Contribution of Colonoscopy in the Diagnosis of Chronic Diarrhea at the Digestive Endoscopy Centre of the General Hospital Idrissa Pouye
Mamadou Ngoné Guèye1, Caleb Ngreppe Mbetibanga1, Salamata Diallo2, Cheikh Ahmadou Bamba Cissé1, Marième Polèle Fall2, Gnagna Diouf1, Mame Aïssé Thioubou3, Marie Louise Bassène2, Daouda Dia1 and Mouhamadou Mbengue1
1Department of Hepato-gastroenterology, Idrissa Pouye General Hospital, Senegal
2Department of Hepato-gastroenterology, Aristide Ledantec Hospital, Senegal
3Department of Hepato-gastroenterology, Ziguinchor Peace Hospital, Senegal
Submission:January 03 2022; Published:January 20, 2022
*Corresponding author:Mamadou Ngoné Guèye, Department of Hepato-Gastroenterology, Idrissa Pouye General Hospital, Dakar, Senegal
How to cite this article: Gueye M N, Mbetibanga C N, Diallo S, Cissé C A B, Fall M P, et al. Contribution of Colonoscopy in the Diagnosis of Chronic Diarrhea at the Digestive Endoscopy Centre of the General Hospital Idrissa Pouye. Adv Res Gastroentero Hepatol, 2022; 18(3): 555986. DOI: 10.19080/ARGH.2022.18.555986.
Abstract
Introduction : Chronic diarrhea is a common clinical syndrome affecting about 5% of the world’s population. It has multiple etiologies. Ileo-colonoscopy plays a major role in the diagnostic process. The main objective of this work was to determine the contribution of colonoscopy in the exploration of chronic diarrhoea.
Material and Method : This was a retrospective study over a period of 6 years and 4 months (January 2015 to April 2021) at HOGIP. All colonoscopy reports performed for the exploration of chronic diarrhoea were collected. Data collection and analysis were performed with the Sphynx V5 software.
Results : One hundred and thirteen reports were analysed (9.62% of colonoscopies). The average age of the patients was 46 years (extremes 16 and 83 years). There was a predominance of women with a sex ratio of 0.95. All patients had chronic diarrhoea, which was bloody in 51% of cases. The colonic preparation was considered good in 87.6% of patients. The examination was well tolerated in 99 patients (87.6% of cases). The caecal floor was visualised in 101 patients (89.4% of cases). The last ileal loop was catheterised in only 13 cases (11.5% of cases). Colonoscopy was normal in 68 patients (60.2% of cases). In 32 patients (28.32%) inflammatory lesions were found and in 16 patients neoplastic lesions (14.15%).
Biopsies were performed in 110 patients (97.5% of cases) but only 77 (68.1%) biopsy results were found. Colonoscopy with pathological examination resulted in a diagnosis of microscopic colitis in 21 patients (18.6%), UC in 13 patients (11.5%), Crohn’s disease in 4 patients (3.5%) and colonic adenocarcinoma in 11 patients (9.7%). Normal colonoscopy with normal histology was observed in 11 patients (9.7%), with diarrhoea being a predominantly diarrhoeal functional disorder. In 17 patients (15.04%), endoscopy and histology were consistent with non-specific colitis, but no etiology could be determined.
Conclusion : The contribution of colonoscopy in the exploration of chronic diarrhoea remains considerable. This endoscopic examination enabled an etiological diagnosis to be made in more than 80% of the cases of chronic diarrhoea in our study. The diagnosis of microscopic colitis in about 1/5 of the patients demonstrates the importance of performing colonic biopsies even in the absence of macroscopic abnormalities in chronic diarrhoea.
Keywords: Ileocolonoscopy; Chronic diarrhoea; Colonoscopy; Pseudomembranous colitis
Introduction
Chronic diarrhoea is a common clinical syndrome affecting about 5% of the world’s population [1]. It is defined by WHO as changes in bowel transit lasting four weeks or more characterised by reduced stool consistency, increased daily evacuation frequency and daily stool weight > 300 g. Its aetiologies are multiple and varied, dominated by colonic and distal ileal causes [2]. Ileocolonoscopy plays a key role in the diagnosis and management of chronic diarrhoea. It is a fundamental endoscopic examination for the diagnosis of colonic diseases. It allows the exploration of the colonic mucosa and the taking of biopsies in pathological areas, and in certain situations, it has a therapeutic interest.
In Sub-Saharan Africa, in contrast to acute diarrhoea, overall data on chronic diarrhoea are very rare. In Senegal, to our knowledge, no published study has focused on chronic diarrhoea as a syndrome, hence the interest of this work whose aim was to determine the contribution of colonoscopy in the exploration of chronic diarrhoea.
Material and Methods
We conducted a retrospective study between January 2015 and April 2021 in the digestive endoscopy unit of the Internal Medicine and Hepato-gastroenterology Department of the Idrissa POUYE Hospital in Grand Yoff. All patients with chronic diarrhoea who had undergone colonoscopy and had complete reports were included.
a) Data were collected from the lower GI endoscopy registry.
b) Data collected were age, sex, indications for examination, level of exploration, tolerance and endoscopic findings. The pathological findings of the biopsies that were received were also collected.
c) The data were collected on a pre-established form. They were entered using the Sphinx software version 5.1.0.2. Data analysis was carried out with SPSS (Statistical package for Social Sciences) version 18.
Results
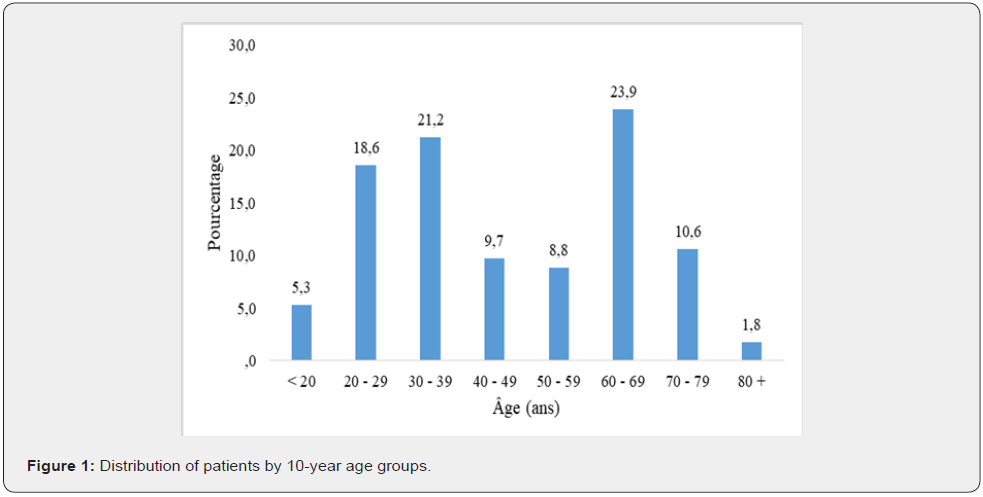
We collected 122 colonoscopy reports from patients with chronic diarrhoea of any age and sex out of a total number of 1174 colonoscopies performed during the study period, representing 10.4% of colonoscopies. Nine reports were excluded due to lack of gender, age and conclusion. The results presented are based on 113 patient reports. The mean age was 46 years with extremes of 16 and 83 years. The most common age range was 60-69 years (Figure 1). The sex ratio was 0.95 with a female predominance (58 women). All the patients had chronic diarrhoea, the majority of which was glairo-bloody (51% of cases), glairy (31.4% of cases) or liquid (17.6% of cases). This chronic diarrhoea was associated with AEG in 11.5% of cases, rectal discharge in 10.6% of cases, abdominal pain in 10.6% of cases, fever in 0.9% of cases and one case of vomiting (0.9%).
All colonoscopies were performed without sedation. The most commonly used product for colonic preparation was Polyethylene Glycol (PEG) or Fortrans, used in 109 patients or 96.5%, followed by Normacol used in 4 patients or 3.5%. The colonic preparation protocol used in all our patients was split-dose. Colonoscopy was complete in 101 patients (89.4%), in 12 patients the cecum could not be reached due to stenosis in 8 cases (66.7%) and poor tolerance in 4 cases (33.3%). The Boston score was specified in 55 patients (48.7%) and the mean score was 8. The colonic preparation was judged to be good in 87.6% of patients, average in 3.6% and poor in 8.8%. Colonoscopy was complete in 101 patients (89.4%). In 12 patients, the cecum could not be reached due to stenosis in 8 cases or 66.7% and poor tolerance in 4 cases or 33.3%. The last ileal loop was only catheterised in 13 cases (11.5%).
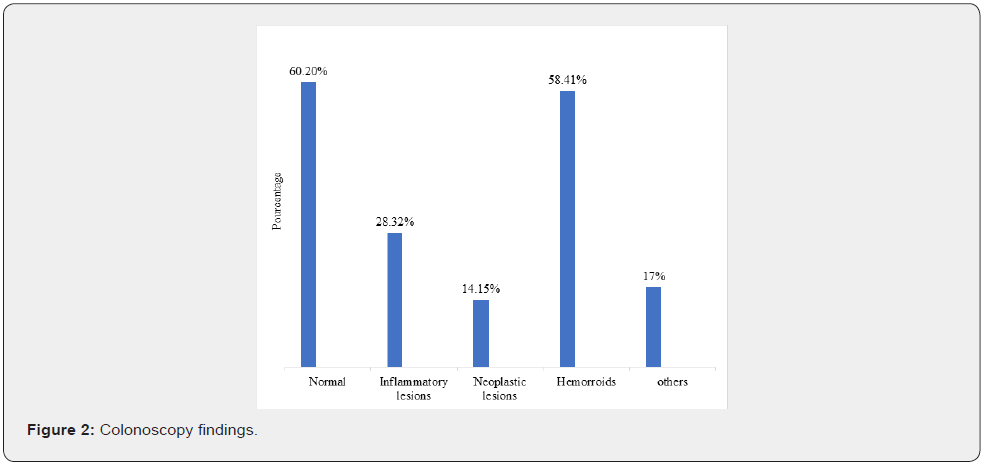
Colonoscopy was normal in 68 patients or 60.2% of cases (Figure 2). In 32 patients, inflammatory lesions were found. The extent of the lesions varied, with 23 (71.9%) extending beyond the left colonic angle. Most of the inflammatory lesions were erythematous, erosive and ulcerated. One case of pseudomembranous colitis was observed in a 64-year-old diabetic patient. In view of these inflammatory lesions, colonoscopy concluded that UC was probable in 25 cases (78.1%) and Crohn’s disease in 6 cases (18.6%). Neoplastic-like lesions were visualise in 16 patients. The rectum was the most frequent site (56.3%),followed by the ascending colon (25%), descending colon (12.5%), caecum (12.5%) and sigmoid colon in 6.25% of cases.The lesions were ulcerative in 10 cases (62.5%) and bulging in 5 cases (31.1%). They resulted in an impassable stenosis at colonoscopy in 8 cases (66.7%). It should be noted that 3 patients had both inflammatory and neoplastic lesions. Apart from inflammatory and neoplastic lesions, polyps were observed in 10 patients (8.8%) and diverticula in 9 patients (7.9 %). In addition, rectal retrovision revealed turgid internal hemorrhoids in 66 patients (58.41%).
Biopsies were performed in 110 patients, in 97.5% of cases, but only 77 biopsy results were found (68.1%).
Of the 68 patients who had a normal colonoscopy, pathological examination was normal in 11, or 9.7% of the total number. Microscopic colitis was reported in 21 patients or 18.6% of the total number. It was predominantly lymphocytic in 19 cases or 90.5% and collagenous in 2 cases or 9.5%. In the remaining 36 patients who had a normal colonoscopy (31.8%), the pathological examination showed a non-specific colitis and in 3.5% the pathological examination was normal.
For inflammatory lesions on colonoscopy, pathological findings were consistent with UC in 13 patients or 11.5% of cases, Crohn’s disease in 4 patients or 3.5% of cases and nonspecific colitis in 15 patients or 13.3% of cases.In patients with neoplastic lesions on colonoscopy, the histological findings were consistent with tubular adenocarcinoma in 11 patients, or 9.7% of the total number.In 5 cases, the pathological examination did not provide histological confirmation but rather indicated a nonspecific colitis, 4.4% of the total number of patients.The diagnosis retained after endoscopic and histological examinations was that of microscopic colitis in 21 patients (18.6%), IBD in 17 patients (15 %), with 13 UC (11.5%) and 4 Crohn’s disease (3.5%). The diagnosis of adenocarcinoma was retained in 11 patients or 9.7 %. Lesions suspected of neoplasia were not histologically confirmed in 5 cases. One case of pseudomembranous colitis was reported (0.9%). Eleven patients (9.7%) had normal endoscopy with normal histology, the diarrhoea was probably part of a functional bowel disorder with diarrhoea predominance. In 17 patients (15.04%), endoscopy and histology were consistent with nonspecific colitis, but no etiology could be determined.
Discussions
The mean age of the patients was 46 years, with extremes of 16 and 83 years. The most common age range was 60 to 69 years. Our results are comparable to the literature. Indeed, Ian et al. [3] in a 2002 study in Australia on routine biopsy in patients undergoing colonoscopy for chronic diarrhoea reported an average age of 45 years with extremes of 17 and 85 years. The same finding was reported in Morocco in 2006 in a study on the contribution of colonoscopy to chronic diarrhoea with a mean age of 45 years with extremes of 15 and 86 years [4]. The young average age found in patients with chronic diarrhoea could be explained by the frequency of functional intestinal disorders. Indeed, in several studies of IBS the average age was around 40 to 50 years [5,6]. Secondly, the incidence of IBD, which is constantly increasing, is more frequent in the young adult population. Indeed, it has been reported in Europe that the incidence increased by 30% from 1988 to 2008 with an average age of around 48 years with a female predominance in CD [7].
In our study, there was a female predominance with 58 women (51.3%) and a sex ratio of 0.95. Similar results have been reported in previous studies in Africa and the rest of the world. Indeed, Al- Bayatti et al [2] in a study conducted in Iraq in 2002 on the etiologies of chronic diarrhoea reported a female predominance with 62%. Similarly, in Morocco, El Hachhab [8] found a sex ratio of 0.93 in 2013 in a study on the contribution of colonoscopy in chronic diarrhoea. This female predominance could be explained by the frequency of functional intestinal disorders with a predominance of diarrhoea in women. Indeed, several studies have shown that functional intestinal disorders are 1.5 to 3 times more prevalent in women than in men [9,10]. Similarly, a systematic review of several studies conducted in 2012 on the global prevalence and risk factors of functional bowel disorders showed a significantly higher prevalence of functional bowel disorders in women than in men (sex ratio 1.67) [11]. Indeed, this female frequency is explained by female hypersensitivity with a particular hormonal status making her more vulnerable to functional bowel disorders [12].
Colonoscopy was normal in 60.2% of patients. This result was consistent with the literature. Indeed, Joon-Hyoek et al. [13], Marcella et al. [14], and Aourarh [4] reported respectively 71.1%, 72% and 54% normal colonoscopy. Normal colonoscopy is common in the investigation of chronic diarrhoea. These diarrhoeas are most often classified as functional diarrhoea according to the Rome IV classification.
Microscopic colitis is also a frequent cause of chronic diarrhoea with normal colonoscopy. Indeed, MCs, initially considered rare, have seen a marked and steady increase in incidence over the past 20 years, reaching a plateau more recently [15,16]. In our series, biopsies found 18.6% of microscopic colitis. Our results are similar to those of recent studies reported in Tunisia by Hasnaoui et al. [17] in 2018 and in Europe by Macaigne et al. [18] in 2009, which noted a prevalence of around 15%. This high rate of microscopic colitis underlines the importance of systematically performing biopsies, even in case of normal colonoscopy during the exploration of chronic diarrhoea. The combination of colonoscopy and biopsy led to a diagnosis of IBD in 15% of cases. This frequency is lower than those reported in the Maghreb and the West. Indeed, Al-Bayatti et al [2] reported 28% IBD in their study on the aetiologies of chronic diarrhoea in 2002; similarly, Aourarh [4] reported 22% IBD with 12.5% UC and 9.5% Crohn’s disease [19].
Neoplastic lesions on colonoscopy were histologically confirmed in 11 patients (9.7%), all in favour of adenocarcinoma. Similar results have been reported in the literature. Indeed, El Hachhab [8] reported malignancy in 5.5% of patients and three other series in the literature [2,4,20] reported proportions of 6%, 2.5% and 3% respectively. This rate of neoplastic lesions in our series can be explained by the existence of colorectal cancers which are most often revealed by chronic diarrhoea, especially in elderly subjects. In fact, chronic diarrhoea is a symptom common to several types of malignant tumours and is associated with colorectal cancers in 20% of cases. As a result, colorectal cancer should be suspected in cases of unexplained chronic diarrhoea, especially in the elderly [21,22]. In our series, 11 patients or 9.7% had normal endoscopy with normal histology. The diarrhoea was probably a predominantly diarrhoeal IFT. This is a diagnosis of elimination after ruling out other organic causes of chronic diarrhoea. Our study did not report any infectious causes, in particular parasitic or bacterial, even though we are in a tropical zone where infectious causes are quite frequent and most often linked to immunodepression. This could be explained by the fact that these infectious causes are more prominent during acute diarrhoea. However, cases of tuberculous ileitis have been reported in the literature.
Conclusion
a) The contribution of colonoscopy in the exploration of chronic diarrhoea remains considerable. This endoscopic examination enabled an etiological diagnosis to be made in more than 80% of the cases of chronic diarrhoea in our study. The diagnosis of microscopic colitis in about 1/5 of the patients demonstrates the importance of performing colonic biopsies even in the absence of macroscopic abnormalities in chronic diarrhoea.
References
- Camilleri M (2004) Chronic diarrhea: a review on pathophysiology and management for the clinical gastroenterologist. Clin Gastroenterol Hepatol 2(3): 198-206.
- Al Bayatti SM (2002) Etiology of chronic diarrhea. Saudi Med J 23(26): 675-679.
- Ian FY, Donald GO, Neville EH (2002) Routine colonic mucosal biopsy and iléoscopie increases diagnostic yield in patients undergoing colonoscopy for diarrhea. J Gastroenterol Hepatol 17(3): 276-80.
- Aourarh A (2006) Contribution of colonoscopy in the diagnostic orientation of chronic diarrhea. Thesis of medicine N° 186, Rabat.
- Dapoigny M, Dyard F, Grimaud JC, Guyot P, Van Ganse E (2003) Functional bowel disorders and health care consumption; observational study in private gastroenterology. Gastroenterol Clin et Biol 27(3): 265-71.
- Mayindza EEL, Itoudi BPE, Bourobou BJA, Boukandou MMM (2020) Epidemiological study of functional bowel disorders in health facilities in Libreville (Gabon). J Applied Biosciences 155: 15986-15991.
- Gower RC, Vasseur F, Fumery M, Savoye G, Salleron J, et al. (2013) Epidemiology of inflammatory bowel diseases : new insights from a French population-based registry (EPIMAD). Dig Liver Dis 45(2): 89-94.
- El Hachhab L (2013) The contribution of colonoscopy in chronic diarrhea (About 339 cases). Thesis of medicine No. 1261, Fez.
- Camengo PSM, Mbeko SM, Service G (2012) Functional bowel disorders in gastroenterology consultation at the Amitié University Hospital in Bangui. J Afr Hepato Gastroenterol 6: 107-111.
- Fernández BF, Esteve M, Alsina M, Farré C, González C, et al. (2007) Systematic evaluation of the causes of chronic watery diarrhea with functional characteristics. Am J Gastroenterol 102(11): 2520-2528.
- Lovell RM, Ford AC (2012) Global prevalence of and risk factors for irritable bowel syndrome : a meta-analysis. Clin Gastroenterol Hepatol 10(7): 712-721.
- Functional Bowel Disorders: A Woman's Issue.
- Joon HL, Poong LR, Jae JK, Kwang CK, Seung WP, et al. (1997) The role of mucosal biopsy in the diagnosis of chronic diarrhea: value of multiple biopsies when colonoscopic finding is normal or nonspecific. Kor J Inter Med 12(2): 182-187.
- Marcella M, Roger W, Perove S (2004) Colonoscopy and SeHCAT for investigation of chronic diarrhea. Digestion 69(4): 211-218.
- Gentile N, Khanna S, Loftus J, Smyrk TC, Tremaine WJ, et al. (2014) The epidemiology of microscopic colitis in Olmsted County from 2002 to 2010 : a population-based study. Clin Gastroenterol Hepatol 12(5): 838-842.
- Tong J, Zheng Q, Zhang C, Lo R, Shen J, et al. (2015) Incidence, prevalence and temporal trends of microscopic colitis : a systematic review and meta-analysis. Am J Gastroenterol 110(2): 265-276.
- Hasnaoui B, Mahmoudi M, Ouni A, Khsiba A, Medhioub M, et al. (2018) Microscopic colitis: About 27 cases. Rev Med Interne 39: 148-149.
- Macaigne G, Obratasova A, Locher C, Chayette C, Domenigoni X, et al. (2009) Etiology of microscopic colitis: results of a retrospective multicentre study in 64 patients. Gastroenterol Clin Biol 33(3): 309.
- Chouraki V, Dauchet L, Merle V, Dupas JL, Lerebours E, et al. (2008) Incidence of Crohn's disease and ulcerative colitis in northern France from 1988 to 2005: results of the EPIMAD register. RESP 1246(1005): 247-258.
- Otegbayo JA, Otegbeye FM, Rotimi O (2005) Microscopic colitis syndrome. J Natl Med Assoc 97(5): 678-682.
- Jervoise H, Andreyev N, Davidson SE, Gillespie C, Allum WH, et al. (2012) Practice guidance on the management of acute and chronic gastrointestinal problems arising as a result of treatment for cancer. Gut 61(2): 179-192.
- Siegel R, DeSantis C, Jemal A (2014) Colorectal cancer statistics. Cancer J Clin 64(2): 104-117.






























