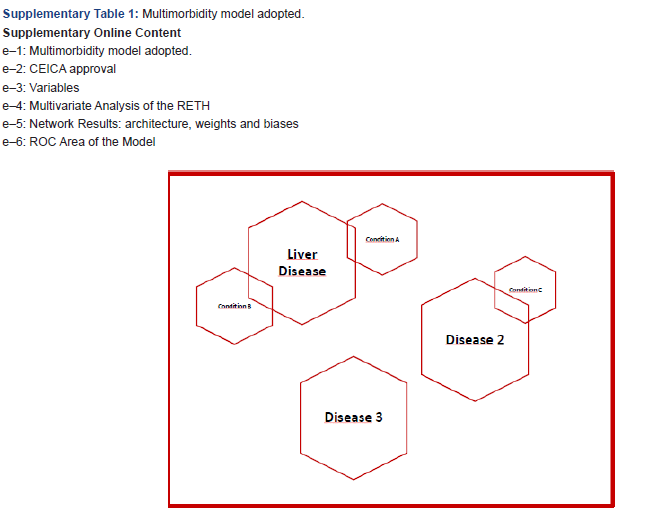
More than half of the patients with a liver transplant (OLT) will present at least one significant complication during the first year, therefore the criteria for assigning an organ must have an appropriate combination of benefit and utility, in which a very important role is played. important concept of “survival benefit” [1-2]. High complication rates may be the result of using organs from more limited donors (older age, donors in asystole, with expanded criteria, etc.) and/or receiver characteristics (age, disease status, comorbidities, etc.). Comorbidity is a medical term, coined by AR Feinstein in 1970, and subjected to several terminological proposals. Multimorbidity could be defined as the presence of different diseases or conditions that accompany a main chronic disease two (Supplemental Information e-1). In recent years, the indications for OLT have been expanded, in addition to increasing the age of the patients included in the list, and with this the presence of comorbidities is increasing [3]. There are studies that analyze the impact of a certain comorbidity on the results of liver transplantation: coronary heart disease [4-6] chronic kidney disease [7], diabetes [8], non-liver cancer [9]. Most of the indicators described to adjust donor-recipient allocation share some limitations: poor external validation when applied to populations other than those described [10,11] the statistical methodology of most of them is a logistic regression [12,13] and do not include recipient comorbidities. Medicine is an ideal field for the use of known techniques such as Big Data Analysis (BDA) and machine learning (ML), which may allow us in the future to improve our clinical research capacity and more accurately target the therapies we provide to our patients [14]. Artificial Neural Networks (ANN/ANN) thus constitute an alternative multivariate analysis method. The objective of this study is to analyze the predictive value of comorbidities in liver graft survival in the first year.
Materials and Methods
Data sources
The study was carried out from the data of all patients with a liver transplant (first transplant) performed at the Hospital Clinico Universitario Lozano Blesa (Aragón, Spain) from 2010 to 2021. The study has the Approval of the Research Ethics Committee of the Autonomous Community of Aragon (CEICA) (Act 1/2022) (Supplemental Information e-2).
Uhlig K, Leff B, Kent D, Dy S, Brunnhuber K, Burgers JS, et al. (2014) A framework for crafting clinical practice guidelines that are relevant to the care and management of people with multimorbidity. J Gen Intern Med 29(4): 670-679/

Variables and event
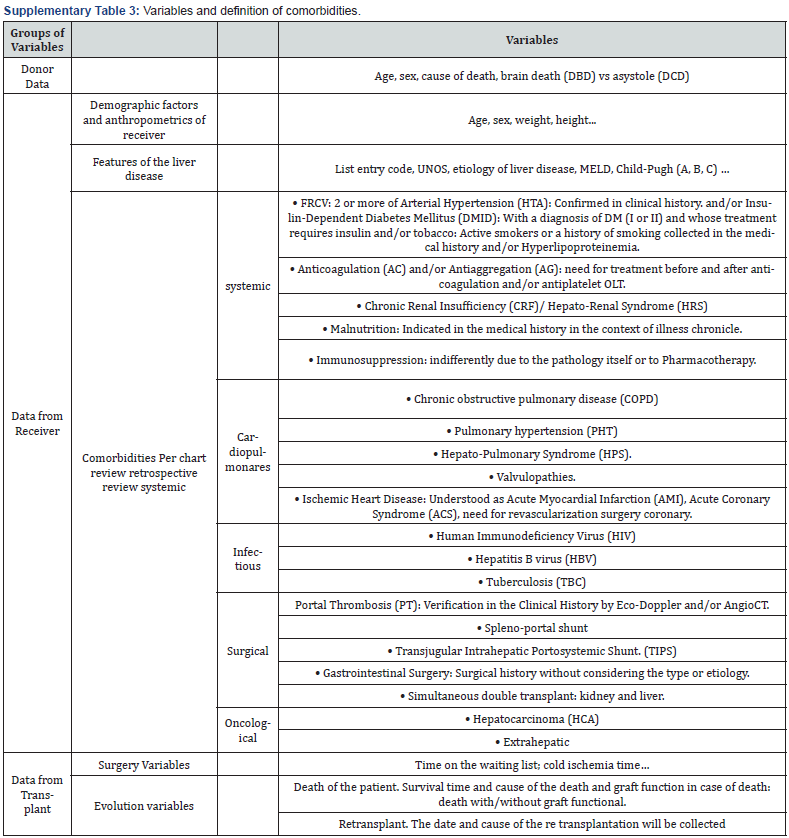
Thus, 3 large groups of variables were collected (Supplementary Information e-3): Donor Data: age, sex, cause of death, DBD, DCD; Receiver Data: Demographic and anthropometric factors of the recipient: Sex, age, weight, height...Characteristics of liver disease: code entry list, etiology of liver disease, MELD, Child- Pugh, comorbidities; Y Transplant Data: Surgery Variables: time on list Stand by; cold ischemia time Evolution variables: Death of the patient. Survival time and cause of death will be collected according to RETH categorization and graft function in case of death: death with/without a functioning graft; Re-transplantation. The Event object of study is defined as graft loss in the first year, either due to re-transplantation or death due to any cause with graft dysfunction.
They will be collected according to the categorization of the Spanish Liver Transplant Registry (RETH). http://www.ont.es/infesp/Paginas/Registro- Hepatico.aspx
Conventional statistics
For the quantitative variables, central tendency parameters will be obtained (arithmetic, geometric and harmonic mean, and mode), measures of dispersion (standard deviation, standard error, coefficient of variation, range, and variance) and measures of shape (Coefficient of kurtosis or flattening and coefficient of asymmetry). For qualitative variables, the frequency distribution will be calculated according to the categories (responses) existing in each of them. The following tests will be used in the hypothesis contrast: Pearson’s Chi-square derived from contingency tables for qualitative variables; Student’s “t” or Non-Parametric Test for quantitative variables, depending on their normal distribution.
Artificial neural network (ANN/ANN)
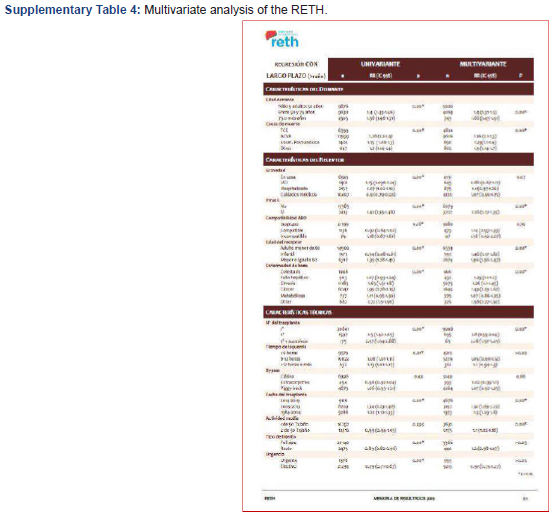
With the variables with statistical significance in graft survival described in the RETH based on data from 28,609 patients (Cox Analysis) fifteen (Supplementary Information e-4) and the comorbidities collected with a prevalence greater than 2%, a predictive model was created using an Artificial Neural Network (MLP: Multilayer Perceptron). In the exploratory ANN model, the data was randomly divided into a learning sample (70%) and a validation sample (30%). The hyperbolic tangent activation function was used in the hidden layer and SoftMax in the output layer. The learning parameters were Batches, Scaled Conjugate Gradient as algorithm, Initial Lambda 0.0000005, Initial Sigma 0.00005, Interval center 0.
Available at: http://www.ont.es/infesp/Paginas/RegistroHepatico.aspx
ANN sensitivity analysis
A sensitivity analysis, also known as an analysis of the importance of Variable (IV) to determine the optimal variables in the construction of the ANN model [16]. An IV value greater than 0.03 was considered clinically important (predictive): between 0.03-0.1 somewhat predictive and > 0.1 highly predictive.
Programs
For data treatment, the statistical package IBM® was used. - SPSS® -Statistics version 26.0. (©Copyright IBM Corporation 1989 to 2013, Chicago, IL, USA). For the design and validation of the Artificial Neural Network, the IBM® program will be used. -Neural Network version 25.0. A Wald p-value of p < 0.05 was considered significant.
Results
General description
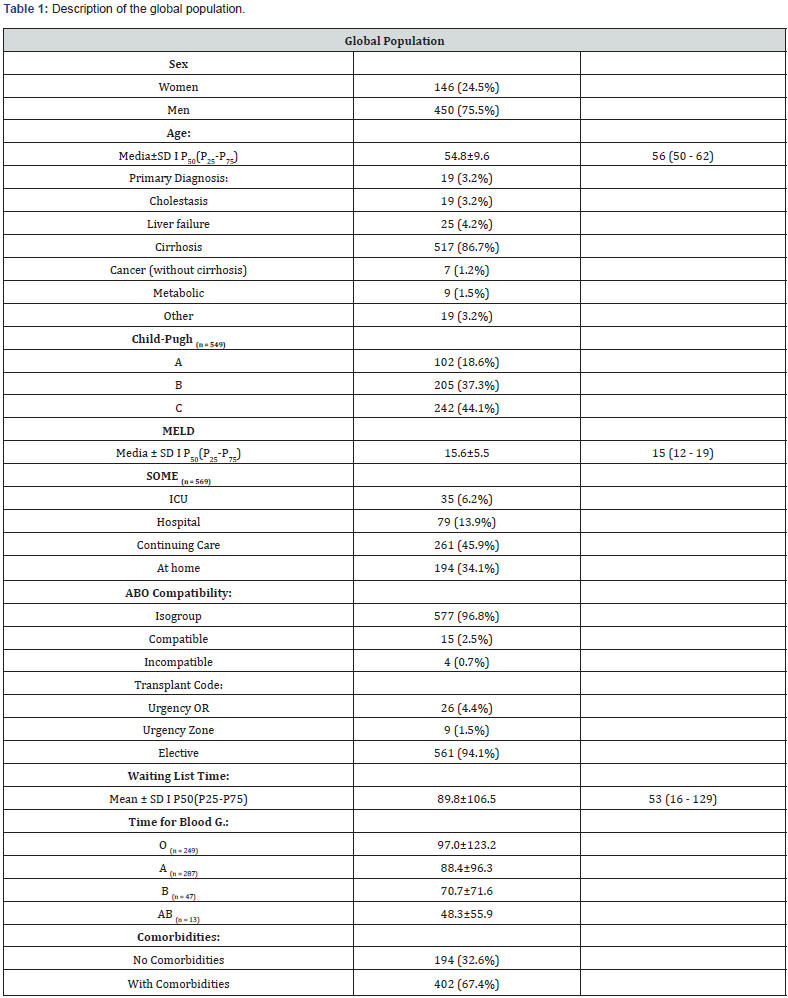
The general description of the studied series is shown in table 1. The majority were male (75.5%), the mean age of the patients was 54.8±9.6 years, the main cause of transplantation was cirrhosis (86.7%) and 67.4% of patients had some associated comorbidity.
UNOS: United Network for Organ Sharing.
Groups description
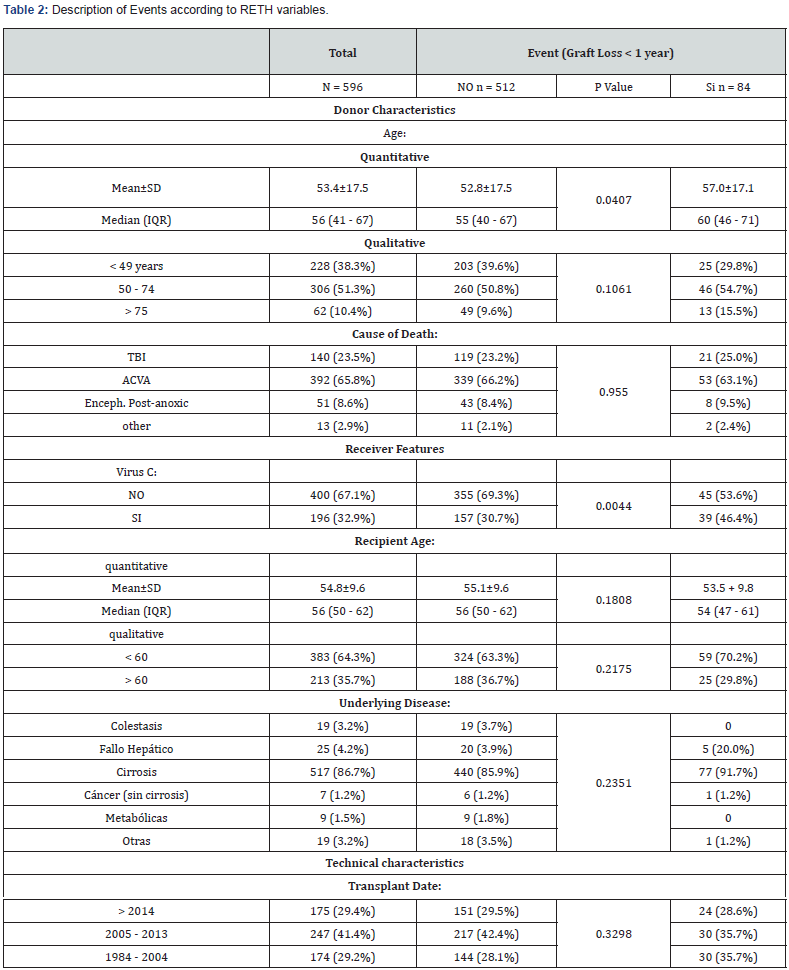
Graft loss due to transplantation or death with dysfunction occurred in 14% of cases. In table 2 These groups are described with respect to the variables that the RETH considers to be statistically significant. In our series, only the age of the donor (52.8±17.5 vs. 57.0±17.1, p<0.05) and liver disease caused by Virus C (30.7% vs. 46.4%, p<0.01) showed statistically significant differences between both groups.
Groups description: comorbidities
In Table 3a description of the two groups is shown in relation to the event with respect to all the comorbidities analyzed. Of all the comorbidities studied, they presented statistical. significance with respect to the appearance of the event: Taking antiaggregant and/or anticoagulants (4.5% vs. 11.9%, p<0.01) and portal vein thrombosis. (30.7% vs. 46.4%, p<0.01), both with a p<0.01.
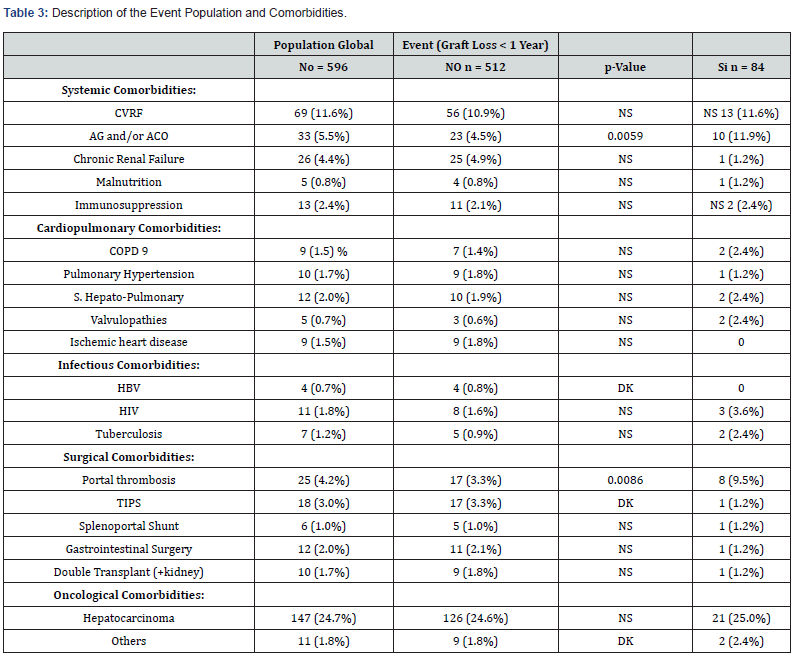
FRCV: 2 or more for hypertension, diabetes, tobacco, dyslipidemia); AG/ACO: Antiaggregants and/or Anticoagulants; COPD: Chronic Obstructive Pulmonary Disease; HBV: Hepatitis B Virus; HIV: Human Immunodeficiency Virus; TIPS: Transjugular Intrahepatic Portosystemic Shunt In bold, variables introduced in the ANN (prevalence >2% in both groups)
Artificial neural network: importance of variables
Based on the 6 variables recognized by the RETH as independent predictors of graft survival, and the 5 comorbidities in our series with a prevalence >2% in both groups; an RNA 11:8:2 was designed (Supplemental Information e-5).The sensitivity analysis of the variables included in the network calculated the parameter IV and normalized IV (IV n), the results of which are detailed in table 3. Almost all the variables showed a certain predictive capacity, the highest being the recipient’s age. (IV: 0.159; IVn: 100%) and the age of the donor (IV: 0.132; IVn: 83.1%), followed by 3 morbidities: taking antiaggregant and/or anticoagulants (IV:0.124; IVn: 78.4%), previous immunosuppression (IV: 0.110; IVn: 69.6%) and portal vein thrombosis (IV: 0.105; IVn: 66.3%). The presence of associated hepatocarcinoma did not show predictive value in graft survival (IV: 0.019; IVn: 11.8%).

Discussion
There are many indicators that aim to predict the probability of liver graft survival, however, when extrapolating them to populations other than where they were described (external validation) show poor results. In a recent meta-analysis published in 2021 [17] in Germany, a joint review of the prediction capacity of the DRI, ET-DRIYBA Ren compassing 12 items. The authors conclude that the AUC curves were low for all and did not discriminate well between graft loss and graft survival. The outcome of the transplant was mainly influenced by the age of the donor, the MELD, and the cause of the transplant relative to the recipient. Also in 2021, a retrospective cohort of 177 patients in Brazil is published [18]. In this study, the indices SOFT, BAR and DRI and the following conclusions were reached: SOFT, which includes receiver data among its variables, was the only one capable of offering an area under the curve > 0.7 (0.73), followed by the BAR index (0.69). It is concluded that the scores with data from both the recipient and the donor (SOFT and BAR) are more accurate in predicting graft survival.
One of the reasons that may justify the difficult extrapolation of these indicators to other populations is that they include few characteristics of the recipient. Analyzing previous studies, we can see how special relevance has been given to the existence of a high MELD value [19-21] or specific pathologies that could establish a contraindication twenty-one However, it is not so easy to find studies that analyze multimorbidity. Yes, there are some studies of comorbidities regarding the mortality of liver transplants. patients: Volk et al. [22] proposed a modified Charlson Index to predict mortality at 5 years; Cardoso et al. [23] found six variables related to 5-year mortality and Tovikkai et al. [24] In a study carried out in the United Kingdom, they observed that there are 4 factors related to the risk of mortality at 90 days: congestive heart failure, history of extrahepatic malignancy, cardiovascular disease, and chronic kidney disease (Table 4).
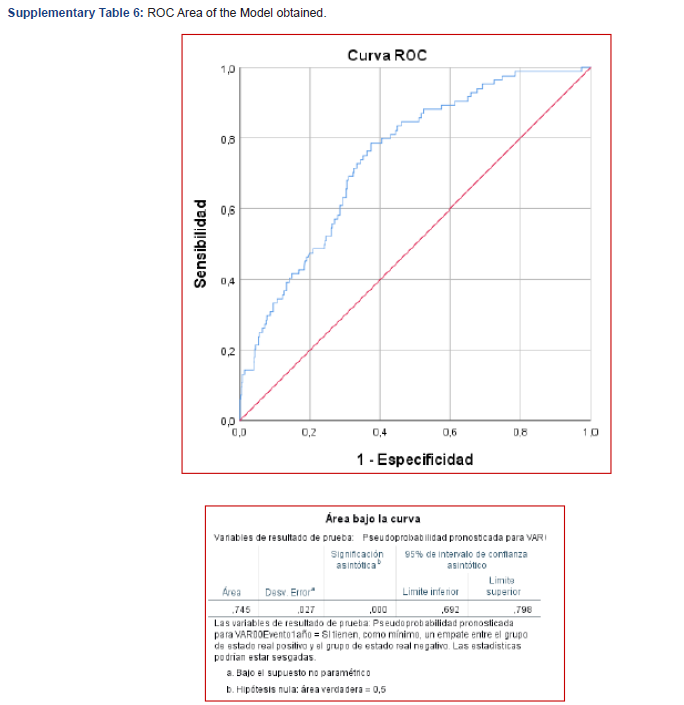
Only the presence of cardiovascular disease was a risk factor for mortality in all the periods studied (90 days, 1 year and 5 years). In our study, the way in which comorbidities can influence graft survival is assessed, introducing them into an ANN model with 6 independent factors related to it, based on a National Multicenter Registry (RETH) that includes more than 28,000 patients. Of the 11 variables analyzed, 10 turned out to have a certain predictive capacity, and 4 of them were comorbidities, in a model that showed a c-statistic of 0.745 (95% CI 0.692-0.798, asymptotic p < 0.001), greater than some of those indicated in other works (Supplemental Information e-6). ANNs can account for outliers and nonlinear interactions between variables and can reveal previously unrecognized or weak relationships between input variables and an outcome. Therefore, ANNs often include parameters that do not reach significance using conventional statistics, as observed in other studies [25.26].
In a University of Pennsylvania article published in 2020 [27]. A review is carried out on the criteria for selecting the recipient in liver transplantation. It exposes the importance of this selection not only including the main cause of hepatic morbidity, but also that some contraindications that were previously absolute are now relative and must be considered. Among these pathologies, portal vein thrombosis, HIV, morbid obesity... and others also analyzed in our study stand out. The authors stress that especially in some transplant candidate patients “older than 65 years”, it should be considered that they have a ‘favorable comorbidity profile’. The DACOLT project has recently been published (Danish Comorbidity Liver Transplant Recipient), a prospective study initiated in Denmark in 2021 [28]. This study also contemplates many of the comorbidities included in ours, however, it aims to analyze. the survival of the patient and not of the graft. One of its objectives is to determine the potential of all these comorbidity factors and to what extent they can be used to develop guidelines for detection, follow-up, and treatment in liver transplantation. Our studio has several limitations. First, data was collected retrospectively and from a single center, which may lead to population bias. Second, the population sample is small, which prevents having an acceptable prevalence of multimorbidity for both groups. Finally, the described sensitivity analysis is based on an ANN model that gave moderate network performance (c-statistic: 0.745;95%CI 0.692-0.798), although not very different from other models. In conclusion, in an ANN predictive model, together with consistent variables such as donor and recipient age, it would be important to introduce recipient comorbidities, some of which may be highly predictive clinical factors in liver graft survival in the first year.
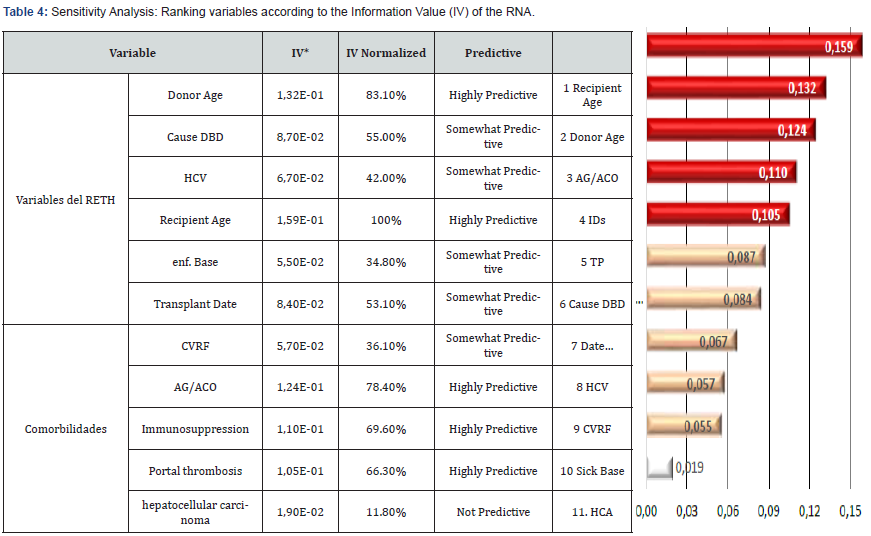
(*) ≤ 0.03 Not predictive; 0.03-0.1 Somewhat predictive; > 0.1 Highly predictive
DBD: Death Brain Donor; VHC: Virus Hepatitis C; FRCV: Factores Riesgo Cardiovascular; AG/ACO: Antiagregación y/o Anticoagulación
IV: Information Value
Acknowledgment
The authors want to show their gratitude to all those responsible for RETH. Conflict of interests the authors declare that they have no conflict of interest.
References
- Knight M, Barber K, Gimson A, Collett D, Neuberger J (2012) Implications of changing the minimal survival benefit in liver transplantation. Liver Transpl 18(5): 549-557.
- Bernabeu Wittel M, Alonso Coello P, Rico Blázquez M, Rotaeche del Campo R, Sánchez Gómez S, et al. (2014) Development of clinical practice guidelines for patients with comorbidity and multiple diseases. Aten Primaria 46(7): 385-392.
- Ravaioli M, Grande G, Gioia P, Cucchetti A, Cescon M, et al. (2016) Risk Avoidance and Liver Transplantation: A Single-center Experience in a National Network. Ann Surg 264(5): 778-786.
- D'Avola D, Cuervas-Mons V, Martí J, Ortiz de Urbina J, Yadó L, et al. (2017) Cardiovascular morbidity and mortality after liver transplantation: The protective role of mycophenolate mofetil. Liver Transpl 23(4): 498-509.
- Snipelisky DF, McRee C, Seeger k, Levy M, Saphiro BP (2015) Coronary Interventions before Liver Transplantation Might Not Avert Postoperative Cardiovascular Events. Tex Heart Inst J 42(5): 438-442.
- Skaro AI, Gallon LG, Lyuksemburg V, Jay Cl, Zhao L, et al. (2016) The impact of coronary artery disease on outcomes after liver transplantation. J Cardiovasc Med 17(12): 875-885.
- Nair S, Verma S, Tuluvath PJ (2002) Pretransplant renal function predicts survival in patients undergoing orthotopic liver transplantation. Hepatology 35(5): 1179-1185.
- Kuo HT, Lum E, Martin P, Bunnapradist S (2016) Effect of diabetes and acute rejection on liver transplant outcomes: An analysis of transplantation network/united network for organ sharing database. Liver Transpl 22(6): 796-804.
- Brattström C, Granath F, Edgren G, Smedby KE, Wilczek HE (2013) Overall and cause specific mortality in transplant recipients with a pretransplantation cáncer history. Transplantation 96(3): 297-305.a
- Audrey Winter, Cyrille Féray, Etienne Audureau, René Écochard, Christian Jacquelinet, et al. (2017) External validation of the Donor Risk Index and the Eurotransplant Donor Risk Index on the French liver transplantation registry. Liver Int 37(8): 1229-1238.
- Collett D, Friend PJ, Watson CJE (2017) Factors associated with short- and long-term liver graft survival in the United Kingdom: development of a UK Donor Liver Index. Transplantation 101(4): 786-792.
- S Feng, NP Goodrich, JL Bragg Gresham, DM Dykstra, JD Punch, et al. (2006) Characteristics associated with liver graft failure: the concept of a Donor Risk Index. Am J Transplant 6(4): 783-790.
- AE Braat, JJ Blok, H Putter, R Adam, AK Burroughs, et al. (2012) The Eurotransplant Donor Risk Index in Liver Transplantation: ETDRI. Am J Transpl 12(10): 2789-2796.
- Núñez A, Armengol MA y Sánchez M (2019) Big Data Analysis and Machine Learning in Intensive Care Units. Med Intensiva 43(7): 416-426.
- Memoria de Resultados del Registro Español de Trasplante Hepá
- Hong WD, Ji YF, Wang D, Chen TZ, Zhu QH (2011) Use of artificial neural network to predict esophageal varices in patients with HBV related cirrhosis. Hepat Mon 11(7): 544-547.
- Lozanovski VJ, Probst P, Arefidoust A, Ramouz A, Aminizadeh E, et al. (2021) Prognostic role of the Donor Risk Index, the Eurotransplant Donor Risk Index, and the Balance of Risk score on graft loss after liver transplantation. Transpl Int 34(5): 778-800.
- Torterolli F, Watanabe RK, Tabushi FI, Peixoto IL, Nassif Pan, et al. (2021) Bar, Soft and Dri posthepatic transplantation: what is the best for survival analysis? Arq Bras Cir Dig 34(1): e1576.
- Grat M, Wronka KM, Patkowski W, Stypulkowski J, Grat K, et al. (2016) Effects of Donor Age and Cold Ischemia on Liver Transplantation Outcomes According to the Severity of Recipient Status. Dig Dis Sci 61(2): 626-635.
- Schlegel A, Linecker M, Kron P, Györi G, De Oliveira ML, et al. (2017) Risk Assessment in Highand Low-MELD Liver Transplantation. Am J Transpl 17(4): 1050-1063.
- Schoening W, Helbig M, Buescher N, Andreou A, Schmitz V, et al. (2016) Eurotransplant donor-riskindex and recipient factors: influence on long-term outcome after liver transplantation - A large singlecenter experience. Clin Transplant 30(5): 508-517.
- Volk ML, Hernández JC, Lock AS, Marrero JA (2007) Modified Charlson comorbidity index for predicting survival after liver transplantation. Liver Transpl 13(11): 1515-1520.
- Cardoso FS, Bagshaw SM, Abraldes JG, Kneteman NM, Meeberg G, et al. (2015) Comorbidities have a limited impact on post-transplant survival in carefully selected cirrhotic patients: a population-based cohort study. Ann Hepatol 14(4): 505-514.
- Tovikkai C, Charman SC, Paseedom RK, Gimson AE, Van der Meulen (2015) Time-varying impact of comorbidities on mortality after liver transplantation: a national cohort study using linked clinical and administrative data. BMJ Open 5(5): e006971.
- Andersson B, Andersson R, Ohlsson M, Nilsson J (2011) Prediction of severe acute pancreatitis at admission to hospital using artificial neural networks. Pancreatology 11(3): 328-335.
- Hong W, Chen X, Jin S, Huang Q, Zhu Q, et al. (2013) Use of an artificial neural network to predict persistent organ failure in patients with acute pancreatitis. Clinics 68(1): 27-31.
- Mahmud N (2020) Selection for Liver Transplantation: Indications and Evaluation. Curr Hepatol Rep 19(3): 203-212.
- Thomsen MT, Hogh J, Knudsen AD, Jensen AMR, Gelpi M, et al. (2021) The Danish comorbidity in liver transplant recipients study (DACOLT): a non-interventional prospective observational cohort study. BMC Gastroenterol 21(1): 145-154.






























